Abstract
Aims
To assess the time-dependent effect of sleep quality on diabetes and coronary artery disease (CAD) incidence among young adults.
Methods
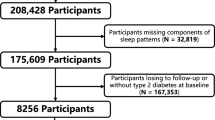
Incident rates of diabetes and CAD during a mean follow-up of 6.4 ± 4.1 years were assessed among 26,023 men (mean age 30.9 ± 5.6 years) of the Metabolic Lifestyle and Nutrition Assessment in Young Adults stratified by sleep quality at baseline, as assessed by the Mini-Sleep Questionnaire (MSQ). Incident diabetes and CAD were analyzed using a Cox proportional hazard model.
Results
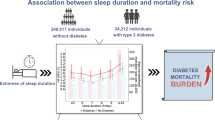
There were 445 cases of diabetes and 92 cases of CAD during 151,312 person-years. An abnormal MSQ score was associated with a 53 % higher incidence of diabetes (95 % CI 1.22–1.94, p < 0.001) compared to those with a normal score, after adjustment for clinical and biochemical diabetes risk factors. The increased risk associated with abnormal sleep quality remained when MSQ was modeled as a continuous time-dependent variable in a multivariable model (HR = 1.036, 95 % CI 1.024–1.049, p < 0.001). The increased risk was higher among overweight or obese participants (BMI and MSQ interaction p = 0.046). Sustained abnormality in MSQ score resulted in higher HR for diabetes (2.35; 95 % CI 1.564–3.519, p < 0.001). In addition, abnormal sleep quality was associated with a 2.38 higher incidence of CAD (95 % CI 1.38–4.11, p = 0.002), after adjustment for traditional clinical and biochemical risk factors.
Conclusions
Sleep quality contributes to the development of diabetes and CAD in apparently healthy young adults in a time-dependent manner. The use of a simple questionnaire to assess sleep quality may be a useful tool for risk stratification in this population.



Similar content being viewed by others
References
Killick R, Banks S, Liu PY (2012) Implications of sleep restriction and recovery on metabolic outcomes. J Clin Endocrinol Metab 97:3876–3890
Cappuccio FP, D’Elia L, Strazzullo P et al (2010) Quantity and quality of sleep and incidence of type 2 diabetes: a systematic review and meta-analysis. Diabetes Care 33:414–420
Resta O, Foschino-Barbaro MP, Legari G et al (2001) Sleep-related breathing disorders, loud snoring and excessive daytime sleepiness in obese subjects. Int J Obes Relat Metab Disord 25:669–675
Petrov ME, Kim Y, Lauderdale D et al (2013) Longitudinal associations between objective sleep and lipids: the CARDIA study. Sleep 36:1587–1595
Bjorkelund C, Bondyr-Carlsson D, Lapidus L et al (2005) Sleep disturbances in midlife unrelated to 32-year diabetes incidence: the prospective population study of women in Gothenburg. Diabetes Care 28:2739–2744
Meisinger C, Heier M, Loewel H (2005) Sleep disturbance as a predictor of type 2 diabetes mellitus in men and women from the general population. Diabetologia 48:235–241
Tirosh A, Shai I, Tekes-Manova D et al (2005) Normal fasting plasma glucose levels and type 2 diabetes in young men. N Engl J Med 353:1454–1462
Tirosh A, Shai I, Afek A et al (2011) Adolescent BMI trajectory and risk of diabetes versus coronary disease. N Engl J Med 364:1315–1325
Twig G, Afek A, Shamiss A et al (2012) White blood cell count and the risk for coronary artery disease in young adults. PLoS ONE 7:e47183
Alster J, Shemesh Z, Ornan M et al (1993) Sleep disturbance associated with chronic tinnitus. Biol Psychiatry 34:84–90
Klein E, Koren D, Arnon I et al (2003) Sleep complaints are not corroborated by objective sleep measures in post-traumatic stress disorder: a 1-year prospective study in survivors of motor vehicle crashes. J Sleep Res 12:35–41
Shochat T, Tzischinsky O, Oksenberg A et al (2007) Validation of the Pittsburgh Sleep Quality Index Hebrew translation (PSQI-H) in a sleep clinic sample. Isr Med Assoc J 9:853–856
Tzischinsky O, Latzer Y (2006) Sleep-wake cycles in obese children with and without binge-eating episodes. J Paediatr Child Health 42:688–693
Test T, Canfi A, Eyal A et al (2011) The influence of hearing impairment on sleep quality among workers exposed to harmful noise. Sleep 34:25–30
Tonetti L, Fabbri M, Erbacci A et al (2014) Association between seasonal affective disorder and subjective quality of the sleep/wake cycle in adolescents. Psychiatry Res 215:624–627
Falavigna A, de Souza Bezerra ML, Teles AR et al (2011) Consistency and reliability of the Brazilian Portuguese version of the Mini-Sleep Questionnaire in undergraduate students. Sleep Breath 15:351–355
Falavigna A, de Souza Bezerra ML, Teles AR et al (2011) Sleep disorders among undergraduate students in Southern Brazil. Sleep Breath 15:519–524
Melamed S, Oksenberg A (2002) Excessive daytime sleepiness and risk of occupational injuries in non-shift daytime workers. Sleep 25:315–322
Twig G, Gluzman I, Tirosh A et al (2014) Cognitive function and the risk for diabetes among young men. Diabetes Care 37:2982–2988
Twig G, Afek A, Shamiss A et al (2013) White blood cells count and incidence of type 2 diabetes in young men. Diabetes Care 36:276–282
Twig G, Afek A, Derazne E et al (2014) Diabetes risk among overweight and obese metabolically healthy young adults. Diabetes Care 37:2989–2995
