Abstract
Purpose
Growing evidence suggests an association between lumbar paraspinal muscle degeneration and low back pain (LBP). Currently, time-consuming and laborious manual segmentations of paraspinal muscles are commonly performed on magnetic resonance imaging (MRI) axial scans. Automated image analysis algorithms can mitigate these drawbacks, but they often require individual MRIs to be aligned to a standard “reference” atlas. Such atlases are well established in automated neuroimaging analysis. Our aim was to create atlases of similar nature for automated paraspinal muscle measurements.
Methods
Lumbosacral T2-weighted MRIs were acquired from 117 patients who experienced LBP, stratified by gender and age group (30–39, 40–49, and 50–59 years old). Axial MRI slices of the L4–L5 and L5–S1 levels at mid-disc were obtained and aligned using group-wise linear and nonlinear image registration to produce a set of unbiased population-averaged atlases for lumbar paraspinal muscles.
Results
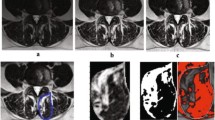
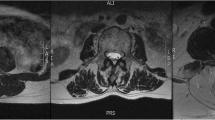
The resulting atlases represent the averaged morphology and MRI intensity features of the corresponding cohorts. Differences in paraspinal muscle shapes and fat infiltration levels with respect to gender and age can be visually identified from the population-averaged data from both linear and nonlinear registrations.
Conclusion
We constructed a set of population-averaged atlases for developing automated algorithms to help analyze paraspinal muscle morphometry from axial MRI scans. Such an advancement could greatly benefit the fields of paraspinal muscle and LBP research.
Graphical abstract
These slides can be retrieved under Electronic Supplementary Material.





Similar content being viewed by others
References
Balague F, Mannion AF, Pellise F, Cedraschi C (2012) Non-specific low back pain. Lancet 379(9814):482–491. https://doi.org/10.1016/S0140-6736(11)60610-7
Deyo RA, Weinstein JN (2001) Low back pain. N Engl J Med 344(5):363–370. https://doi.org/10.1056/NEJM200102013440508
Refshauge KM, Maher CG (2006) Low back pain investigations and prognosis: a review. Br J Sports Med 40(6):494–498. https://doi.org/10.1136/bjsm.2004.016659
Zotti MGT, Boas FV, Clifton T, Piche M, Yoon WW, Freeman BJC (2017) Does pre-operative magnetic resonance imaging of the lumbar multifidus muscle predict clinical outcomes following lumbar spinal decompression for symptomatic spinal stenosis? Eur Spine J 26(10):2589–2597. https://doi.org/10.1007/s00586-017-4986-x
Shahidi B, Parra CL, Berry DB, Hubbard JC, Gombatto S, Zlomislic V, Allen RT, Hughes-Austin J, Garfin S, Ward SR (2017) Contribution of lumbar spine pathology and age to paraspinal muscle size and fatty infiltration. Spine 42(8):616–623. https://doi.org/10.1097/BRS.0000000000001848
Hodges P, Holm AK, Hansson T, Holm S (2006) Rapid atrophy of the lumbar multifidus follows experimental disc or nerve root injury. Spine 31(25):2926–2933. https://doi.org/10.1097/01.brs.0000248453.51165.0b
Yarjanian JA, Fetzer A, Yamakawa KS, Tong HC, Smuck M, Haig A (2013) Correlation of paraspinal atrophy and denervation in back pain and spinal stenosis relative to asymptomatic controls. PM&R 5(1):39–44. https://doi.org/10.1016/j.pmrj.2012.08.017
Ranger TA, Cicuttini FM, Jensen TS, Peiris WL, Hussain SM, Fairley J, Urquhart DM (2017) Are the size and composition of the paraspinal muscles associated with low back pain? A systematic review. Spine J 17(11):1729–1748. https://doi.org/10.1016/j.spinee.2017.07.002
Takayama K, Kita T, Nakamura H, Kanematsu F, Yasunami T, Sakanaka H, Yamano Y (2016) New predictive index for lumbar paraspinal muscle degeneration associated with aging. Spine 41(2):E84–E90. https://doi.org/10.1097/BRS.0000000000001154
Fortin M, Videman T, Gibbons LE, Battie MC (2014) Paraspinal muscle morphology and composition: a 15-year longitudinal magnetic resonance imaging study. Med Sci Sports Exerc 46(5):893–901. https://doi.org/10.1249/MSS.0000000000000179
