Summary
Background
The aim of the study was to evaluate patients attitudes with benign prostatic hyperplasia at the risk of progression during a 12-month period of observation.
Materials and methods
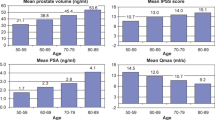
A total of 426 patients from 45 outpatients centers were included and prospectively followed. Inclusion criteria were: age > 50 years, International Prostate Symptom Score (IPSS) > 8, prostate volume > 30 cm3 (transabdominal ultrasound) and PSA > 1.5 to < 10 ng/ml.
Results
In all, 28.6 % patients were naive, 62.9 % used monotherapy (alpha-blocker), and 8.5 % combined treatment (alpha-blocker/5alpha-reductase inhibitor/dutasteride). The most bothersome symptoms were the weak urine stream (60.8 %) and nocturia (59.2 %). Patients expectations from the treatment were stabilization of the disease and reducing the risk of surgery rather than rapid resolution of symptoms. Despite the presence of symptoms, 2.3 % patients claimed that benign prostatic hyperplasia/lower urinary tract symptoms had no impact on their quality of life (QoL), in 48.1 % only little impact on QoL, and 47.9 % patients percepted their symptoms as severe. Out of 71.4 % patients treated previously, 26.5 % patients were indecisive about the satisfaction of present treatment. Visual analog score was percepted more optimistically rather than the IPSS. Pearsonʼs correlation r = 0.68 at the beginning and r = 0.83 at the end of the study.
Conclusions
Prostate and Expectations of Treatment Epidemiology Research study highlights and reflects on patients behavior and self-perception, patients self-perception of the disease and therapeutic priorities during the 1 year of observation.
Zusammenfassung
Hintergrund
Das Ziel dieser 1-Jahres-Studie war die Evaluation der Patientenwahrnehmung von Miktionsbeschwerden (LUTS) infolge benigner Prostatahyperplasie und die Erwartungen an die medikamentöse Therapie.
Material und Methoden
Es wurden prospektiv 426 Patienten aus 45 ambulanten Zentren in diese Studie eingeschlossen. Die Einschlusskriterien waren: Alter > 50 Jahre, IPSS > 8, Prostatavolumen > 30 cm3 und ein PSA-Wert zwischen 1,5 und 10 ng/ml.
Ergebnisse
Von den 426 Patienten waren 28,6 % behandlungsnaiv, 62,9 % verwendeten eine Monotherapie mit einem Alpha-Blocker und 8,5 % eine Kombinationstherapie mit einem Alpha-Blocker und einem 5-Alpha-Reduktase-Hemmer (Dutasterid). Die vom Patienten als unangenehmsten empfundenen LUTS waren der schwache Harnstrahl (60,8 %) und die Nykturie (59,2 %). Die Patienten erwarteten von der medikamentösen Therapie eher eine Stabilisierung der LUTS und eine Verringerung des Risikos einer Operation als eine schnelle Linderung der LUTS. Bei 47,4 % der Patienten führten LUTS zu einer hochgradigen Verschlechterung der Lebensqualität.
Schlussfolgerungen
Die vorliegende 1-Jahres-Studie reflektiert die Wahrnehmung von LUTS und die Erwartungen des Patienten an die Therapie.



Similar content being viewed by others
References
Emberton M, Marberger M, de la Rosette J. Understanding patient and physician perceptions of benign prostatic hyperplasia in Europe: The Prostate Research on Behavior and Education (PROBE) survey. Int J Clin Pract. 2007;62(1):18–26.
Teillac P. Benign prostatic hyperplasia: patient's perception of medical treatment and their expectations: results of French survey involving patients treated with finasteride. Therapie. 2002;57:473–83.
Watson V, Ryan M, Brown CT, Barnett G, Ellis BW, Emberton M. Eliciting preferences for drug treatment of lower urinary tract symptoms associated with benign prostatic hyperplasia. J Urol. 2004;172:2321–5.
Ushijima S, Ukimura O, Okihara K, Mizutani Y, Kawauchi A, Miki T. Visual analog scale questionnaire to asses quality of life specific symptom of the International Prostate Symptom Score. J Urol. 2006;176:665–71.