Nilsson PM, Roost M, Engstrom G et al (2004) Incidence of diabetes in middle-aged men is related to sleep disturbances. Diabetes Care 27:2464–2469
Kawakami N, Takatsuka N, Shimizu H (2004) Sleep disturbance and onset of type 2 diabetes. Diabetes Care 27:282–283
Hayashino Y, Fukuhara S, Suzukamo Y et al (2007) Relation between sleep quality and quantity, quality of life, and risk of developing diabetes in healthy workers in Japan: the High-risk and Population Strategy for Occupational Health Promotion (HIPOP-OHP) Study. BMC Public Health 7:129
Boyko EJ, Seelig AD, Jacobson IG et al (2013) Sleep characteristics, mental health, and diabetes risk: a prospective study of U.S. military service members in the Millennium Cohort Study. Diabetes Care 36:3154–3161
Mallon L, Broman JE, Hetta J (2005) High incidence of diabetes in men with sleep complaints or short sleep duration: a 12-year follow-up study of a middle-aged population. Diabetes Care 28:2762–2767
Jarrin DC, McGrath JJ, Quon EC (2014) Objective and subjective socioeconomic gradients exist for sleep in children and adolescents. Health Psychol 33:301–305
Chandola T, Britton A, Brunner E et al (2008) Work stress and coronary heart disease: what are the mechanisms? Eur Heart J 29:640–648
Yusuf S, Hawken S, Ounpuu S et al (2005) Obesity and the risk of myocardial infarction in 27,000 participants from 52 countries: a case-control study. Lancet 366:1640–1649
Vgontzas AN, Bixler EO, Lin HM et al (2001) Chronic insomnia is associated with nyctohemeral activation of the hypothalamic-pituitary-adrenal axis: clinical implications. J Clin Endocrinol Metab 86:3787–3794
Morgenstern M, Wang J, Beatty N et al (2014) Obstructive sleep apnea: an unexpected cause of insulin resistance and diabetes. Endocrinol Metab Clin North Am 43:187–204
Liu R, Liu X, Zee PC et al (2014) Association between sleep quality and C-reactive protein: results from national health and nutrition examination survey, 2005–2008. PLoS ONE 9:e92607
Michels N, Clays E, De Buyzere M et al (2013) Children’s sleep and autonomic function: low sleep quality has an impact on heart rate variability. Sleep 36:1939–1946
Chouchou F, Pichot V, Pepin JL et al (2013) Sympathetic overactivity due to sleep fragmentation is associated with elevated diurnal systolic blood pressure in healthy elderly subjects: the PROOF-SYNAPSE study. Eur Heart J 34(2122–31):31a
Schmidt FP, Basner M, Kroger G et al (2013) Effect of nighttime aircraft noise exposure on endothelial function and stress hormone release in healthy adults. Eur Heart J 34:3508a–3514a
Polotsky VY, Li J, Punjabi NM et al (2003) Intermittent hypoxia increases insulin resistance in genetically obese mice. J Physiol 552:253–264
Drager LF, Li J, Reinke C et al (2011) Intermittent hypoxia exacerbates metabolic effects of diet-induced obesity. Obesity (Silver Spring) 19:2167–2174
Li J, Thorne LN, Punjabi NM et al (2005) Intermittent hypoxia induces hyperlipidemia in lean mice. Circ Res 97:698–706
Vassy JL, Durant NH, Kabagambe EK et al (2012) A genotype risk score predicts type 2 diabetes from young adulthood: the CARDIA study. Diabetologia 55:2604–2612
Vassy JL, Hivert MF, Porneala B et al (2014) Polygenic type 2 diabetes prediction at the limit of common variant detection. Diabetes 63:2172–2182
Nguyen QM, Srinivasan SR, Xu JH et al (2011) Elevated liver function enzymes are related to the development of prediabetes and type 2 diabetes in younger adults: the Bogalusa Heart Study. Diabetes Care 34:2603–2607
Vivante A, Twig G, Tirosh A et al (2014) Childhood history of resolved glomerular disease and risk of hypertension during adulthood. JAMA 311:1155–1157
Twig G, Livneh A, Vivante A et al (2014) Cardiovascular and metabolic risk factors in inherited autoinflammation. J Clin Endocrinol Metab 99:E2123–E2128
Acknowledgments
This study was supported by a research grant of the IDF Medical Corp and the Israeli ministry of defense (GT). GT and AT were partially supported by a grant from the Pinchas Borenstein Talpiot Medical Leadership Program, Chaim Sheba Medical Center, Tel Hashomer, Israel. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Conflict of interest
None.
Ethical standard
The study was approved by the institutional review board of the Israel Defense Forces Medical Corps.
Human and Animal Rights disclosure
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975. The Institutional Review Board of the IDF Medical Corps approved this study and waived the need for informed consent with the assurance of strict maintenance of participants’ anonymity during data analyses.
Informed consent
The need for informed consent was waived from this study on the basis of strict maintenance of participants’ anonymity during database analyses.
Author information
Authors and Affiliations
Corresponding author
Additional information
Managed by Massimo Federici.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Twig, G., Shina, A., Afek, A. et al. Sleep quality and risk of diabetes and coronary artery disease among young men. Acta Diabetol 53, 261–270 (2016). https://doi.org/10.1007/s00592-015-0779-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-015-0779-z