Abstract
Purpose
Our purpose was to investigate whether the NO donor, 3-(2-hydroxy-1-methyl-2-nitroso-hydrazino)-N-methyl-1-propanamine (NOC7), restored cardiac function following global ischemia in an isolated rat heart model and whether intracellular messengers were involved in its effect.
Methods
Isolated rat hearts (n = 36) were randomly divided into six groups. The sham control group was perfused with modified Krebs-Henseleit bicarbonate buffer (KHB) alone. The ischemic control group and the NOC7 groups were subjected to 35 min of global ischemia, followed by 30 min of reperfusion with KHB alone, or reperfusion with KHB including NOC7 at 0.2, 2, 20, or 200 μM, respectively. Left ventricular developed pressure (LVDP), the maximum and the minimal rate of rise in LVP (±dP/dt), and coronary flow were measured continuously. Cyclic adenosine monophosphate (cAMP) and cyclic guanosine monophosphate (cGMP) levels were measured in myocardium homogenate, using enzyme immunoassay (EIA) methods.
Results
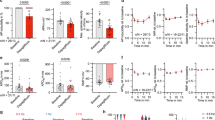
NOC7 at 2 and 20 μM rescued myocardial performance (LVDP, 111.9 ± 10.5% and 124.3 ± 12.5% of baseline, respectively; P < 0.05 vs ischemic control) at 30 min after reperfusion. However, NOC7 at 200 μM reduced the LVDP to 55.3 ± 6.0% of baseline. Coronary flows remain unchanged. The cAMP levels increased significantly from 0.83 ± 0.44 pmol·mg−1 protein in the ischemic control group to 1.79 ± 0.39, 1.86 ± 0.25, and 2.63 ± 0.24 pmol·mg−1 protein, in the groups with NOC7 at 2, 20, and 200 μM, respectively (P < 0.05). The cGMP level increased from 1.49 ± 0.61 pmol·mg−1 protein in the ischemic control group to 3.92 ± 0.66 pmol·mg−1 protein in the group with NOC7 at 200 μM alone (P < 0.05).
Conclusion
NOC7 appeared to exert a biphasic effect on the contractile force of the isolated rat heart after 35-min global ischemia. The balance between intracellular cAMP and cGMP levels seemed to be involved in its mechanism.
Similar content being viewed by others
References
Murry CE, Jennings RB, Reimer KA. Preconditioning with ischemia: a delay of lethal cell injury in ischemic myocardium. Circulation. 1986;74:1124–1136.
American Heart Association. American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Part 7.5. Postresuscitation support. Circulation. 2005;112:IV84–IV88.
Sarkar D, Vallance P, Amirmansour C, Harding SE. Positive inotropic effects of NO donors in isolated guinea-pig and human cardiomyocytes independent of NO species and cyclic nucleotides. Cardiovasc Res. 2000;48:430–439.
Kojda G, Kottenberg K, Nix P, Schluter KD, Piper HM, Noack E. Low increase in cGMP induced by organic nitrates and nitrovasodilators improves contractile response of rat ventricular myocytes. Circ Res. 1996;78:91–101.
Kelly RA, Balligand JL, Smith TW. Nitric oxide and cardiac function. Circ Res. 1996;79:363–380.
Okada H, Kurita T, Mochizuki T, Morita K, Sato S. The cardio-protective effect of dexmedetomidine on global ischaemia in isolated rat hearts. Resuscitation. 2007;74:538–545.
Vila-Petroff MG, Younes A, Egan J, Lakatta EG, Sollott SJ. Activation of distinct camp-dependent and cGMP-dependent pathways by nitric oxide in cardiac myocytes. Circ Res. 1999;84:1020–1031.
Moalem J, Weiss HR, Davidov T, Rodriguez R, Molino B, Lazar MJ, Scholz PM. Heart failure reduces both the effects and interaction between cyclic GMP and cyclic AMP. J Surg Res. 2006;134:300–306.
Kojda G, Kottenberg K. Regulation of basal myocardial function by NO. Cardiovasc Res. 1999;41:514–523.
Paulus WJ, Frantz S, Kelly RA. Nitric oxide and cardiac contractility in human heart failure: time for reappraisal. Circulation. 2001;104:2260–2262.
Layland J, Solaro RJ, Shah AM. Regulation of cardiac contractile function by troponin I phosphorylation. Cardiovasc Res. 2005;66:12–21.
Rastaldo R, Pagliaro P, Cappello S, Penna C, Mancardi D, Westerhof N, Losano G. Nitric oxide and cardiac function. Life Sci. 2007;81:779–793.
Brown GC, Borutaite V. Nitric oxide and mitochondrial respiration in the heart. Cardiovasc Res. 2007;75:283–290.
Bryan NS, Rassaf T, Maloney RE, Rodriguez CM, Saijo F, Rodriguez JR, Feelisch M. Cellular targets and mechanisms of nitros(yl)ation: an insight into their nature and kinetics in vivo. Proc Natl Acad Sci U S A. 2004;101:4308–4313.
Hearse DJ, Bolli R. Reperfusion induced injury: manifestations, mechanisms, and clinical relevance. Cardiovasc Res. 1992;26:101–108.
Piper HM, Garcia-Dorado D, Ovize M. A fresh look at reperfusion injury. Cardiovasc Res. 1998;38:291–300.
Maxwell SR, Lip GY. Reperfusion injury: a review of the pathophysiology, clinical manifestations and therapeutic options. Int J Cardiol. 1997;58:95–117.
Ferdinandy P, Danial H, Ambrus I, Rothery RA, Schulz R. Peroxynitrite is a major contributor to cytokine-induced myocardial contractile failure. Circ Res. 2000;87:241–247.
Amrani M, Chester AH, Jayakumar J, Schyns CJ, Yacoub MH. L-Arginine reverses low coronary reflow and enhances postischaemic recovery of cardiac mechanical function. Cardiovasc Res. 1995;30:200–204.
Hiramatsu T, Forbess JM, Miura T, Mayer JE Jr. Effects of L-arginine and L-nitro-arginine methyl ester on recovery of neonatal lamb hearts after cold ischemia. Evidence for an important role of endothelial production of nitric oxide. J Thorac Cardiovasc Surg. 1995;109:81–86; discussion 87.
Pabla R, Buda AJ, Flynn DM, Salzberg DB, Lefer DJ. Intracoronary nitric oxide improves postischemic coronary blood flow and myocardial contractile function. Am J Physiol. 1995;269:H1113–H1121.
Author information
Authors and Affiliations
About this article
Cite this article
Hui, Y., Mochizuki, T., Kondo, K. et al. Nitric oxide donor, NOC7, reveals biphasic effect on contractile force of isolated rat heart after global ischemia. J Anesth 22, 229–235 (2008). https://doi.org/10.1007/s00540-008-0625-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-008-0625-3