Abstract
Introduction
This study evaluated the relationship between postoperative knee flexion angles and the position of femoral and tibial components in unicompartmental knee arthroplasty (UKA).
Materials and methods
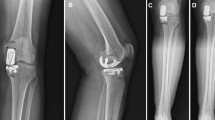
Eighteen patients (a total of 22 knees: three men, four knees; 15 females, 18 knees) who underwent navigation-assisted UKA were included. Pre- and postoperative computed tomography images were applied on 3D software, which were matched and used to calculate the position of femoral and tibial components. Correspondingly, we investigated the relationship between the knee range of motion (ROM) at 1-year postoperative follow-up and the position of femoral and tibial components.
Results
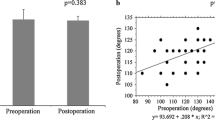
At 1-year post-UKA, the knee flexion angle was associated with the posterior flexion angle of tibial components. This particular angle was significantly greater in the group with equal or greater postoperative knee ROM compared to preoperative ROM (5.2 ± 2.1°) than in the group with less postoperative knee ROM compared to preoperative ROM (2.6 ± 1.6°, p < 0.01). There was no significant difference between both groups in the femoral component position, preoperative posterior slope of the medial tibial plateau, change in the pre- to postoperative posterior tibial slope, and postoperative knee society score.
Conclusion
The posterior flexion angle of the tibial component affected the improvement/deterioration of the postsurgery knee flexion angle in navigation-assisted UKA. For improved outcomes after UKA using navigation systems, surgeons should aim to achieve a 5° to 8° posterior flexion angle of the tibial component.



Similar content being viewed by others
References
Yang KY, Wang MC, Yeo SJ, Lo NN (2003) Minimally invasive unicondylar versus total condylar knee arthroplasty—early results of a matched-pair comparison. Singapore Med J 44:559–562. https://doi.org/10.1007/s00167-011-1787-3
Lombardi AV Jr, Berend KR, Walter CA, Aziz-Jacobo J, Cheney NA (2009) Is recovery faster for mobile-bearing unicompartmental than total knee arthroplasty? Clin Orthop Relat Res 467:1450–1457. https://doi.org/10.1007/s11999-009-0731-z
Lyons MC, MacDonald SJ, Somerville LE, Naudie DD, McCalden RW (2012) Unicompartmental versus total knee arthroplasty database analysis: is there a winner? Clin Orthop Relat Res 470:84–90. https://doi.org/10.1007/s11999-011-2144-z
Heyse TJ, El-Zayat BF, De Corte R, Chevalier Y, Scheys L, Innocenti B, Fuchs-Winkelmann S, Labey L (2014) UKA closely preserves natural knee kinematics in vitro. Knee Surg Sports Traumatol Arthrosc 22:1902–1910. https://doi.org/10.1007/s00167-013-2752-0
Goh GSH, Bin Abd Razak HR, Tay DKJ, Chia SL, Lo NN, Yeo SJ (2018) Unicompartmental knee arthroplasty achieves greater flexion with no difference in functional outcome, quality of life, and satisfaction vs total knee arthroplasty in patients younger than 55 years. A propensity score-matched cohort analysis. J Arthroplasty 33:355–361. https://doi.org/10.1016/j.arth.2017.09.022
Lygre SH, Espehaug B, Havelin LI, Furnes O, Vollset SE (2010) Pain and function in patients after primary unicompartmental and total knee arthroplasty. J Bone Joint Surg Am 92:2890–2897. https://doi.org/10.2106/jbjs.i.00917
Newman JH, Ackroyd CE, Shah NA (1998) Unicompartmental or total knee replacement? Five-year results of a prospective, randomized trial of 102 osteoarthritic knees with unicompartmental arthritis. J Bone Joint Surg Br 80:862–865. https://doi.org/10.1302/0301-620x.80b5.0800862