Fortin M, Omidyeganeh M, Battie MC, Ahmad O, Rivaz H (2017) Evaluation of an automated thresholding algorithm for the quantification of paraspinal muscle composition from MRI images. Biomed Eng Online 16(1):61. https://doi.org/10.1186/s12938-017-0350-y
Young AA, Frangi AF (2009) Computational cardiac atlases: from patient to population and back. Exp Physiol 94(5):578–596. https://doi.org/10.1113/expphysiol.2008.044081
Fonov V, Evans AC, Botteron K, Almli CR, McKinstry RC, Collins DL, Brain Development Cooperative G (2011) Unbiased average age-appropriate atlases for pediatric studies. Neuroimage 54(1):313–327. https://doi.org/10.1016/j.neuroimage.2010.07.033
Xiao Y, Fonov V, Beriault S, Al Subaie F, Chakravarty MM, Sadikot AF, Pike GB, Collins DL (2015) Multi-contrast unbiased MRI atlas of a Parkinson’s disease population. Int J Comput Assist Radiol Surg 10(3):329–341. https://doi.org/10.1007/s11548-014-1068-y
Cabezas M, Oliver A, Llado X, Freixenet J, Cuadra MB (2011) A review of atlas-based segmentation for magnetic resonance brain images. Comput Methods Programs Biomed 104(3):e158–e177. https://doi.org/10.1016/j.cmpb.2011.07.015
May A, Gaser C (2006) Magnetic resonance-based morphometry: a window into structural plasticity of the brain. Curr Opin Neurol 19(4):407–411. https://doi.org/10.1097/01.wco.0000236622.91495.21
Xiao Y, Bailey L, Chakravarty MM, Beriault S, Sadikot AF, Pike GB, Collins DL (2012) Atlas-based segmentation of the subthalamic nucleus, red nucleus, and substantia nigra for deep brain stimulation by incorporating multiple MRI contrasts. Paper presented at the Proceedings of the third international conference on Information Processing in Computer-Assisted Interventions, Pisa, Italy
Xiao Y, Fonov VS, Beriault S, Gerard I, Sadikot AF, Pike GB, Collins DL (2015) Patch-based label fusion segmentation of brainstem structures with dual-contrast MRI for Parkinson’s disease. Int J Comput Assist Radiol Surg 10(7):1029–1041. https://doi.org/10.1007/s11548-014-1119-4
Tustison NJ, Avants BB, Cook PA, Zheng Y, Egan A, Yushkevich PA, Gee JC (2010) N4ITK: improved N3 bias correction. IEEE Trans Med Imaging 29(6):1310–1320. https://doi.org/10.1109/TMI.2010.2046908
Nyul LG, Udupa JK, Zhang X (2000) New variants of a method of MRI scale standardization. IEEE Trans Med Imaging 19(2):143–150. https://doi.org/10.1109/42.836373
Peng YG, Ganesh A, Wright J, Xu WL, Ma Y (2012) RASL: robust alignment by sparse and low-rank decomposition for linearly correlated images. IEEE Trans Pattern Anal 34(11):2233–2246. https://doi.org/10.1109/Tpami.2011.282
Avants BB, Tustison NJ, Song G, Cook PA, Klein A, Gee JC (2011) A reproducible evaluation of ANTs similarity metric performance in brain image registration. Neuroimage 54(3):2033–2044. https://doi.org/10.1016/j.neuroimage.2010.09.025
Ashburner J, Hutton C, Frackowiak R, Johnsrude I, Price C, Friston K (1998) Identifying global anatomical differences: deformation-based morphometry. Hum Brain Mapp 6(5–6):348–357
Litjens G, Kooi T, Bejnordi BE, Setio AAA, Ciompi F, Ghafoorian M, van der Laak JAWM, van Ginneken B, Sanchez CI (2017) A survey on deep learning in medical image analysis. Med Image Anal 42:60–88. https://doi.org/10.1016/j.media.2017.07.005
Shattuck DW, Mirza M, Adisetiyo V, Hojatkashani C, Salamon G, Narr KL, Poldrack RA, Bilder RM, Toga AW (2008) Construction of a 3D probabilistic atlas of human cortical structures. Neuroimage 39(3):1064–1080. https://doi.org/10.1016/j.neuroimage.2007.09.031
Acknowledgement
This project was partly funded by the Natural Sciences and Engineering Research Council of Canada (NSERC) Discovery Grant RGPIN-2015-04136.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xiao, Y., Fortin, M., Battié, M.C. et al. Population-averaged MRI atlases for automated image processing and assessments of lumbar paraspinal muscles. Eur Spine J 27, 2442–2448 (2018). https://doi.org/10.1007/s00586-018-5704-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-018-5704-z