Abstract
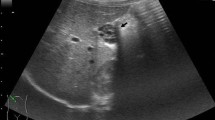
We herein report a case of gallbladder carcinoma associated with occult pancreatobiliary reflux (PR) in the absence of pancreatobiliary maljunction. A 67-year-old woman was referred to our hospital for the evaluation and treatment of a gallbladder tumor. Ultrasonography and computed tomography showed a nodular lesion in the fundus of the gallbladder, indicating the possibility of a gallbladder carcinoma. Endoscopic ultrasonography showed the nodular tumor and thickness of the surrounding epithelium. Endoscopic retrograde cholangiopancreatography revealed a normal pancreaticobiliary junction without the common channel and a slight dilatation of the common bile duct (15 mm in diameter). An open cholecystectomy and partial resection of the liver bed of the gallbladder with regional lymphadenectomy was performed. A C-tube was inserted from the cut end of the cystic duct into the common bile duct to prevent bile stasis. Biliary amylase and lipase levels sampled in the gallbladder were 2604 IU/l and 775 IU/l, respectively. Biliary amylase level in the bile collected from the C-tube in the common bile duct was 119 550 IU/l on postoperative day (POD) 6 and 22 265 IU/l on POD 12. These observations suggested that PR was present in this patient. The histopathological findings of the resected specimen showed a well-differentiated adenocarcinoma of the gallbladder with invasion to the muscle layer and no metastasis of the resected lymph nodes. A high index of nuclear staining for MIB-I in the cancer cells (about 10%) was exhibited, and a few cells in the normal epithelium also stained positive.
Similar content being viewed by others
References
InstitutionalAuthorNameThe Japanese Study Group on Pancreaticobiliary Maljunction (1994) ArticleTitleDiagnostic criteria of pancreaticobiliary maljunction J Hepatobiliary Pancreat Surg 1 219–21 Occurrence Handle10.1007/BF02391070
S Tashiro T Imaizumi H Ohkawa A Okada T Katoh Y Kawarada et al. (2003) ArticleTitlePancreaticobiliary maljunction: retrospective and national-wide survey in Japan J Hepatobiliary Pancreat Surg 10 345–51 Occurrence Handle14598134 Occurrence Handle10.1007/s00534-002-0741-7
M Seki A Yanagisawa E Ninomiya Y Ninomiya H Ohta A Saiura et al. (2005) ArticleTitleClinicopathology of pancreaticobiliary maljunction: relationship between alterations in background biliary epithelium and neoplastic development J Hepatobiliary Pancreat Surg 12 254–62 Occurrence Handle15995816 Occurrence Handle10.1007/s00534-004-0966-8
S Yamauchi A Koga S Matsumoto M Tanaka F Nakayama (1987) ArticleTitleAnomalous junction of pancreaticobiliary duct without congenital choledochal cyst: a possible risk factor for gallbladder cancer Am J Gastroenterol 82 20–4 Occurrence Handle3799576 Occurrence Handle1:STN:280:BiiD1MjhvVY%3D
T Kamisawa A Okamoto (2006) ArticleTitleBiliopancreatic and pancreatobiliary refluxes in cases with and without pancreatobiliary maljunction: diagnosis and clinical implication Digestion 73 328–36 Occurrence Handle10.1159/000095424
F Itokawa T Itoi K Nakamura A Sofuni K Kakimi F Moriyasu et al. (2004) ArticleTitleAssessment of occult pancreatobiliary reflux in patients with pancreaticobiliary disease by ERCP J Gastroenterol 39 988–94 Occurrence Handle15549453 Occurrence Handle10.1007/s00535-004-1428-4
JK Sai M Suyama Y Kubokawa (2006) ArticleTitleA case of gallbladder carcinoma associated with pancreatobiliary reflux in the absence of a pancreaticobiliary maljunction: a hint for early diagnosis of gallbladder carcinoma World J Gastroenterol 12 4593–5 Occurrence Handle16874881
JK Sai M Suyama B Nobukawa Y Kubokawa N Sato (2005) ArticleTitleSevere dysplasia of the gallbladder associated with occult pancreatobiliary reflux J Gastroenterol 40 756–60 Occurrence Handle16082594 Occurrence Handle10.1007/s00535-005-1621-0
JK Sai M Suyama B Nobukawa Y Kubokawa K Yokomizo N Sato (2005) ArticleTitlePrecancerous mucosal changes in the gallbladder of patients with occult pancreatobiliary reflux Gastrointes Endosc 61 264–8 Occurrence Handle10.1016/S0016-5107(04)02586-6
M Sugiyama Y Atomi (2001) ArticleTitlePeriampullary diverticula cause pancreatobiliary reflux Scand J Gastroenterol 9 994–7 Occurrence Handle10.1080/003655201750305549
JK Sai J Ariyama M Suyama Y Kubokawa N Sato (2002) ArticleTitleOccult regurgitation of pancreatic juice into the biliary tract: Diagnosis with secretin injection magnetic resonance cholangiopancreatography Gastrointest Endosc 56 929–32 Occurrence Handle12447317 Occurrence Handle10.1016/S0016-5107(02)70379-9
T Itoi A Tsuchida F Itokawa A Sofuni T Kurihara T Tsuchiya et al. (2005) ArticleTitleHistologic and genetic analysis of the gallbladder in patients with occult pancreatobiliary reflux Int J Mol Med 15 425–30 Occurrence Handle15702232
M Sugiyama Y Atomi (1999) ArticleTitleDoes endoscopic sphincterotomy cause prolonged pancreatobiliary reflux? Am J Gastroenterol 94 795–8 Occurrence Handle10086668 Occurrence Handle10.1111/j.1572-0241.1999.00953.x Occurrence Handle1:STN:280:DyaK1M7osVCksA%3D%3D
Author information
Authors and Affiliations
About this article
Cite this article
Inagaki, M., Goto, J., Suzuki, S. et al. Gallbladder carcinoma associated with occult pancreatobiliary reflux in the absence of pancreaticobiliary maljunction. J Hepatobiliary Pancreat Surg 14, 529–533 (2007). https://doi.org/10.1007/s00534-006-1217-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00534-006-1217-y