Abstract
There is a growing appreciation for the role that acute kidney injury (AKI) plays in the propagation of critical illness. In children, AKI is not only an independent predictor of morbidity and mortality, but is also associated with especially negative outcomes when concurrent with acute lung injury (ALI). Experimental data provide evidence that kidney–lung crosstalk occurs and can be bidirectionally deleterious, although details of the precise molecular mechanisms involved in the AKI–ALI interaction remain incomplete. Clinically, ALI, and the subsequent clinical interventions used to stabilize gas exchange, carry consequences for the homeostasis of kidney function. Meanwhile, AKI negatively affects lung physiology significantly by altering the homeostasis of fluid balance, acid–base balance, and vascular tone. Experimental AKI research supports an “endocrine” role for the kidney, triggering a cascade of extra-renal inflammatory responses affecting lung homeostasis. In this review, we will discuss the pathophysiology of kidney–lung crosstalk, the multiple pathways by which AKI affects kidney–lung homeostasis, and discuss how these phenomena may be unique in critically ill children. Understanding how AKI may affect a “balance of communication” that exists between the kidneys and the lungs is requisite when managing critically ill children, in whom imbalance is the norm.
Similar content being viewed by others
Introduction
Organ cross-talk is of particular importance to practitioners in the intensive care unit (ICU); many disease processes that affect ICU patients carry the potential to affect a number of different tissue beds. In such multiple organ dysfunction syndromes (MODS), global injury becomes augmented when dysfunction in individual organs contributes to the dysfunction of other organs via aberrant organ–organ homeostasis (i.e., cross-talk). Also, therapeutic interventions (i.e., mechanical ventilation) initiated by intensivists, targeted at specific organ dysfunction, can often carry broader consequences. In order to properly manage these complex patients, it is crucial to understand organ cross-talk in baseline health and during critical illness.
Proper individual organ function, and therefore baseline organ cross-talk, depends on appropriate oxygen metabolism. Single- or multi-organ disease is often a phenotypic manifestation of aberrant oxygen delivery at the tissue level (hypoxia) or impaired oxygen utilization (dysoxia) [1]. From applied physiology, oxygen delivery can be quantified as:
where DO2 is oxygen delivery, CO is cardiac output, and CaO2 is the content of oxygen in arterial blood. Broken down further:
where VO2 = oxygen consumption at the tissue bed, A-V O2 = the arterial to venous oxygen content difference, HR = heart rate, SV = stroke volume, Hgb = hemoglobin, SpO2 = the peripheral saturation of oxygen, and paO2 = partial pressure of oxygen in the arterial blood. At first glance, it would appear that the kidneys are not involved in this equation; conceivably, oxygen delivery is directly proportional only to cardiac output and to arterial oxygen content such that delivery in “organ terms” is:
However, kidney function is a prerequisite for both cardiac and lung function. The kidney is central to oxygen delivery as it governs the following (Fig. 1):
The kidney plays a central role in supporting oxygen delivery. a Increases in preload (oliguric acute kidney injury) affect cardiac performance. b Afterload determined by renal effects on vascular tone affects stroke volume. c) Acid–base balance affects enzymatic function (black) and vascular resistance (red). d Control of erythropoietin affects oxygen-carrying capacity (CaO2)
-
1.
Fluid balance (i.e., preload, a critical lever of stroke volume as per Starling’s relationship of volume and cardiac output)
-
2.
Vascular tone (i.e., hormonal regulation through renin angiotensin and afterload, a critical determinant of left ventricular systolic wall tension according to LaPlace’s law relating pressure and wall tension)
-
3.
Electrolyte and acid–base balance (i.e., regulation of tissue-level oxygen uptake and global cellular enzymatic function)
-
4.
Erythropoietin production (i.e., affecting hemoglobin concentration and thus oxygen-carrying capacity)
Conceptually, the equation for oxygen delivery could then be rewritten:
where “∫”(integral) refers to the aggregate kidney functions listed above. It should be noted that kidney function carries a directly proportional relationship to both cardiac and lung function, meaning that if kidney function decreases, cardiac and lung function decrease in an obligatory manner. Therefore, kidney dysfunction, from a purely physiological–mathematical perspective, carries the potential to severely disrupt tissue oxygen delivery and utilization. Resuscitation targets for critically ill adults and children are typically focused on proper oxygen supply and demand at the tissue level [2, 3]. As this review will attest, AKI makes these targets more difficult to attain. The interdependence of the lungs and kidneys is highly susceptible to both critical illness and the interventions used to treat critical illness. Understanding the epidemiology and pathophysiology of AKI–acute lung injury (ALI)—in pediatric critical care is crucial to recognizing the clinical manifestations of the phenomena and to creating the most effective restorative therapies.
