Abstract
Purpose
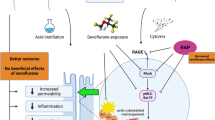
The glycocalyx is a glycoprotein-polysaccaride layer covering the endothelium luminal surface, and plays a key regulatory role in several endothelial functions. Lung ischemia reperfusion (IR) is a clinical entity that occurs in everyday thoracic surgery and causes glycocalix destruction and a florid local and systemic immune response. Moreover, sevoflurane is able to modulate the inflammatory response triggered by IR lung injury. In this study, we evaluated the protective effects of sevoflurane on the pulmonary endothelial glycocalyx in an in-vivo lung autotransplant model in pigs.
Methods
Sixteen Large White pigs underwent pneumonectomy plus lung autotransplant. They were divided into two groups depending on the hypnotic agent received (propofol or anesthetic preconditioning with sevoflurane). Glycocalyx components (syndecan-1 and heparan sulphate), cathepsin B, chemokines (MCP-1, MIP-1, and MIP-2) and adhesion molecules (VCAM and ICAM-1) were measured at four different timepoints using porcine-specific enzyme-linked immunosorbent assay (ELISA) kits.
Results
There were no differences between groups in weight or in surgical and one-lung ventilation time. Greater glycocalyx destruction and higher chemokine and adhesion molecule expression were observed in the group that did not receive sevoflurane. Heparan sulphate and serum syndecan levels were higher in the propofol group (P < 0.0001) after reperfusion, as was cathepsin B activity (P < 0.015). MCP-1, MIP-1, MIP-2, VCAM, and ICAM-1 levels were also higher in the propofol group (P < 0.006).
Conclusion
Sevoflurane preconditioning protects pulmonary glycocalyx and reduces expression of leukocyte chemokines in an in-vivo model of pulmonary IR.
Similar content being viewed by others
References
Danielli JF. Capillary permeability and oedema in the perfused frog. J Physiol. 1940;98(1):109–29.
Bennett HS, Luft JH, Hampton JC. Morphological classifications of vertebrate blood capillaries. Am J Physiol. 1959;196(2):381–90.
O’Callaghan R, Job KM, Dull RO, Hlady V. Stiffness and heterogeneity of the pulmonary endothelial glycocalyx measured by atomic force microscopy. Am J Physiol Lung Cell Mol Physiol. 2011;301(3):L353–60.
Oo YH, Adams DH. The role of chemokines in the recruitment of lymphocytes to the liver. J Autoimmun. 2010;34(1):45–54.
Klinke A, Nussbaum C, Kubala L, Friedrichs K, Rudolph TK, Rudolph V. Myeloperoxidase attracts neutrophils by physical forces. Blood. 2011;117(4):1350–8.
Cioffi DL, Pandey S, Alvarez DF, Cioffi EA. Terminal sialic acids are an important determinant of pulmonary endothelial barrier integrity. Am J Physiol Lung Cell Mol Physiol. 2012;302(10):L1067–77.
Dudek SM, Garcia JG. Cytoskeletal regulation of pulmonary vascular permeability. J Appl Physiol (1985). 2001;91(4):1487–500.
Zharikov SI, Sigova AA, Chen S, Bubb MR, Block ER. Cytoskeletal regulation of the l-arginine/NO pathway in pulmonary artery endothelial cells. Am J Physiol Lung Cell Mol Physiol. 2001;280(3):L465–73.
Becker BF, Chappell D, Bruegger D, Annecke T, Jacob M. Therapeutic strategies targeting the endothelial glycocalyx: acute deficits, but great potential. Cardiovasc Res. 2010;87(2):300–10.
Ivanov AN, Puchinyan DM. Norkin IA. Vascular endothelial Barrier Function. Usp Fiziol Nauk. 2015;46(2):72–96.
van Golen RF, van Gulik TM, Heger M. Mechanistic overview of reactive species-induced degradation of the endothelial glycocalyx during hepatic ischemia/reperfusion injury. Free Radic Biol Med. 2012;52(8):1382–402.
Monahan LJ. Acute respiratory distress syndrome. Curr Probl Pediatr Adolesc Health Care. 2013;43(10):278–84.
Nettelbladt O, Hallgren R. Hyaluronan (hyaluronic acid) in bronchoalveolar lavage fluid during the development of bleomycin-induced alveolitis in the rat. Am Rev Respir Dis. 1989;140(4):1028–32.
Liu YY, Lee CH, Dedaj R, Zhao H, Mrabat H, Sheidlin. High-molecular-weight hyaluronan—a possible new treatment for sepsis-induced lung injury: a preclinical study in mechanically ventilated rats. Crit Care. 2008;12(4):R102.
Bedirli N, Demirtas CY, Akkaya T, Salman B, Alper M, Bedirli A. Volatile anesthetic preconditioning attenuated sepsis induced lung inflammation. J Surg Res. 2012;178(1):e17–23.
Jiang T, Liu Y, Ma M, Zong L, Yiliyaer X, Zhang H. The role of remote ischemic preconditioning in ischemia-reperfusion injury in rabbits with transplanted lung. Clin Lab. 2015;61(5–6):481–6.
Annecke T, Chappell D, Chen C, Jacob M, Welsch U, Sommerhoff CP. Sevoflurane preserves the endothelial glycocalyx against ischaemia-reperfusion injury. Br J Anaesth. 2010;104(4):414–21.
Chappell D, Heindl B, Jacob M, Annecke T, Chen C, Rehm M. Sevoflurane reduces leukocyte and platelet adhesion after ischemia-reperfusion by protecting the endothelial glycocalyx. Anesthesiology. 2011;115(3):483–91.
