Abstract
Purpose
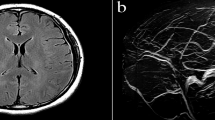
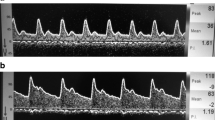
Post-dural puncture headache (PDPH) may be resulted from significant changes in cerebral blood flow, which could be visualized by Transcranial Doppler (TCD). This study was performed to investigate if TCD can be used to predict the occurrence of PDPH in high-risk patients.
Methods
This prospective observational study was conducted on ninety ASA I and II pregnant females undergoing elective cesarean section (CS) under spinal anesthesia. TCD was performed to all patients within 24 h before the operation, at 24 h and 48 h in the post-operative period to measure mean velocity (MV) and Gosling pulsatility index (PI) in the right middle cerebral artery. For 5 days postoperatively, all patients were assessed and the PDPH patients were identified, their pre- and post-puncture TCD measurements were compared with the corresponding measurements of PDPH-free patients and ROC analysis was done to evaluate the predictive value of TCD parameters.
Results
17 patients (18.8%) developed PDPH. PDPH group was significantly higher regarding MV and significantly lower with regard to PI at all times except for the pre-spinal PI. The MV values in all patients showed statistical significant increase within the first 48 h after CS as compared with those before delivery. In PDPH group there was high statistical significant decrease in PI values at 24 h and 48 h compared to the pre-puncture values. The pre-puncture MV was the parameter of the best accuracy for predicting PDPH with a cutoff of MV > 68.4 cm/s and the post-puncture PI at 24 h was the best predictive of PDPH with a cutoff value of < 0.75.
Conclusion
TCD might prove a useful tool in predicting PDPH suggesting that higher pre-puncture MV with a cutoff value > 68.4 cm/s and post-puncture lower PI at 24 h with a cutoff < 0.75 are the best predictive parameters.
Trial registration
This clinical trial was registered with ClinicalTrials.gov (NCT03464253).




Similar content being viewed by others
References
Mohammed EL, El Shal SM. Efficacy of different size Quincke spinal needles in reduction of incidence of post-dural puncture headache (PDPH) in Caesarean section (CS) randomized controlled study. Egypt J Anaesth. 2017;33(1):53–8.
Isikay CT, Uzuner N, Gucuyener D, Ozdemir G. The effects of hematocrit and age on transcranial Doppler measurements in patients with recent ischemic stroke. Neurol India. 2005;53(1):51–4.
Bardon J, Ray C LE, Samama CM, Bonnet MP. Risk factors of post-dural puncture headache receiving a blood-patch in the obstetric patients. Minerva Anestesiol. 2016;82(6):641–8.
Sachs A, Smiley R. Post-dural puncture headache: the worst common complication in obstetric anesthesia. Semin Perinatol. 2014;38(6):386–94.
Peralta F, Higgins N, Lange E, Wong CA, McCarthy RJ. The relationship of body mass index with the incidence of postdural puncture headache in parturients. Anesth Analg. 2015;121(2):451–6.
Macario A, Scibetta WC, Navarro J, Riley E. Analgesia for labor pain: a cost model. Anesthesiology. 2000;92(3):841–50.
Schievink WI. Spontaneous spinal cerebral spinal fluid leaks and intracranial hypotension. JAMA. 2006;295(19):2286–96.
Kracoff SL, Kotlovker V. Post dural puncture headache—review and suggested new treatment. Open J Anesth. 2016;6:148–63.
Venturelli PM, Brunser AM, Gaete J, Illanes S, López J, Olavarría VV, Reccius A, Brinck P, González F, Cavada G, Lavados PM. Reliability of hand-held transcranial doppler with m-mode ultrasound in middle cerebral artery measurement. J Med Ultrasound. 2017;25(2):76–81.
Vadhera RB, Babazade R, Suresh MS, Alvarado MC, Cruz AL, Belfort MA. Role of transcranial Doppler measurements in postpartum patients with post-dural puncture headache: a pilot study. Int J Obstet Anesth. 2017;29:90–1.
Bathala L, Mehndiratta MM, Sharma VK. Transcranial Doppler: Technique and common findings (part 1). Ann Indian Acad Neurol. 2013;16(2):174–9.
Nowaczewska M, Ksiazkiewicz B. Cerebral blood flow characteristics in patients with post-lumbar puncture headache. J Neurol. 2012;259(4):665–9.
Headache classification subcommittee of the International Headache Society. The international classification of headache disorders, 2nd edition. Cephalalgia. 2004;24(1):9–160.
Ghosh S, Nayak SK, Roy S. Assessment of post dural puncture headache in patients undergoing caesarean section: a comparison between 25 G Quinke V/S whitacre needles. BJMMR. 2017;19(9):1–7.
Gobel H, Klostermann H, Lindner V, Schenkl S. Changes in cerebral haemodynamics in cases of post-lumbar puncture headache: a prospective transcranial Doppler ultrasound study. Cephalalgia. 1990;10(3):117–22.
Bellner J, Romner B, Reinstrup P, Kristiansson KA, Ryding E, Brandt L. Transcranial Doppler sonography pulsatility index (PI) reflects intracranial pressure (ICP). Surg Neurol. 2004;62(1):45–51.
Cipolla MJ. The adaptation of the cerebral circulation to pregnancy: mechanisms and consequences. J Cereb Blood Flow Metab. 2013;33(4):465–78.
Serra-Serra V, Kyle PM, Chandran R, Redman CW. Maternal middle cerebral artery velocimetry in normal pregnancy and postpartum. Br J Obstet Gynaecol. 1997;104(8):904–9.
Batur Caglayan HZ, Nazliel B, Cinar M, Ataoglu E, Moraloglu O, Irkec C. Assessment of maternal cerebral blood flow velocity by transcranial Doppler ultrasound before delivery and in the early postpartum period. J Matern Fetal Neonatal Med. 2019;32(4):584–9.
Anzola GP, Brighenti R, Cobelli M, Giossi A, Mazzucco S, Olivato S, Pari E, Piras MP, Padovani A, Rinaldi F, Turri G. Cerebral haemodynamics in early puerperium: a prospective study. Ultrasound. 2017;25(2):107–14.
Williams K, Galerneau F. Maternal transcranial Doppler in pre-eclampsia and eclampsia. Ultrasound Obstet Gynecol. 2003;21(5):507–13.
Demarin V, Rundek T, Hodek B. Maternal cerebral circulation in normal and abnormal pregnancies. Acta Obstet Gynecol Scand. 1997;76(7):619–24.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest.
About this article
Cite this article
Mowafy, S.M.S., Abd Ellatif, S.E. Transcranial Doppler role in prediction of post-dural puncture headache in parturients undergoing elective cesarean section: prospective observational study. J Anesth 33, 426–434 (2019). https://doi.org/10.1007/s00540-019-02652-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-019-02652-2