Abstract
Aims
We sought to investigate temporal trends in prediabetes prevalence among US adolescents using two definitions and evaluate relationships with obesity and a MetS-severity score.
Methods
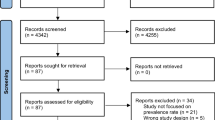
We evaluated data from 5418 non-Hispanic white, non-Hispanic black, and Hispanic adolescents aged 12–19 participating in the National Health and Nutrition Examination Survey 1999–2014 with complete data regarding MetS and hemoglobin A1c (HbA1c). Prediabetes status was defined by American Diabetes Association (ADA) criteria: fasting glucose 100–125 mg/dL or HbA1c 5.7%–6.4%. MetS severity was assessed with a MetS-severity Z-score.
Results
Prevalence of prediabetes as defined by HbA1c abnormalities significantly increased from 1999–2014, while prevalence of prediabetes as defined by fasting glucose abnormalities showed no significant temporal trend. There were variations in these trends across different racial/ethnic groups. MetS Z-score was overall more strongly correlated with HbA1c, fasting insulin, and the homeostasis model of insulin resistance than was BMI Z-score. These correlations were true in each racial/ethnic group with the exception that in non-Hispanic white adolescents, in whom the MetS Z-score was not significantly correlated with HbA1c measurements.
Conclusion
We found conflicting findings of temporal trends of US adolescent prediabetes prevalence based on the ADA’s prediabetes criteria. The increasing prevalence of prediabetes by HbA1c assessment is concerning and raises the urgency for increased awareness and appropriate measures of prediabetes status among physicians and patients.


Similar content being viewed by others
References
American Diabetes Association (2014) Standards of medical care in diabetes-2014. Diabetes Care 37:S14–S80
May AL, Kuklina EV, Yoon PW (2012) Prevalence of cardiovascular disease risk factors among US adolescents, 1999–2008. Pediatrics 129:1035–1041
Nichols GA, Hillier TA, Brown JB (2007) Progression from newly acquired impaired fasting glusose to type 2 diabetes. Diabetes Care 30:228–233
Sacks DB, Arnold M, Bakris GL et al (2011) Guidelines and recommendations for laboratory analysis in the diagnosis and management of diabetes mellitus. Diabetes Care 34:e61–e99
Garnett SP, Gow M, Ho M et al (2014) Improved insulin sensitivity and body composition, irrespective of macronutrient intake, after a 12 month intervention in adolescents with pre-diabetes; RESIST a randomised control trial. BMC Pediatr 14:289
Ford ES, Ajani UA, Mokdad AH (2005) The metabolic syndrome and concentrations of C-reactive protein among U.S. youth. Diabetes Care 28:878–881
Kursawe R, Santoro N (2014) Metabolic syndrome in pediatrics. Adv Clin Chem 65:91–142
DeBoer MD, Gurka MJ (2014) Low sensitivity of the metabolic syndrome to identify adolescents with impaired glucose tolerance: an analysis of NHANES 1999–2010. Cardiovasc Diabetol 13:83
Lee AM, Gurka MJ, DeBoer MD (2016) Trends in metabolic syndrome severity and lifestyle factors among adolescents. Pediatrics 137:1–9
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419
Ogden CL, Carroll MD, Kit BK, Flegal KM (2012) Prevalence of obesity and trends in body mass index among US children and adolescents, 1999–2010. JAMA 307:483–490
National Center for Health Statistics C, National health and nutrition examination survey protocol. http://www.cdc.gov/nchs/nhanes/nhanes_questionnaires.htm
Gurka MJ, Ice CL, Sun SS, DeBoer MD (2012) A confirmatory factor analysis of the metabolic syndrome in adolescents: an examination of sex and racial/ethnic differences. Cardiovasc Diabetol 11:128
Gurka MJ, Lilly CL, Norman OM, DeBoer MD (2014) An examination of sex and racial/ethnic differences in the metabolic syndrome among adults: a confirmatory factor analysis and a resulting continuous severity score. Metabolism 63:218–225
DeBoer MD, Gurka MJ, Woo JG, Morrison JA (2015) Severity of metabolic syndrome as a predictor of cardiovascular disease between childhood and adulthood: the princeton lipid research cohort study. J Am Coll Cardiol 66:755–757
DeBoer MD, Gurka MJ, Woo JG, Morrison JA (2015) Severity of the metabolic syndrome as a predictor of type 2 diabetes between childhood and adulthood: the Princeton Lipid Research Cohort Study. Diabetologia 58:2745–2752
Lee AM, Charlton JR, Carmody JB, Gurka MJ, DeBoer MD (2016) Metabolic risk factors in non-diabetic adolescents with glomerular hyperfiltration. Nephrol Dial Transpl. doi: 10.1093/ndt/gfw231
Lippi G, Targher G (2011) A laboratory standpoint on the role of hemoglobin A1c for the diagnosis of diabetes in childhood: more doubts than certainties? Pediatr Diabetes 12:183–186