Simon Adiego C, Gonzalez-Casaurran G, Azcarate Perea L, Isea Vina J, Vara Ameigeiras E, Garcia Martin C, Casanova J. Experimental Swine lung autotransplant model to study lung ischemia-reperfusion injury. Arch Bronconeumol. 2011;47(6):283–9.
Casanova J, Garutti I, Simon C, Giraldez A, Martin B, Gonzalez G. The effects of anesthetic preconditioning with sevoflurane in an experimental lung autotransplant model in pigs. Anesth Analg. 2011;113(4):742–8.
Ng CS, Wan S, Yim AP, Arifi AA. Pulmonary dysfunction after cardiac surgery. Chest. 2002;121(4):1269–77.
de Perrot M, Liu M, Waddell TK, Keshavjee S. Ischemia-reperfusion-induced lung injury. Am J Respir Crit Care Med. 2003;167(4):490–511.
Kennedy TP, Rao NV, Hopkins C, Pennington L, Tolley E, Hoidal JR. Role of reactive oxygen species in reperfusion injury of the rabbit lung. J Clin Invest. 1989;83(4):1326–35.
Karck M, Haverich A. Nifedipine and diltiazem reduce pulmonary edema formation during postischemic reperfusion of the rabbit lung. Res Exp Med (Berl). 1992;192(2):137–44.
Collins SR, Blank RS, Deatherage LS, Dull RO. Special article: the endothelial glycocalyx: emerging concepts in pulmonary edema and acute lung injury. Anesth Analg. 2013;117(3):664–74.
Chappell D, Jacob M, Hofmann-Kiefer K, Rehm M, Welsch U, Conzen P. Antithrombin reduces shedding of the endothelial glycocalyx following ischaemia/reperfusion. Cardiovasc Res. 2009;83(2):388–96.
Chappell D, Jacob M, Paul O, Rehm M, Welsch U, Stoeckelhuber M. The glycocalyx of the human umbilical vein endothelial cell: an impressive structure ex vivo but not in culture. Circ Res. 2009;104(11):1313–7.
Lucchinetti E, Ambrosio S, Aguirre J, Herrmann P, Harter L, Keel M. Sevoflurane inhalation at sedative concentrations provides endothelial protection against ischemia-reperfusion injury in humans. Anesthesiology. 2007;106(2):262–8.
Mohamed MM, Sloane BF. Cysteine cathepsins: multifunctional enzymes in cancer. Nat Rev Cancer. 2006;6(10):764–75.
Lee HT, Kim M, Jan M, Emala CW. Anti-inflammatory and antinecrotic effects of the volatile anesthetic sevoflurane in kidney proximal tubule cells. Am J Physiol Renal Physiol. 2006;291(1):F67–78.
Rehm M, Zahler S, Lotsch M, Welsch U, Conzen P, Jacob M. Endothelial glycocalyx as an additional barrier determining extravasation of 6% hydroxyethyl starch or 5% albumin solutions in the coronary vascular bed. Anesthesiology. 2004;100(5):1211–23.
Reitsma S, Slaaf DW, Vink H, van Zandvoort MA, Oude Egbrink MG. The endothelial glycocalyx: composition, functions, and visualization. Pflugers Arch. 2007;454(3):345–59.
Luo X, Miao CH, Ge BX, Jiang H. Effects of isoflurane, sevoflurane and desflurane on expression of ICAM-1 and VCAM-1 in LPS-induced rat lung microvascular endothelial cells. Zhejiang Da Xue Xue Bao Yi Xue Ban. 2010;39(5):464–9.
Mulivor AW, Lipowsky HH. Inhibition of glycan shedding and leukocyte-endothelial adhesion in postcapillary venules by suppression of matrix metalloprotease activity with doxycycline. Microcirculation. 2009;16(8):657–66.
Wang L, Fuster M, Sriramarao P, Esko JD. Endothelial heparan sulfate deficiency impairs l-selectin- and chemokine-mediated neutrophil trafficking during inflammatory responses. Nat Immunol. 2005;6(9):902–10.
Ley K, Laudanna C, Cybulsky MI, Nourshargh S. Getting to the site of inflammation: the leukocyte adhesion cascade updated. Nat Rev Immunol. 2007;7(9):678–89.
Middleton J, Neil S, Wintle J, Clark-Lewis I, Moore H, Lam C. Transcytosis and surface presentation of IL-8 by venular endothelial cells. Cell. 1997;91(3):385–95.
Suter D, Spahn DR, Blumenthal S, Reyes L, Booy C, Z’Graggen BR. The immunomodulatory effect of sevoflurane in endotoxin-injured alveolar epithelial cells. Anesth Analg. 2007;104(3):638–45.
Acknowledgments
The authors are grateful to the statistical department at Gregorio Maranon Hospital. Financial support and sponsorship: the study was funded by grants from Carlos III Health Institute (Grant No. FISS PI07/00840) and the “Proyecto Investigar” by ABBOTT laboratories (Grant No. FGICBJ-2013 in Biomedic Investigation Foundation at Gregorio Marañon Hospital in Madrid).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
About this article
Cite this article
Casanova, J., Simon, C., Vara, E. et al. Sevoflurane anesthetic preconditioning protects the lung endothelial glycocalyx from ischemia reperfusion injury in an experimental lung autotransplant model. J Anesth 30, 755–762 (2016). https://doi.org/10.1007/s00540-016-2195-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-016-2195-0