Abstract
Purpose
Migrants with cancer struggle to communicate with their health care team. This study aimed to identify health-care related unmet needs and communication issues for migrants who develop cancer and factors associated with these challenges. In this paper, the findings related to communication issues are presented.
Patients and methods
Seventy-three cancer patients diagnosed within the previous 3 years and 18 carers, who had migrated to Australia and spoke the designated languages, participated in focus groups or structured interviews. Participants were recruited from ethnic community support organisations, support groups and Oncology clinics within three metropolitan hospitals in two states of Australia. Focus groups and semi-structured interviews were conducted in participants’ own language or English as preferred, audio-taped, transcribed and translated into English and analysed using qualitative methods.
Results
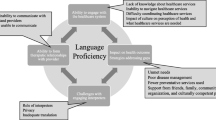
Four themes emerged: (1) cultural isolation, alienation and identification; (2) language and communication difficulties; (3) interpreter issues; and (4) advice for health professionals. Participants, especially those less acculturated, described feeling alone and misunderstood, failing to comprehend medical instructions, being unable to communicate questions and concerns and a lack of consistency in interpreters and interpretation.
Conclusions
Migrants with cancer experience additional challenges to those of native-born patients. Participants provided cogent advice regarding optimal communication with people from their culture. There is clearly a need to develop strategies to increase the cultural competence of care to people from different countries.
Similar content being viewed by others
References
Australian Bureau of Statistics (2006) Australian social trends (4102.0). AGPS, Canberra
Du XL, Meyer TE, Franzini L (2007) Meta-analysis of racial disparities in survival in association with socioeconomic status among men and women with colon cancer. Cancer 109(11):2161–2170
Krupski TL, Sonn G, Kwan L, Maliski S, Fink A, Litwin MS (2005) Ethnic variation in health-related quality of life among low-income men with prostate cancer. Ethn Dis 15(3):461–468
Gotay CC, Holup JL, Pagano I (2002) Ethnic differences in quality of life among early breast and prostate cancer survivors. Psycho-oncol 11(2):103–113
Mayerowitz BE, Richardson J, Hudson S, Leedham B (1998) Ethnicity and cancer outcomes: behavioural and psychosocial considerations. Psycho Bull 123:47–70
Buckle JM, Horn SD, Oates VM, Abbey H (1992) Severity of illness and resource use differences among white and black hospitalized elderly. Arch Intern Med 152:1596–1603
Goldstein D, Thewes B, Butow P (2002) Communicating in a multicultural society II: Greek community attitudes towards cancer in Australia. Internal Medicine Journal. Intern Med J 32:289–296
NBCC Exploring Cultural attitudes to breast cancer; Towards the development of culturally appropriate information resources for women from Greek, Italian, Arabic and Polish speaking backgrounds. ISBN 0-9586732-8-4, 1997
Gonzalez G (1997) Health care in the United States; A perspective from the front line. In: Surbone Z (ed) Communication with the cancer patient; Information and truth. The NY Academy of Sciences, NY, pp 211–222
Janz NK, Mujahid MS, Hawley ST, Griggs JJ, Hamilton AS, Katz SJ (2008) Racial/ethnic differences in adequacy of information and support for women with breast cancer. Cancer 113(5):1058–1067
Chambers T (2000) Cross-cultural issues in caring for patients with cancer. Cancer Treat Res 102:23–37
Lindert J, Ehrenstein OS, Priebe S, Mielck A, Brahler E (2009) Depression and anxiety in labor migrants and refugees—a systematic review and meta-analysis. Soc Sci Med 69(2):246–257
Parker G, Chan B, Tully L, Eisenbruch M (2005) Depression in the Chinese: the impact of acculturation (2005). Psychol Med 35(10):1475–1483
