Abstract
Purpose
To gain insight into a new technology, a novel facet arthroplasty device (TFAS) was compared to a rigid posterior fixation system (UCR). The axial and bending loads through the implants and at the bone-implant interfaces were evaluated using an ex vivo biomechanical study and matched finite element analysis. Kinematic behaviour has been reported for TFAS, but implant loads have not. Implant loads are important indicators of an implant’s performance and safety. The rigid posterior fixation system is used for comparison due to the extensive information available about these systems.
Methods
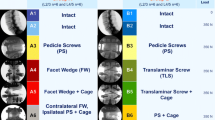
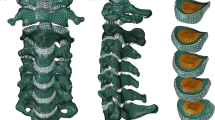
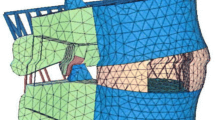
Unconstrained pure moments were applied to 13 L3–S1 cadaveric spine segments. Specimens were tested intact, following decompression, UCR fixation and TFAS implantation at L4–L5. UCR fixation was via standard pedicle screws and TFAS implantation was via PMMA-cemented transpedicular stems. Three-dimensional 10 Nm moments and a 600 N follower load were applied; L4–L5 disc pressures and implant loads were measured using a pressure sensor and strain gauges, respectively. A finite element model was used to calculate TFAS bone-implant interface loads.
Results
UCR experienced greater implant loads in extension (p < 0.004) and lateral bending (p < 0.02). Under flexion, TFAS was subject to greater implant moments (p < 0.04). At the bone-implant interface, flexion resulted in the smallest TFAS (average = 0.20 Nm) but greatest UCR (1.18 Nm) moment and axial rotation resulted in the greatest TFAS (3.10 Nm) and smallest UCR (0.40 Nm) moments. Disc pressures were similar to intact for TFAS but not for UCR (p < 0.04).
Conclusions
These results are most applicable to the immediate post-operative period prior to remodelling of the bone-implant interface since the UCR and TFAS implants are intended for different service lives (UCR—until fusion, TFAS—indefinitely). TFAS reproduced intact-like anterior column load-sharing—as measured by disc pressure. The highest bone-implant moment of 3.1 Nm was measured in TFAS and for the same loading condition the UCR interface moment was considerably lower (0.4 Nm). For other loading conditions, the differences between TFAS and UCR were smaller, with the UCR sometimes having larger values and for others the TFAS was larger. The long-term physiological meaning of these findings is unknown and demonstrates the need for a better understanding of the relationship between spinal arthroplasty devices and the host tissue as development of next generation motion-preserving posterior devices that hope to more accurately replicate the natural functions of the native tissue continues.





Similar content being viewed by others
References
Acosta FL Jr, Aryan HE, Ames CP (2005) Emerging directions in motion preservation spinal surgery. Neurosurg Clin N Am 16(4):665–669, vii
Mayer HM, Korge A (2002) Non-fusion technology in degenerative lumbar spinal disorders: Facts, questions, challenges. Eur Spine J 11(Suppl 2):S85–S91
Singh K, An HS (2006) Motion preservation technologies: alternatives to spinal fusion. Am J Orthop 35(9):411–416
Ghiselli G, Wang JC, Bhatia NN, Hsu WK, Dawson EG (2004) Adjacent segment degeneration in the lumbar spine. J Bone Joint Surg Am 86-A(7):1497–1503
Hilibrand AS, Robbins M (2004) Adjacent segment degeneration and adjacent segment disease: the consequences of spinal fusion? Spine J 4(6 Suppl):190S–194S
Park P, Garton HJ, Gala VC, Hoff JT, McGillicuddy JE (2004) Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine 29(17):1938–1944
Crawford NR (2005) Biomechanics of lumbar arthroplasty. Neurosurg Clin N Am 16(4):595–602, v
Cunningham BW (2004) Basic scientific considerations in total disc arthroplasty. Spine J 4(6 Suppl):219S–230S
Cunningham BW, Gordon JD, Dmitriev AE, Hu N, McAfee PC (2003) Biomechanical evaluation of total disc replacement arthroplasty: an in vitro human cadaveric model. Spine 28(20):S110–S117
Galbusera F, Fantigrossi A, Raimondi MT, Sassi M, Fornari M, Assietti R (2006) Biomechanics of the c5–c6 spinal unit before and after placement of a disc prosthesis. Biomech Model Mechanobiol 5(4):253–261
