Summary
Background
The blood concentrations of total cholesterol and low-density lipoprotein (LDL) do not predict survival in patients older than 60 years. The atherogenic index of plasma (AIP) is a logarithm of the triacylglycerol to high-density lipoprotein (HDL) ratio and a surrogate for the concentration of small dense LDL. It might be a better reflection of the risk of all-cause death in elderly patients.
Methods
We conducted a prospective observational study of patients with arterial hypertension older than 60 years. The concentrations of total cholesterol, LDL, HDL and triacylglycerol were measured at the time of the recruitment and the patients were observed for 10 years. Cox regression analysis was performed to assess the effects of lipoproteins and AIP on survival.
Results
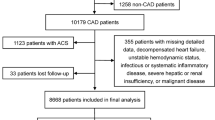
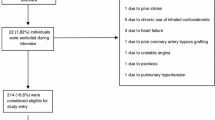
A total of 500 patients were recruited and 473 of them (226 men, 247 women) either died or successfully completed the 10-year follow-up and were included in the analysis. The AIP was positively associated, while HDL concentration was negatively associated with the risk of all-cause death adjusted for age, smoking habits, statin use, history of diabetes mellitus, myocardial infarction, stroke and peripheral artery occlusive disease (PAOD) in elderly women but not in men. The LDL, total cholesterol, triacylglycerol and non-HDL concentrations were not associated with the risk of death in both sexes.
Conclusions
The AIP is positively associated with the risk of all-cause death in elderly women with arterial hypertension independent of age, smoking habits, statin therapy and comorbidities.
Similar content being viewed by others
Abbreviations
- AIP:
-
Atherogenic index of plasma
- BMI:
-
Body mass index
- CAD:
-
Coronary artery disease
- CVD:
-
Cardiovascular disease
- HDL:
-
High-density lipoprotein
- LDL:
-
Low-density lipoprotein
- TAG:
-
Triacylglycerol
- VLDL:
-
Very low-density lipoprotein
References
Nichols M, Townsend N, Scarborough P, Rayner M. Cardiovascular disease in Europe 2014: Epidemiological update. Eur Heart J. 2014;35:2950–9.
Lloyd-Jones D, Adams R, Carnethon M, American Heart Association, Stroke Statistics Subcommittee, et al. Heart disease and stroke statistics – 2009 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2009;119:e21–e181.
Kannel WB, Dawber TR, Kagana A, Revotskie N, Stokes J 3rd. Factors of risk in the development of coronary heart disease-six year follow-up experience. The Framingham Study. Ann Intern Med. 1961;55:33–50.
Wilson PW, D’Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. Prediction of coronary heart disease using risk factor categories. Circulation. 1998;97:1837–47.
Rosenson RS. Low high-density lipoprotein cholesterol and cardiovascular disease: Risk reduction with statin therapy. Am Heart J. 2006;151:556–63.
Pedro-Botet J, Climent E, Chillarón JJ, Toro R, Benaiges D, Flores-Le Roux JA. Statins for primary cardiovascular prevention in the elderly. J Geriatr Cardiol. 2015;12:431–8.
Tikhonoff V, Casiglia E, Mazza A, Scarpa R, Thijs L, Pessina AC, Staessen JA. Low-density lipoprotein cholesterol and mortality in older people. J Am Geriatr Soc. 2005;53:2159–64.
Cabrera MA, de Andrade SM, Dip RM. Lipids and all-cause mortality among older adults: A 12-year follow-up study. ScientificWorldJournal. 2012;2012:930139.
Ravnskov U, Diamond DM, Hama R, Hamazaki T, Hammarskjöld B, Hynes N, Kendrick M, Langsjoen PH, Malhotra A, Mascitelli L, McCully KS, Ogushi Y, Okuyama H, Rosch PJ, Schersten T, Sultan S, Sundberg R. Lack of an association or an inverse association between low-density-lipoprotein cholesterol and mortality in the elderly: A systematic review. BMJ Open. 2016;6:e10401.
Lu W, Resnick HE, Jablonski KA, Jones KL, Jain AK, Howard WJ, Robbins DC, Howard BV. Non-HDL cholesterol as a predictor of cardiovascular disease in type 2 diabetes: The strong heart study. Diabetes Care. 2003;26:16–23.
van Deventer HE, Miller WG, Myers GL, Sakurabayashi I, Bachmann LM, Caudill SP, Dziekonski A, Edwards S, Kimberly MM, Korzun WJ, Leary ET, Nakajima K, Nakamura M, Shamburek RD, Vetrovec GW, Warnick GR, Remaley AT. Non-HDL cholesterol shows improved accuracy for cardiovascular risk score classification compared to direct or calculated LDL cholesterol in a dyslipidemic population. Clin Chem. 2011;57:490–501.
Dobiásová M, Frohlich J. The plasma parameter log (TG/HDL-C) as an atherogenic index: correlation with lipoprotein particle size and esterification rate in apoB-lipoprotein-depleted plasma (FER(HDL)). Clin Biochem. 2001;34:583–8.
Lamarche B, Tchernof A, Moorjani S, Cantin B, Dagenais GR, Lupien PJ, Després JP. Small, dense low-density lipoprotein particles as a predictor of the risk of ischemic heart disease in men. Prospective results from the Quebec cardiovascular study. Circulation. 1997;5:69–75.
Toft-Petersen AP, Tilsted HH, Aarøe J, Rasmussen K, Christensen T, Griffin BA, Aardestrup IV, Andreasen A, Schmidt EB. Small dense LDL particles – a predictor of coronary artery disease evaluated by invasive and CT-based techniques: A case-control study. Lipids Health Dis. 2011;10:21.
