Abstract.
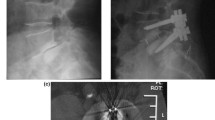
The aim of this study was to evaluate the short-term radiological and functional outcome of surgical treatment for symptomatic, low-grade, adult isthmic spondylolisthesis. Twelve patients underwent a monosegmental fusion for symptomatic spondylolisthesis. Posterior reduction with pedicle screw instrumentation was followed by second-stage anterior interbody fusion with a cage. All patients underwent a decompressive laminectomy. At an average of 2.1 (range 1.4–3.0) years following surgery, all patients completed the Oswestry questionnaire, VAS back pain score and a questionnaire detailing their work status. Radiographs were evaluated for maintenance of reduction and fusion. The patients (nine male, three female; mean age 42, range 22–54 years) had experienced preoperative symptoms for an average of 38 (range 6–96) months. An average preoperative slip of 21% (range 11–36%) was reduced to 7% (range 0–17%). Reduction of slip was maintained at latest follow-up, at which time the average VAS score was 2.8 (range 0–8) and the average Oswestry score was 13 (range 0–32). All patients achieved a successful fusion. There were no postoperative nerve root deficits. All patients stated that they would be prepared to undergo the same procedure again if required. Seventy-five percent returned to their pre-symptom work status. Our findings suggest that posterior reduction and anterior fusion for low-grade adult isthmic spondylolisthesis may yield good functional short-term results. A high fusion rate and maintenance of reduction with a low complication rate may be expected. Further follow-up is necessary to evaluate long-term outcome.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Electronic Publication
Rights and permissions
About this article
Cite this article
Spruit, .M., Pavlov, .P., Leitao, .J. et al. Posterior reduction and anterior lumbar interbody fusion in symptomatic low-grade adult isthmic spondylolisthesis: short-term radiological and functional outcome. Eur Spine J 11, 428–433 (2002). https://doi.org/10.1007/s00586-002-0400-3
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00586-002-0400-3