Abstract
Background
Previous studies investigating the impact of tumor location on colorectal cancer prognosis only compared two groups by location, e.g., ‘right-sided colon vs. left-sided colon,’ ‘colon vs. rectum,’ and ‘right-sided (right-sided colon) vs. left-sided (left-sided colon and rectum).’ This nationwide multicenter retrospective study aimed to clarify the prognostic impact of tumor location in patients with stage III colorectal cancer by classifying tumors into three groups: right-sided colon, left-sided colon, and rectum.
Methods
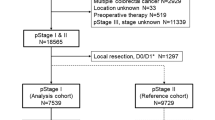
Subjects were 9194 patients with stage III colorectal cancer who underwent curative surgery from 1997 to 2012. Relapse-free survival (RFS) after primary surgery and overall survival (OS) after recurrence were examined.
Results
Rectal cancer (n = 2922) was associated with worse RFS compared to right-sided colon cancer (n = 2362) (hazard ratio (HR) 0.65; 95% CI 0.59–0.72; p < 0.001) and left-sided colon cancer (n = 3910) (HR 0.72; 95% CI 0.66–0.78; p < 0.001) after adjusting for key clinical factors (i.e., sex, age, histological type, CEA, adjuvant therapy, T category, and N category). Among patients with recurrence (n = 2823), rectal cancer was associated with better OS compared to right-sided colon cancer (HR 1.23; 95% CI 1.08–1.40; p = 0.002) and worse OS compared to left-sided colon cancer (HR 0.88; 95% CI 0.79–0.99; p = 0.029). Twenty percent of right-sided colon cancer recurrences exhibited peritoneal dissemination, 42% of left-sided colon cancer recurrences were liver metastases, and 33% of rectal cancer recurrences were local recurrences.
Conclusions
The three tumor locations (right-sided colon, left-sided colon, rectum) had different prognostic implications for recurrence after curative resection and overall mortality, suggesting that tumor location serves as a prognostic biomarker in stage III colorectal cancer.




Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- CSS:
-
Cancer-specific survival
- dMMR:
-
Deficient mismatch repair
- HR:
-
Hazard ratio
- OS:
-
Overall survival
- RFS:
-
Relapse-free survival
References
Arnold D, Lueza B, Douillard JY, et al. Prognostic and predictive value of primary tumour side in patients with RAS wild-type metastatic colorectal cancer treated with chemotherapy and EGFR directed antibodies in six randomized trials. Ann Oncol. 2017;28:1713–29.
Tejpar S, Stintzing S, Ciardiello F, et al. Prognostic and predictive relevance of primary tumor location in patients with RAS wild-type metastatic colorectal cancer: retrospective analyses of the CRYSTAL and FIRE-3 trials. JAMA Oncol. 2017;3:194–201.
Shida D, Tanabe T, Boku N, et al. Prognostic value of primary tumor sidedness for unresectable stage IV colorectal cancer: a retrospective study. Ann Surg Oncol. 2019;26:1358–65.
Shida D. ASO author reflections: prognostic impact of primary tumor sidedness for unresectable stage IV colorectal cancer. Ann Surg Oncol. 2019;26:666–7.
Kamath SD, Khorana AA. Does sidedness matter in unresectable colorectal cancer? Ann Surg Oncol. 2019;26:1588–91.
Petrelli F, Tomasello G, Borgonovo K, et al. Prognostic survival associated with left-sided vs. right-sided colon cancer: a systematic review and meta-analysis. JAMA Oncol. 2017;3:211–9.
Ha GW, Kim JH, Lee MR. Oncologic effects of primary tumor-sidedness on patients with stages 1–3 colon cancer: a meta-analysis. Ann Surg Oncol. 2019;26:1366–75.
Yahagi M, Okabayashi K, Hasegawa H, et al. The worse prognosis of right-sided compared with left-sided colon cancers: a systematic review and meta-analysis. J Gastrointest Surg. 2016;20:648–55.
Karim S, Brennan K, Nanji S, et al. Association between prognosis and tumor laterality in early-stage colon cancer. JAMA Oncol. 2017;3:1386–92.
Warschkow R, Sulz MC, Marti L, et al. Better survival in right-sided versus left-sided stage I-III colon cancer patients. BMC Cancer. 2016;16:554.
Ishihara S, Murono K, Sasaki K, et al. Impact of primary tumor location on postoperative recurrence and subsequent prognosis in nonmetastatic colon cancers: a multicenter retrospective study using a propensity score analysis. Ann Surg. 2018;267:917–21.
Kishiki T, Kuchta K, Matsuoka H, et al. The impact of tumor location on the biological and oncological differences of colon cancer: Multi-institutional propensity score-matched study. Am J Surg. 2019;217:46–52.
Allemani C, Matsuda T, Di Carlo V, et al. Global surveillance of trends in cancer survival 2000–14 (CONCORD-3): analysis of individual records for 37 513 025 patients diagnosed with one of 18 cancers from 322 population-based registries in 71 countries. Lancet. 2018;391:1023–75.
Benson AB 3rd, Venook AP, Cederquist L, et al. Colon cancer, version 1.2017, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 2017;15:370–98.
Benson AB, Venook AP, Al-Hawary MM, et al. Rectal cancer, version 2.2018, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 2018;16:874–901.
