Abstract
Purpose
There are no reports about the effect of bradycardia on stroke volume variation (SVV), and we hypothesized that induced bradycardia alters the value of SVV. Landiolol, an ultra-short-acting adrenergic β1-receptor blocking agent, was reported to induce bradycardia without decreasing blood pressure. The initial aim of this prospective study was to investigate changes in SVV values by induced bradycardia in patients with good cardiac function.
Methods
At 30 min after anesthesia induction, if heart rate (HR) was >80 bpm, the patient was chosen as a subject. Ten ASA physical status I–II patients aged 38–75 years who were scheduled for elective abdominal surgery were included in this study. Baseline values were recorded, and then administration of landiolol was started at 125 μg/kg/min for 1 min and then continued at 40 μg/kg/min. SVV and other parameters were recorded at baseline and 3 min after continuous landiolol injection.
Results
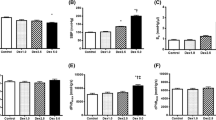
Landiolol significantly decreased systolic arterial pressure, and diastolic arterial pressure, contrary to our expectations, and also HR, SVV, cardiac output, stroke volume index, and pressure of end-tidal CO2, whereas systemic vascular resistance values increased significantly.
Conclusions
SVV decreased after continuous administration of a β1-adrenergic blocker, probably because of a decrease in the difference of maximum stroke volume (SV) and minimum SV, or the downward shift of the Frank–Starling curve that occurred after landiolol administration. We believe that SVV values might be overestimated or misinterpreted when HR is decreased by landiolol and might not necessarily indicate that the patient is hypervolemic or normovolemic.

Similar content being viewed by others
References
Michard F. Changes in arterial pressure during mechanical ventilation. Anesthesiology. 2005;103:419–28.
Wajima Z, Shiga T, Imanaga K, Inoue T. Assessment of the effect of rapid crystalloid infusion on stroke volume variation and pleth variability index after a preoperative fast. J Clin Monit Comput. 2010;24:385–9.
Biais M, Nouette-Gaulain K, Cottenceau V, Revel P, Sztark F. Uncalibrated pulse contour-derived stroke volume variation predicts fluid responsiveness in mechanically ventilated patients undergoing liver transplantation. Br J Anaesth. 2008;101:761–8.
Backer D, Heenen S, Piagnerelli M, Koch M, Vincent J-L. Pulse pressure variations to predict fluid responsiveness: influence of tidal volume. Intensive Care Med. 2005;31:517–23.
Reuter DA, Bayerlein J, Goepfert MS, Weis FC, Kilger E, Lamm P, Goetz AE. Influence of tidal volume on left ventricular stroke volume variation measured by pulse contour analysis in mechanically ventilated patients. Intensive Care Med. 2003;29:476–80.
Renner J, Gruenewald M, Quaden R, Hanss R, Meybohm P, Steinfath M, Scholz J, Bein B. Influence of increased intra-abdominal pressure on fluid responsiveness predicted by pulse pressure variation and stroke volume variation in a porcine model. Crit Care Med. 2009;37:650–8.
Jacques D, Bendjelid K, Duperret S, Colling J, Piriou V, Viale JP. Pulse pressure variation and stroke volume variation during increased intra-abdominal pressure: an experimental study. Crit Care. 2011;15:R33.
Wajima Z. Large dose of flunitrazepam attenuates baroreflex control of heart rate in man. J Anesth. 1991;5:10–6.
Wajima Z, Inoue T, Ogawa R. The effects of an intravenous nicardipine injection on baroreflex control of heart rate in man. J Anesth. 1993;7:40–7.
Wajima Z, Inoue T, Ogawa R. The effects of butorphanol on baroreflex control of heart rate in man. J Anesth. 1993;7:411–8.
Wajima Z, Shiga T, Imanaga K, Inoue T. Do induced hypertension and hypotension affect stroke volume variation in man? J Clin Anesth. 2012;24:207–11.