Goel VK, Grauer JN, Patel T, Biyani A, Sairyo K, Vishnubhotla S, Matyas A, Cowgill I, Shaw M, Long R, Dick D, Panjabi MM, Serhan H (2005) Effects of charite artificial disc on the implanted and adjacent spinal segments mechanics using a hybrid testing protocol. Spine 30(24):2755–2764
Atlas SJ, Delitto A (2006) Spinal stenosis: surgical versus nonsurgical treatment. Clin Orthop Relat Res 443:198–207
Wilke HJ, Schmidt H, Werner K, Schmolz W, Drumm J (2006) Biomechanical evaluation of a new total posterior-element replacement system. Spine 31(24):2790–2796 (discussion 2797)
Zhu Q, Larson CR, Sjovold SG, Rosler DM, Keynan O, Wilson DR, Cripton PA, Oxland TR (2007) Biomechanical evaluation of the total facet arthroplasty system: 3-dimensional kinematics. Spine 32(1):55–62
Goel VK, Panjabi MM, Patwardhan AG, Dooris AP, Serhan H (2006) Test protocols for evaluation of spinal implants. J Bone Joint Surg Am 88(Suppl 2):103–109
DiAngelo DJ, Foley KT, Morrow BR, Schwab JS, Song J, German JW, Blair E (2004) In vitro biomechanics of cervical disc arthroplasty with the prodisc-c total disc implant. Neurosurg Focus 17(3):E7
Denoziere G, Ku DN (2006) Biomechanical comparison between fusion of two vertebrae and implantation of an artificial intervertebral disc. J Biomech 39(4):766–775
Goel VK, Kiapour A, Faizan A, Krishna M, Friesem T (2007) Finite element study of matched paired posterior disc implant and dynamic stabilizer (360 motion preservation system). SAS J 01(01):55–62
Chang BS, Brown PR, Sieber A, Valdevit A, Tateno K, Kostuik JP (2004) Evaluation of the biological response of wear debris. Spine J 4(6 Suppl):239S–244S
Jacobs JJ, Hallab NJ, Urban RM, Wimmer MA (2006) Wear particles. J Bone Joint Surg Am 88(Suppl 2):99–102
Goel VK, Mehta A, Jangra J, Faizan A, Kiapour A, Hoy RW, Fauth AR (2007) Anatomic facet replacement system (afrs) restoration of lumbar segment mechanics to intact: a finite element study and in vitro cadaver investigation. SAS J 01(01):46–54
Yang KH, King AI (1984) Mechanism of facet load transmission as a hypothesis for low-back pain. Spine 9(6):557–565
Zhu QA, Park YB, Sjovold SG, Niosi CA, Wilson DC, Cripton PA, Oxland TR (2008) Can extra-articular strains be used to measure facet contact forces in the lumbar spine? An in vitro biomechanical study. Proc Inst Mech Eng [H] 222(2):171–184
Goertzen DJ, Lane C, Oxland TR (2004) Neutral zone and range of motion in the spine are greater with stepwise loading than with a continuous loading protocol. An in vitro porcine investigation. J Biomech 37(2):257–261
Cripton PA, Bruehlmann SB, Orr TE, Oxland TR, Nolte LP (2000) In vitro axial preload application during spine flexibility testing: Towards reduced apparatus-related artefacts. J Biomech 33(12):1559–1568
Patwardhan AG, Havey RM, Carandang G, Simonds J, Voronov LI, Ghanayem AJ, Meade KP, Gavin TM, Paxinos O (2003) Effect of compressive follower preload on the flexion-extension response of the human lumbar spine. J Orthop Res 21(3):540–546
Cripton PA, Jain GM, Wittenberg RH, Nolte LP (2000) Load-sharing characteristics of stabilized lumbar spine segments. Spine 25(2):170–179
Frei H, Oxland TR, Nolte LP (2002) Thoracolumbar spine mechanics contrasted under compression and shear loading. J Orthop Res 20(6):1333–1338
Steffen T, Baramki HG, Rubin R, Antoniou J, Aebi M (1998) Lumbar intradiscal pressure measured in the anterior and posterolateral annular regions during asymmetrical loading. Clin Biomech (Bristol, Avon) 13(7):495–505
Perry CC (2003) Separate measurements of combined loads. http://www.vishay.com/brands/measurements_group/guide/ta/msg/msg.htm
Carpenter Technology Corporation (2000) Titanium Alloy Ti 6Al-4V [Technical Datasheet]. http://cartech.ides.com/datasheet.aspx?i=101&E=269 (7/01/2000)
Carpenter Technology Corporation (2007) BioDur Carpenter CCM Alloy [Technical Datasheet]. http://cartech.ides.com/datasheet.aspx?i=101&E=8 (1/18/2007)
Elliott DM, Setton LA (2001) Anisotropic and inhomogeneous tensile behavior of the human anulus fibrosus: experimental measurement and material model predictions. J Biomech Eng 123(3):256–263
Kumaresan S, Yoganandan N, Pintar FA, Maiman DJ (1999) Finite element modeling of the cervical spine: role of intervertebral disc under axial and eccentric loads. Med Eng Phys 21(10):689–700
