Abstract
Purpose
Simpson grade II removal (coagulation of the dural attachment after gross total removal) of spinal meningioma is considered an acceptable alternative, but increased recurrence after more than 10 years has been reported. More attention must be paid to the long-term surgical outcomes after Simpson grade II removal.
Methods
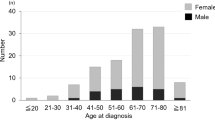
A retrospective review was performed for 20 patients (M:F = 5:15; age, 59 ± 9 years) with Simpson grade II removal (mean follow-up period, 12.9 years; range 10.0–17.5). Magnetic resonance (MR) imaging was conducted in 17 patients at 88 ± 52 months (range 12–157). During the same period, Simpson grade I removal (removal of the dural origin) was performed in 21 patients (follow-up, 89 ± 87 months; range 9–316). Radiological recurrence was defined as a visible tumor on a follow-up MR image, and clinical tumor recurrence was defined as the recurrence of symptoms.
Results
At the final follow-up, neurological symptoms had improved in 16/20 patients and remained stable in 4/20. A recurrent tumor was detected in one patient due to increased back pain at 92 months postoperative, but the symptom was stable without surgery until the last follow-up (124 months). The radiological and clinical recurrence-free survival periods were 150 ± 7 months (95 % CI 136–163) and 204 ± 6 months (95 % CI 193–215), respectively. There was no recurrence after Simpson grade I removal, whereas neurological deterioration occurred in two patients after surgery.
Conclusions
Simpson grade II removal may be an alternative option if the risk of complications with Simpson grade I removal is expected to be high.


Similar content being viewed by others
References
King AT, Sharr MM, Gullan RW, Bartlett JR (1998) Spinal meningiomas: a 20-year review. Br J Neurosurg 12:521–526
Solero CL, Fornari M, Giombini S, Lasio G, Oliveri G, Cimino C, Pluchino F (1989) Spinal meningiomas: review of 174 operated cases. Neurosurgery 25:153–160
Riad H, Knafo S, Segnarbieux F, Lonjon N (2013) Spinal meningiomas: surgical outcome and literature review. Neurochirurgie 59:30–34. doi:10.1016/j.neuchi.2012.10.137
Yoon SH, Chung CK, Jahng TA (2007) Surgical outcome of spinal canal meningiomas. J Korean Neurosurg Soc 42:300–304. doi:10.3340/jkns.2007.42.4.300
Nakamura M, Tsuji O, Fujiyoshi K, Hosogane N, Watanabe K, Tsuji T, Ishii K, Toyama Y, Chiba K, Matsumoto M (2012) Long-term surgical outcomes of spinal meningiomas. Spine 37:E617–E623. doi:10.1097/BRS.0b013e31824167f1
Cohen-Gadol AA, Zikel OM, Koch CA, Scheithauer BW, Krauss WE (2003) Spinal meningiomas in patients younger than 50 years of age: a 21-year experience. J Neurosurg 98:258–263
Kayaselcuk F, Zorludemir S, Bal N, Erdogan B, Erdogan S, Erman T (2004) The expression of survivin and Ki-67 in meningiomas: correlation with grade and clinical outcome. J Neurooncol 67:209–214
Yamasaki F, Yoshioka H, Hama S, Sugiyama K, Arita K, Kurisu K (2000) Recurrence of meningiomas. Cancer 89:1102–1110
Lanzafame S, Torrisi A, Barbagallo G, Emmanuele C, Alberio N, Albanese V (2000) Correlation between histological grade, MIB-1, p53, and recurrence in 69 completely resected primary intracranial meningiomas with a 6 year mean follow-up. Pathol Res Pract 196:483–488. doi:10.1016/S0344-0338(00)80050-3
Maiuri F, De Caro ML, de Divitiis O, Vergara P, Mariniello G (2011) Spinal meningiomas: age-related features. Clin Neurol Neurosurg 113:34–38. doi:10.1016/j.clineuro.2010.08.017
Roser F, Nakamura M, Bellinzona M, Ritz R, Ostertag H, Tatagiba MS (2006) Proliferation potential of spinal meningiomas. Eur Spine J 15:211–215. doi:10.1007/s00586-005-0937-z
Qi ST, Liu Y, Pan J, Chotai S, Fang LX (2012) A radiopathological classification of dural tail sign of meningiomas. J Neurosurg 117:645–653. doi:10.3171/2012.6.JNS111987