Barbadoro P, Ensini A, Leardini A, d'Amato M, Feliciangeli A, Timoncini A, Amadei F, Belvedere C, Giannini S (2014) Tibial component alignment and risk of loosening in unicompartmental knee arthroplasty: a radiographic and radiostereometric study. Knee Surg Sports Traumatol Arthrosc 22:3157–3162. https://doi.org/10.1007/s00167-014-3147-6
Arirachakaran A, Choowit P, Putananon C, Muangsiri S, Kongtharvonskul J (2015) Is unicompartmental knee arthroplasty (UKA) superior to total knee arthroplasty (TKA)? A systematic review and meta-analysis of randomized controlled trial. Eur J Orthop Surg Traumatol 25:799–806. https://doi.org/10.1007/s00590-015-1610-9
Furnes O, Espehaug B, Lie SA, Vollset SE, Engesaeter LB, Havelin LI (2007) Failure mechanisms after unicompartmental and tricompartmental primary knee replacement with cement. J Bone Joint Surg Am 89:519–525. https://doi.org/10.2106/jbjs.f.00210
Koskinen E, Eskelinen A, Paavolainen P, Pulkkinen P, Remes V (2008) Comparison of survival and cost-effectiveness between unicondylar arthroplasty and total knee arthroplasty in patients with primary osteoarthritis: a follow-up study of 50,493 knee replacements from the Finnish Arthroplasty Register. Acta Orthop 79:499–507. https://doi.org/10.1080/17453670710015490
Niinimäki T, Eskelinen A, Mäkelä K, Ohtonen P, Puhto AP, Remes V (2014) Unicompartmental knee arthroplasty survivorship is lower than TKA survivorship: a 27-year Finnish registry study. Clin Orthop Relat Res 472:1496–1501. https://doi.org/10.1007/s11999-013-3347-2
Brumby SA, Carrington R, Zayontz S, Reish T, Scott RD (2003) Tibial plateau stress fracture: a complication of unicompartmental knee arthroplasty using 4 guide pinholes. J Arthroplasty 18:809–812. https://doi.org/10.1016/s0883-5403(03)00330-9
Romanowski MR, Repicci JA (2002) Minimally invasive unicondylar arthroplasty: eight-year follow-up. Am J Knee Surg 15:17–22. https://doi.org/10.1097/00132585-200210040-00004
Seon JK, Song EK, Yoon TR, Seo HY, Cho SG (2007) Tibial plateau stress fracture after unicondylar knee arthroplasty using a navigation system: two case reports. Knee Surg Sports Traumatol Arthrosc 15:67–70. https://doi.org/10.1007/s00167-006-0097-7
Yang KY, Yeo SJ, Lo NN (2003) Stress fracture of the medial tibial plateau after minimally invasive unicompartmental knee arthroplasty: a report of 2 cases. J Arthroplasty 18:801–803. https://doi.org/10.1016/s0883-5403(03)00332-2
Hamilton TW, Pandit HG, Inabathula A, Ostlere SJ, Jenkins C, Mellon SJ, Dodd CA, Murray DW (2017) Unsatisfactory outcomes following unicompartmental knee arthroplasty in patients with partial thickness cartilage loss: a medium-term follow-up. Bone Joint J 99:475–482. https://doi.org/10.1302/0301-620x.99b4.bjj-2016-1061.r1
Lee SY, Bae JH, Kim JG, Jang KM, Shon WY, Kim KW, Lim HC (2014) The influence of surgical factors on dislocation of the meniscal bearing after Oxford medial unicompartmental knee replacement: a case-control study. Bone Joint J 96:914–922. https://doi.org/10.1302/0301-620x.96b7.33352
Hernigou P, Deschamps G (2004) Posterior slope of the tibial implant and the outcome of unicompartmental knee arthroplasty. J Bone Joint Surg [Am] 86:506–511. https://doi.org/10.2106/00004623-200403000-00007
Keene G, Simpson D, Kalairajah Y (2006) Limb alignment in computer-assisted minimally-invasive unicompartmental knee replacement. J Bone Joint Surg Br 88:44–48. https://doi.org/10.1302/0301-620x.88b1.16266
