Abstract
Objective
We have reviewed the endoscopic retrograde cholangiopancreatography (ERCP) images of patients with autoimmune pancreatitis (AIP) and pancreatic carcinoma (Pca) in an attempt to identify findings that would facilitate making a differential diagnosis between AIP and Pca.
Methods
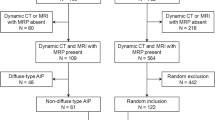
The study cohort consisted of 39 patients diagnosed with AIP and 62 patients diagnosed with Pca. The ERCP findings in the pancreatic duct and biliary tract were compared between the two groups.
Results
The ERCP images revealed that AIP patients had a higher prevalence of narrowing of the main pancreatic duct (MPD) for ≥3 cm of its length and a higher prevalence for the presence of side branches in the narrowed portion of the MPD than Pca patients (p < 0.001 and p < 0.001, respectively). In contrast, the prevalence of an upstream MPD having a maximal diameter ≥4 cm was significantly higher in the Pca patient group (p < 0.001). The discriminant analysis identified three significant factors: (1) whether or not side branches were present; (2) total length of the narrowed portion of the MPD; (3) maximal diameter of the upstream MPD. It was impossible to differentiate Pca from AIP in the two Pca patients in whom ERCP revealed both narrowing of the MPD for >5 cm of its length and the presence of side branches.
Conclusions
Among our patient cohort, the ERCP findings in terms of the length of the narrowed portion of the MPD, the presence of side branches, and maximal diameter of the upstream MPD enabled differential diagnosis between AIP and Pca in most of the cases. However, it must be borne in mind that some Pca patients have ERCP findings similar to those of AIP patients.













Similar content being viewed by others
References
Yoshida K, Toki F, Takeuchi T, Watanabe S, Shiratori K, Hayashi N. Chronic pancreatitis caused by an autoimmune abnormality. Dig Dis Sci. 1995;40:1561–8.
Okazaki K, Uchida K, Ohana M, Nakase H, Uose S, Inai M, et al. Autoimmune-related pancreatitis is associated with autoantibodies and a Th1/Th2-type cellular immune response. Gastroenterology. 2000;118:573–81.
Hamano H, Kawa S, Horiuchi A, Unno H, Furuya N, Akamatsu T, et al. High serum IgG4 concentrations in patients with sclerosing pancreatitis. N Engl J Med. 2001;344:732–8.
Kawaguchi K, Koike M, Tsuruta K, Okamato A, Tabata I, Fujita N. Lymphoplasmacytic sclerosing pancreatitis with cholangitis: a variant of primary sclerosing cholangitis extensively involving pancreas. Hum Pathol. 1991;22:387–95.
Kamisawa T, Furuta N, Hayashi Y, Tsuruta K, Okamoto A, Amemiya K, et al. Close relationship between autoimmune pancreatitis and multifocal fibrosclerosis. Gut. 2003;52:683–7.
Horiuchi A, Kawa S, Hamano H, Hayama M, Ota H, Kiyosawa K. ERCP features in 27 patients with autoimmune pancreatitis. Gastrointest Endosc. 2002;55:494–9.
Nishino T, Toki F, Oyama H, Oi I, Kobayashi M, Takasaki K, et al. Biliary tract involvement in autoimmune pancreatitis. Pancreas. 2005;30:76–82.
Nishino T, Toki F, Oyama H, Shimizu K, Shiratori K. Long-term outcome of autoimmune pancreatitis after oral prednisolone therapy. Intern Med. 2006;45:497–501.
Hirano K, Tada M, Isayama H, Yogioka H, Sasaki T, Kogure H, et al. Long-term prognosis of autoimmune pancreatitis with and without corticosteroid treatment. Gut. 2007;56:1719–24.
Chari ST, Smyrk TC, Levy MJ, Topazian MD, Takahashi N, Zhang L, et al. Diagnosis of autoimmune pancreatitis: the Mayo Clinic experience. Clin Gastroenterol Hepatol. 2006;4:1010–6.
Kim KP, Kim MH, Kim JC, Lee SS, Seo DW, Lee SK. Diagnostic criteria for autoimmune chronic pancreatitis revisited. World J Gastroenterol. 2006;12:2487–96.
Okazaki K, Kawa S, Kamisawa T, Naruse S, Tanaka S, Nishimori I, et al. Clinical diagnostic criteria of autoimmune pancreatitis: revised proposal. J Gastroenterol. 2006;41:626–31.
Nakazawa T, Ohara H, Sano H, Ando T, Imai H, Takada H, et al. Difficulty in diagnosing autoimmune pancreatitis. Gastrointest Endosc. 2007;65:99–108.
Wakabayashi T, Kawaura Y, Satomura Y, Watanabe H, MotooY Okai T, et al. Clinical and imaging features of autoimmune pancreatitis with focal pancreatic swelling or mass forming pancreatitis and pancreatic carcinoma. Am J Gastroenterol. 2003;98:2679–87.
Kamisawa T, Egawa N, Nakajima H, Tsuruta K, Okamoto A, Kamata N. Clinical difficulties in differentiation of autoimmune pancreatitis and pancreatic carcinoma. Am J Gastroenterol. 2003;98:2694–9.
Ghazale A, Chari ST, Smyrk TC, Levy MJ, Topazian MD, Takahashi N, et al. Value of serum IgG4 in the diagnosis of autoimmune pancreatitis and in distinguishing it from pancreatic cancer. Am J Gastroenterol. 2007;102:1646–53.
Kamisawa T, Imai M, Yui Cen P, Tu Y, Egawa N, Tsuruta K, et al. Strategy for differentiating autoimmune pancreatitis from pancreatic cancer. Pancreas. 2008;37:e62–7.
Hoki N, Mizuno N, Sawaki A, Tajika M, Takayama R, Shimizu Y, et al. Diagnosis of autoimmune pancreatitis using endoscopic ultrasonography. J Gastroenterol. 2009;44:154–9.
Kamisawa T, Okamoto A. Autoimmune pancreatitis: proposal of IgG4-related sclerosing disease. J Gastroenterol. 2006;41:613–25.
Nakazawa T, Ohara H, Sano H, Aoki S, Kobayashi S, Okamoto T, et al. Cholangiography can discriminate sclerosing cholangitis with autoimmune pancreatitis from primary sclerosing cholangitis. Gastrointest Endosc. 2004;60:937–44.
Nishino T, Oyama H, Hashimoto E, Toki F, Kobayashi M, Shiratori K. Clinicopathological differentiation between sclerosing cholangitis with autoimmune pancreatitis and primary sclerosing cholangitis. J Gastroenterol. 2007;42:550–9.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nishino, T., Oyama, H., Toki, F. et al. Differentiation between autoimmune pancreatitis and pancreatic carcinoma based on endoscopic retrograde cholangiopancreatography findings. J Gastroenterol 45, 988–996 (2010). https://doi.org/10.1007/s00535-010-0250-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00535-010-0250-4