Abstract
Purpose
This prospective study describes disease/treatment, personal characteristics, and social/family contextual variables as risk and resilience factors that predict social competence in pediatric brain tumor survivors (PBTS).
Methods
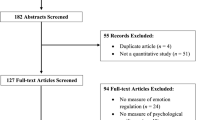
Ninety-one PBTS (51% male, mean age 11.21 years, off-treatment, attending a regular classroom >50% of the time) participated. PBTS and their primary caregivers (proxy) completed the Social Skills Rating System (SSRS) to assess social competence at baseline, 2, and 8 months follow-up. At baseline, medical information (e.g., tumor type and location, cranial irradiation therapy (CIT)), personal characteristics (e.g., child’s age and gender, intelligence, executive function, attention, and memory), and social/family factors (family income and ethnicity) were obtained.
Results
Using mixed model multivariable analyses with a longitudinal component, tumor type (medulloblastoma) (p < 0.01) and poor executive function, specifically, emotional control, were the best predictors of low total and assertion self-reported SSRS scores (p < 0.02). Receiving CIT was associated with low proxy-reported assertion (p = 0.035), and cooperation score (p = 0.02). Poor emotional control was associated with low proxy-reported total (p = 0.032), assertion (p = 0.023), and self-control scores (p = 0.007). Being non-White was associated with low proxy-reported total (p = 0.016), self-control (p = 0.040), responsibility (p = 0.035), and cooperation scores (p = 0.002). There were no significant changes over time.
Conclusions
This study supports a multifactorial model of insult and non-insult factors (medical, personal, and social context) as determinants of social competence in PBTS. Data from both informants identify determinants of social competence. These factors need to be considered in future interventions to help children better improve their social competence.





Similar content being viewed by others
References
Kaatsch P (2010) Epidemiology of childhood cancer. Cancer Treat Rev 36(4):2777–2785
Patel S, Bhatnagar A, Wear C, Osiro S, Gabriel A, Kimball D, John A, Fields PJ, Tubbs S, Loukas M (2014) Are pediatric brain tumors on the rise in the USA? Significant incidence and survival findings from the SEER database analysis. Childs Nerv Syst 30:147–154
Barrera M, Shaw AK, Speechley KN, Maunsell E, Pogany L (2005) Educational and social late effects of childhood cancer and related clinical, personal, and familial characteristics. Cancer 104:1751–1760
De Ruiter MA, Van Mourik R, Schouten Van Meeteren AY, Grootenhuis MA, Oosterlaan J (2013) Neurocognitive consequences of a paediatric brain tumour and its treatment: a meta-analysis. Dev Med Child Neurol 55:408–417
Robinson KE, Fraley CE, Pearson MM, Kuttesch JF Jr, Compas BE (2013) Neurocognitive late effects of pediatric brain tumors of the posterior fossa: a quantitative review. J Int Neuropsychol Soc 19:44–53
Roddy E, Mueller S (2016) Late effects of treatment of pediatric central nervous system tumors. J Child Neurol 31:237–254
Turner CD, Rey-Casserly C, Liptak CC, Chordas C (2009) Late effects of therapy for pediatric brain tumor survivors. J Child Neurol 24:1455–1463
Vannatta K, Gerhardt C, Wells R, Noll RB (2007) Intensity of CNS treatment of pediatric cancer: prediction of social outcomes. Pediatr Blood Cancer 49:716–722
Gurney JG, Krull KR, Kadan-Lottick N, Nicholson HS, Nathan PC, Zebrack B, Tersak JM, Ness KK (2009) Social outcomes in the childhood cancer survivor study cohort. J Clin Oncol 27(14):2390–2395
Hudson MM, Mertens AC, Yasui Y, Hobbie W, Chen H, Gurney JG, Yeazel M, Recklitis CJ, Marina N, Robison LR, Oeffinger KC (2003) Health status of adult long-term survivors of childhood cancer; a report from the childhood cancer survivor study. JAMA 290:1583–1592