Epidemiology: AKI, ALI, and multi-organ disease syndrome
Acute kidney injury occurs at an alarming rate; approximately 10 % of critically ill children suffer from varying degrees of AKI [4]. If “severe” AKI is defined by the need for renal replacement therapy, the estimated incidence is 1–2 % of all critically ill children [5]. In those children, the mortality rate approaches 50 % [6, 7]. For children undergoing cardiopulmonary bypass, the incidence of AKI increases (10–50 %) [8]. Additionally, recent data suggest that even in the non-critically ill pediatric population, AKI secondary to nephrotoxic medications occurs at an alarming rate [9]. Both non-oliguric and oliguric AKI carry notably increased morbidity risk, including longer duration of mechanical ventilation, hospital length of stay [10], and mortality [11].
Acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) are severe disorders of pulmonary inflammation that occur in critically ill children independently or in concert with multi-organ disease. The most common etiologies are direct lung injury (as occurs with parenchymal lung infection (i.e., pneumonia) or hemorrhage) and indirect lung injury (secondary to inflammation as occurs with sepsis) [12]. In children, estimates suggest that roughly 5,000 children will suffer from ALI/ARDS yearly [13]. In published studies, mortality from ALI/ARDS in children is greater than 25 % [14].
While not the only driver of both AKI and ALI, sepsis-induced MODS is the most common lead-point cause for both and therefore serves as the best surrogate for pediatric AKI–ALI epidemiology. Over 40,000 children in the United States suffer from sepsis each year and incur a mortality of nearly 10 %. More importantly, several studies strongly suggest that sepsis is the leading cause of pediatric mortality worldwide [15, 16]. In MODS, respiratory failure and kidney injury are associated with high rates of morbidity and mortality. Further, reversing a long-standing paradigm, a decade of epidemiological study now suggests that patients (children) are not just dying with AKI, but from AKI. For the intensivist, it is imperative to understand the mechanistic details of how the kidney is an active participant of negative inter-organ crosstalk and not just an innocent bystander.
The kidney “engine”
Clinical and experimental data hint that in some forms of critical illness, kidney injury may be the primary perturbation of homeostasis that subsequently leads to remote organ dysfunction. In this view kidney injury becomes the “engine,” rather than a sign of, multiple organ dysfunction (Fig. 2). The extra-renal effects of AKI (i.e., dual organ clinical “syndromes”) have experimental evidence and are based on sound theoretical constructs.
Acute kidney injury affects heart function; cardiovascular problems that occur with AKI include hypotension, decreased cardiac contractility, and cardiac arrhythmias [17]. In a model of isolated renal ischemic–reperfusion injury, rats with AKI suffered decreased left ventricular shortening fraction and increased myocardial apoptosis versus their sham cohorts [18]. The cardio-renal interaction controls extracellular fluid volume and arterial blood pressure via the renin–angiotensin feedback system, production of nitric oxide and reactive oxygen species, and regulation of the sympathetic nervous system [19]. Diminished cardiac function coupled with renal dysfunction (cardiorenal syndrome) in children is associated with prolonged hospitalization (length of stay increased from 18 ± 25 to 33 ± 30 days) and greater in-hospital mortality or need for mechanical circulatory support adjusted odds ratio 10.2 (95 % confidence interval; 1.7–61.2) [20]. A paucity of literature, however, indicates the current absence of firm evidence supporting causal effects of AKI on the heart. The kidney and heart likely participate in bidirectional crosstalk, but the specifics of the interaction require further investigation.
Acute kidney injury affects the hematological system. Uremia during AKI can lead to a “hemato-renal syndrome,” a coagulopathy from decreased platelet–vessel wall adhesion, impaired platelet release of α-granule proteins and β-thromboglobulin, and altered blood cell rheology [21]. The kidney is connected to the hematological system through the hormone erythropoietin (epo). In a rodent model of AKI, epo transcriptional ability remained high; however, epo response to blood oxygen was reduced [22]. In patients with end-stage kidney disease, anemia may be secondary to both inhibited production of epo and from cytokine-mediated inhibition of iron transport [23]. A small clinical study of patients with AKI on hemofiltration indicated that epo levels decreased toward the end of disease [24]. Further studies examining the effects of AKI on epo production are required to bolster the argument that AKI leads to alteration of the kidney–heme interaction.
