Abstract
Aims
To describe functional status (FS), general health (GH) and symptom distress (SD) from admission to 1 year post-SCT and to identify medical, demographic, and/or patient-reported outcome variables associated with patient-perceived GH.
Material and methods
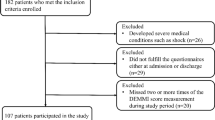
Forty-one patients (27 women) with a median age of 44 (18–65) years answered three questionnaires (SIP, SWED-QUAL, and SFID-SCT) from admission to 1 year post-SCT.
Results
At discharge, 59% of the patients reported poor FS and GH, and 24% reported >10 simultaneous symptoms. After 1 year post-SCT, 22% still reported poor FS, 32% poor GH, and 12% >10 simultaneous symptoms. Compared with admission, significantly larger proportions of the patients reported poor GH at discharge (20 vs 59%, p = .001), poor FS at 6 months (24 vs 59%, p = .004), and poor GH [The number of symptoms was found to be significantly associated with poor GH at discharge (OR 1.330, p = .009) and at 1 year post-SCT (OR 2.000, p = .010)]. Patients reporting “poor GH” at discharge and at 1 year post-SCT reported a median of 7 and 10 symptoms, respectively. Patients with “good GH” reported a median of three symptoms both at T1 and T4. “Tiredness”, “anxiety”, “mouth dryness”, “loss of appetite”, and “diarrhoea” were reported by a larger proportion of the patients reporting “poor GH”.
Conclusions
The results confirm that some patients who have undergone a SCT have a negatively affected life situation. The study indicates that actively asking for symptoms and applying the best treatment for symptom alleviation are among the most important measures that SCT teams can take to help the patients perceive better general health and an improved life situation.

Similar content being viewed by others
References
Andrykowski MA, Bishop MM, Hahn EA, Cella DF, Beaumont JL, Brady MJ, Horowitz MM, Sobocinski KA, Rizzo JD, Wingard JR (2005) Long-term health-related quality of life, growth, and spiritual well-being after hematopoietic stem-cell transplantation. J Clin Oncol 23:599–608
Bailis DS, Segall A, Chipperfield JG (2003) Two views of self-rated general health status. Soc Sci Med 56:203–217
Baker F, Wingard JR, Curbow B, Zabora J, Jodrey D, Fogarty L, Legro M (1994) Quality of life of bone marrow transplant long-term survivors. Bone Marrow Transplant 13:589–596
Baker F, Zabora J, Polland A, Wingard J (1999) Reintegration after bone marrow transplantation. Cancer Pract 7:190–197
Barsevick AM, Dudley W, Beck S, Sweeney C, Whitmer K, Nail L (2004) A randomized clinical trial of energy conservation for patients with cancer-related fatigue. Cancer 100:1302–1310
Bergner M, Bobbitt RA, Carter WB, Gilson BS (1981) The Sickness Impact Profile: development and final revision of a health status measure. Med Care 19:787–805
Broers S, Kaptein AA, Le Cessie S, Fibbe W, Hengeveld MW (2000) Psychological functioning and quality of life following bone marrow transplantation: a 3-year follow-up study. J Psychosom Res 48:11–21
Brorsson B, Ifver J, Hays RD (1993) The Swedish Health-Related Quality of Life Survey (SWED-QUAL). Qual Life Res 2:33–45
Brown CG, Wingard J (2004) Clinical consequences of oral mucositis. Semin Oncol Nurs 20:16–21
Coates A, Porzsolt F, Osoba D (1997) Quality of life in oncology practice: prognostic value of EORTC QLQ-C30 scores in patients with advanced malignancy. Eur J Cancer 33:1025–1030
Coleman EA, Hall-Barrow J, Coon S, Stewart CB (2003) Facilitating exercise adherence for patients with multiple myeloma. Clin J Oncol Nurs 7:529–534, 540
Courneya KS, Friedenreich CM, Sela RA, Quinney HA, Rhodes RE, Handman M (2003) The group psychotherapy and home-based physical exercise (group-hope) trial in cancer survivors: physical fitness and quality of life outcomes. Psychooncology 12:357–374
