Abstract
Purpose
The object of this study was to compare minimally invasive surgery (MIS) with open surgery in a severely affected subgroup of degenerative spondylolisthetic patients with severe stenosis (SDS) and high-grade facet osteoarthritis (FJO).
Methods
From January 2009 to February 2010, 49 patients with severe SDS and high-grade FJO were treated using either MIS or open TLIF. Intraoperative and diagnostic data, including perioperative complications and length of hospital stay (LOS), were collected, using retrospective chart review. Surgical short- and long-term outcomes were assessed according to the Oswestry disability index (ODI) and visual analog scale (VAS) for back and leg pain.
Results
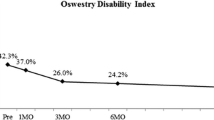
Comparing MIS and open surgery, the MIS group had lesser blood loss, significantly lesser need for transfusion (p = 0.02), more rapid improvement of postoperative back pain in the first 6 weeks of follow-up and a shorter LOS. On the other hand, we experienced in the MIS group a longer operative time. The distribution on the postoperative ODI (p = 0.841), VAS leg (p = 0.943) and back pain (p = 0.735) scores after a mean follow-up of 2 years were similar. The overall proportion of complications showed no significant difference between the groups (29 % in the MIS group vs. 28 % in the open group, p = 0.999).
Conclusion
Minimally invasive surgery for severe SDS leads to adequate and safe decompression of lumbar stenosis and results in a faster recovery of symptoms and disability in the early postoperative period.


Similar content being viewed by others
Abbreviations
- CSF:
-
Cerebrospinal fluid
- CT:
-
Computerized tomography
- EBL:
-
Estimated blood loss
- FJO:
-
Facet joint osteoarthritis
- LBP:
-
Low back pain
- LOS:
-
Length of hospital stay
- MR:
-
Magnetic resonance
- MIS:
-
Minimally invasive surgery
- TLIF:
-
Transforaminal interbody fusion
- SD:
-
Standard deviation
- SDS:
-
Stenotic degenerative spondylolisthesis
- VAS:
-
Visual analog scale
References
Dhall SS, Wang MY, Mummaneni PV (2008) Clinical and radiographic comparison of mini-open transforaminal lumbar interbody fusion with open transforaminal lumbar interbody fusion in 42 patients with long-term follow-up. J Neurosurg Spine 9(6):560–565
Gelalis ID, Arnaoutoglou C, Christoforou G, Lykissas MG, Batsilas I, Xenakis T (2010) Prospective analysis of surgical outcomes in patients undergoing decompressive laminectomy and posterior instrumentation for degenerative lumbar spinal stenosis. Acta Orthop Traumatol Turc 44(3):235–240
Holly LT, Schwender JD, Rouben DP, Foley KT (2006) Minimally invasive transforaminal lumbar interbody fusion: indications, technique, and complications. Neurosurg Focus 20(3):E6
Hsieh PC, Koski TR, Sciubba DM, Moller DJ, O’Shaughnessy BA, Li KW, Gokaslan ZL, Ondra SL, Fessler RG, Liu JC (2008) Maximizing the potential of minimally invasive spine surgery in complex spinal disorders. Neurosurg Focus 25(2):E19
Logroscino CA, Proietti L, Pola E, Scaramuzzo L, Tamburrelli FC (2011) A minimally invasive posterior lumbar interbody fusion for degenerative lumbar spine instabilities. Eur Spine J 20(Suppl 1):S41–S45
Lowe TG, Tahernia AD, O’Brien MF, Smith DA (2002) Unilateral transforaminal posterior lumbar interbody fusion (TLIF): indications, technique, and 2-year results. J Spinal Disord Tech 15(1):31–38
Mummaneni PV, Rodts GE Jr (2005) The mini-open transforaminal lumbar interbody fusion. Neurosurgery 57(4 Suppl):256–261
Oppenheimer JH, De Castro I, McDonnell DE (2009) Minimally invasive spine technology and minimally invasive spine surgery: a historical review. Neurosurg Focus 27(3):E9
Park P, Foley KT (2008) Minimally invasive transforaminal lumbar interbody fusion with reduction of spondylolisthesis: technique and outcomes after a minimum of 2 years’ follow-up. Neurosurg Focus 25(2):E16
Park Y, Ha JW, Lee YT, Oh HC, Yoo JH, Kim HB (2011) Surgical outcomes of minimally invasive transforaminal lumbar interbody fusion for the treatment of spondylolisthesis and degenerative segmental instability. Asian Spine J 5(4):228–236