While liver function affects kidney function, AKI leading to liver dysfunction has been difficult to prove. Experimentally, ischemic models of AKI are associated with increased levels of inflammatory and apoptotic mediators in the liver [25]. Clinically, azotemia increases the risk of hepatic encephalopathy in patients with liver failure owing to the increased absorption of ammonia (NH3) in the gut, failure to maintain the appropriate NH3/NH4 + balance (from AKI), and resultant increases in translocation of NH3 to the brain [26]. Hepatorenal syndrome (HRS), defined as the presence of advanced hepatic disease and kidney dysfunction absent shock, infection, or nephrotoxins carries significant morbidity in children [27].
Acute kidney injury may carry significant consequence for proper central nervous system function. AKI can deleteriously affect neuro-renal crosstalk. Experimentally, mice subjected to ischemic kidney injury have significantly altered higher neurological executive function and increased levels of glial apoptosis than sham cohorts [28]. AKI affects cerebral blood flow and regulation of the neurotransmitters γ-aminobutyric acid (GABA) and N-methyl-D-aspartate (NMDA) [29]. Guanadino compounds (e.g., creatinine) are increased in the cerebrospinal fluid of end-stage kidney disease patients and these may increase cortical excitability by acting as GABAA receptor antagonists and NMDA receptor agonists [30]. Patients with traumatic brain injury or cerebral edema with concurrent AKI are known to have worsened mortality [31], although the mechanism for this is unclear.
Acute kidney injury negatively impacts the immune system through immuno-renal crosstalk. Altered immunological response, disrupted T-cell trafficking and loss of balance between the pro- and anti-inflammatory transcriptome after isolated AKI have been described [32, 33]. Patients with AKI are known to be at a higher risk of infection secondary to fluid overload, metabolic acidosis, malnutrition, and uremia [34]. This again may be a clinical manifestation of the kidney acting as a mediator of systemic inflammation, and AKI causing a maladaptive response to stress (i.e., infection) [35].
Finally, AKI affects reno-pulmonary crosstalk; several immune-mediated pulmonary–renal syndromes are described (Goodpasture’s disease and Wegener’s granulomatosis). The remainder of this review focuses on the interactions between the kidneys and lungs, with a focus on the influence of AKI, particularly in the critically ill child.
Kidney–lung crosstalk
ALI and kidney function
Lung function influences kidney function by three distinct homeostatic mechanisms, which can be affected during ALI: gas exchange (pO2 and pCO2), inflammatory cytokine release, and cardiopulmonary interactions.
The kidney is highly sensitive to changes in oxygen tension. Under normal conditions, the combination of high oxygen consumption by the renal concentrating apparatus (especially in the loops of Henle and the proximal tubules) and relatively low total renal blood flow creates areas of the kidney that are always under the threat of hypoxic injury. Even though quantitative renal VO2 is “low,” autoregulation of renal blood flow is required for the renal parenchyma to optimize DO2 and low O2 tension throughout the medulla and concentrating apparatus. During ALI, however, this autoregulation is insufficient to maintain adequate oxygenation because parenchymal lung disease leads to decreased arterial oxygen content and oxygen availability. Severe hypoxemia has been demonstrated to decrease renal blood flow [36], but the precise effects of adaptive mechanisms to hypoxia, including nitric oxide, vasopressin, prostaglandin I2, and several interleukins [37], are unknown.
Carbon dioxide (pCO2) is involved in the regulation of renal vascular tone. Hypercapnia affects renal blood flow directly and indirectly. Directly, hypercapnia may decrease renal blood flow by stimulating renal vasoconstriction (via norepinephrine release), although the net effects on GFR are conflicting [38, 39]. Indirectly, systemic vasodilation triggered by high pCO2 may lower effective renal perfusion and activate the renin–angiotensin–aldosterone feedback response . Renovascular changes seen in hypercapnia are independent of changes in pO2 [38]. The net effect of hypercapnia, seen over time in patients with long-standing lung disease, is a marked reduction in glomerular filtration (GFR) [40].
