Abstract
Background
A major concern in the use of the argon beam coagulator system is the potential risk of argon gas embolism.
Methods
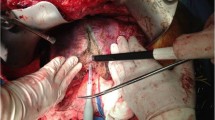
Seven cases with argon gas embolism in the English literature were reviewed along with the current case. The latter case was a 77-year-old female having laparoscopic hepatectomy after application of the microwave coagulation system on the cutting planes.
Results
Immediately following shots of an argon beam to control local bleeding at the needle hole in the liver caused by microwave coagulation, the end-tidal carbon disappeared, followed by cardiovascular collapse. After 18 min of cardiovascular resuscitation, the tumors were resected under laparotomy.
Conclusions
After reviewing the cases, pneumoperitoneum (57.1%), hepatic needle punctures (42.8%) and direct application of the argon beam to the liver (28.6%) can be considered as risky processes in such events. Caution is necessary in the use of an argon beam in liver surgery to avoid life-threatening gas embolism.



Similar content being viewed by others
Abbreviations
- ABC:
-
Argon beam coagulator
- HCC:
-
Hepatocellular carcinoma
- LC:
-
Liver cirrhosis
- Lap:
-
Laparoscope
- MCT:
-
Microwave coagulation therapy
- N/A:
-
Not available
- PTLD:
-
Post-transplant lymphoproliferative disorders
- s/p LTx:
-
State of post liver transplantation
References
Yamashita Y, Takada T, Kawarada Y, et al. Surgical treatment of patients with acute cholecystitis: Tokyo guidelines. J Hepatobiliary Pancreat Surg 2007;14:91–7.
Shimada M, Hashizume M, Maehara S, et al. Laparoscopic hepatectomy for hepatocellular carcinoma. Surg Endosc. 2001;15:541–4.
Kaneko H. Laparoscopic hepatectomy: indications and outcomes. J Hepatobiliary Pancreat Surg. 2005;12:438–43.
Belli G, Fantini C, D’Agostino A, et al. Laparoscopic hepatic resection for completely exophytic hepatocellular carcinoma on cirrhosis. J Hepatobiliary Pancreat Surg. 2005;12:488–93.
Belli G, Fantini C, D’Agostino A, Belli A, Cioffi L, Russolillo N. Laparoscopic left lateral hepatic lobectomy: a safer and faster technique. J Hepatobiliary Pancreat Surg. 2006;13:149–54.
ECRI. Argon beam coagulation systems. Health Devices. 1994;19:299–320.
Croce E, Azzola M, Russo R, et al. Laparoscopic liver tumour resection with the argon beam. Endosc Surg Allied Technol. 1994;2:186–8.
Veyckemans F, Michel I, et al. Venous gas embolism from an Argon coagulator. Anesthesiology. 1996;85:443–4.
Stojeba N, Mahoudeau G, Segura P, et al. Possible venous argon gas embolism complicating argon gas enhanced coagulation during liver surgery. Acta Anaesthesiol Scand. 1999;43:866–7.
Kono M, Yahagi N, Kitahara M, et al. Cardiac arrest associated with use of an argon beam coagulator during laparoscopic cholecystectomy. Br J Anaesth. 2001;87:644–6.
Ousmane ML, Fleyfel M, Vallet B. Venous gas embolism during liver surgery with argon-enhanced coagulation. Eur J Anaesthesiol. 2002;19:225.
Min SK, Kim JH, Lee SY. Carbon dioxide and argon gas embolism during laparoscopic hepatic resection. Acta Anaesthesiol Scand. 2007;51:949–53.
Palmer M, Miller CW, van Way CW 3rd, et al. Venous gas embolism associated with argon-enhanced coagulation of the liver. J Invest Surg. 1993;6:391–9.
Van Thiel DH, Gavaler JS, Wright H, et al. Liver biopsy. Its safety and complications as seen at a liver transplant center. Transplantation. 1993;55:1087–90.
Midorikawa T, Kumada K, Kikuchi H, et al. Microwave coagulation therapy for hepatocellular carcinoma. J Hepatobiliary Pancreat Surg. 2000;7:252–9.
Adornato DC, Gildenberg PL, Ferrario CM, et al. Pathophysiology of intravenous air embolism in dogs. Anesthesiology. 1978;49:120–7.
Roberts MW, Mathiesen KA, Ho HS, et al. Cardiopulmonary responses to intravenous infusion of soluble and relatively insoluble gases. Surg Endosc. 1997;11:341–6.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Ikegami, T., Shimada, M., Imura, S. et al. Argon gas embolism in the application of laparoscopic microwave coagulation therapy. J Hepatobiliary Pancreat Surg 16, 394–398 (2009). https://doi.org/10.1007/s00534-008-0039-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00534-008-0039-5