Hashiguchi Y, Muro K, Saito Y, et al. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2019 for the treatment of colorectal cancer. Int J Clin Oncol. 2019;25:1–42.
UICC. TNM classification of malignant tumours eighth edition. Brierley JD, Gospodarowicz MK, Wittekind C, editors. New York: John Wiley and Sons, Ltd; 2017.
Austin PC, Lee DS, Fine JP. Introduction to the analysis of survival data in the presence of competing risks. Circulation. 2016;133:601–9.
Guinney J, Dienstmann R, Wang X, et al. The consensus molecular subtypes of colorectal cancer. Nat Med. 2015;21:1350–6.
Franko J, Shi Q, Meyers JP, et al. Prognosis of patients with peritoneal metastatic colorectal cancer given systemic therapy: an analysis of individual patient data from prospective randomised trials from the analysis and research in cancers of the digestive system (ARCAD) database. Lancet Oncol. 2016;17:1709–19.
Shida D, Yoshida T, Tanabe T, et al. Prognostic impact of R0 resection and targeted therapy for colorectal cancer with synchronous peritoneal metastasis. Ann Surg Oncol. 2018;25:1646–53.
Akiyoshi T, Watanabe T, Miyata S, et al. Results of a Japanese nationwide multi-institutional study on lateral pelvic lymph node metastasis in low rectal cancer: is it regional or distant disease? Ann Surg. 2012;255:1129–34.
Sinicrope FA, Mahoney MR, Yoon HH, et al. Analysis of molecular markers by anatomic tumor site in stage III colon carcinomas from adjuvant chemotherapy trial NCCTG N0147 (Alliance). Clin Cancer Res. 2015;21:5294–304.
Yamauchi M, Morikawa T, Kuchiba A, et al. Assessment of colorectal cancer molecular features along bowel subsites challenges the conception of distinct dichotomy of proximal versus distal colorectum. Gut. 2012;61:847–54.
Taieb J, Shi Q, Pederson L, et al. Prognosis of microsatellite instability and/or mismatch repair deficiency stage III colon cancer patients after disease recurrence following adjuvant treatment: results of an ACCENT pooled analysis of seven studies. Ann Oncol. 2019;30:1466–71.
Shida D, Ochiai H, Tsukamoto S, et al. Long-term outcomes of laparoscopic versus open D3 dissection for stage II/III colon cancer: Results of propensity score analyses. Eur J Surg Oncol. 2018;44:1025–30.
Pai RK, Jayachandran P, Koong AC, et al. BRAF-mutated, microsatellite-stable adenocarcinoma of the proximal colon: an aggressive adenocarcinoma with poor survival, mucinous differentiation, and adverse morphologic features. Am J Surg Pathol. 2012;36:744–52.
Tran B, Kopetz S, Tie J, et al. Impact of BRAF mutation and microsatellite instability on the pattern of metastatic spread and prognosis in metastatic colorectal cancer. Cancer. 2011;117:4623–32.
Aoyama T, Oba K, Honda M, et al. Impact of postoperative complications on the colorectal cancer survival and recurrence: analyses of pooled individual patients’ data from three large phase III randomized trials. Cancer Med. 2017;6:1573–80.
Ho YH, Siu SK, Buttner P, et al. The effect of obstruction and perforation on colorectal cancer disease-free survival. World J Surg. 2010;34:1091–101.
Carraro PG, Segala M, Orlotti C, et al. Outcome of large-bowel perforation in patients with colorectal cancer. Dis Colon Rectum. 1998;41:1421–6.
Acknowledgements
This study is based on data from 24 hospitals, which are members of the Japanese Study Group for Postoperative Follow-up of CRC, as follows: Ichiro Takemasa (Sapporo Medical University); Kenichi Hakamada (Hirosaki University); Hitoshi Kameyama (Niigata University); Yasukimi Takii (Niigata Cancer Center Hospital); Hideki Ueno (National Defense Medical College); Heita Ozawa (Tochigi Cancer Center); Soichiro Ishihara (the University of Tokyo); Keiichi Takahashi (Tokyo Metropolitan Cancer and Infectious diseases Center Komagome Hospital); Yukihide Kanemitsu (National Cancer Center Hospital); Michio Itabashi (Tokyo Women’s Medical University); Tomomichi Kiyomatsu (National Center for Global Health and Medicine); Yusuke Kinugasa (Tokyo Medical and Dental University); Koji Okabayashi (Keio University); Yojiro Hashiguchi (Teikyo University); Tadahiko Masaki (Kyorin University); Masahiko Watanabe (Kitasato University); Akio Shiomi (Shizuoka Cancer Center); Tsunekazu Hanai (Fujita Health University); Koji Komori (Aichi Cancer Center Hospital); Yoshiharu Sakai (Kyoto University); Masayuki Ohue (Osaka International Cancer Institute); Shingo Noura (Osaka Rosai Hospital); Naohiro Tomita (Hyogo College of Medicine); and Yoshito Akagi (Kurume University).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shida, D., Inoue, M., Tanabe, T. et al. Prognostic impact of primary tumor location in Stage III colorectal cancer-right-sided colon versus left-sided colon versus rectum: a nationwide multicenter retrospective study. J Gastroenterol 55, 958–968 (2020). https://doi.org/10.1007/s00535-020-01706-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-020-01706-7