Abstract
Purpose
This systematic review aims to identify the risk factors for depression in cancer patients undergoing chemotherapy.
Methods
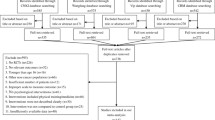
Eight electronic databases were searched from inception of the databases established until August 2017. References for the included studies were retrieved by manual searching. The quality of the eligible studies was appraised by two persons using the 11-item checklist of the Agency for Healthcare Research and Quality (AHRQ).
Results
Among 5988 potentially relevant articles, 43 studies were eligible, with 17 studies of high quality and 25 studies of moderate quality. A total of 65 factors were extracted, including sociodemographic characteristics (n = 20), physiological condition (n = 20), disease and treatment (n = 12), and psychosocial factors (n = 13). Only social support, anxiety, perceived stress, and self-efficacy were found to be consistently associated with depression in cancer patients. There is not enough evidence to support the link between the other 61 factors and depression in cancer patients undergoing chemotherapy.
Conclusions
This review suggests that the development of depression programs should take social support, anxiety, perceived stress, and self-efficacy into account. More original studies with rigorous design are necessary to further confirm those 61 inconclusive risk factors for depression in cancer patients receiving chemotherapy.

Similar content being viewed by others
References
Bergerot CD, Mitchell HR, Ashing KT, Kim Y (2017) A prospective study of changes in anxiety, depression, and problems in living during chemotherapy treatments: effects of age and gender. Support Care Cancer 25:1897–1904
Piacentine LB, Miller JF, Haberlein S, Bloom AS (2015) Perceived cognitive changes with chemotherapy for breast cancer: a pilot study. Appl Nurs Res 29:9–11
Duc S, Rainfray M, Soubeyran P, Fonck M, Blanc JF, Ceccaldi J, Cany L, Brouste V, Mathoulinpélissier S (2016) Predictive factors of depressive symptoms of elderly patients with cancer receiving first-line chemotherapy. Psycho-Oncology 26:15–21
Mitchell AJ, Chan M, Bhatti H, Halton M, Grassi L, Johansen C, Meader N (2011) Prevalence of depression, anxiety, and adjustment disorder in oncological, haematological, and palliative-care settings: a meta-analysis of 94 interview-based studies. Lancet Oncol 12:160–174
Saevarsdottir T, Fridriksdottir N, Gunnarsdottir S (2010) Quality of life and symptoms of anxiety and depression of patients receiving cancer chemotherapy. Cancer Nurs 33:e1–e10
Chen SJ, Chang CH, Chen KC, Liu CY (2016) Association between depressive disorders and risk of breast cancer recurrence after curative surgery. Medicine 95:e4547
Schneider S, Moyer A (2009) Depression as a predictor of disease progression and mortality in cancer patients: a meta-analysis. Cancer 115:3304–3305
Polikandrioti M, Evaggelou E, Zerva S, Zerdila M, Koukoularis D, Kyritsi E (2008) Evaluation of depression in patients undergoing chemotherapy. Health Sci J 2:162–172
Park H, Yoon HG (2013) Menopausal symptoms, sexual function, depression, and quality of life in Korean patients with breast cancer receiving chemotherapy. Support Care Cancer 21:2499–2507
Jehn CF, Becker B, Flath B, Nogai H, Vuong L, Schmid P, Lüftner D (2015) Neurocognitive function, brain-derived neurotrophic factor (BDNF) and IL-6 levels in cancer patients with depression. J Neuroimmunol 287:88–92
Fagundes C, Jones D, Vichaya E, Lu C, Cleeland CS (2014) Socioeconomic status is associated with depressive severity among patients with advanced non-small cell lung cancer: treatment setting and minority status do not make a difference. J Thorac Oncol 9:1459–1463
Yan L, Yuan C (2011) Levels of fatigue in Chinese women with breast cancer and its correlates: a cross-sectional questionnaire survey. J Am Assoc Nurse Pract 23:153–160
