Abstract
Introduction
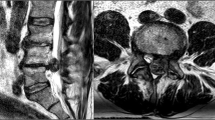
Postdural disc herniation has been documented rarely and the pathogenesis is still unknown. The average age of postdural disc herniations is between 50 and 60 years, and the sites most frequently affected by postdural lumbar disc herniations are L3–L4 and L4–L5, only less than 10 % in L5–S1. Although magnetic resonance imaging (MRI) is a useful tool in the diagnosis of this disease, the postdural disc herniation is usually misdiagnosed as extradural spine tumor preoperatively. The definitive diagnosis is made during operation or according to the postoperative pathology.
Methods
In this article, we described here a 48-year-old male patient who presented with intermittent pain in the low back and frequent urination for 4 years as well as hypesthesia and pain of the left lower extremity for 1 month.
Results
A standard total laminectomy was performed and the histopathological diagnosis was consistent with a degenerated intervertebral disc. The patient presented significant relief of the pain and of the neurological symptoms, but no improvement of frequent urination, in the postoperative period.
Conclusions
The diagnosis of postdural disc herniations is very difficult and mainly based on intraoperative and histopathological results. Early surgical intervention is important to relieve symptoms and prevent severe neurological deficits.



Similar content being viewed by others
References
Brock MPS, Mayer HM (1992) The form and structure of the extruded disc. Spine 17(12):1457–1461
Bonaroti EAWW (1998) Posterior epidural migration of an extruded lumbar disc fragment causing cauda equina syndrome clinical and magnetic resonance imaging evaluation. Spine 23(3):378–381
Schellinger DMH, Vidic B, Patronas NJ, Deveikis JP, Muraki AS, Abdullah DC (1990) Disk fragment migration. Radiology 175(3):831–836
Tarukado K, Tono O, Doi T (2014) Ordinary disc herniation changing into posterior epidural migration of lumbar disc fragments confirmed by magnetic resonance imaging: a case report of a successful endoscopic treatment. Asian Spine J 8(1):69–73
Lumbar VL (1973) spinal block by posterior rotation of anulus fibrosus. Case Rep J Neurosurg 39(5):642–647
Carvi y Nievas MN HH (2009) Unusual sequestered disc fragments simulating spinal tumors and other space-occupying lesions. Clinical article. J Neurosurg Spine 11(1):42–48
Kim JSLS, Arbatti NJ (2010) Dorsal extradural lumbar disc herniation causing cauda equina syndrome : a case report and review of literature. J Korean Neurosurg Soc 47(3):217–220
Robe PMD, Lenelle J, Stevenaert A (1999) Posterior epidural migration of sequestered lumbar disc fragments. Report of two cases. J Neurosurg 90(2 Suppl):264–266
ElAsri ACNO, Akhaddar A, Gazzaz M, Belhachmi A, El Mostarchid B, Boucetta M (2008) Posterior epidural migration of lumbar disk fragments: report of two cases and review of the literature. Surg Neurol 70(6):668–671
Teufack SGSH, Harrop J, Ratliff J (2010) Dorsal epidural intervertebral disk herniation with atypical radiographic findings: case report and literature review. J Spinal Cord Med 33(3):268–271
Akhaddar A, El-Asri A, Boucetta M (2011) Posterior epidural migration of a lumbar disc fragment: a series of 6 cases. J Neurosurg Spine 15(1):117–128
Sengoz A, Kotil K, Tasdemiroglu E (2011) Posterior epidural migration of herniated lumbar disc fragment. J Neurosurg Spine 14(3):313–317
Dösoğlu MIM, Gezen F, Ziyal MI (2001) Posterior epidural migration of a lumbar disc fragment causing cauda equina syndrome—case report and review of the relevant literature. Eur Spine J 10(4):348–351
Manabe S (1986) A. T. Epidural migration of extruded cervical disc and its surgical treatment. Spine 11(9):873–878
Chow GH GJ, Brown CW (1996) Multifocal metachronous epidural abscesses of the spine. A case report. Spine (Phila Pa 1976) 21(9):1094–1097
Bonaldi VMDH, Starr MR, Sarazin L, Richardson J (1996) Tophaceous gout of the lumbar spine mimicking an epidural abscess: MR features. AJNR Am J Neuroradiol 17(10):1949–1952
Neugroschl CKP, Gigaud M, Ragragui O, Maitrot D, Manelfe C, Dietemann JL (1999) Posterior extradural migration of extruded thoracic and lumbar disc fragments: role of MRI. Neuroradiology 41(9):630–635
Kuzeyli K CE, Usul H, Baykal S, Yazar U, karaarslan G, Arslan E, Peksoylu B (2003) Posterior Epidural migration of lumbar disc fragments—report of three cases. Spine 28(3):E64–E67
Tatli M, Güzel A, Ceviz A, Karadağ O (2005) Posterior epidural migration of sequestered lumbar disc fragment causing cauda equina syndrome.pdf. Br J Neurosurg 19(3):257–259
DE Sakas FM, Young S, Toland J (1995) Posterior thecal lumbar disc herniation mimicking synovial cyst. Neuroradiology 37(3):192–194
Tatter SBCG (1994) Hemorrhage into a lumbar synovial cyst causing an acute cauda equina syndrome. Case report. J Neurosurg 81(3):449–452
Baker JK HG (1994) Cyst of the ligamentum flavum. Spine (Phila Pa 1976) 19(9):1092–1094
Hu HPHQ (1992) Posterior epidural migration of sequestered lumbar disc fragments. Report of two cases. Neuroradiology 34(2):98–102
D’Andrea GTG, Roperto R, Celli P, Orlando ER, Ferrante L (2004) Intradural lumbar disc herniations: the role of MRI in preoperative diagnosis and review of the literature. Neurosurg Rev 27(2):75–80
Lakshmanan P, Ahuja S, Lyons K, Howes J, Davies PR (2006) Sequestrated lumbar intervertebral disc in the posterior epidural space: a report on two cases and review of the literature. Spine J Off J North Am Spine Soc 6(5):583–586
Wasserstrom RMA, Black JF, Lehman RA (1993) Intradural lumbar disk fragment with ring enhancement on MR. AJNR Am J Neuroradiol. 14(2):401–404
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any potential conflict of interest.
Rights and permissions
About this article
Cite this article
Li, K., Li, Z., Geng, W. et al. Postdural disc herniation at L5/S1 level mimicking an extradural spinal tumor. Eur Spine J 25 (Suppl 1), 80–83 (2016). https://doi.org/10.1007/s00586-015-4125-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4125-5