Abstract
Purpose
To compare measurements of motor evoked potential latency stimulated either magnetically (mMEP) or electrically (eMEP) and central motor conduction time (CMCT) made pre-operatively in conscious patients using transcranial and intra-operatively using electrical cortical stimulation before and after successful instrumentation for the treatment of adolescent idiopathic scoliosis.
Methods
A group initially of 51 patients with adolescent idiopathic scoliosis aged 12–19 years was evaluated pre-operatively in the outpatients’ department with transcranial magnetic stimulation. The neurophysiological data were then compared statistically with intra-operative responses elicited by transcranial electrical stimulation both before and after successful surgical intervention. MEPs were measured as the cortically evoked compound action potentials of Abductor hallucis. Minimum F-waves were measured using conventional nerve conduction methods and the lower motor neuron conduction time was calculated and this was subtracted from MEP latency to give CMCT.
Results
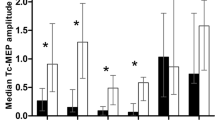
Pre-operative testing was well tolerated in our paediatric/adolescent patients. No neurological injury occurred in any patient in this series. There was no significant difference in the values of mMEP and eMEP latencies seen pre-operatively in conscious patients and intra-operatively in patients under anaesthetic. The calculated quantities mCMCT and eCMCT showed the same statistical correlations as the quantities mMEP and eMEP latency.
Conclusions
The congruency of mMEP and eMEP and of mCMCT and eCMCT suggests that these measurements may be used comparatively and semi-quantitatively for the comparison of pre-, intra-, and post-operative spinal cord function in spinal deformity surgery.






Similar content being viewed by others
References
Aleem AW, Thuet ED, Padberg AM et al (2015) Spinal cord monitoring data in pediatric spinal deformity patients with spinal cord pathology. Spine Deform 3:88–94
Bhagat S, Durst A, Grover H et al (2015) An evaluation of multimodal spinal cord monitoring in scoliosis surgery: a single centre experience of 354 operations. Eur Spine J 24:1399–1407
Brocke J, Irlbacher K, Hauptmann B et al (2005) Transcranial magnetic and electrical stimulation compared: does TES activate intracortical neuronal circuits? Clin Neurophysiol 116:2748–2756
Cho SK, Lenke LG, Bolon SM et al (2015) Can intraoperative spinal cord monitoring reliably help prevent paraplegia during posterior vertebral column resection surgery? Spine 3:73–81
Fehlings MG, Brodke DS, Norvell DC et al (2010) The evidence for intraoperative neurophysiological monitoring in spine surgery: does it make a difference? Spine (Phila Pa 1976) 35:S37–S46
Fitzgerald PB, Daskalakis ZJ (2012) A practical guide to the use of repetitive transcranial magnetic stimulation in the treatment of depression. Brain Stimul 5:287–296
Fitzsimons L, Disner SG, Bress JN (2009) Effective utilization and future directions for repetitive transcranial magnetic stimulation: a guide for psychiatric nurses. J Am Psychiatr Nurses Assoc 15:314–324
Frye RE, Rotenberg A, Ousley M et al (2008) Transcranial magnetic stimulation in child neurology: current and future directions. J Child Neurol 23:79–96
Galletly C, Fitzgerald P, Clarke P et al (2010) A practical guide to setting up a repetitive transcranial magnetic stimulation (rTMS) service. Australas Psychiatry 18:314–317
Galloway GM, Dias BR, Brown JL et al (2013) Transcranial magnetic stimulation may be useful as a preoperative screen of motor tract function. J Clin Neurophysiol 30:386–389
Glasby MA (2005) An assessment of the predictive value of laboratory studies in the management of peripheral nerve injuries. M.D. Thesis University of Edinburgh
Glasby MA (1995) The control of posture and movement. In: Glasby MA, Huang CL-H (eds) Applied physiology for surgery and critical care. Butterworth Heinemann, Oxford
Jalinous R (2001) A guide to magnetic stimulation. The Magstim Company Ltd, UK
Kelleher MO, Tan G, Sarjeant R et al (2008) Predictive value of intraoperative neurophysiological monitoring during cervical spine surgery: a prospective analysis of 1055 consecutive patients. J Neurosurg Spine 8:215–221
Kimiskidis VK, Potoupnis M, Papagiannopoulos SK et al (2007) Idiopathic scoliosis: a transcranial magnetic stimulation study. J Musculoskelet Neuronal Interact 7:155–160
Kimura J (2001) Electrodiagnosis in diseases of nerve and muscle, 3rd edn. F. A. Davis, Philadelphia
Merton PA, Hill DK, Morton HB et al (1982) Scope of a technique for electrical stimulation of human brain, spinal cord, and muscle. Lancet 2:597–600
Morris SAC, Walsh P, Kane N et al (2014) The use of intraoperative monitoring during spinal deformity surgery. Bone Jt J (Orthopaed Proc) 96:29
Noonan KJ, Walker T, Feinberg JR et al (2002) Factors related to false- versus true-positive neuromonitoring changes in adolescent idiopathic scoliosis surgery. Spine (Phila Pa 1976) 27:825–830
Pastorelli F, Di Silvestre M, Plasmati R et al (2011) The prevention of neural complications in the surgical treatment of scoliosis: the role of the neurophysiological intraoperative monitoring. Eur Spine J 20 Suppl 1:S105–S114
Picht T, Schmidt S, Brandt S et al (2011) Preoperative functional mapping for rolandic brain tumor surgery: comparison of navigated transcranial magnetic stimulation to direct cortical stimulation. Neurosurgery 69:581–588 (discussion 8)
Schwartz DM, Auerbach JD, Dormans JP et al (2007) Neurophysiological detection of impending spinal cord injury during scoliosis surgery. J Bone Jt Surg (Am) 89:2440–2449
Sinclair C, Faulkner D, Hammond G (2006) Flexible real-time control of MagStim 200(2) units for use in transcranial magnetic stimulation studies. J Neurosci Methods 158:133–136
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Glasby, M.A., Tsirikos, A.I., Henderson, L. et al. Transcranial magnetic stimulation in the semi-quantitative, pre-operative assessment of patients undergoing spinal deformity surgery. Eur Spine J 26, 2103–2111 (2017). https://doi.org/10.1007/s00586-016-4737-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4737-4