Abstract
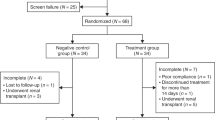
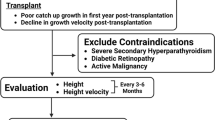
Recombinant human growth hormone (rhGH) is a new treatment modality for short children with chronic renal failure (CRF) prior to and during dialysis. It is difficult to analyze whether dialysis patients respond less to rhGH than children with CRF on conservative treatment because they are older and often in a pubertal age range. One hundred and eight patients were treated with 28–30 IU rhGH/kg per week for at least 1 year. We analyzed the growth response to rhGH in 56 prepubertal patients aged less than 10 years at the start of rhGH treatment; 38 children with a mean age of 6.5±2.4 years were on conservative treatment (CT) and 18 patients with a mean age of 6.5±2 years on dialysis treatment (D). Mean height velocity was 4.9±2.3 cm/year in children on CT and 4.6±1.8 cm/year in children on D. During the 1 st treatment year, height velocity was 9.5±3.8 cm/year in CT patients and 7.3±1.3 cm/year in D patients (P<0.05). The change in height was +1.1±0.8 standard deviation (SD) in CT patients and +0.5±0.4 SD in D patients (P<0.005). During the 2nd treatment year, the change in height was again greater in CT patients (0.5±0.4 SD vs. 0.2±0.4 SD;P<0.05). The difference in height velocity and change in height standard deviation score was also significant when a subgroup of patients was matched for sex, age, height. Height velocity and the change in height velocity during rhGH treatment were not correlated with residual renal function, the degree of anemia, or metabolic acidosis. We conclude that short children on D respond less to rhGH than short children on CT, indicating a greater insensitivity to rhGH during D treatment.
Similar content being viewed by others
References
Mehls O, Haffner D (1995) Treatment of growth retardation in uraemic children. Nephrol Dial Transplant [Suppl] 10: 80–89
Fine RN, Kohaut EC, Brown D, Periman AJ, for the Gentech Cooperative Study Group (1993) Growth after recombinant human growth hormone treatment in children with chronic renal failure: report of a multicenter randomized double blind placebo-controlled study. J Pediatr 124: 374–382
Tönshoff B, Mehls O, Heinrich U, Blum WF, Ranke MB, Schauer A (1990) Growth-stimulating effects of recombinant human growth hormone in children with end-stage renal disease. J Pediatr 116: 561–566
Mehls O, Broyer M on behalf of the European/Australian Study Group (1994) Growth response to recombinant human growth hormone in short prepubertal children with chronic renal failure or without dialysis. Acta Paediatr [Suppl] 399: 81–87
Tönshoff B, Dietz M, Haffner D, Tönshoff C, Stövr B, Mehls O and members of the German Study Group for Growth Hormone Treatment in Chronic Renal Failure (1991) Effects of 2 years of growth hormone treatment in short children with renal disease. Acta Paediatr Scand [Suppl] 279: 33–41
Wühl E, Haffner T, Tönshoff B, Mehls O, and the German Study Group for Growth Hormone Treatment in Chronic Renal Failure (1993) Predictors of growth response to rhGH in short children before and after renal transplantation. Kidney Int [Suppl] 44: 76–82
Schaefer F, Wühl E, Haffner D, Mehls O and the German Group for Growth Hormone Treatment in Chronic Renal Failure (1994) Stimulation of growth by recombinant human growth hormone in children undergoing peritoneal or hemodialysis treatment. Adv Perit Dial 10: 321–326
Prader A, Largo RH, Molinari L, Issler C (1989) Physical growth of Swiss children from birth to 20 years of age. Helv Paediatr Acta [Suppl] 52: 1–125
Tanner JM, Whitehouse RH, Cameron N, Marshall WA, Healy MJR, Goldstein H (1983) Assessment of skeletal maturity and prediction of adult height (TW2 method), 2nd edn. Academic Press, New York
