Abstract
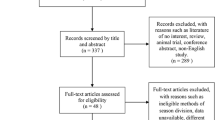
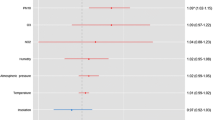
The association between cerebrovascular accidents (CVA) and weather has been described across several studies showing multiple conflicting results. In this paper, we aim to conduct a meta-analysis to further clarify this association, as well as to find the potential sources of heterogeneity. PubMed, EMBASE, and Google Scholar were searched from inception through 2015, for articles analyzing the correlation between the incidence of CVA and temperature. A pooled effect size (ES) was estimated using random effects model and expressed as absolute values. Subgroup analyses by type of CVA were also performed. Heterogeneity and influence of covariates—including geographic latitude of the study site, male percentage, average temperature, and time interval—were assessed by meta-regression analysis. Twenty-six articles underwent full data extraction and scoring. A total of 19,736 subjects with CVA from 12 different countries were included and grouped as ischemic strokes (IS; n = 14,199), intracerebral hemorrhages (ICH; n = 3798), and subarachnoid hemorrhages (SAH; n = 1739). Lower ambient temperature was significantly associated with increase in incidence of overall CVA when using unadjusted (pooled ES = 0.23, P < 0.001) and adjusted data (pooled ES = 0.03, P = 0.003). Subgroup analyses showed that lower temperature has higher impact on the incidence of ICH (pooled ES = 0.34, P < 0.001), than that of IS (pooled ES = 0.22, P < 0.001) and SAH (pooled ES = 0.11, P = 0.012). In meta-regression analysis, the geographic latitude of the study site was the most influencing factor on this association (Z-score = 8.68). Synthesis of the existing data provides evidence supporting that a lower ambient temperature increases the incidence of CVA. Further population-based studies conducted at negative latitudes are needed to clarify the influence of this factor.



Similar content being viewed by others
References
Aho K, Harmsen P, Hatano S, Marquardsen J, Smirnov V, Strasser T (1980) Cerebrovascular disease in the community: results of a who collaborative study. Bull World Health Organ 58:113
Alexander P (2013) Association of monthly frequencies of diverse diseases in the calls to the public emergency service of the city of Buenos Aires during 1999-2004 with meteorological variables and seasons. Int J Biometeorol 57:83–90
Alperovitch A, Lacombe JM, Hanon O, Dartigues JF, Ritchie K, Ducimetiere P et al (2009) Relationship between blood pressure and outdoor temperature in a large sample of elderly individuals: the three-city study. Arch Intern Med 169:75–80
Azevedo E, Ribeiro JA, Lopes F, Martins R, Barros H (1995) Cold: a risk factor for stroke? J Neurol 242:217–221
Barer D, Ebrahim S, Smith C (1984) Factors affecting day to day incidence of stroke in Nottingham. Br Med J (Clin Res Ed) 289:662
Beguiristain JM, Mar J, Arrazola A (2005) The cost of cerebrovascular accident. Rev Neurol 40:406–411
Borenstein M, Hedges LV, Higgins JPT, Rothstein HR (2009) Introduction to meta-analysis. John Wiley & Sons, New York
Bull GM (1973) Meteorological correlates with myocardial and cerebral infarction and respiratory disease. Br J Prev Soc Med 27:108–113
Capon A, Demeurisse G, Zheng L (1992) Seasonal variation of cerebral hemorrhage in 236 consecutive cases in Brussels. Stroke; a Journal of Cerebral Circulation 23:24–27
Cevik Y, Dogan NO, Das M, Ahmedali A, Kul S, Bayram H (2015) The association between weather conditions and stroke admissions in Turkey. Int J Biometeorol 59:899–905
Chang CL, Shipley M, Marmot M, Poulter N (2004) Lower ambient temperature was associated with an increased risk of hospitalization for stroke and acute myocardial infarction in young women. J Clin Epidemiol 57:749–757
Chen ZY, Chang SF, Su CL (1995) Weather and stroke in a subtropical area: Ilan, Taiwan. Stroke; a Journal of Cerebral Circulation 26:569–572
Cohen J (1992) A power primer. Psychol Bull 112:155–159
