Abstract
Background/purpose
In patients with hilar biliary malignancies, preservation of the middle hepatic artery (MHA, segment IV artery) where it runs close to the tumor in the hepatic hilum may lead to resection with positive margins. This retrospective study assessed the safety of combined resection of the MHA with right hemihepatectomy, caudate lobectomy, and bile duct resection for hilar biliary malignancies.
Methods
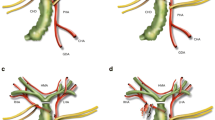
Of 61 patients with hilar biliary malignancies who underwent right hemihepatectomy, we classified the branching patterns of the MHA according to the origins and courses in the hilum. The MHA was resected without reconstruction in 16 patients in whom the artery ran close to the tumor. We compared the perioperative outcomes in these patients with those of patients who did not undergo resection of the artery.
Results
Anatomically, the MHA ran on the right side of the umbilical portion of the portal vein in 40 (66%) patients. Perioperative data for the patients who underwent combined resection were similar to those in whom the MAH was preserved. There were no postoperative complications that could be directly related to the arterial resection.
Conclusions
Combined resection of the MHA during right hemihepatectomy for hilar biliary malignancies has a safe perioperative course.


Similar content being viewed by others
References
Yamaguchi R, Nagino M, Oda K, Kamiya J, Uesaka K, Nimura Y. Perineural invasion has a negative impact on survival of patients with gallbladder carcinoma. Br J Surg. 2002;89:1130–6.
Kondo S, Hirano S, Ambo Y, Tanaka E, Okushiba S, Morikawa T, et al. Forty consecutive resections of hilar cholangiocarcinoma with no postoperative mortality and no positive ductal margins: results of a prospective study. Ann Surg. 2004;240:95–101.
Skandalakis JE, Skandalakis LJ, Skandalakis PN, Mirilas P. Hepatic surgical anatomy. Surg Clin North Am. 2004;84:413–35.
Onishi H, Kawarada Y, Das BC, Nakano K, Gadzijev EM, Ravnik D, et al. Surgical anatomy of the medial segment (S4) of the liver with special reference to bile ducts and vessels. Hepatogastroenterology. 2000;47:143–50.
Majno PE, Prêtre R, Mentha G, Morel P. Operative injury to the hepatic artery. Consequences of a biliary-enteric anastomosis and principles for rational management. Arch Surg. 1996;131:211–5.
Gupta N, Solomon H, Fairchild R, Kaminski DL. Management and outcome of patients with combined bile duct and hepatic artery injuries. Arch Surg. 1998;133:176–81.
Tanaka K, Nishimura A, Hombo K, Furoi A, Ikoma A, Yamauchi T, et al. The development of a pyogenic liver abscess following radical resection of cholangiocellular carcinoma with ligation of the right hepatic artery: report of a case. Surg Today. 1994;24:659–62.
Smith GS, Birnbaum BA, Jacobs JE. Hepatic infarction secondary to arterial insufficiency in native livers: CT findings in 10 patients. Radiology. 1998;208:223–9.
Ikegami T, Kawasaki S, Matsunami H, Hashikura Y, Nakazawa Y, Miyagawa S, et al. Should all hepatic arterial branches be reconstructed in living-related liver transplantation? Surgery. 1996;119:431–6.
Kondo S, Katoh H, Hirano S, Ambo Y, Tanaka E, Okushiba S. Portal vein resection and reconstruction prior to hepatic dissection during right hepatectomy and caudate lobectomy for hepatobiliary cancer. Br J Surg. 2003;90:694–7.
Mays ET, Wheeler CS. Demonstration of collateral arterial flow after interruption of hepatic arteries in man. N Engl J Med. 1974;290:993–6.
Parks RW, Chrysos E, Diamond T. Management of liver trauma. Br J Surg. 1999;86:1121–35.
Miyazaki M, Ito H, Nakagawa K, Ambiru S, Shimizu H, Yoshidome H, et al. Unilateral hepatic artery reconstruction is unnecessary in biliary tract carcinomas involving lobar hepatic artery: implications of interlobar hepatic artery and its preservation. Hepatogastroenterology. 2000;47:1526–30.
Stratta RJ, Wood RP, Langnas AN, Hollins RR, Bruder KJ, Donovan JP, et al. Diagnosis and treatment of biliary tract complications after orthotopic liver transplantation. Surgery. 1989;106:675–83.
Colonna JO 2nd, Shaked A, Gomes AS, Colquhoun SD, Jurim O, McDiarmid SV, et al. Biliary strictures complicating liver transplantation. Incidence, pathogenesis, management, and outcome. Ann Surg. 1992;216:344–50.
Buis CI, Hoekstra H, Verdonk RC, Porte RJ. Causes and consequences of ischemic-type biliary lesions after liver transplantation. J Hepatobiliary Pancreat Surg. 2006;13:517–24.
Nakanuma Y, Hoso M, Sanzen T, Sasaki M. Microstructure and development of the normal and pathologic biliary tract in humans, including blood supply. Microsc Res Tech. 1997;38:552–70.
Kawarada Y, Das BC, Taoka H. Anatomy of the hepatic hilar area: the plate system. J Hepatobiliary Pancreat Surg. 2000;7:580–6.
Arnold MM, Kreel L, Lo YF, Law H. Are the hepatic arteries “end arteries”? Invest Radiol. 1991;26:337–42.
Terada T, Ishida F, Nakanuma Y. Vascular plexus around intrahepatic bile ducts in normal livers and portal hypertension. J Hepatol. 1989;8:139–49.
Kondo S, Hirano S, Ambo Y, Tanaka E, Kubota T, Katoh H. Arterioportal shunting as an alternative to microvascular reconstruction after hepatic artery resection. Br J Surg. 2004;91:248–51.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Hirano, S., Kondo, S., Tanaka, E. et al. Safety of combined resection of the middle hepatic artery in right hemihepatectomy for hilar biliary malignancy. J Hepatobiliary Pancreat Surg 16, 796–801 (2009). https://doi.org/10.1007/s00534-009-0107-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00534-009-0107-5