Prayson RA, Chamberlain WA, Angelov L (2010) Clear cell meningioma: a clinicopathologic study of 18 tumors and examination of the use of CD10, CA9, and RCC antibodies to distinguish between clear cell meningioma and metastatic clear cell renal cell carcinoma. AIMM 18:422–428. doi:10.1097/PAI.0b013e3181dd35d2
Schaller B (2005) Spinal meningioma: relationship between histological subtypes and surgical outcome? J Neurooncol 75:157–161
Kim CH, Chung CK (2011) Surgical outcome of a posterior approach for large ventral intradural extramedullary spinal cord tumors. Spine 36:E531–E537. doi:10.1097/BRS.0b013e3181dc8426
Voulgaris S, Alexiou GA, Mihos E, Karagiorgiadis D, Zigouris A, Fotakopoulos G, Drosos D, Pahaturidis D (2010) Posterior approach to ventrally located spinal meningiomas. Eur Spine J 19:1195–1199. doi:10.1007/s00586-010-1295-z
Setzer M, Vatter H, Marquardt G, Seifert V, Vrionis FD (2007) Management of spinal meningiomas: surgical results and a review of the literature. Neurosurg Focus 23:E14. doi:10.3171/FOC-07/10/E14
Klekamp J, Samii M (1999) Surgical results for spinal meningiomas. Surg Neurol 52:552–562. doi:10.1016/S0090-3019(99)00153-6
Simpson D (1957) The recurrence of intracranial meningiomas after surgical treatment. J Neurol Neurosurg Psychiatry 20:22–39
Lee SH, Chung CK, Kim CH, Yoon SH, Hyun SJ, Kim KJ, Kim ES, Eoh W, Kim HJ (2013) Long-term outcomes of surgical resection with or without adjuvant radiation therapy for treatment of spinal ependymoma: a retrospective multicenter study by the Korea Spinal Oncology Research Group. Neuro Oncol 15:921–929. doi:10.1093/neuonc/not038
Sohn S, Chung CK, Park SH, Kim ES, Kim KJ, Kim CH (2013) The fate of spinal schwannomas following subtotal resection: a retrospective multicenter study by the Korea spinal oncology research group. J Neurooncol 114:345–351. doi:10.1007/s11060-013-1190-7
McCormick PC, Torres R, Post KD, Stein BM (1990) Intramedullary ependymoma of the spinal cord. J Neurosurg 72:523–532. doi:10.3171/jns.1990.72.4.0523
Sohn S, Chung CK (2013) Conventional posterior approach without far lateral approach for ventral foramen magnum meningiomas. J Korean Neurosurg Soc 54:373–378. doi:10.3340/jkns.2013.54.5.373
Park SB, Jahng TA, Kim CH, Chung CK (2009) Thoracic and lumbar laminoplasty using a translaminar screw: morphometric study and technique. J Neurosurg Spine 10:603–609. doi:10.3171/2009.2.SPINE08257
Yamamuro K, Seichi A, Kimura A, Kikkawa I, Kojima M, Inoue H, Hoshino Y (2012) Histological investigation of resected dura mater attached to spinal meningioma. Spine 37:E1398–E1401. doi:10.1097/BRS.0b013e318268c419
Postalci L, Tugcu B, Gungor A, Guclu G (2011) Spinal meningiomas: recurrence in ventrally located individuals on long-term follow-up; a review of 46 operated cases. Turk Neurosurg 21:449–453. doi:10.5137/1019-5149.JTN.3518-10.2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure and funding source
This work was supported by the National Research Foundation of Korea (NRF) grant funded by the Korea government (MSIP) (No. 2010-0028631). The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. This study was approved by the institutional review board of the Seoul National University Hospital Clinical Research Institute (IRB No. 1306-106-500).
Additional information
On behalf of the Korea Spinal Oncology Research Group.
Rights and permissions
About this article
Cite this article
Kim, C.H., Chung, C.K., Lee, SH. et al. Long-term recurrence rates after the removal of spinal meningiomas in relation to Simpson grades. Eur Spine J 25, 4025–4032 (2016). https://doi.org/10.1007/s00586-015-4306-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4306-2