Abstract
Purpose
A previous survey of the Multinational Association of Supportive Care in Cancer (MASCC) members found low frequency of spiritual care provision. We hypothesized that physicians with special training in palliative medicine would demonstrate an increased sense of responsibility for and higher self-reported adequacy to provide spiritual care to patients than health professionals with general training.
Methods
We surveyed members of the Australian and New Zealand Palliative Medicine Society (ANZSPM) to ascertain their spiritual care practices. We sent 445 e-mails on four occasions, inviting members to complete the online survey. Tabulated results were analyzed to describe the results.
Results
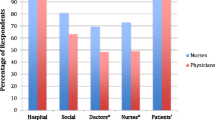
One hundred and fifty-eight members (35.5 %) responded. Physicians working primarily in palliative care comprised the majority (95 %) of the sample. Significantly more of the ANZSPM than MASCC respondents had previously received training in spiritual care and had pursued training in the previous 2 years. There was a significant difference between the two groups with regard to interest in and self-reported ability to provide spiritual care. Those who believed it was their responsibility to provide spiritual care were more likely to have had training, feel they could adequately provide spiritual care, and were more likely to refer patients if they could not provide spiritual care themselves.
Conclusions
Training in spiritual care was more common in healthcare workers who had received training in palliative care. ANZSPM members gave higher scores for both the importance of spiritual care and self-reported ability to provide it compared to MASCC members.
Similar content being viewed by others
References
Cobb M, Puchalski CM, Rumbold B (eds) (2012) Oxford textbook of spirituality in healthcare. Oxford University Press, Oxford
Best M, Butow P, Olver I (2014) The doctor’s role in helping dying patients with cancer achieve peace: a qualitative study. Palliat Med 28:1139–1145
Matthews D, McCullough M, DB L, et al. (1998) Religious commitment and health status: a review of the research and implications for family medicine. Arch Fam Med 7:118–124
Brady MJ, Peterman AH, Fitchett G, Mo M, Cella D (1999) A case for including spirituality in quality of life measurement in oncology. Psychooncology 8:417–428
Boston P, Towers A, Barnard D (2001) Embracing vulnerability: risk and empathy in palliative care. J Palliat Care 17:248–253
Edwards A, Pang N, Shiu V, Chan c (2010) Review: the understanding of spirituality and the potential role of spiritual care in end-of-life and palliative care: a meta-study of qualitative research. Palliat Med 24:753–770
Winkelman WD, Lauderdale K, Balboni MJ, Phelps AC, Peteet JR, Block SD, Kachnic LA, VanderWeele TJ, Balboni TA (2011) The relationship of spiritual concerns to the quality of life of advanced cancer patients: preliminary findings. J Palliat Med 14:1022–1028
Best M, Butow P, Olver I (2014) Spiritual support of cancer patients and the role of the doctor. Support Care Cancer 22:1333–1339
Best M, Butow P, Olver I (2015) Creating a safe space: a qualitative inquiry into the way doctors discuss spirituality. Palliat Support Care. doi:10.1017/S1478951515001236
Best M, Butow P, Olver I (2015) Do patients want doctors to talk about spirituality? A systematic literature review. Patient Educ Couns 98:1320–1328
Ramondetta LM, Sun C, Surbone A, Olver I, Ripamonti C, Konishi T, Baider L, Johnson J (2013) Surprising results regarding MASCC members’ beliefs about spiritual care. Support Care Cancer 21:2991–2998
Saunders CM (2006) Cicely Saunders: selected writings 1958–2004. Oxford University Press, Oxford
Sulmasy DP (2002) A biopsychosocial-spiritual model for the care of patients at the end of life. Gerontol 42:24–33
Best M, Butow P, Olver I (2015) Doctors discussing religion and spirituality: a systematic literature review. Palliat Med. doi:10.1177/0269216315600912
Braun V, Clarke V (2006) Using thematic analysis in psychology. Qual Res Psychol 3:77–101
Puchalski C, Romer AL (2000) Taking a spiritual history allows clinicians to understand patients more fully. J Palliat Med 3:129–137
Best M, Aldridge L, Butow P, Olver I, Webster F (2015) Conceptual analysis of suffering in cancer: a systematic review. Psychooncology 24:977–986