Schwartz GJ, Brion LP, Spitzer A (1987) The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children and adolescents. Pediatr Clin North Am 34: 571–590
Kramer MS, Rooks Y, Washington L, Pearson HA (1980) Pre- and postnatal growth and development in children with sickle cell anemia. J Pediatr 96: 857–860
Mehls O, Ritz E (1983) Skeletal growth in experimental uremia. Kidney Int [Suppl] 15: 853–862
Schaefer F, André JL, Krug C, Messinger D, Scigalla P (1991) Growth and skeletal maturation in dialysed children treated with rh-erythropoietin (r-HuEPO) — a multicenter study. Pediatr Nephrol 5: C61
Jabs K (1995) Effect of correction of anemia with recombinant human erythropoietin on growth. Pediatr Nephrol 10: 324–327
May RC, Kelly RA, Mitch WE (1987) Mechanisms for defects in muscle protein metabolism in rats with chronic uremia. J Clin Invest 79: 1099–1103
McSherry E, Sebastian A, Morris RC Jr (1973) Correction of impaired growth in children with classic renal tubular acidosis by sustained correction of acidosis. Clin Res 21: 700–711
Cooke RE, Boyden DG, Haller E (1960) The relationship of acidosis and growth retardation. J Pediatr 57: 326–337
Mehls O, Ritz E, Gilli G, Kreusser W (1978) Growth in renal failure. Nephron 21: 237–247
Betts PR, Magrath G (1974) Growth pattern and dietary intake of children with chronic renal insufficiency. BMJ 2: 189–194
Kleinknecht C, Broyer M, Hout C, Marti-Henneberg C, Dartois AM (1983) Growth and development of nondialyzed children with chronic renal failure. Kidney Int [Suppl] 15: 40–47
Schaefer F, Wingen A-M, Hennicke M, Rigden S, Mehls O and European Study Group for Nutritional Treatment of Chronic Renal Failure in Childhood (1995) Disease-specific growth charts for prepubertal children with chronic renal failure due to congenital renal disorders. Pediatr Nephrol 10: 288–293
Tönshoff B, Eden S, Weiser E, Carlson B, Robinson ICAF, Blum WF, Mehls O (1994) Reduced hepatic growth hormone (GH) receptor gene expression and increased plasma GH binding protein in experimental uremia. Kidney Int 45: 1085–1092
Postel-Vinay MC, Tar A, Crosnier H, Broyer M, Rappaport R, Tönshoff B, Mehls O (1991) Plasma growth hormone binding is low in uremic children. Pediatr Nephrol 5: 545–547
Tönshoff B, Powell DR, Dongling Z, Domene HM, Blum WF, Moore LC, Kaskel FJ (1995) Decreased hepatic insulin-like growth factor (IGF)-I and increased IGF binding protein (IGFBP)-I and-2 gene expression in experimental uremia. )abstract). J Am Soc Nephrol 6: 1032
Tönshoff B, Blum WF, Mehls O (1995) Serum insulin-like growth factors (IGFs) and IGF binding proteins 1, 2 and 3 in children with end-stage renal failure. Pediatr Nephrol 10: 269–274
Author information
Authors and Affiliations
Consortia
Additional information
Study group members: K. Bittner (Ansbach), J. H. H. Ehrich, G. Filler, J. Gellermann (Berlin), H. Hampel (Berlin), H. Bachmann (Bremen), H. Ruder (Erlangen), K. E. Bonzel, B. Scheller (Essen), J. Dippel (Frankfurt), L. B. Zimmerhackl (Freiburg), J. Kreuder, W. Rascher (Gießen), D. Müller-Wiefel (Hamburg), D. Haffner, O. Mehls, R. Nissel, E. Wühl (Heidelberg (coordinators)), J. Misselwitz, B. Rönnefarth (Jena), U. Querfeld (Köln), H. Eichstädt, C. Greiner, E. Keller (Leipzig), H. P. Weber (Lüdenscheid), H. R. Heise, D. Wiemann (Magdeburg), R. Beetz (Mainz), D. Sasse, M. Soergel (Marburg), K. Pistor, A. Zlotkowski (Moers), B. Klare (München), R. Eife (München), E. Kuwertz-Bröking (Münster), M. Wigger, M. Mix (Rostock), O. Eichler (Suhl)
Rights and permissions
About this article
Cite this article
Wühl, E., Haffner, D., Nissel, R. et al. Short dialyzed children respond less to growth hormone than patients prior to dialysis. Pediatr Nephrol 10, 294–298 (1996). https://doi.org/10.1007/BF00866763
Received:
Revised:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00866763