Lewis G (2003) Fatigue testing and performance of acrylic bone-cement materials: state-of-the-art review. J Biomed Mater Res B Appl Biomater 66(1):457–486
Morgan EF, Bayraktar HH, Keaveny TM (2003) Trabecular bone modulus-density relationships depend on anatomic site. J Biomech 36(7):897–904
Polikeit A, Nolte LP, Ferguson SJ (2003) The effect of cement augmentation on the load transfer in an osteoporotic functional spinal unit: finite-element analysis. Spine 28(10):991–996
Silva MJ, Keaveny TM, Hayes WC (1997) Load sharing between the shell and centrum in the lumbar vertebral body. Spine 22(2):140–150
Kumaresan S, Yoganandan N, Pintar FA (1999) Finite element analysis of the cervical spine: a material property sensitivity study. Clin Biomech (Bristol, Avon) 14(1):41–53
Polikeit A, Ferguson SJ, Nolte LP, Orr TE (2003) Factors influencing stresses in the lumbar spine after the insertion of intervertebral cages: finite element analysis. Eur Spine J 12(4):413–420
Webb S (2006) Chapter 46: Total facet arthroplasty system (tfas). In: Kim DH, Cammisa FP, Fessler RG (eds) Dynamic reconstruction of the spine. Thieme, New York, p xix
Haberl H, Cripton PA, Orr TE, Beutler T, Frei H, Lanksch WR, Nolte LP (2004) Kinematic response of lumbar functional spinal units to axial torsion with and without superimposed compression and flexion/extension. Eur Spine J 13(6):560–566
Rohlmann A, Riley LH, Bergmann G, Graichen F (1996) In vitro load measurement using an instrumented spinal fixation device. Med Eng Phys 18(6):485–488
Rohlmann A, Bergmann G, Graichen F (1997) Loads on an internal spinal fixation device during walking. J Biomech 30(1):41–47
Rohlmann A, Bergmann G, Graichen F, Weber U (1997) Comparison of loads on internal spinal fixation devices measured in vitro and in vivo. Med Eng Phys 19(6):539–546
Rohlmann A, Graichen F, Weber U, Bergmann G (2000) 2000 volvo award winner in biomechanical studies: Monitoring in vivo implant loads with a telemeterized internal spinal fixation device. Spine 25(23):2981–2986
Renner SM, Lim TH, Kim WJ, Katolik L, An HS, Andersson GB (2004) Augmentation of pedicle screw fixation strength using an injectable calcium phosphate cement as a function of injection timing and method. Spine 29(11):E212–E216
Tan JS, Kwon BK, Dvorak MF, Fisher CG, Oxland TR (2004) Pedicle screw motion in the osteoporotic spine after augmentation with laminar hooks, sublaminar wires, or calcium phosphate cement: A comparative analysis. Spine 29(16):1723–1730
Wittenberg RH, Lee KS, Shea M, White AA 3rd, Hayes WC (1993) Effect of screw diameter, insertion technique, and bone cement augmentation of pedicular screw fixation strength. Clin Orthop Relat Res 296:278–287
Cholewicki J, McGill SM, Norman RW (1995) Comparison of muscle forces and joint load from an optimization and emg assisted lumbar spine model: towards development of a hybrid approach. J Biomech 28(3):321–331
Reeves NP, Cholewicki J (2003) Modeling the human lumbar spine for assessing spinal loads, stability, and risk of injury. Crit Rev Biomed Eng 31(1–2):73–139
Wilke HJ, Neef P, Caimi M, Hoogland T, Claes LE (1999) New in vivo measurements of pressures in the intervertebral disc in daily life. Spine 24(8):755–762
Wilke HJ, Rohlmann A, Neller S, Graichen F, Claes L, Bergmann G (2003) Issls prize winner: a novel approach to determine trunk muscle forces during flexion and extension: a comparison of data from an in vitro experiment and in vivo measurements. Spine 28(23):2585–2593
Acknowledgments
Financial support in the form of a research grant from Archus Orthopedics, Redmond, Washington is gratefully acknowledged. We also thank Dr. Thomas Oxland for invaluable comments and suggestions on the manuscript.
Conflict of interest
AB and MLV are employees of Exponent and JAO and DMR are employees of Archus. Exponent received consulting income from Archus. All other authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sjovold, S.G., Zhu, Q., Bowden, A. et al. Biomechanical evaluation of the Total Facet Arthroplasty System® (TFAS®): loading as compared to a rigid posterior instrumentation system. Eur Spine J 21, 1660–1673 (2012). https://doi.org/10.1007/s00586-012-2253-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2253-8