Phelps AC, Maciejewski PK, Nilsson M, Balboni TA, Wright AA, Paulk ME, Trice E, Schrag D, Peteet JR, Block SD, Prigerson HG (2009) Religious coping and use of intensive life-prolonging care near death in patients with advanced cancer. JAMA 301:1140–1147
Pargament KI, Koenig HG, Tarakeshwar N, Hahn J (2004) Religious coping methods as predictors of psychological, physical and spiritual outcomes among medically ill elderly patients: a two-year longitudinal study. J Health Psychol 9:713–730
Thompson GN, Chochinov HM, Wilson KG, McPherson CJ, Chary S, O’Shea FM, Kuhl DR, Fainsinger RL, Gagnon PR, Macmillan KA (2009) Prognostic acceptance and the well-being of patients receiving palliative care for cancer. J Clin Oncol 27:5757–5762
McClain CS, Rosenfeld B, Breitbart W (2003) Effect of spiritual well-being on end-of-life despair in terminally-ill cancer patients. Lancet 361:1603–1607
Handzo G, Koenig HG (2004) Spiritual Care: whose job is it anyway? South Med J 97:1242–1244
Puchalski CM, Vitillo R, Hull SK, Reller N (2014) Improving the spiritual dimension of whole person care: reaching national and international consensus. J Palliat Med 17:642–656
Alcorn S (2010) “If god wanted me yesterday, I wouldn’t be here today”: religious and spiritual themes in patients’ experiences of advanced cancer. J Palliat Med 13:581–588
Moadel A, Morgan C, Fatone A, Grennan J, Carter J, Laruffa G, Skummy A, Dutcher J (1999) Seeking meaning and hope: self-reported spiritual and existential needs among an ethnically-diverse cancer patient population. Psychooncology 8:378–385
Chochinov HM, Hack T, Hassard T, Kristjanson LJ, McClement S, Harlos M (2005) Dignity therapy: a novel psychotherapeutic intervention for patients near the end of life. J Clin Oncol 23:5520–5525
Epstein-Peterson ZD, Sullivan AJ, Enzinger AC, Trevino KM, Zollfrank AA, Balboni MJ, VanderWeele TJ, Balboni TA (2015) Examining forms of spiritual care provided in the advanced cancer setting. Am J Hospice Palliat Medicine 32(7):750–757
Surbone A, Baider L (2010) The spiritual dimension of cancer care. Crit Rev Oncol Hematol 73:228–235
Puchalski C, Ferrell B, Virani R, Otis-Green S, Baird P, Bull J, Chochinov H, Handzo G, Nelson-Becker H, Prince-Paul M, Pugliese K, Sulmasy D (2009) Improving the quality of spiritual care as a dimension of palliative care: the report of the Consensus Conference. J Palliat Med 12:885–904
Boston PH, Mount BM (2006) The caregiver’s perspective on existential and spiritual distress in palliative care. J Pain Symptom Manage 32:13–26
Holland JM, Neimeyer RA (2005) Reducing the risk of burnout in end-of-life care settings: the role of daily spiritual experiences and training. Palliat Support Care 3:173–181
Huggard P (2003) Compassion fatigue: how much can I give? Med Educ 37:163–164
Paal P, Helo Y, Frick E (2015) Spiritual care training provided to healthcare professionals: a systematic review. J Pastoral Care Counsel 69:19–30
Pargament KI, Zinnbauer BJ, Scott AB, Butter EM, Zerowin J, Stanik P (2003) Red flags and religious coping: Identifying some religious warning signs among people in crisis1. J Clin Psychol 59:1335–1348
Steinhauser K, Voils C, Clipp E, Bosworth H, Christakis N, Tulsky J (2006) “Are you at peace?”: One item to probe spiritual concerns at the end of life. Arch Int Med 166:101–105
Kristeller J, Zumbrun C, Schilling R (1999) ‘I would if I could’: how oncologists and oncology nurses address spiritual distress in cancer patients. Psychooncology 8:451–458
Best M, Aldridge L, Butow P, Olver I, Price M, Webster F (2014) Assessment of spiritual suffering in the cancer context: a systematic literature review. Palliat Support Care 13(5):1335–1361
Asai M, Morita T, Akechi T, Sugawara Y, Fujimori M, Akizuki N, Nakano T, Uchitomi Y (2007) Burnout and psychiatric morbidity among physicians engaged in end-of-life care for cancer patients: a cross-sectional nationwide survey in Japan. Psychooncology 16:421–428
Girgis A, Hansen V, Goldstein D (2009) Are Australian oncology health professionals burning out? A view from the trenches. Eur J Cancer 45:393–399
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest. The authors have full control of all primary data, and we agree to allow the journal to review the data if requested.
Rights and permissions
About this article
Cite this article
Best, M., Butow, P. & Olver, I. Palliative care specialists’ beliefs about spiritual care. Support Care Cancer 24, 3295–3306 (2016). https://doi.org/10.1007/s00520-016-3135-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-016-3135-0