Pathria M, Sartoris DJ, Resnick D (1987) Osteoarthritis of the facet joints: accuracy of oblique radiographic assessment. Radiology 164(1):227–230
Peng CW, Yue WM, Poh SY, Yeo W, Tan SB (2009) Clinical and radiological outcomes of minimally invasive versus open transforaminal lumbar interbody fusion. Spine 34(13):1385–1389
Potter BK, Freedman BA, Verwiebe EG, Hall JM, Polly DW Jr, Kuklo TR (2005) Transforaminal lumbar interbody fusion: clinical and radiographic results and complications in 100 consecutive patients. J Spinal Disord Tech 18:337–346
Quante M, Kesten H, Richter A, Halm H (2012) Transforaminal lumbar interbody fusion for the treatment of degenerative spondylolisthesis. Orthopade 41(2):153–162
Rosenberg WS, Mummaneni PV (2001) TLIF: technique, complications, and early results. Neurosurgery 48:569–574
Ryang YM, Oertel MF, Mayfrank L, Gilsbach JM, Rohde V (2008) Standard open microdiscectomy versus minimal access trocar microdiscectomy: results of a prospective randomized study. Neurosurgery 62(1):174–181
Salehi SA, Tawk R, Ganju A, LaMarca F, Liu JC, Ondra SL (2004) Transforaminal lumbar interbody fusion: surgical technique and results in 24 patients. Neurosurgery 54:368–374
Scheufler KM, Dohmen H, Vougioukas VI (2007) Percutaneous transforaminal lumbar interbody fusion for the treatment of degenerative lumbar instability. Neurosurgery 60(4 Suppl 2):203–212
Schizas C, Michel J, Kosmopoulos V, Theumann N (2007) Computer tomography assessment of pedicle screw insertion in percutaneous posterior transpedicular stabilization. EurSpine J 16(5):613–617
Schizas C, Theumann N, Burn A, Tansey R, Wardlaw D, Smith FW, Kulik G (2010) Qualitative grading of severity of lumbar spinal stenosis based on the morphology of the dural sac on magnetic resonance images. Spine (Phila Pa 1976) 35(21):1919–1924
Schwender JD, Holly LT, Rouben DP, Foley KT (2005) Minimally invasive transforaminal lumbar interbody fusion (TLIF): technical feasibility and initial results. J Spinal Disord Tech 18(Suppl):S1–S6
Scott J, Huskisson EC (1976) Graphic representation of pain. Pain 2(2):175–184
Wang J, Zhou Y, Zhang ZF, Li CQ, Zheng WJ, Liu J (2010) Comparison of one-level minimally invasive and open transforaminal lumbar interbody fusion in degenerative and isthmic spondylolisthesis grades 1 and 2. Eur Spine J 19(10):1780–1784
Wang MY, Cummock MD, Yu Y, Trivedi RA (2010) An analysis of the differences in the acute hospitalization charges following minimally invasive versus open posterior lumbar interbody fusion. J Neurosurg Spine 12(6):694–699
Weiner BK, Nguyen HV, Hazard SW (2006) Transforaminal lumbar interbody fusion: an independent assessment of outcomes in a difficult patient population. Med Sci Monit 12:CR99–CR102
Weinstein JN, Lurie JD, Tosteson TD, Zhao W, Blood EA, Tosteson AN, Birkmeyer N, Herkowitz H, Longley M, Lenke L, Emery S, Hu SS (2009) Surgical compared with non operative treatment for lumbar degenerative spondylolisthesis. Four-year results in the Spine Patient Outcomes Research Trial (SPORT) randomized and observational cohorts. J Bone Joint Surg Am 91(6):1295–1304
Whitecloud TS 3rd, Davis JM, Olive PM (1994) Operative treatment of the degenerated segment adjacent to a lumbar fusion. Spine (Phila Pa 1976) 19(5):531–536
Whitecloud TS 3rd, Roesch WW, Ricciardi JE (2001) Transforaminal interbody fusion versus anterior-posterior interbody fusion of the lumbar spine: a financial analysis. J Spinal Disord 14(2):100–103
Wood MJ, Mannion RJ (2010) Improving accuracy and reducing radiation exposure in minimally invasive lumbar interbody fusion. J Neurosurg Spine 12(5):533–539
Conflict of interest
The authors report no conflict of interest concerning the materials and methods used in this study or the findings specified in this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Archavlis, E., Carvi y Nievas, M. Comparison of minimally invasive fusion and instrumentation versus open surgery for severe stenotic spondylolisthesis with high-grade facet joint osteoarthritis. Eur Spine J 22, 1731–1740 (2013). https://doi.org/10.1007/s00586-013-2732-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2732-6