Rissel C (1997) The development and application of a scale of acculturation, Australian and New Zealand. Journal of Public Health 21:606–613
Stenner P (1993) Discoursing jealousy. In: Parker I (ed) E Burman. Routledge, Discourse Analytic Research. London, pp 114–134
Davies B, Harre R (1990) Positioning: the discursive production of selves. Journal of the Theory of Social Behaviour 20:43–65
Schwaderer KA (2007) Itano JK Bridging the healthcare divide with patient navigation: development of a research program to address disparities. Clin J Oncol Nurs 11(5):633–639
Waitzkin H (1985) Information giving in medical care. JHealth SocBehav 26(2):81–101
Johnson RL, Roter D, Powe NR, Cooper LA (2004) Patient race/ethnicity and quality of patient-physician communication during medical visits. Am J Public Health 94(12):2084–2090
Ashing KT, Padilla G, Tejero J, Kagawa-Singer M (2003) Understanding the breast cancer experience of Asian American women. Psycho-oncology 12:38–58
National Breast Cancer Centre & National Cancer Control Initiative (2002) Clinical practice guidelines for the psychosocial care of adults with cancer—draft for consultation. National Breast Cancer Centre & National Cancer Control Initiative, Sydney
Reisfield GM, Wilson GR (2004) Use of metaphor in the discourse on cancer. J Clin Oncol 22(19):4024–4027
Kaufert JM, Koolage WW (1984) Role conflict among ‘culture brokers’: the experience of native Canadian medical interpreters. Soc Sci Med 18:283–286
Flores G (2005) The impact of medical interpreter services on the quality of health care: a systematic review. Med Care Res Rev 62:255–299
Barlow-Stewart K, Yeo SS, Meiser B, Goldstein D, Tucker K, Eisenbruch M (2006) Towards cultural competence in cancer genetic counseling and genetics education: lessons learned from Chinese-Australians. Genet Med 8(1):1–9
Interpreter use and satisfaction with interpersonal aspects of care for Spanish-speaking patients. Med. Care 36(10):1461–1470, 1998
Chu KC, Miller BA, Springfield SA (2007) Measures of racial/ethnic health disparities in cancer mortality rates and the influence of socioeconomic status. J Natl Med Assoc 99(10):1092–1100
Eshiett Michael UA, Parry EHO (2003) Migrants and health: a cultural dilemma. Clin Med 3:229–231
Acknowledgements
This study was funded by a grant from the Australian National Health and Medical Research Council (no. 457432). Some additional financial support was provided by Cancer Australia.
We are grateful to the organisations which assisted with access to and recruitment of community informants and research participants: CanRevive; Healthpac Medical Centre; Multicultural Cancer Information Service, Cancer Council NSW; St. George Hospital; Prince of Wales Hospital; Chinese Cancer Support VIC; Cancer Information Support Service, Cancer Council VIC, Peter MacCallum Cancer Centre. We would also like to thank Dr. Winston Liauw, Dr. Craig Lewis, Seije Gutierrez, Dr. Ven Tan, Eleanor Yip, Norma Leung, Gunjan Tripathi, Dorothy Yui, Anna Epifanio, Doreen Akkerman, Elizabeth Ballinger and Alison Hocking for assistance with identification of potential participants. We are most grateful to our members of community advisory boards who have provided invaluable advice on community engagement, interpretation of qualitative data and study procedures. Respectively they are (1) Greek Advisory Board: Nicole Komninou, Fr. Sophronios Konidaris, Maria Petrohilos, Bill Gonopoulos, Dr. Peter Calligeros, Elfa Moraitakis; (2) Chinese Advisory Board: Wendy Wang, Theresa Chow, Daniel Chan, Viola Yeung, Dr. Agnes Li, Hudson Chen, Dr. Ven Tan, Nancy Tam, Soo See Yeo, Prof. Richard Chye; (3) Arabic Advisory Board: Fr. Antonios Kaldas, Mona Saleh, Seham Gerges, Katya Nicholl.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Butow, P.N., Sze, M., Dugal-Beri, P. et al. From inside the bubble: migrants’ perceptions of communication with the cancer team. Support Care Cancer 19, 281–290 (2011). https://doi.org/10.1007/s00520-010-0817-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-010-0817-x