Abstract
Aims
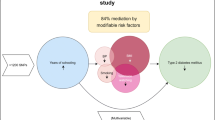
To investigate whether maternal educational level is associated with gestational diabetes mellitus (GDM), and to what extent risk factors for GDM mediate the effect of educational level.
Methods
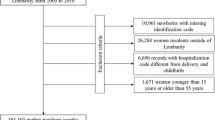
We examined data of 7,511 pregnant women participating in a population-based cohort study in Rotterdam, the Netherlands. The highest achieved education was categorized into four levels. Diagnosis of GDM was retrieved from delivery records. Odds ratios (OR) of GDM were calculated for levels of education, adjusting for confounders and potential mediators. Mediators were selected according to Baron and Kenny’s causal step approach.
Results
Adjusted for ethnicity, age, family history of diabetes and parity, women in the lowest educational level were three times more likely to develop GDM than women in the highest level (OR 3.07; 95 % CI 1.37, 6.89). Selected mediators were alcohol use and body mass index (BMI). Additional adjustment for alcohol use attenuated the OR to 2.54 (95 % CI 1.11, 5.78). The individual addition of BMI attenuated the OR to 2.35 (95 % CI 1.03, 5.35). All mediators together explained 51 % (95 % CI −122, −25) of the association between low education and GDM.
Conclusions
Low maternal educational level is associated with GDM, which is mainly due to higher rates of overweight and obesity. In order to reduce the higher rates of GDM, and consequently type 2 diabetes among women in low socioeconomic subgroups, prevention and intervention strategies need to be focused on reducing the rates of overweight and obesity before pregnancy.
Similar content being viewed by others
References
Cheung NW, Byth K (2003) Population health significance of gestational diabetes. Diabetes Care 26:2005–2009
Boney CM, Verma A, Tucker R, Vohr BR (2005) Metabolic syndrome in childhood: association with birth weight, maternal obesity, and gestational diabetes mellitus. Pediatrics 115:e290–e296
Gillman MW, Rifas-Shiman S, Berkey CS, Field AE, Colditz GA (2003) Maternal gestational diabetes, birth weight, and adolescent obesity. Pediatrics 111:e221–e226
Fadl H, Magnuson A, Ostlund I, Montgomery S, Hanson U, Schwarcz E (2014) Gestational diabetes mellitus and later cardiovascular disease: a Swedish population based case-control study. BJOG. doi:10.1111/1471-0528.12754
Shah BR, Retnakaran R, Booth GL (2008) Increased risk of cardiovascular disease in young women following gestational diabetes mellitus. Diabetes Care 31:1668–1669
Rathmann W, Giani G (2004) Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 27:2568–2569 author reply 2569
Evans JM, Newton RW, Ruta DA, MacDonald TM, Morris AD (2000) Socio-economic status, obesity and prevalence of type 1 and type 2 diabetes mellitus. Diabet Med 17:478–480
Agardh EE, Ahlbom A, Andersson T et al (2004) Explanations of socioeconomic differences in excess risk of type 2 diabetes in Swedish men and women. Diabetes Care 27:716–721
Bo S, Menato G, Bardelli C et al (2002) Low socioeconomic status as a risk factor for gestational diabetes. Diabetes Metab 28:139–140
Ben-Haroush A, Yogev Y, Hod M (2004) Epidemiology of gestational diabetes mellitus and its association with type 2 diabetes. Diabet Med 21:103–113
Saldana TM, Siega-Riz AM, Adair LS (2004) Effect of macronutrient intake on the development of glucose intolerance during pregnancy. Am J Clin Nutr 79:479–486
Hosler AS, Nayak SG, Radigan AM (2011) Stressful events, smoking exposure and other maternal risk factors associated with gestational diabetes mellitus. Paediatr Perinat Epidemiol 25:566–574
Jaddoe VW, Mackenbach JP, Moll HA et al (2006) The Generation R Study: design and cohort profile. Eur J Epidemiol 21:475–484
Jaddoe VW, Bakker R, van Duijn CM et al (2007) The Generation R Study biobank: a resource for epidemiological studies in children and their parents. Eur J Epidemiol 22:917–923
Jaddoe VW, van Duijn CM, Franco OH et al (2012) The Generation R Study: design and cohort update 2012. Eur J Epidemiol 27:739–756
World Medical Association I (2009) Declaration of Helsinki. Ethical principles for medical research involving human subjects. J Indian Med Assoc 107:403–405
Statistics Netherlands (2004) Standaard Onderwijsindeling 2003. Voorburg/Heerlen
McNamee R (2003) Confounding and confounders. Occup Environ Med 60:227–234 quiz 164, 234
Statistics Netherlands (2004) Allochtonen in Nederland 2004. Voorburg/Heerlen.
