Abstract
Background
Delayed trunk and lower limb muscle activation is associated with balance loss and fall injuries in subjects with recurrent low back pain (LBP).
Purpose
This study was conducted to compare differences in the onset of muscle contractions of the trunk and lower limb muscles following a treadmill-induced step perturbation between subjects with and without LBP.
Methods
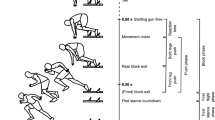
Eighty-three right limb dominant individuals (43 subjects with LBP and 40 control subjects) were exposed to the perturbation (0.31 m/s velocity for 0.2 m). The electromyography (EMG) reaction times were analyzed during the first step following the perturbation. The EMG electrodes were placed on both sides of the trunk and lower limbs, including the rectus abdominis (RA), erector spinae (ES), tibialis anterior (TA), and gastrocnemius (GA) muscles.
Results
The group x muscle interaction was statistically significant (F = 9.44, p = 0.003). The TA muscle activation was significantly delayed compared to the RA, ES, and GA. There was a significant interaction on side x muscle (F = 4.14, p = 0.04). The RA muscles were significantly delayed on the non-dominant (t = − 3.35, p = 0.001) and dominant (t = − 2.53, p = 0.01) sides in the LBP group.
Conclusion
The LBP group demonstrated a delayed reaction time on the RA muscles, which indicated poor trunk control relative to the lower limbs. The delayed bilateral RA muscle might indicate possible coordination problems relative to the ES and lower limb muscles, which may lead to potential fall hazards.



Similar content being viewed by others
References
Woolf AD, Pfleger B (2003) Burden of major musculoskeletal conditions. Bull World Health Organ 81:646–656
Sung PS, Maxwell MJ (2017) Kinematic chain reactions on trunk and dynamic postural steadiness in subjects with recurrent low back pain. J Biomech 59:109–115. https://doi.org/10.1016/j.jbiomech.2017.06.001
Tsao H, Galea MP, Hodges PW (2008) Reorganization of the motor cortex is associated with postural control deficits in recurrent low back pain. Brain 131:2161–2171. awn154 [pii]. https://doi.org/10.1093/brain/awn154
D'Hooge R, Hodges P, Tsao H, Hall L, Macdonald D, Danneels L (2013) Altered trunk muscle coordination during rapid trunk flexion in people in remission of recurrent low back pain. J Electromyogr Kinesiol 23:173–181. S1050-6411(12)00163-0 [pii]. https://doi.org/10.1016/j.jelekin.2012.09.003
Silfies SP, Squillante D, Maurer P, Westcott S, Karduna AR (2005) Trunk muscle recruitment patterns in specific chronic low back pain populations. Clin Biomech (Bristol, Avon) 20:465–473
Dankaerts W, O'Sullivan PB, Burnett AF, Straker LM (2007) The use of a mechanism-based classification system to evaluate and direct management of a patient with non-specific chronic low back pain and motor control impairment--a case report. Man Ther 12:181–191. S1356–689X(06)00075-0 [pii]. https://doi.org/10.1016/j.math.2006.05.004
Laird RA, Kent P, Keating JL (2012) Modifying patterns of movement in people with low back pain -does it help? A systematic review. BMC Musculoskelet Disord 13:169. https://doi.org/10.1186/1471-2474-13-169
Brumagne S, Janssens L, Janssens E, Goddyn L (2008) Altered postural control in anticipation of postural instability in persons with recurrent low back pain. Gait Posture 28:657–662. S0966-6362(08)00110-0 [pii]. https://doi.org/10.1016/j.gaitpost.2008.04.015
Sung PS, Danial P (2018) Trunk reaction time and kinematic changes following slip perturbations in subjects with recurrent low back pain. Ann Biomed Eng 46:488–497. https://doi.org/10.1007/s10439-017-1972-8
Prins MR, Griffioen M, Veeger TTJ, Kiers H, Meijer OG, van der Wurff P, Bruijn SM, van Dieen JH (2018) Evidence of splinting in low back pain? A systematic review of perturbation studies. Eur Spine J 27:40–59. https://doi.org/10.1007/s00586-017-5287-0