Pandit H, Hamilton TW, Jenkins C, Mellon SJ, Dodd CA, Murray DW (2015) The clinical outcome of minimally invasive Phase 3 Oxford unicompartmental knee arthroplasty: a 15-year follow-up of 1000 UKAs. Bone Joint J 97:1493–1500. https://doi.org/10.1302/0301-620x.97b11.35634
Yoshida K, Tada M, Yoshida H, Takei S, Fukuoka S, Nakamura H (2013) Oxford phase 3 unicompartmental knee arthroplasty in Japan—clinical results in greater than one thousand cases over ten years. J Arthroplasty 28:168–171. https://doi.org/10.1016/j.arth.2013.08.019
Chatellard R, Sauleau V, Colmar M, Robert H, Raynaud G, Brilhault J, d’Orthopédie S, de Traumatologie de l’Ouest (SOO), (2013) Medial unicompartmental knee arthroplasty: does tibial component position influence clinical outcomes and arthroplasty survival? Orthop Traumatol Surg Res 99:S219–S225. https://doi.org/10.1016/j.rcot.2013.03.005
Cobb J, Henckel J, Gomes P, Harris S, Jakopec M, Rodriguez F, Barrett A, Davies B (2006) Hands-on robotic unicompartmental knee replacement: a prospective, randomised controlled study of the acrobot system. J Bone Joint Surg Br 88:188–197. https://doi.org/10.1302/0301-620x.88b2.17220
Dunbar NJ, Roche MW, Park BH, Branch SH, Conditt MA, Banks SA (2012) Accuracy of dynamic tactile-guided unicompartmental knee arthroplasty. J Arthroplast 27:803–808. https://doi.org/10.1016/j.arth.2011.09.021
Cossey AJ, Spriqqins AJ (2005) The use of computer-assisted surgical navigation to prevent malalignment in unicompartmental knee arthroplasty. J Arthroplasty 20:29–34. https://doi.org/10.1016/j.arth.2004.10.012
Jung KA, Kim SJ, Lee SC, Hwang SH, Ahn NK (2010) Accuracy of implantation during computer-assisted minimally invasive Oxford unicompartmental knee arthroplasty: a comparison with a conventional instrumented technique. Knee 17:387–391. https://doi.org/10.1016/j.knee.2009.11.003
Konyves A, Willis-Owen CA, Spriggins AJ (2010) The long-term benefit of computer-assisted surgical navigation in unicompartmental knee arthroplasty. J Orthop Surg Res 31(5):94. https://doi.org/10.1186/1749-799x-5-94
Rosenberger RE, Fink C, Quirbach S, Attal R, Tecklenburg K, Hoser C (2008) The immediate effect of navigation on implant accuracy in primary mini-invasive unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 16:1133–1140. https://doi.org/10.1007/s00167-008-0618-7
Seon JK, Song EK, Park SJ, Yoon TR, Lee KB, Jung ST (2009) Comparison of minimally invasive unicompartmental knee arthroplasty with or without a navigation system. J Arthroplasty 24:351–357. https://doi.org/10.1016/j.arth.2007.10.025
Song EK, Mohite N, Lee SH, Na BR, Seon JK, (2016) Comparison of outcome and survival after unicompartmental knee arthroplasty between navigation and conventional techniques with an average 9-year follow-up. J Arthroplasty 31:395–400. https://doi.org/10.1016/j.arth.2015.09.012
Valenzuela GA, Jacobson NA, Geist DJ, Valenzuela RG, Teitge RA (2013) Implant and limb alignment outcomes for conventional and navigated unicompartmental knee arthroplasty. J Arthroplasty 28:463–468. https://doi.org/10.1016/j.arth.2012.09.001
Weber P, Crispin A, Schmidutz F, Utzschneider S, Pietschmann MF, Jansson V, Müller PE (2013) Improved accuracy in computer-assisted unicondylar knee arthroplasty: a meta-analysis. Knee Surg Sports Traumatol Arthrosc 21:2453–2461. https://doi.org/10.1007/s00167-013-2370-x
