Abstract
Background/Purpose
It has been reported that hepatic resection may be preferable to other modalities for the treatment of small hepatocellular carcinomas (HCCs), by contributing to improved overall and disease-free survival. Ablation techniques such as radiofrequency ablation (RFA) have also been used as therapy for small HCCs; however, few studies have compared the two treatments based on long-term outcomes. The effectiveness of hepatic resection and RFA for small nodular HCCs within the Milan criteria were compared.
Methods
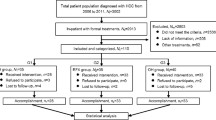
A retrospective cohort study was performed with 278 consecutive patients who underwent curative hepatic resection (n = 123) or initial RFA percutaneously (n = 110) or surgically (thoracoscopic-, laparoscopic-, and open-approaches; n = 45) for HCC. The selection criteria for treatment were based on uniform criteria. Mortality related to therapy and 3- and 5-year overall and disease-free survivals were analyzed.
Results
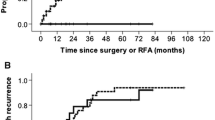
The model for endstage liver disease (MELD) scores for all patients in the series were less than 13. There were no therapy-related mortalities in either the hepatic resection or RFA groups. The incidence of death within 1 year after therapy (1.6 and 1.9%, respectively) was similar in the hepatic resection and RFA groups. The group that underwent hepatic resection showed a trend towards better survival (P = 0.06) and showed significantly better disease-free survival (P = 0.02) compared with the RFA group, although differences in liver functional reserve existed. The advantage of hepatic resection was more evident for patients with single tumors and patients with grade A liver damage. In contrast, patients with multinodular tumors survived longer when treated with RFA, regardless of the grade of liver damage. Further analysis showed that surgical RFA could potentially have survival benefits similar to those of hepatic resection for single tumors, and that surgical RFA had the highest efficacy for treating multinodular tumors.
Conclusions
In patients with small HCCs within the Milan criteria, hepatic resection should still be employed for those patients with a single tumor and well-preserved liver function. RFA should be chosen for patients with an unresectable single tumor or those with multinodular tumors, regardless of the grade of liver damage. In order to increase long-term oncological control, surgical RFA seems preferable to percutaneous RFA, if the patient’s condition allows them to tolerate surgery.



Similar content being viewed by others
References
Hasegawa K, Kokudo N, Imamura H, et al. Prognostic impact of anatomic resection for hepatocellular carcinoma. Ann Surg. 2005;242:252–9.
Fan ST, Ng IO, Poon RT, et al. Hepatectomy for hepatocellular carcinoma: the surgeon’s role in long-term survival. Arch Surg. 1999;134:1124–30.
Regimbeau JM, Kianmanesh R, Farges O, et al. Extent of liver resection influences the outcome in patients with cirrhosis and small hepatocellular carcinoma. Surgery. 2002;131:311–7.
Livraghi T, Giorgio A, Marin G, et al. Hepatocellular carcinoma and cirrhosis in 746 patients: long-term results of percutaneous ethanol injection. Radiology. 1995;197:101–8.
Lin SM, Lin CJ, Lin CC, et al. Radiofrequency ablation improves prognosis compared with ethanol injection for hepatocellular carcinoma less than or equal to 4 cm. Gastroenterology. 2004;127:1714–23.
Shiina S, Teratani T, Obi S, et al. A randomized controlled trial of radiofrequency ablation with ethanol injection for small hepatocellular carcinoma. Gastroenterology. 2005;129:122–30.
Teratani T, Toshida H, Shiina S, et al. Radiofrequency ablation for hepatocellular carcinoma in so-called high-risk locations. Hepatology. 2006;43:1101–8.
Aramaki M, Kawano K, Ohno T, et al. Microwave coagulation therapy for unresectable hepatocellular carcinoma. Hepatogastroenterology. 2004;51:1784–7.
Francica G, Marone G. Ultrasound-guided percutaneous treatment of hepatocellular carcinoma by radiofrequency hyperthermia with a “cooled-tip needle”. A preliminary clinical experience. Eur J Ultrasound. 1999;9:145–53.
Befler AS, Di Bisceglie AM. Hepatocellular carcinomas: diagnosis and treatment. Gastroenterology. 2002;122:1609–19.
Curley SA, Izzo F, Ellis LM, et al. Radiofrequency ablation of hepatocellular cancer in 110 patients with cirrhosis. Ann Surg. 2000;232:381–91.
Sutherland LM, Williams JAR, Padbury RTA. Radiofrequency ablation of liver tumors. Arch Surg. 2006;141:181–90.
Yu HC, Le JM, Kim DG, et al. Recurrence pattern of the radiofrequency ablation for hepatocellular carcinoma (abstract). J Hepatobiliary Pancreat Surg. 2002;9(Suppl 1):125.
Vivarelli M, Guglielmi A, Ruzzenente A, et al. Surgical resection versus percutaneous radiofrequency ablation in the treatment of hepatocellular carcinoma on cirrhotic liver. Ann Surg. 2004;240:102–7.
Ikeda K, Kobayashi M, Saitoh S, et al. Cost-effectiveness of radiofrequency ablation and surgical therapy for small hepatocellular carcinoma of 3 cm or less in diameter. Hepatol Res. 2005;33:241–9.