Courneya KS, Keats MR, Turner AR (2000) Physical exercise and quality of life in cancer patients following high dose chemotherapy and autologous bone marrow transplantation. Psychooncology 9:127–136
Dimeo F, Schmittel A, Fietz T, Schwartz S, Kohler P, Boning D, Thiel E (2004) Physical performance, depression, immune status and fatigue in patients with hematological malignancies after treatment. Ann Oncol 15:1237–1242
Dimeo FC (2001) Effects of exercise on cancer-related fatigue. Cancer 92:1689–1693
Dimeo FC, Thomas F, Raabe-Menssen C, Propper F, Mathias M (2004) Effect of aerobic exercise and relaxation training on fatigue and physical performance of cancer patients after surgery. A randomised controlled trial. Support Care Cancer 12:774–779
Dodd MJ, Miaskowski C, Paul SM (2001) Symptom clusters and their effect on the functional status of patients with cancer. Oncol Nurs Forum 28:465–470
Edman L, Larsen J, Hägglund H, Gardulf A (2001) Health-related quality of life, symptom distress and sense of coherence in adult survivors of allogeneic stem-cell transplantation. Eur J Cancer Care 10:124–130
Eriksson I, Unden AL, Elofsson S (2001) Self-rated health. Comparisons between three different measures. Results from a population study. Int J Epidemiol 30:326–333
Fayers PM, Machin D (2000) Methods for missing forms. In: Quality of life: assessment, analysis and interpretation. Wiley, Chichester, pp 236–245
Fayers PM, Machin D (2000) Missing data. In: Quality of life: assessment, analysis and interpretation. Wiley, Chichester, pp 224–247
Fayers PM, Sprangers MA (2002) Understanding self-rated health. Lancet 359:187–188
Fife B, Huster G, Cornetta K, Kennedy V, Akard L, Broun E (2000) Longitudinal study of adaptation to the stress of bone marrow transplantation. J Clin Oncol 18:1539–1549
Gaston-Johansson F, Fall-Dickson JM, Nanda J, Ohly KV, Stillman S, Krumm S, Kennedy MJ (2000) The effectiveness of the comprehensive coping strategy program on clinical outcomes in breast cancer autologous bone marrow transplantation. Cancer Nurs 23:277–285
Given B, Given CW, McCorkle R, Kozachik S, Cimprich B, Rahbar MH, Wojcik C (2002) Pain and fatigue management: results of a nursing randomized clinical trial. Oncol Nurs Forum 29:949–956
Gratwohl A, Baldomero H, Frauendorfer K, Urbano-Ispizua A (2006) EBMT activity survey 2004 and changes in disease indication over the past 15 years. Bone Marrow Transplant 37:1069–1085
Gratwohl A, Passweg J, Baldomero H, Urbano-Ispizua A (2001) Hematopoietic stem cell transplantation activity in Europe 1999. Bone Marrow Transplant 27:899–916
Hayes S, Davies PS, Parker T, Bashford J, Newman B (2004) Quality of life changes following peripheral blood stem cell transplantation and participation in a mixed-type, moderate-intensity, exercise program. Bone Marrow Transplant 33:553–558
Hosmer D, Lemesshow S (1989) Applied logistic regression. Wiley, New York
Jacobsen PB, Meade CD, Stein KD, Chirikos TN, Small BJ, Ruckdeschel JC (2002) Efficacy and costs of two forms of stress management training for cancer patients undergoing chemotherapy. J Clin Oncol 20:2851–2862
Jenkins PL, Linington A, Whittaker JA (1991) A retrospective study of psychosocial morbidity in bone marrow transplant recipients. Psychosomatics 32:65–71
Kim SD, Kim HS (2005) Effects of a relaxation breathing exercise on fatigue in haemopoietic stem cell transplantation patients. J Clin Nurs 14:51–55
Krishnasamy M (1995) Oral problems in advanced cancer. Eur J Cancer Care 4:173–177