Lee JM, Eason A, Nelson C, Kazzi NG, Cowan AE, Tarini BA (2014) Screening practices for identifying type 2 diabetes in adolescents. J Adolesc Health 54:139–143
Lee JM, Wu EL, Tarini B, Herman WH, Yoon E (2011) Diagnosis of diabetes using hemoglobin A1c: should recommendations in adults be extrapolated to adolescents? J Pediatr 158:947.e1-3–952.e1-3
Nowicka P, Santoro N, Liu H et al (2011) Utility of hemoglobin A(1c) for diagnosing prediabetes and diabetes in obese children and adolescents. Diabetes Care 34:1306–1311
Chan CL, McFann K, Newnes L, Nadeau KJ, Zeitler PS, Kelsey M (2014) Hemoglobin A1c assay variations and implications for diabetes screening in obese youth. Pediatr Diabetes 15:557–563
Cowie CC, Rust KF, Byrd-Holt DD et al (2010) Prevalence of diabetes and high risk for diabetes using A1C criteria in the U.S. population in 1988–2006. Diabetes Care 33:562–568
Kapadia C, Zeitler P (2012) Society DaTCotPE. Hemoglobin A1c measurement for the diagnosis of Type 2 diabetes in children. Int J Pediatr Endocrinol 2012:31
Love-Osborne KA, Sheeder J, Svircev A, Chan C, Zeitler P, Nadeau KJ (2013) Use of glycosylated hemoglobin increases diabetes screening for at-risk adolescents in primary care settings. Pediatr Diabetes 14:512–518
Ehehalt S, Gauger N, Blumenstock G et al (2010) Hemoglobin A1c is a reliable criterion for diagnosing type 1 diabetes in childhood and adolescence. Pediatr Diabetes 11:446–449
Expert Committee on the Diagnosis and Classification of Diabetes Mellitus (2003) Report of the expert committee on the diagnosis and classification of diabetes mellitus. Diabetes Care 26(Suppl 1):S5–20
International Expert Committee (2009) International Expert Committee report on the role of the A1C assay in the diagnosis of diabetes. Diabetes Care 32:1327–1334
DeBoer MD, Gurka MJ, Hill Golden S et al (2016) Independent associations between metabolic syndrome severity and future coronary heart disease by sex and race. J Am Coll Card (in press)
Sumner AE (2009) Ethnic differences in triglyceride levels and high-density lipoprotein lead to underdiagnosis of the metabolic syndrome in black children and adults. J Pediatr 155:e7–e11
Ukegbu UJ, Castillo DC, Knight MG et al (2011) Metabolic syndrome does not detect metabolic risk in African men living in the U.S. Diabetes Care 34:2297–2299
Arslanian S, Suprasongsin C, Janosky JE (1997) Insulin secretion and sensitivity in black versus white prepubertal healthy children. J Clin Endocrinol Metab 82:1923–1927
Ziemer DC, Kolm P, Weintraub WS et al (2010) Glucose-independent, black-white differences in hemoglobin A1c levels: a cross-sectional analysis of 2 studies. Ann Intern Med 152:770–777
Dabelea D, Mayer-Davis EJ, Saydah S et al (2014) Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA 311:1778–1786
Pihoker C, Gilliam LK, Ellard S et al (2013) Prevalence, characteristics and clinical diagnosis of maturity onset diabetes of the young due to mutations in HNF1A, HNF4A, and Glucokinase: results from the SEARCH for diabetes in youth. J Clin Endocrinol Metab 98:4055–4062
Steck AK, Winter WE (2011) Review on monogenic diabetes. Curr Opin Endocrinol Diabetes Obes 18:252–258
Weiss R (2007) Impaired glucose tolerance and risk factors for progression to type 2 diabetes in youth. Pediatric Diabetes 8:70–75
Malin SK, Gerber R, Chipkin SR, Braun B (2012) Independent and combined effects of exercise training and metformin on insulin sensitivity in individuals with prediabetes. Diabetes Care 35:131–136
Association AD (2013) Economic costs of diabetes in the U.S. in 2012. Diabetes Care 36:1033–1046
Buse JB, Kaufman FR, Linder B et al (2013) Diabetes screening with hemoglobin A(1c) versus fasting plasma glucose in a multiethnic middle-school cohort. Diabetes Care 36:429–435
Funding
This work was supported by National Institutes of Health grant 1R01HL120960 (MJG and MDD).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Ethical standard
This study was approved by the ethics review board of the National Center for Health Statistics, and all participants provided their informed consent in writing.
Human and animal rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Managed by Massimo Federici.
Rights and permissions
About this article
Cite this article
Lee, A.M., Fermin, C.R., Filipp, S.L. et al. Examining trends in prediabetes and its relationship with the metabolic syndrome in US adolescents, 1999–2014. Acta Diabetol 54, 373–381 (2017). https://doi.org/10.1007/s00592-016-0958-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-016-0958-6