Wajima Z, Shiga T, Imanaga K, Inoue T. Prophylactic continuous administration of landiolol, a novel β1 blocker, blunts hyperdynamic responses during electroconvulsive therapy without altering seizure activity. Int J Psychiatry Clin Pract. 2010;14:132–6.
Wajima Z, Tsuchida H, Shiga T, Imanaga K, Inoue T. Intravenous landiolol, a novel β1-adrenergic blocker, reduces the minimum alveolar concentration of sevoflurane in women. J Clin Anesth. 2011;23:292–6.
Goyagi T, Tanaka M, Nishikawa T. Landiolol attenuates the cardiovascular response to tracheal intubation. J Anesth. 2005;19:282–6.
Iwasawa K, Nakagawa H, Katou M, Yonezawa K, Nishizawa M, Yanagiya N. Effects of landiolol hydrochloride on cardiohemodynamics in patients who underwent coronary artery bypass grafting (in Japanese with English abstract). Masui (Jpn J Anesthesiol). 2005;54:402–7.
Biais M, Vidil L, Sarrabay P, Cottenceau V, Revel P, Sztark F. Changes in stroke volume induced by passive leg raising in spontaneously breathing patients: comparison between echocardiography and Vigileo/FloTrac device. Crit Care. 2009;13:R195.
Kramer A, Zygun D, Hawes H, Easton P, Ferland A. Pulse pressure variation predicts fluid responsiveness following coronary artery bypass surgery. Chest. 2004;126:1563–8.
Michard F, Lopes MR, Auler JO Jr. Pulse pressure variation: beyond the fluid management of patients with shock. Crit Care. 2007;11:131.
Kobayashi S, Susa T, Tanaka T, Murakami W, Fukuta S, Okuda S, Doi M, Wada Y, Nao T, Yamada J, Okamura T, Yano M, Matsuzaki M. Low-dose β-blocker in combination with milrinone safely improves cardiac function and eliminates pulsus alternans in patients with acute decompensated heart failure. Circ J. 2012;76:1646–53.
Iskandrian AS, Bemis CE, Hakki AH, Panidis I, Heo J, Toole JG, Hua TA, Allin D, Kane-Marsch S. Effects of esmolol on patients with left ventricular dysfunction. J Am Coll Cardiol. 1986;8:225–31.
Aboab J, Sebille V, Jourdain M, Mangalaboyi J, Gharbi M, Mansart A, Annane D. Effects of esmolol on systemic and pulmonary hemodynamics and on oxygenation in pigs with hypodynamic endotoxin shock. Intensive Care Med. 2011;37:1344–51.
Hayashida M, Orii R, Komatsu K, Chinzei M, Nakagawa Y, Nishiyama T, Suwa K, Hanaoka K. Effects of cardiac output on PETCO2 and PaCO2 during combined inhalational-epidural anesthesia. Masui. 1997;46:1290–8.
Shibutani K, Muraoka M, Shirasaki S, Kubal K, Sanchala VT, Gupte P. Do changes in end-tidal PCO2 quantitatively reflect changes in cardiac output? Anesth Analg. 1994;79:829–33.
de Wilde RB, Geerts BF, van den Berg PC, Jansen JR. A comparison of stroke volume variation measured by the LiDCOplus and FloTrac-Vigileo system. Anaesthesia. 2009;64:1004–9.
Fukuda I. Clinical usefulness of the FloTrac system—efficacy of arterial pressure-based cardiac output and stroke volume variations (in Japanese with English abstract). JJSCA (J Jpn Soc Clin Anesth). 2011;31:81–90.
Acknowledgments
This study was supported solely by departmental resources.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Wajima, Z., Shiga, T., Imanaga, K. et al. Does intravenous landiolol, a β1-adrenergic blocker, affect stroke volume variation?. J Anesth 27, 890–894 (2013). https://doi.org/10.1007/s00540-013-1622-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-013-1622-8