de Steenhuijsen Piters WA, Algra A, van den Broek MF, Dorhout Mees SM, Rinkel GJ (2013) Seasonal and meteorological determinants of aneurysmal subarachnoid hemorrhage: a systematic review and meta-analysis. J Neurol 260:614–619
Ettehad D, Emdin CA, Kiran A, Anderson SG, Callender T, Emberson J, et al (2015) Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. Lancet (London, England)
Feigin VL, Nikitin YP, Bots ML, Vinogradova TE, Grobbee DE (2000) A population-based study of the associations of stroke occurrence with weather parameters in Siberia, Russia (1982-92). Eur J Neurol 7:171–178
Gomes J, Damasceno A, Carrilho C, Lobo V, Lopes H, Madede T et al (2015) Triggering of stroke by ambient temperature variation: a case-crossover study in Maputo, Mozambique. Clin Neurol Neurosurg 129:72–77
Grant RL (2014) Converting an odds ratio to a range of plausible relative risks for better communication of research findings. BMJ (Clinical Research Ed) 348:f7450
Gunes H, Kandis H, Saritas A, Dikici S, Buyukkaya R (2015) The relationship between ischemic stroke and weather conditions in Duzce, Turkey. World Journal of Emergency Medicine 6:207–211
Han MH, Yi HJ, Kim YS, Kim YS (2015) Effect of seasonal and monthly variation in weather and air pollution factors on stroke incidence in Seoul, Korea. Stroke; a Journal of Cerebral Circulation 46:927–935
Hong YC, Rha JH, Lee JT, Ha EH, Kwon HJ, Kim H (2003) Ischemic stroke associated with decrease in temperature. Epidemiology (Cambridge, Mass) 14:473–478
Hori A, Hashizume M, Tsuda Y, Tsukahara T, Nomiyama T (2012) Effects of weather variability and air pollutants on emergency admissions for cardiovascular and cerebrovascular diseases. Int J Environ Health Res 22:416–430
Jeong TS, Park CW, Yoo CJ, Kim EY, Kim YB, Kim WK (2013) Association between the daily temperature range and occurrence of spontaneous intracerebral hemorrhage. Journal of Cerebrovascular and Endovascular Neurosurgery 15:152–157
Jimenez-Conde J, Ois A, Gomis M, Rodriguez-Campello A, Cuadrado-Godia E, Subirana I et al (2008) Weather as a trigger of stroke. Daily meteorological factors and incidence of stroke subtypes. Cerebrovascular Diseases (Basel, Switzerland) 26:348–354
Judd SE, Tangpricha V (2009) Vitamin d deficiency and risk for cardiovascular disease. The American Journal of the Medical Sciences 338:40–44
Keatinge WR, Coleshaw SR, Cotter F, Mattock M, Murphy M, Chelliah R (1984) Increases in platelet and red cell counts, blood viscosity, and arterial pressure during mild surface cooling: factors in mortality from coronary and cerebral thrombosis in winter. Br Med J (Clin Res Ed) 289:1405–1408
Lejeune JP, Vinchon M, Amouyel P, Escartin T, Escartin D, Christiaens JL (1994) Association of occurrence of aneurysmal bleeding with meteorologic variations in the north of France. Stroke; a Journal of Cerebral Circulation 25:338–341
Lian H, Ruan Y, Liang R, Liu X, Fan Z (2015) Short-term effect of ambient temperature and the risk of stroke: a systematic review and meta-analysis. Int J Environ Res Public Health 12:9068–9088
Low RB, Bielory L, Qureshi AI, Dunn V, Stuhlmiller DF, Dickey DA (2006) The relation of stroke admissions to recent weather, airborne allergens, air pollution, seasons, upper respiratory infections, and asthma incidence, September 11, 2001, and day of the week. Stroke; a Journal of Cerebral Circulation 37:951–957
Magalhaes R, Silva MC, Correia M, Bailey T (2011) Are stroke occurrence and outcome related to weather parameters? Results from a population-based study in northern Portugal. Cerebrovascular Diseases (Basel, Switzerland) 32:542–551
Marniemi J, Alanen E, Impivaara O, Seppanen R, Hakala P, Rajala T et al (2005) Dietary and serum vitamins and minerals as predictors of myocardial infarction and stroke in elderly subjects. Nutrition, Metabolism, and Cardiovascular Diseases: NMCD 15:188–197
Matsumoto M, Ishikawa S, Kajii E (2010) Cumulative effects of weather on stroke incidence: a multi-community cohort study in Japan. Journal of Epidemiology/Japan Epidemiological Association 20:136–142