Akechi T, Okuyama T, Uchida M, Nakaguchi T, Sugano K, Kubota Y, Ito Y, Kizawa Y, Komatsu H (2012) Clinical indicators of depression among ambulatory cancer patients undergoing chemotherapy. Jpn J Clin Oncol 42:1175–1180
Farrell C, Brearley SG, Pilling M, Molassiotis A (2013) The impact of chemotherapy-related nausea on patients’ nutritional status, psychological distress and quality of life. Support Care Cancer 21:59–66
Haisfield-Wolfe ME, Mcguire DB, Soeken K, Geiger-Brown J, De Forge BR (2009) Prevalence and correlates of depression among patients with head and neck cancer: a systematic review of implications for research. Oncol Nurs Forum 36:107–125
Brandão T, Schulz MS, Matos PM (2017) Psychological adjustment after breast cancer: a systematic review of longitudinal studies. Psycho-Oncology 26:917–926
Caruso R, Nanni MG, Riba M, Sabato S, Mitchell AJ, Croce E, Grassi L (2017) Depressive spectrum disorders in cancer: prevalence, risk factors and screening for depression: a critical review. Acta Oncol 56:146–155
Shuangshuang W, Yanqing Y, Huimin X, Xiuyan L, Ying C (2016) Systematic review and meta-analysis of the risk factors for depression in cancer chemotherapy patients. http://www.crd.york.ac.uk/PROSPERO/display_record.php?ID=CRD42016036619. Accessed 24 March 2016
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Lijun F, Shujing W, Hua W (2011) Prevalence of depression and the relationship between depression and social support in chemotherapy patients. J Qilu Nurs 17:31–32
Mei T (2008) Prevalence of depression in chemotherapy patients. Chin Gen Pract Nurs 6:1601–1603. https://doi.org/10.3969/j.issn.1674-4748.2008.18.002
Faul LA, Jim HS, Minton S, Fishman M, Tanvetyanon T, Jacobsen PB (2011) Relationship of exercise to quality of life in cancer patients beginning chemotherapy. J Pain Symptom Manag 41:859–869
Jianci Z (2015) Influencing factors of negative emotions and well - being in chemotherapy patients and observation of psychological intervention. Chin J Prim Med Pharm 22:765–767. https://doi.org/10.3760/cma.j.issn.1008-6706.2015.05.045
Xu L (2014) The change of quality of life, anxiety and depression and the influencing factors of patients with lung cancer before and after chemotherapy. Dissertation,Tianjin Medical University
Mielcarek P, Nowicka-Sauer K, Kozaka J (2017) Anxiety and depression in patients with advanced ovarian cancer: a prospective study. J Psychosom Obstet Gynecol 37:57–67
Pandey M, Sarita GP, Devi N, Thomas BC, Hussain BM, Krishnan R (2006) Distress, anxiety, and depression in cancer patients undergoing chemotherapy. World J Surg Oncol 4:68
Quattropani MC, Lenzo V, Filastro A (2017) Predictive factors of anxiety and depression symptoms in patients with breast cancer undergoing chemotherapy. An explorative study based on metacognitions 23:67–73
Meihua W, Yanyun W, Xiuying C, Gong Z, Xiaohong C, Xiuyu Y (2004) Investigation on the influence factors of depression in chemotherapy patients and nursing countermeasures. Fujian Med J 26:201–202. https://doi.org/10.3969/j.issn.1002-2600.2004.06.150
Wen Q, Shao Z, Zhang P, Zhu T, Li D, Wang S (2017) Mental distress, quality of life and social support in recurrent ovarian cancer patients during active chemotherapy. Eur J Obstet Gynecol Reprod Biol 216:85–91
Heinze S, Egberts F, Rötzer S, Volkenandt M, Tilgen W, Linse R, Boettjer J, Vogt T, Spieth K, Eigentler T (2010) Depressive mood changes and psychiatric symptoms during 12-month low-dose interferon-[alpha] treatment in patients with malignant melanoma: results from the multicenter DeCOG trial. J Immunother 33:106–114
Chintamani GA, Khandelwal R, Tandon M, Jain S, Kumar Y, Narayan N, Bamal R, Srinivas S, Saxena S (2011) The correlation of anxiety and depression levels with response to neoadjuvant chemotherapy in patients with breast cancer. J Royal Soc Med Cardiovasc Dis 2:15
Dehua L, Hui Z, Xiujing G, Jing F (2016) Associations between stress coping strategies and perceived social support in young patients with gynecologic cancers. J Sichuan Univ (Medical Science Edition) 47:402–405. https://doi.org/10.13464/j.scuxbyxb.2016.03.021