Hong SN, Lee SY, Choi MS, et al. Comparing the outcomes of radiofrequency ablation and surgery in patients with a single small hepatocellular carcinoma and well-preserved hepatic function. J Clin Gastroenterol. 2005;39:247–52.
Chen MS, Li JQ, Zheng Y, et al. A prospective randomized trial comparing percutaneous local ablation therapy and partial hepatectomy for small hepatocellular carcinoma. Ann Surg. 2006;243:321–8.
Ueno S, Tanabe G, Sako K, et al. Discrimination value of the new western prognostic system (CLIP score) for hepatocellular carcinoma in 662 Japanese patients. Cancer of the liver Italian program. Hepatology. 2001;34:529–34.
Ueno S, Tanabe G, Nuruki K, et al. Prognostic performance of the new classification of primary liver cancer of Japan (4th edition) for patients with hepatocellular carcinoma: a validation analysis. Hepatol Res. 2002;24:395–403.
Ueno S, Tanabe G, Nuruki K, et al. Prognosis of hepatocellular carcinoma associated with Child class B and C cirrhosis in relation to treatment: a multivariate analysis of 411 patients at a single center. J Hepatobiliary Pancreat Surg. 2002;9:469–77.
Liver Cancer Study Group of Japan. The general rules for the clinical and pathological study of primary liver cancer. 4th ed. Tokyo: Kanehara; 2001.
Yoshidome Y, Tanabe G, Ueno S, et al. Risk prediction using histology of noncancerous liver before hepatic resection for hepatocellular carcinoma. Hepatogastroenterology. 2001;48:518–22.
Ueno S, Tanabe G, Yoshida A, et al. Postoperative prediction of and strategy for metastatic recurrent hepatocellular carcinoma according to histologic activity of hepatitis. Cancer. 1999;86:248–54.
Komorizono Y, Oketani M, Sako K, et al. Risk factors for local recurrence of small hepatocellular carcinoma tumors after a single session, single application of percutaneous radiofrequency ablation. Cancer. 2003;97:1253–62.
Sasaki A, Iwashita Y, Shibata K, et al. Improved long-term survival after liver resection for hepatocellular carcinoma in the modern era: retrospective study from HCV-endemic areas. World J Surg. 2006;30:1567–78.
Okamoto M, Utsunomiya T, Wakiyama S, et al. Specific gene-expression profiles of noncancerous liver tissue predict the risk for multicentric occurrence of hepatocellular carcinoma in hepatitis C virus-positive patients. Ann Surg Oncol. 2006;13:947–54.
Murray KF, Carithers RL. AASLD practice guidelines: evaluation of the patient for liver transplantation. Hepatology. 2005;41:1–26.
Amitrano L, Guardascione MA, Bennato R, et al. MELD score and hepatocellular carcinoma identify patients at different risk of short-term mortality among cirrhotics bleeding from esophageal varices. J Hepatol. 2005;42:820–5.
Shi M, Zhang CQ, Zhang YQ, et al. Micrometastases of solitary hepatocellular carcinoma and appropriate resection margin. World J Surg. 2004;28:376–81.
Hori T, Nagata K, Hasuike S, et al. Risk factors for the local recurrence of hepatocellular carcinoma after a single session of percutaneous radiofrequency ablation. J Gastroenterol. 2003;38:977–81.
Rhim H, Yoon KH, Lee JM, et al. Major complications after radiofrequency thermal ablation of hepatic tumors: spectrum of imaging findings. Radiographics. 2003;23:123–4.
Mulier S, Mulier P, Ni Y, et al. Complications of radiofrequency ablation coagulation of liver tumors. Br J Surg. 2002;89:1206–22.
Tateishi R, Shiina S, Teratani T, et al. Percutaneous radiofrequency ablation for hepatocellular carcinoma. An analysis of 1,000 cases. Cancer. 2005;103:1201–9.
Yokoyama T, Egami K, Miyamoto M, et al. Percutaneous and laparoscopic approaches of radiofrequency ablation treatment for liver cancer. J Hepatobiliary Pancreat Surg. 2003;10:425–7.
Acknowledgments
The authors thank Kensuke Nuruki and Yoshitio Ogura (Department of Surgical Oncology and Digestive Surgery, Kagoshima University Graduate School of Medical and Dental Sciences, Kagoshima); Yasushi Imamura, Takuya Hiwaki, Yasunari Hiramine, Masahiro Hamanoue, and Shigeho Maenohara (Department of Internal Medicine, JA Kagoshima Kouseiren Hospital, Kagoshima); Toshihiko Shibatou, Katsumi Sako, Yasuji Komorizono, Shuho Shigenobu, Tsutomu Tamai, Koutaro Kumagaya, Akihiro Moriuchi, Hirohumi Uto, Makoto Oketani, and Akio Ido (Department of Digestive and Life-style related Disease, Kagoshima University Graduate School of Medical and Dental Sciences, Kagoshima) for their material support and technical help.
Author information
Authors and Affiliations
Consortia
Corresponding author
About this article
Cite this article
Ueno, S., Sakoda, M., Kubo, F. et al. Surgical resection versus radiofrequency ablation for small hepatocellular carcinomas within the Milan criteria. J Hepatobiliary Pancreat Surg 16, 359–366 (2009). https://doi.org/10.1007/s00534-009-0069-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00534-009-0069-7