Cavell TA (1990) Social adjustment, social performance and social skills: a tri-component model of social competence. J Child Clin Psychol 19:111–122
Yeates KO, Bigler ED, Dennis M, Gerhardt CA, Rubin KH, Stancin T, Taylor HG, Vannatta K (2007) Social outcomes in childhood brain disorder: a heuristic integration of social neuroscience and developmental psychology. Pyschol Bull 133:535–566
Butler RW, Fairclough DL, Katz ER, Kazak AE, Noll RB, Thompson RD, Sahler OJ (2013) Intellectual functioning and multi-dimensional attentional processes in long-term survivors of a central nervous system related pediatric malignancy. Life Sci 93:611–616
Gunn M, Mört S, Arola M, Taskinen M, Riikonen P, Möttönen M, Lähteenmäki PM (2015) Quality of life and late-effects among childhood brain tumor survivors: a mixed method analysis. Psychooncology 25(6):677–683
Boman KK, Lindblad F, Hjern A (2010) Long-term outcomes of childhood cancer survivors in Sweden: a population-based study of education, employment, and income. Cancer 116:1385–1391
Carlson SM, Moses LJ, Claxton LJ (2004) Individual differences in executive functioning and theory of mind: an investigation of inhibitory control and planning ability. J Exp Child Psychol 87(4):299–319
Crick NR, Dodge KA (1994) A review and reformulation of social information-processing mechanisms in children’s social adjustment. Psychol Bull 115:74–101
Lemerise EA, Arsenio WF (2000) An integrated model of emotion processes and cognition in social information processing. Child Dev 71(1):107–118
Schulte F, Barrera M (2014) Social competence in childhood brain tumor survivors: evaluating the psychometric properties of assessment tools. Support Care Cancer 22(2):561–569
Hocking MC, McCurdy M, Turner E, Kazak AE, Noll RB, Phillips P, Barakat LP (2015) Social competence in pediatric brain tumor survivors: application of a model from social neuroscience and developmental psychology. Pediatric Blood Cancer 62:375–384
Bhat SR, Goodwin TL, Burwinkle TM, Lansdale MF, Dahl GV, Huhn SL, Gibbs IC, Donaldson SS, Rosenblum RK, Varni JW, Fisher PG (2005) Profile of daily life in children with brain tumors: an assessment of health-related quality of life. J Clin Oncol 23:5493–5500
Sands SA, Milner JS, Goldberg J, Mukhi V, Moliterno JA, Maxfield C, Wisoff JH (2005) Quality of life and behavioral follow-up study of pediatric survivors of craniopharyngioma. J Neurosurg 103:302–311
Patel SK, Mullins WA, O'Neil SH, Wilson K (2011) Neuropsychological differences between survivors of supratentorial and infratentorial brain tumours. J Intellect Disabil Res 55:30–40
Larysz D, Blamek S, Larysz P, Pietras K, Mandera M (2010) Posterior fossa brain tissue injury: developmental, neuropsychological, and neurological consequences of brain tumors in children. Acta Neurochir Suppl 106:271–274
Jain N, Krull KR, Brouwers P, Chintagumpala MM, Woo SY (2008) Neuropsychological outcome following intensity-modulated radiation therapy for pediatric medulloblastoma. Pediatr Blood Cancer 51:275–279
Knight SJ, Conklin HM, Palmer SL, Schreiber JE, Armstrong CL, Wallace D et al (2014) Working memory abilities among children treated for medulloblastoma: parent report and child performance. J Pediatr Psychol 39:501–511
Robinson KE, Kutlesch JF, Champion JE, Anderotti CF, Hipp DW, Bettis A et al (2010) A qualitative meta-analysis of neurocognitive sequalae in survivors or pediatric brain tumours. Pediatr Blood Cancer 55:525–531
Wolfe KR, Walsh KS, Reynolds NC, Mitchell F, Reddy AT, Paitin I, Madan-Swain A (2013) Executive functions and social skills in survivors of pediatric brain tumor. Child Neuropsychol 19:370–384
Poggi G, Liscio M, Galbiati S, Adduci A, Massimino M, Gandola L et al (2005) Brain tumors in children and adolescents: cognitive and psychological disorders at different ages. Psychooncology 14:386–395