Kawakami J, Nickel JC. Acute urinary retention and surgery for benign prostatic hyperplasia: patient's perspective. Can J Urol. 1999;6:819–22.
Agarwal A, Eryuzlu LN, Cartwright R, Thorlund K, Tammela TL, Guyatt GH, Auvinen A, Tikkinen KA. What is the most bothersome lower urinary tract symptom? Individual- and population-level perspectives for both men and women. Eur Urol. 2014;65(6):1211–7.
Vaughan CP, Auvinen A, Cartwright R. Impact of obesity on urinary storage symptoms: results from the FINNO study. J Urol. 2013;189:1377–82.
Irwin DE, Abrams P, Milsom I, Kopp Z, Reilly K. EPIC Study Group understanding the elements of overactive bladder: questions raised by the EPIC study. BJU Int. 2008;101:1381–7.
Mozad MA. Lifestyle changes to prevent BPH: heart healthy = prostate healthy. Urol Nurs. 2003;23:439–41.
Kupelian V, Wei JT, O'Leary MP, Kusek JW, Litman HJ, Link CL, McKinlay JB, BACH Survery Investigators. Prevalence of lower urinary tract symptoms and effect on quality of life in a racially and ethnically diverse random sample: the Boston Area Community Health (BACH) Survey. Arch Intern Med. 2006;166(21):2381–7.
Kupelian V, Rosen RC, Link CL, McVary KT, Aiyer LP, Mollon P, Kaplan SA, McKinlay JB. Association of urological symptoms and chronic illness in men and women: contributions of symptom severity and duration—results from the BACH Survey. J Urol. 2009;181(2):694–700.
Li MK, Garcia L, Patron N, Moh LC, Sundram M, Leungwattanakij S, Pripatnanont C, Cheng C, Chi-Wai M, Loi-Cheong N. An Asian multinational prospective observational registry of patients with benign prostatic hyperplasia, with a focus on comorbidities, lower urinary tract symptoms and sexual function. BJU Int. 2008;101(2):197–202.
Mondul AM, Giovannucci E, Platz EA. A prospective study of obesity, and the incidence and progression of lower urinary tract symptoms. J Urol. 2014;191(3):715–21.
Sarma AV, Burke JP, Jacobson DJ, McGree ME, St Sauver J, Girman CJ, Lieber MM, Herman W, Macoska J, Montie JE, Jacobsen SJ. Associations between diabetes and clinical markers of benign prostatic hyperplasia among community-dwelling Black and White men. Diabetes Care. 2008;31(3):476–82.
Sarma AV, St Sauver JL, Hollingsworth JM, Jacobson DJ, McGree ME, Dunn RL, Lieber MM, Jacobsen SJ, Urologic Diseases in America Project. Diabetes treatment and progression of benign prostatic hyperplasia in community-dwelling black and white men. Urology. 2012;79(1):102–8.
Pöyhönen A, Häkkinen JT, Koskimäki J, Tammela TL, Auvinen A. Natural course of lower urinary tract symptoms in men not requiring treatment—a 5-year longitudinal population-based study. Urology. 2014;83(2):411–5.
Maserejian NN, Chen S, Chiu GR, Araujo AB, Kupelian V, Hall SA, McKinlay JB. Treatment status and progression or regression of lower urinary tract symptoms in a general adult population sample. J Urol. 2014;191(1):107–13.
Acknowledgments
The study was funded by an unconditional research grant from GlaxoSmithKline Inc., Slovakia, which played a role in conducting the study as well as the data collection.
Conflicts of interest
Danica Fackovcova, MD, is a scientific consultant to GlaxoSmithKline-Slovakia. All other authors have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Weibl, P., Klatte, T., Laurinc, P. et al. Patient’s behavior and attitudes toward the management of benign prostatic hyperplasia among patients with the risk of disease progression: prospective study by “Prostate and Expectations of Treatment Epidemiology Research (PETER) study group”. Wien Klin Wochenschr 127, 363–368 (2015). https://doi.org/10.1007/s00508-014-0668-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00508-014-0668-4