Larsen J, Gardulf A, Nordström G, Björkstrand B, Ljungman P (1996) Health-related quality of life in women with breast cancer undergoing autologous stem-cell transplantation. Cancer Nurs 19:368–375
Larsen J, Nordström G, Björkstrand B, Ljungman P, Gardulf A (2003) Symptom distress, functional status and health-related quality of life prior to high-dose chemotherapy with stem-cell transplantation. Eur J Cancer Care 12:71–80
Larsen J, Nordström G, Ljungman P, Gardulf A (2004) Symptom occurrence, symptom intensity, and symptom distress in patients undergoing high-dose chemotherapy with stem-cell transplantation. Cancer Nurs 27:55–64
Lee SJ, Fairclough D, Parsons SK, Soiffer RJ, Fisher DC, Schlossman RL, Antin JH, Weeks JC (2001) Recovery after stem-cell transplantation for hematologic diseases. J Clin Oncol 19:242–252
Mock V, Barsevick A, Escalante C, Hinds P, O’Connor T, Piper BF, Rugo HS (2006) Cancer-related fatigue. In: Clinical practice guidelines in oncology. The National Comprehensive Cancer Network
Oldervoll LM, Kaasa S, Knobel H, Loge JH (2003) Exercise reduces fatigue in chronic fatigued Hodgkins disease survivors-results from a pilot study. Eur J Cancer 39:57–63
Osoba D (1999) What has been learned from measuring health-related quality of life in clinical oncology. Eur J Cancer 35:1565–1570
Pett MA (1997) Cochran’s Q tests. In: Nonparametric statistics for health care research: statistics for small samples and unusual distributions. Sage Publications, Thousand Oaks, pp 123–131
Saleh US, Brockopp DY (2001) Quality of life one year following bone marrow transplantation: psychometric evaluation of the quality of life in bone marrow transplant survivors tool. Oncol Nurs Forum 28:1457–1464
Siegel S, Castellan NJ (1988) Friedman two-way analysis of variance by ranks. In: Nonparametric statistics for the behavioral sciences. McGraw–Hill, New York, pp 175–183
Sullivan M (1988) The Sickness Impact Profile (SIP): an instrument for overall health assessment; a basic evaluation. J Drug Ther Res 13:167–169
Syrjala KL, Langer SL, Abrams JR, Storer BE, Martin PJ (2005) Late effects of hematopoietic cell transplantation among 10-year adult survivors compared with case-matched controls. J Clin Oncol 23:6596–6606
van Weert E, Hoekstra-Weebers J, Otter R, Postema K, Sanderman R, van der Schans C (2006) Cancer-related fatigue: predictors and effects of rehabilitation. Oncologist 11:184–196
Wilson RW, Jacobsen PB, Fields KK (2005) Pilot study of a home-based aerobic exercise program for sedentary cancer survivors treated with hematopoietic stem cell transplantation. Bone Marrow Transplant 35:721–727
Acknowledgements
We wish to express our gratitude to the staff at the Department of Hematology and the Center for Allogeneic Stem-Cell Transplantation at the Karolinska University Hospital at Huddinge, Stockholm, for help with including patients in the study. We are also grateful to Hilary Hocking for language revision and Katarina Wiberg Hedman for support with the statistical analyses. This study was supported by grants from the Gunnar, Arvid, and Elisabeth Nilsson Fund for Combating Cancer, the Swedish Foundation for Health Care Sciences and Allergy Research, the Tobias Foundation, the Research Committee for Caring Sciences at Karolinska Institutet, the Nursing Development and Research Committee at Huddinge University Hospital, and the Committee for Research and Education at Karolinska University Hospital (Stockholm, Sweden).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Larsen, J., Nordström, G., Ljungman, P. et al. Factors associated with poor general health after stem-cell transplantation. Support Care Cancer 15, 849–857 (2007). https://doi.org/10.1007/s00520-006-0200-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-006-0200-0