Kullgren KA, Morris RD, Morris MK, Krawiecki N (2003) Risk factors associated with long-term social and behavioral problems among children with brain tumors. J Psychosoc Oncol 21(1):73–87
Barrera M, Schulte F (2009) A group social skills intervention program for survivors of childhood brain tumors. J Pediatr Psychol 34:1108–1118
Barrera M, Atenafu EG, Sung L, Bartels U, Schulte F, Chung J et al (2017) A randomized control intervention trial to improve social skills and quality of life in pediatric brain tumor survivors. Psychooncology. doi:10.1002/pon.4385
Gresham, FM, Elliott, SN (1990) Social skills rating system manual. American Guidance Service, Inc. Circle Pines, MN
Weschler D (1999) Wechsler Abbreviated Scale of Intelligence (WASI) manual. The Psychological Corporation, San Antonio
Gioia GA, Isquith PK, Guy SC (2000) Behavior rating inventory of executive function. Psychological Assessment Resources Lutz, FL
Conners CK, Staff MHS (eds) (2000) Conners’ Continuous Performance Test II: computer program for windows technical guide and software manual. Mutli-Health Systems North Tonwanda, NY
Talley JL (1993) Children’s auditory verbal learning test-2 professional manual. Psychological Assessment Resources, Odessa
Maddrey AM, Bergeron JA, Lombardo ER, McDonald NK, Mulne AF, Barenberg PD, Bowers DC (2005) Neuropsychological performance and quality of life of 10 year survivors of childhood medulloblastoma. J Neuro-Oncol 72(3):245–253
Ribi K, Relly C, Landolt MA, Alber FD, Boltshauser E, Grotzer MA (2005) Outcome of medulloblastoma in children: long-term complications and quality of life. Neuropediatrics 36(6):357–365
Hensler M, Wolfe K, Lebensburger J, Nieman J, Barnes M, Nolan W, King A, Madan-Swain A (2014) Social skills and executive function among youth with sickle cell disease: a preliminary investigation. J Pediatr Psychol 39(5):493–500
Kiley-Brabeck K, Sobin C (2006) Social skills and executive functioning deficits in children with the 22q11 deletion syndrome. Appl Neuopsychol 13(4):258–268
Schonfeld AM, Paley B, Frankel F, O’Connor MJ (2006) Executive functioning predicts social skills following prenatal alcohol exposure. Child Neuropsychol 12:439–452
Wells EM, Walsh KS, Khademian ZP, Keating RF, Packer RJ (2008) The cerebellar mutism syndrome and its relation to cerebellar cognitive function and the cerebellar cognitive affective disorder. Dev Disabil Res Rev 14(3):221–228
Bodranghien F, Bastian A, Casali C et al (2016) Consensus paper: revisiting the symptoms and signs of cerebellar syndrome. Cerebellum 15(3):369–391
Flores G (2010) Racial and ethnic disparities in the health and health care of children. Pediatrics 125(4):e979–e1020
Swartwout MD, Garnaat SL, Myszka KA, Fletcher JM, Dennis M (2010) Effects of ethnicity and SES on IQ and achievement in spina bifida meningomyelocele. J Pediatr Psychol 35(9):927–936
Meeske K, Katz ER, Palmer SN, Burwinkle T, Varni JW (2004) Parent proxy-reported health-related quality of life and fatigue in pediatric patients diagnosed with brain tumors and acute lymphoblastic leukemia. Cancer 101(9):2116–2125
Valenzuela J, Smith L (2016) Topical review: provider-patient interactions: an important consideration for racial/ethnic health disparities in youth. J Pediatr Psychol 41(4):473–480
Acknowledgements
The authors would like to thank the Canadian Cancer Research Society Institute for funding this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Each participating site obtained local Institutional Ethics Review Board approval.
Ethical approval
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Barrera, M., Atenafu, E.G., Schulte, F. et al. Determinants of social competence in pediatric brain tumor survivors who participated in an intervention study. Support Care Cancer 25, 2891–2898 (2017). https://doi.org/10.1007/s00520-017-3708-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-017-3708-6