Choy WS, Lee KW, Kim HY, Kim KJ, Chun YS, Yang DS (2017) Mobile bearing medial unicompartmental knee arthroplasty in patients whose lifestyles involve high degrees of knee flexion: a 10–14 year follow-up study. Knee 24:829–836. https://doi.org/10.1016/j.knee.2017.05.004
White SH, Ludkowski PF, Goodfellow JW (1991) Anteromedial osteoarthritis of the knee. J Bone Joint Surg Br 73:582–586. https://doi.org/10.1302/0301-620x.73b4.2071640
Vasso M, Del Regno C, D'Amelio A, Viggiano D, Corona K, Schiavone Panni A (2015) Minor varus alignment provides better results than neutral alignment in medial UKA. Knee 22:117–121. https://doi.org/10.1016/j.knee.2014.12.004
Hamamoto Y, Ito H, Furu M, Ishikawa M, Azukizawa M, Kuriyama S, Nakamura S, Matsuda S (2015) Cross-cultural adaptation and validation of the Japanese version of the new Knee Society Scoring System for osteoarthritic knee with total knee arthroplasty. J Orthop Sci 20:849–853. https://doi.org/10.1007/s00776-015-0736-2
Scuderi GR, Bourne RB, Noble PC, Benjamin JB, Lonner JH, Scott WN (2012) The new knee society knee scoring system. Clin Orthop Relat Res 470:3–19. https://doi.org/10.1007/s11999-011-2135-0
Gatha NM, Clarke HD, Fuchs R, Scuderi GR, Insall JN (2004) Factors affecting postoperative range of motion after total knee arthroplasty. J Knee Surg 17:196–202. https://doi.org/10.1055/s-0030-1248221
Lizaur A, Marco L, Cebrian R (1997) Preoperative factors influencing the range of movement after total knee arthroplasty for severe osteoarthritis. J Bone Joint Surg Br 79:626–629. https://doi.org/10.1302/0301-620x.79b4.0790626
Ritter MA, Harty LD, Davis KE, Meding JB, Berend ME (2003) Predicting range of motion after total knee arthroplasty. Clustering, log-linear regression, and regression tree analysis. J Bone Joint Surg Am 85:1278–1285. https://doi.org/10.2106/00004623-200307000-00014
Takayama K, Matsumoto T, Muratsu H, Ishida K, Araki D, Matsushita T, Kuroda R, Kurosaka M (2016) The influence of posterior tibial slope changes on joint gap and range of motion in unicompartmental knee arthroplasty. Knee 23:517–522. https://doi.org/10.1016/j.knee.2016.01.003
Inui H, Taketomi S, Yamagami R, Kawaguchi K, Nakazato K, Tanaka S (2020) Necessary factors to achieve deep flexion for asian populations after Oxford unicompartmental knee arthroplasty. J Knee Surg 33:294–300. https://doi.org/10.1055/s-0039-1678539
Sekiguchi K, Nakamura S, Kuriyama S, Nishitani K, Ito H, Tanaka Y, Watanabe M, Matsuda S (2019) Effect of tibial component alignment on knee kinematics and ligament tension in medial unicompartmental knee arthroplasty. Bone Joint Res 8:126–135. https://doi.org/10.1302/2046-3758.83.BJR-2018-0208.R2
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
M. Hanada acquired and analyzed the data and wrote the manuscript. K. Hotta designed the study and wrote the manuscript. Y. Matsuyama advised on the study and approved the submission.
Corresponding author
Ethics declarations
Conflicts of interest
All authors declare that they have no conflict of interest
Ethical approval
All procedures performed during studies involving human participants were in accordance with the ethical standards of the institution (Hamamatsu University School of Medicine, No. 19–261) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hanada, M., Hotta, K. & Matsuyama, Y. Dependence of knee range of motion on the alignment of femoral and tibial components after medial unicompartmental knee arthroplasty. Eur J Orthop Surg Traumatol 31, 291–298 (2021). https://doi.org/10.1007/s00590-020-02770-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-020-02770-8