Mills PJ, Parker B, Dimsdale JE, Sadler GR, Ancoli-Israel S (2005) The relationship between fatigue and quality of life and inflammation during anthracycline-based chemotherapy in breast cancer. Biol Psychol 69:85–96
Jianhong L, Xiaoli Z, Liuliu Z (2011) Investigation and analysis of psychological status and its related factors for patients with cancer chemotherapy. Int J Nurs (China) 30:1382–1384. https://doi.org/10.3760/cma.j.issn.1673-4351.2011.09.052
Saini A, Berruti A, Ferini-Strambi L, Castronovo V, Rametti E, Giuliano PL, Ramassotto B, Picci RL, Negro M, Campagna S (2013) Restless legs syndrome as a cause of sleep disturbances in cancer patients receiving chemotherapy. J Pain Symptom Manag 46:56–64
Kim SH, Kim M, Lee HS (2016) Symptom clusters in Korean patients with metastatic cancer undergoing palliative chemotherapy. J Hosp Palliat Nurs 18:292–299
Choi EK, Kim IR, Chang O, Kang D, Nam SJ, Lee JE, Lee SK, Im YH, Park YH, Yang JH (2014) Impact of chemotherapy-induced alopecia distress on body image, psychosocial well-being, and depression in breast cancer patients. Psycho-Oncology 23:1103–1110
de Moor JS, de Moor CA, Basenengquist K, Kudelka A, Bevers MW, Cohen L (2006) Optimism, distress, health-related quality of life, and change in cancer antigen 125 among patients with ovarian cancer undergoing chemotherapy. Psychosom Med 68:555–562
Chou HL, Chao TY, Chen TC, Chu CM, Hsieh CH, Yao CT, Janckila AJ (2016) The relationship between inflammatory biomarkers and symptom distress in lung cancer patients undergoing chemotherapy. Cancer Nurs 40:e1–e8
Bergerot CD, Clark KL, Nonino A, Waliany S, Buso MM, Loscalzo M (2015) Course of distress, anxiety, and depression in hematological cancer patients: association between gender and grade of neoplasm. Palliat Support Care 13:115–123
Dai YL, Yang CT, Chen KH, Tang ST (2016) Changes to and determinants of quality of life in patients with advanced non-small-cell lung cancer undergoing initial chemotherapy. J Nurs Res Jnr 25:203–215
Decat CS, de Araujo TC, Stiles J (2011) Distress levels in patients undergoing chemotherapy in Brazil. Psycho-Oncology 20:1130–1133
Meraner V, Gamper EM, Grahmann A, Giesinger JM, Wiesbauer P, Sztankay M, Zeimet AG, Sperner-Unterweger B, Holzner B (2012) Monitoring physical and psychosocial symptom trajectories in ovarian cancer patients receiving chemotherapy. BMC Cancer 12:77
Jiayuan Z, Yuqiu Z, Ziwei F, Yong X, Guangchun Z (2018) Longitudinal trends in anxiety, depression, and quality of life during different intermittent periods of adjuvant breast cancer chemotherapy. Cancer Nurs 41:62–68
Hipkins J, Whitworth M, Tarrier N, Jayson G (2004) Social support, anxiety and depression after chemotherapy for ovarian cancer: a prospective study. Br J Health Psychol 9:569–581
Polat U, Arpacı A, Demir S, Erdal S, Yalcin S (2014) Evaluation of quality of life and anxiety and depression levels in patients receiving chemotherapy for colorectal cancer: impact of patient education before treatment initiation. J Gastrointest Oncol 5:270–275
Gruenigen VEV, Hutchins JR, Reidy AM, Gibbons HE, Daly BJ, Eldermire EM, Fusco NL (2006) Gynecologic oncology patients’ satisfaction and symptom severity during palliative chemotherapy. Health Quality Life Outcomes 4:1–6
Ostacoli L, Saini A, Zuffranieri M, Boglione A, Carletto S, Marco ID, Lombardi I, Picci RL, Berruti A, Comandone A (2014) Quality of life, anxiety and depression in soft tissue sarcomas as compared to more common tumours: an observational study. Appl Res Qual Life 9:123–131
Jihua W, Defang Z, Yingli X (2012) Relationship between depression and social support in chemotherapy patients. Mod J Integr Tradit Chin Western Med 21:4078–4079. https://doi.org/10.3969/j.issn.1008-8849.2012.36.044