Leinonen V, Airaksinen M, Taimela S, Kankaanpaa M, Kukka A, Koivisto T, Airaksinen O (2007) Low back pain suppresses preparatory and triggered upper-limb activation after sudden upper-limb loading. Spine (Phila Pa 1976) 32:E150–155. https://doi.org/10.1097/01.brs.0000256886.94791.94
Jacobs JV, Henry SM, Nagle KJ (2010) Low back pain associates with altered activity of the cerebral cortex prior to arm movements that require postural adjustment. Clin Neurophysiol 121:431–440. https://doi.org/10.1016/j.clinph.2009.11.076
Sung PS, Spratt KF, Wilder DG (2004) A possible methodological flaw in comparing dominant and nondominant sided lumbar spine muscle responses without simultaneously considering hand dominance. Spine (Phila Pa 1976) 29:1914–1922. 00007632-200409010-00016 [pii]
Abboud J, Lardon A, Boivin F, Dugas C, Descarreaux M (2016) Effects of muscle fatigue, creep, and musculoskeletal pain on neuromuscular responses to unexpected perturbation of the trunk: a systematic review. Front Hum Neurosci 10:667. https://doi.org/10.3389/fnhum.2016.00667
van Dieen JH, Reeves NP, Kawchuk G, van Dillen LR, Hodges PW (2019) Analysis of motor control in patients with low back pain: a key to personalized care? J Orthop Sports Phys Ther 49:380–388. https://doi.org/10.2519/jospt.2019.7916
Reeves NP, Cholewicki J, van Dieen JH, Kawchuk G, Hodges PW (2019) Are stability and instability relevant concepts for back pain? J Orthop Sports Phys Ther. https://doi.org/10.2519/jospt.2019.8144
Ghamkhar L, Kahlaee AH (2015) Trunk muscles activation pattern during walking in subjects with and without chronic low back pain: a systematic review. PM R 7:519–526. https://doi.org/10.1016/j.pmrj.2015.01.013
Haddas R, Sawyer SF, Sizer PS, Brooks T, Chyu MC, James CR (2016) Effects of volitional spine stabilization and lower extremity fatigue on knee and ankle during landing performance in a recurrent low back pain population. J Sport Rehab. https://doi.org/10.1123/jsr.2015-0171
Brophy R, Silvers HJ, Gonzales T, Mandelbaum BR (2010) Gender influences: the role of leg dominance in ACL injury among soccer players. Br J Sports Med 44:694–697. bjsm.2008.051243 [pii]. https://doi.org/10.1136/bjsm.2008.051243
Andersen TE, Floerenes TW, Arnason A, Bahr R (2004) Video analysis of the mechanisms for ankle injuries in football. Am J Sports Med 32:69S-79S
Ciccone DS, Just N, Bandilla EB (1996) Non-organic symptom reporting in patients with chronic non-malignant pain. Pain 68:329–341
Sung PS, Danial P (2017) Gender difference of shoulder-pelvic kinematic integration for trunk rotation directions in healthy older adults. Clin Biomech (Bristol, Avon) 50:56–62. https://doi.org/10.1016/j.clinbiomech.2017.09.014
Sung PS, Ham YW (2010) Comparing postural strategy changes following adapted versus non-adapted responses in subjects with and without spinal stenosis. Man Ther 15:261–266. S1356-689X(10)00005-6 [pii]. https://doi.org/10.1016/j.math.2010.01.004
Kajrolkar T, Yang F, Pai YC, Bhatt T (2014) Dynamic stability and compensatory stepping responses during anterior gait-slip perturbations in people with chronic hemiparetic stroke. J Biomech 47:2751–2758. https://doi.org/10.1016/j.jbiomech.2014.04.051
Pai YC, Yang F, Bhatt T, Wang E (2014) Learning from laboratory-induced falling: long-term motor retention among older adults. Age (Dordr) 36:9640. https://doi.org/10.1007/s11357-014-9640-5
Solnik S, DeVita P, Rider P, Long B, Hortobagyi T (2008) Teager-Kaiser Operator improves the accuracy of EMG onset detection independent of signal-to-noise ratio. Acta Bioeng Biomech 10:65–68
Hodges PW, Bui BH (1996) A comparison of computer-based methods for the determination of onset of muscle contraction using electromyography. Electroencephalogr Clin Neurophysiol 101:511–519