Meng G, Tan Y, Fang M, Yang H, Liu X, Zhao Y (2015) Meteorological factors related to emergency admission of elderly stroke patients in Shanghai: analysis with a multilayer perceptron neural network. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research 21:3600–3607
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
Mostofsky E, Wilker EH, Schwartz J, Zanobetti A, Gold DR, Wellenius GA et al (2014) Short-term changes in ambient temperature and risk of ischemic stroke. Cerebrovascular Diseases Extra 4:9–18
Ohshige K, Hori Y, Tochikubo O, Sugiyama M (2006) Influence of weather on emergency transport events coded as stroke: population-based study in Japan. Int J Biometeorol 50:305–311
Ohwaki K, Yano E, Murakami H, Nagashima H, Nakagomi T (2004) Meteorological factors and the onset of hypertensive intracerebral hemorrhage. Int J Biometeorol 49:86–90
Perkovic V, Hewitson TD, Kelynack KJ, Martic M, Tait MG, Becker GJ (2003) Parathyroid hormone has a prosclerotic effect on vascular smooth muscle cells. Kidney & Blood Pressure Research 26:27–33
Rakers F, Schiffner R, Rupprecht S, Brandstadt A, Witte OW, Walther M, et al (2015) Rapid weather changes are associated with increased ischemic stroke risk: a case-crossover study. European Journal of Epidemiology
Rivera-Lara L, Kowalski RG, Schneider EB, Tamargo RJ, Nyquist P (2015) Elevated relative risk of aneurysmal subarachnoid hemorrhage with colder weather in the mid-Atlantic region. Journal of Clinical Neuroscience: Official Journal of the Neurosurgical Society of Australasia 22:1582–1587
Rothwell PM, Wroe SJ, Slattery J, Warlow CP (1996) Is stroke incidence related to season or temperature? The Oxfordshire community stroke project. Lancet (London, England) 347:934–936
Shaposhnikov D, Revich B, Gurfinkel Y, Naumova E (2014) The influence of meteorological and geomagnetic factors on acute myocardial infarction and brain stroke in Moscow, Russia. Int J Biometeorol 58:799–808
Shinkawa A, Ueda K, Hasuo Y, Kiyohara Y, Fujishima M (1990) Seasonal variation in stroke incidence in Hisayama, Japan. Stroke; a Journal of Cerebral Circulation 21:1262–1267
Shiue I, Matzarakis A (2011) When stroke epidemiology meets weather and climate: a heat exposure index from human biometeorology. International Journal of Stroke: Official Journal of the International Stroke Society 6:176
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Sobel E, Zhang ZX, Alter M, Lai SM, Davanipour Z, Friday G et al (1987) Stroke in the Lehigh valley: seasonal variation in incidence rates. Stroke; a Journal of Cerebral Circulation 18:38–42
Tzourio C (2002) Epidemiologic and risk factors in cerebrovascular accidents. Therapie 57:569–576
Voils CI, Crandell JL, Chang Y, Leeman J, Sandelowski M (2011) Combining adjusted and unadjusted findings in mixed research synthesis. J Eval Clin Pract 17:429–434
Woodhouse PR, Khaw KT, Plummer M, Foley A, Meade TW (1994) Seasonal variations of plasma fibrinogen and factor vii activity in the elderly: winter infections and death from cardiovascular disease. Lancet (London, England) 343:435–439
Yeh CJ, Chan P, Pan WH (1996) Values of blood coagulating factors vary with ambient temperature: the cardiovascular disease risk factor two-township study in Taiwan. The Chinese Journal of Physiology 39:111–116
Zheng D, Arima H, Heeley E, Karpin A, Yang J, Chalmers J et al (2015) Ambient temperature and volume of perihematomal edema in acute intracerebral haemorrhage: the interact1 study. International Journal of Stroke: Official Journal of the International Stroke Society 10:25–27
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Zorrilla-Vaca, A., Healy, R.J. & Silva-Medina, M.M. Revealing the association between cerebrovascular accidents and ambient temperature: a meta-analysis. Int J Biometeorol 61, 821–832 (2017). https://doi.org/10.1007/s00484-016-1260-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00484-016-1260-6