Ostacoli L, Saini A, Ferini-Strambi L, Castronovo V, Sguazzotti E, Picci RL, Toje M, Gorzegno G, Capogna S, Dongiovanni V (2010) Restless legs syndrome and its relationship with anxiety, depression, and quality of life in cancer patients undergoing chemotherapy. Qual Life Res Int J Qual Life Aspects Treat Care Rehabil 19:531–537
Xiyuan F, Biru L (2012) Correlative analysis of self-management efficacy and anxiety and depression in patients with gynecological chemotherapy. West China Med J 27:1667–1669 http://kns.cnki.net/KCMS/detail/detail.aspx?dbcode=CJFQ&dbname=CJFD2012&filename=HXYX201211028&uid=WEEvREcwSlJHSldRa1FhcTdWajFuQ2FYWmErbVJpL3AyUk9wSGtQRWxpZz0=$9A4hF_YAuvQ5obgVAqNKPCYcEjKensW4ggI8Fm4gTkoUKaID8j8gFw!!&v=MjYyNDR1eFlTN0RoMVQzcVRyV00xRnJDVVJMS2ZaT1JzRnluZ1U3dk1MVFhTZHJHNEg5UE5ybzlIYklSOGVYMUw=. Accessed 24 Nov 2012
Xiaohong W, Feng Y (2016) The relationship between self - care ability, hope level and depression in patients with breast cancer during chemotherapy. Matern Child Health Care China 31:3898–3900. https://doi.org/10.7620/zgfybj.j.issn.1001-4411.2016.19.08
Jiangyan S, Liwei W, Huiping L, Yuqing P (2010) Correlation between depression of cancer patients undergoing chemotherapy and coping style and quality of life. J Nurs 17:5–8. https://doi.org/10.3969/j.issn.1008-9969.2010.05.002
Blank TO, Bellizzi KM (2008) A gerontologic perspective on cancer and aging. Cancer 112:2569–2576
Huang CQ, Wang ZR, Li YH, Xie YZ, Liu QX (2010) Education and risk for late life depression: a meta-analysis of published literature. Int J Psychiatry Med 40:109–124
Spangler DL, Simons AD, Monroe SM, Thase ME (1996) Gender differences in cognitive diathesis-stress domain match: implications for differential pathways to depression. J Abnorm Psychol 105:653–657
Skarupski KA, Tangney C, Li H, Ouyang B, Evans DA, Morris MC (2010) Longitudinal association of vitamin B-6, folate, and vitamin B-12 with depressive symptoms among older adults over time. Am J Clin Nutr 92:330–335
Alpert JE, Fava M (1997) Nutrition and depression: the role of folate. Nutr Rev 55:145–149
Phillips RM (2012) Nutrition and depression in the community-based oldest-old. Home Healthcare Nurse 30:462–471
Licinio-Paixao J (1989) Hyperinsulinemia; a mediator of decreased food intake and weight loss in anorexia nervosa and major depression. Med Hypotheses 28(2):125–130
Bower JE, Ganz PA, Irwin MR, Kwan L, Breen EC, Cole SW (2011) Inflammation and behavioral symptoms after breast cancer treatment: do fatigue, depression, and sleep disturbance share a common underlying mechanism. J Clin Oncol 29:3517–3522
Cho HJ, Savitz J, Dantzer R, Teague TK, Drevets WC, Irwin MR (2017) Sleep disturbance and kynurenine metabolism in depression. J Psychosom Res 99:1–7
Wang XS, Shi Q, Williams LA, Mao L, Cleeland CS, Komaki RR, Mobley GM, Liao Z (2010) Inflammatory cytokines are associated with the development of symptom burden in patients with NSCLC undergoing concurrent chemoradiation therapy. Brain Behav Immun 24:968–974
Krebber AMH, Buffart LM, Kleijn G, Riepma IC, Bree RD, Leemans CR, Becker A, Brug J, Straten AV, Cuijpers P (2014) Prevalence of depression in cancer patients: a meta-analysis of diagnostic interviews and self-report instruments. Psycho-Oncology 23:121–130
Gariépy G, Honkaniemi H, Quesnel-Vallée A (2016) Social support and protection from depression: systematic review of current findings in Western countries. Br J Psychiatry 209:284–293
Jacobson NC, Newman MG (2014) Avoidance mediates the relationship between anxiety and depression over a decade later. J Anxiety Disord 28(5):437–445
Bandura A (1977) Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev 84:191–215
Funding
The study was supported by the National Natural Science Foundation of China [8140, 1863].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Wen, S., Xiao, H. & Yang, Y. The risk factors for depression in cancer patients undergoing chemotherapy: a systematic review. Support Care Cancer 27, 57–67 (2019). https://doi.org/10.1007/s00520-018-4466-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-018-4466-9