Sung PS, Park MS (2022) Ankle reaction times with tray usage following a slip perturbation between subjects with and without chronic low back pain. Gait Posture 97:196–202. https://doi.org/10.1016/j.gaitpost.2022.07.260
Portney LG, Watkins MP (2009) Foundations of clinical research Applications to practice, 3rd edn. Pearson Education Inc., Upper Saddle
Jubany J, Marina M, Angulo-Barroso R (2017) Electromyographic and kinematic analysis of trunk and limb muscles during a holding task in individuals with chronic low back pain and healthy controls. PM R. https://doi.org/10.1016/j.pmrj.2017.04.008
Troy KL, Donovan SJ, Grabiner MD (2009) Theoretical contribution of the upper extremities to reducing trunk extension following a laboratory-induced slip. J Biomech 42:1339–1344. https://doi.org/10.1016/j.jbiomech.2009.03.004
Tong MH, Mousavi SJ, Kiers H, Ferreira P, Refshauge K, van Dieen J (2017) Is There a Relationship Between Lumbar Proprioception and Low Back Pain? A Systematic Review With Meta-Analysis. Arch Phys Med Rehab 98:120–136. https://doi.org/10.1016/j.apmr.2016.05.016
Schouppe S, Clauwaert A, Van Oosterwijck J, Van Damme S, Palmans T, Wiersema JR, Sanchis-Sanchez E, Danneels L (2020) Does experimentally induced pain-related fear influence central and peripheral movement preparation in healthy people and patients with low back pain? Pain 161:1212–1226. https://doi.org/10.1097/j.pain.0000000000001813
Sung PS, O’Sullivan E, Park MS (2021) The reaction times and symmetry indices in the bilateral trunk and limb muscles in control subjects and subjects with low back pain that persisted two months or longer. Eur Spine J. https://doi.org/10.1007/s00586-021-06797-1
McDowell C, Smyk M, Sung PS (2018) Compensatory strategy between trunk-hip kinematics and reaction time following slip perturbation between subjects with and without chronic low back pain. J Electromyogr Kinesiol 43:68–74. https://doi.org/10.1016/j.jelekin.2018.09.005
Sung PS, Danial P (2018) Trunk sway response to consecutive slip perturbations between subjects with and without recurrent low back pain. Musculoskelet Sci Pract 33:84–89. https://doi.org/10.1016/j.msksp.2017.12.005
You J, Chou Y, Lin C, Su F (2001) Effect of slip on movement of body center of mass relative to base of support. Clin Biomech (Bristol, Avon) 16:167–173
Marigold DS, Patla AE (2002) Strategies for dynamic stability during locomotion on a slippery surface: effects of prior experience and knowledge. J Neurophysiol 88:339–353. https://doi.org/10.1152/jn.00691.2001
Milosevic M, Shinya M, Masani K, Patel K, McConville KM, Nakazawa K, Popovic MR (2016) Anticipation of direction and time of perturbation modulates the onset latency of trunk muscle responses during sitting perturbations. J Electromyogr Kinesiol 26:94–101. https://doi.org/10.1016/j.jelekin.2015.12.003
Mueller J, Engel T, Mueller S, Stoll J, Baur H, Mayer F (2017) Effects of sudden walking perturbations on neuromuscular reflex activity and three-dimensional motion of the trunk in healthy controls and back pain symptomatic subjects. PLoS ONE 12:e0174034. https://doi.org/10.1371/journal.pone.0174034
Acknowledgements
The authors thank participants at Central Michigan University and Dr. DC Lee at BioCAT Inc. for his technical assistance for data analyses and contributions to the study. This study was supported by the Scholarship Council, Lilly Faculty Scholarship Award at Indiana Wesleyan University (2573877).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any financial or personal conflicts of interest in relation to the submission, other people, or any organizations.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sung, P.S., Park, M.S. Delayed response in rectus abdominis muscle following a step perturbation in subjects with and without recurrent low back pain. Eur Spine J 32, 1842–1849 (2023). https://doi.org/10.1007/s00586-023-07639-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07639-y