Jauniaux E, Burton GJ (2007) Morphological and biological effects of maternal exposure to tobacco smoke on the feto-placental unit. Early Hum Dev 83:699–706
Effron B, Tibshirani RJ (1993) An Introduction to the Bootstrap. Chapman and Hall, London
Rudra CB, Sorensen TK, Leisenring WM, Dashow E, Williams MA (2007) Weight characteristics and height in relation to risk of gestational diabetes mellitus. Am J Epidemiol 165:302–308
Seoud MA, Nassar AH, Usta IM, Melhem Z, Kazma A, Khalil AM (2002) Impact of advanced maternal age on pregnancy outcome. Am J Perinatol 19:1–8
Solomon CG, Willett WC, Carey VJ et al (1997) A prospective study of pregravid determinants of gestational diabetes mellitus. JAMA 278:1078–1083
American Diabetes Association (2004) Gestational diabetes mellitus. Diabetes Care 27 Suppl 1: S88–90
van Leeuwen M, Zweers EJ, Opmeer BC et al (2007) Comparison of accuracy measures of two screening tests for gestational diabetes mellitus. Diabetes Care 30:2779–2784
Anna V, van der Ploeg HP, Cheung NW, Huxley RR, Bauman AE (2008) Sociodemographic correlates of the increasing trend in prevalence of gestational diabetes mellitus in a large population of women between 1995 and 2005. Diabetes Care 31:2288–2293
Janghorbani M, Stenhouse EA, Jones RB, Millward BA (2006) Is neighbourhood deprivation a risk factor for gestational diabetes mellitus? Diabet Med 23:313–317
Shen JJ, Tymkow C, MacMullen N (2005) Disparities in maternal outcomes among four ethnic populations. Ethn Dis 15:492–497
Kahn SE, Hull RL, Utzschneider KM (2006) Mechanisms linking obesity to insulin resistance and type 2 diabetes. Nature 444:840–846
Baliunas DO, Taylor BJ, Irving H et al (2009) Alcohol as a risk factor for type 2 diabetes: a systematic review and meta-analysis. Diabetes Care 32:2123–2132
Heianza Y, Arase Y, Saito K et al (2013) Role of alcohol drinking pattern in type 2 diabetes in Japanese men: the Toranomon Hospital Health Management Center Study 11 (TOPICS 11). Am J Clin Nutr 97:561–568
Koppes LL, Dekker JM, Hendriks HF, Bouter LM, Heine RJ (2005) Moderate alcohol consumption lowers the risk of type 2 diabetes: a meta-analysis of prospective observational studies. Diabetes Care 28:719–725
Joosten MM, Beulens JW, Kersten S, Hendriks HF (2008) Moderate alcohol consumption increases insulin sensitivity and ADIPOQ expression in postmenopausal women: a randomised, crossover trial. Diabetologia 51:1375–1381
Davies MJ, Baer DJ, Judd JT, Brown ED, Campbell WS, Taylor PR (2002) Effects of moderate alcohol intake on fasting insulin and glucose concentrations and insulin sensitivity in postmenopausal women: a randomized controlled trial. JAMA 287:2559–2562
Joosten MM, van Erk MJ, Pellis L, Witkamp RF, Hendriks HF (2012) Moderate alcohol consumption alters both leucocyte gene expression profiles and circulating proteins related to immune response and lipid metabolism in men. Br J Nutr 108:620–627
Brien SE, Ronksley PE, Turner BJ, Mukamal KJ, Ghali WA (2011) Effect of alcohol consumption on biological markers associated with risk of coronary heart disease: systematic review and meta-analysis of interventional studies. BMJ 342:d636
Ronksley PE, Brien SE, Turner BJ, Mukamal KJ, Ghali WA (2011) Association of alcohol consumption with selected cardiovascular disease outcomes: a systematic review and meta-analysis. BMJ 342:d671
Terry PD, Weiderpass E, Ostenson CG, Cnattingius S (2003) Cigarette smoking and the risk of gestational and pregestational diabetes in two consecutive pregnancies. Diabetes Care 26:2994–2998
Radesky JS, Oken E, Rifas-Shiman SL, Kleinman KP, Rich-Edwards JW, Gillman MW (2008) Diet during early pregnancy and development of gestational diabetes. Paediatr Perinat Epidemiol 22:47–59
Bo S, Menato G, Lezo A et al (2001) Dietary fat and gestational hyperglycaemia. Diabetologia 44:972–978
Acknowledgments
The Generation R Study is conducted by the Erasmus Medical Centre in close collaboration with the Erasmus University Rotterdam, School of Law and Faculty of Social Sciences, the Municipal Health Service Rotterdam area, Rotterdam, the Rotterdam Homecare Foundation, Rotterdam and the Stichting Trombosedienst & Artsenlaboratorium Rijnmond (STAR), Rotterdam. We gratefully acknowledge the contribution of general practitioners, hospitals, midwives and pharmacies in Rotterdam.
Conflict of interest
Selma H. Bouthoorn, Lindsay M. Silva, Sheila E. Murray, Eric A. P. Steegers, Vincent W. V. Jaddoe, Henriette Moll, Albert Hofman, Johan P. Mackenbach and Hein Raat declare that they have no conflict of interest.
Human and animal rights disclosure
The study was conducted in accordance with the guidelines proposed in the World Medical Association Declaration of Helsinki and has been approved by the Medical Ethical Committee of the Erasmus MC, University Medical Centre Rotterdam [16].
Informed consent disclosure
Written consent was obtained from all patients for being included in the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Managed by Massimo Porta.
Rights and permissions
About this article
Cite this article
Bouthoorn, S.H., Silva, L.M., Murray, S.E. et al. Low-educated women have an increased risk of gestational diabetes mellitus: the Generation R Study. Acta Diabetol 52, 445–452 (2015). https://doi.org/10.1007/s00592-014-0668-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-014-0668-x