Grammer TB, Kleber ME, März W, Silbernagel G, Siekmeier R, Wieland H, Pilz S, Tomaschitz A, Koenig W, Scharnagl H. Low-density lipoprotein particle diameter and mortality: The Ludwigshafen risk and cardiovascular health study. Eur Heart J. 2015;36:31–8.
El Harchaoui K, van der Steeg WA, Stroes ES, Kuivenhoven JA, Otvos JD, Wareham NJ, Hutten BA, Kastelein JJ, Khaw KT, Boekholdt SM. Value of low-density lipoprotein particle number and size as predictors of coronary artery disease in apparently healthymenandwomen: the EPIC-Norfolk prospective population study. J Am Coll Cardiol. 2007;49:547–53.
Dobiásová M, Frohlich J, Sedová M, Cheung MC, Brown BG. Cholesterol esterification and atherogenic index of plasma correlate with lipoprotein size and findings on coronary angiography. J Lipid Res. 2011;52:566–71.
Onat A, Can G, Kaya H, Hergenç G. Atherogenic index of plasma (log10 triglyceride/high-density lipoprotein-cholesterol) predicts high blood pressure, diabetes, and vascular events. J Clin Lipidol. 2010;4:89–98.
Zhu XW, Deng FY, Lei SF. Meta-analysis of atherogenic index of plasma and other lipid parameters in relation to risk of type 2 diabetes mellitus. Prim Care Diabetes. 2015;9:60–7.
Ohmura H, Mokuno H, Sawano M, Hatsumi C, Mitsugi Y, Watanabe Y, Daida H, Yamaguchi H. Lipid compositional differences of small, dense low-density lipoprotein particle influence its oxidative susceptibility: possible implication of increased risk of coronary artery disease in subjects with phenotype B. Metabolism. 2002;51:1081–7.
Lupattelli G, Lombardini R, Schillaci G, Ciuffetti G, Marchesi S, Siepi D, Mannarino E. Flow-mediated vasoactivity and circulating adhesion molecules in hypertriglyceridemia: Association with small, dense LDL cholesterol particles. Am Heart J. 2000;140:521–6.
Walldius G, Jungner I, Holme I, Aastveit AH, Kolar W, Steiner E. High apolipoprotein B, low apolipoprotein A‑I, and improvement in the prediction of fatal myocardial infarction (AMORIS study): A prospective study. Lancet. 2001;358:2026–33.
Watanabe T, Koba S, Kawamura M, Itokawa M, Idei T, Nakagawa Y, Iguchi T, Katagiri T. Small dense low-density lipoprotein and carotid atherosclerosis in relation to vascular dementia. Metabolism. 2004;53:476–82.
Goliasch G, Oravec S, Blessberger H, Dostal E, Hoke M, Wojta J, Schillinger M, Huber K, Maurer G, Wiesbauer F. Relative importance of different lipid risk factors for the development of myocardial infarction at a very young age (≤40 years of age). Eur J Clin Invest. 2012;42:631–6.
Bathum L, Depont Christensen R, Engers Pedersen L, Lyngsie Pedersen P, Larsen J, Nexøe J. Association of lipoprotein levels with mortality in subjects aged 50 + without previous diabetes or cardiovascular disease: A population-based register study. Scand J Prim Health Care. 2013;31:172–80.
Tosheska K, Labudovic D, Jovanova S, Jaglikovski B, Alabakovska S. Cholesteryl ester transfer protein, low density lipoprotein particle size and intima media thickness in patients with coronary heart disease. Bosn J Basic Med Sci. 2011;11:169–73.
Félix-Redondo FJ, Grau M, Fernández-Bergés D. Cholesterol and cardiovascular disease in the elderly. Facts and gaps. Aging Dis. 2013;4:154–69.
Weverling-Rijnsburger AW, Jonkers IJ, van Exel E, Gussekloo J, Westendorp RG. High-density vs low-density lipoprotein cholesterol as the risk factor for coronary artery disease and stroke in old age. Arch Intern Med. 2003;163:1549–54.
Curb JD, Abbott RD, Rodriguez BL, Masaki KH, Chen R, Popper JS, Petrovitch H, Ross GW, Schatz IJ, Belleau GC, Yano K. High density lipoprotein cholesterol and the risk of stroke in elderly men: The Honolulu heart program. Am J Epidemiol. 2004;160:150–7.
Zuliani G, Cavalieri M, Galvani M, Volpato S, Cherubini A, Bandinelli S, Corsi AM, Lauretani F, Guralnik JM, Fellin R, Ferrucci L. Relationship between low levels of high-density lipoprotein cholesterol and dementia in the elderly. The InChianti study. J Gerontol A Biol Sci Med Sci. 2010;65:559–64.
Ferrara A, Barrett-Connor E, Shan J. Total, LDL, and HDL cholesterol decrease with age in older men and women. The Rancho Bernardo Study 1984–1994. Circulation. 1997;96:37–43.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Bendzala, P. Sabaka, M. Caprnda, A. Komornikova, M. Bisahova, R. Baneszova, D. Petrovic, R. Prosecky, L. Rodrigo, P. Kruzliak, and A. Dukat declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Additional information
Matej Bendzala and Peter Sabaka contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Bendzala, M., Sabaka, P., Caprnda, M. et al. Atherogenic index of plasma is positively associated with the risk of all-cause death in elderly women. Wien Klin Wochenschr 129, 793–798 (2017). https://doi.org/10.1007/s00508-017-1264-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-017-1264-1