A cardinal feature of ARDS is a complex inflammatory response leading to downstream consequences on extra-pulmonary organ beds. Patients who suffer from ARDS have increased rates of AKI, and those who have both ARDS and AKI have increased mortality [41]. Pro-inflammatory mediators, IL-1β, IL-6, IL-8, and TNF-α, are all associated with the propagation of AKI [42]. During ALI/ARDS, the local and systemic release of inflammatory mediators can affect renal vascular tone (i.e., via release of nitric oxide) and renal cell viability (i.e., via release of caspase-3 and other pro-apoptotic agents).
Renal perfusion is reliant on cardiopulmonary interaction, which is particularly crucial in patients with ventilatory failure requiring mechanical ventilation (MV). The change from spontaneous to MV dramatically affects cardiac output and is a major contributor to the pathogenesis of AKI during ALI/ARDS. The two major mechanisms by which MV negatively affect kidney function are by a decrease in cardiac output and by stimulation of sympathetic pathways [37]. In ALI/ARDS, high ventilatory pressures required for gas exchange come at the expense of increased afterload on the heart (decreasing right ventricular output), decreased venous return, and ultimately a decreased cardiac output. The reduction in cardiac output decreases renal perfusion and leads to a decrease in GFR. This effect may be particularly significant in children with ALI/ARDS; children have less cardiac “reserve,” higher chest wall compliance (requiring higher pressures to obtain adequate lung tidal volumes), and are at greater risk of intravascular fluid shifts during acute illness [43]. MV triggers counter-regulatory effects in the kidney (i.e., sympathetic stimulation and the renin–angiotensin system), which further decrease filtration and kidney function via local vasoconstriction; positive end-expiratory pressure (PEEP) increases sympathetic tone, which subsequently increases renin activity. Atrial stretch during MV (from increased ventricular afterload) leads to fluid retention [44]. Although less well-documented in pediatrics, the effects of MV-related neuro-hormonal stimulation on kidney function may be a vital connection between the lungs and kidneys.
In summary, the lungs participate in reno-pulmonary crosstalk on multiple levels. Dysregulation of gas exchange, cytokine balance, and cardiac output, resultant either from direct ALI/ARDS or the interventions instituted to treat these diseases, can have significant consequences for proper kidney function. This crosstalk is particularly important for the critically ill pediatric patient owing to both the anatomical differences in the lung (versus adults) and the relative lack of lung “reserve.”
AKI and lung function: from the bedside
Lung function is regulated by the ability of the kidney to balance three distinct metabolic systems (nitrogenous waste, fluid movement, and acid–base), all of which can be negatively affected during AKI. Uremia affects gas exchange and lung mechanics. Clinical studies of adult ICU patients with uremia demonstrate a decrease in the diffusion capacity for carbon monoxide (DLCO), a marker of pulmonary capillary function [45, 46]. Additionally, the negative effects of uremia on forced vital capacity (FVC), forced exhalation volume in 1 s (FEV1), maximal breathing capacity (MBC), have been described [46].
In the normal host, fluid movement is dependent on both hydrostatic and oncotic pressure (modeled by the Starling equation):
where PC-PT gives directionality to hydrostatic pressure and πC-πT gives directionality to oncotic pressure [47]. Under normal conditions fluid stays in the capillary lumen because PC ≃ PT and πC > πT. Fluid overload leads to a large difference between hydrostatic forces and oncotic forces, leading to fluid flux from the capillary bed into the alveolar space. The capillary endothelium between the interstitium and the alveolar beds, which can usually tolerate large fluid pressure discrepancies, is compromised and alveolar edema (pulmonary edema) results [48]. The integrity of tight alveolar–epithelial barriers, required for the drainage of pulmonary edema, is compromised in experimental AKI studies [49]. Data from critically ill children demonstrate a clear association between increasing fluid overload and worsened oxygenation as measured by the oxygenation index [50] and decreased ventilator-free days [51]. The prospective pediatric continuous renal replacement therapy (PP-CRRT) registry has repeatedly demonstrated that increased fluid overload (FO; fluid measured in milliliters and weight in kilograms):
at the time of RRT initiation, is associated with a marked increase in mortality in children [52–55]. Although the exact degree of fluid overload needed to trigger CRRT initiation is controversial, a clinician should be vigilant about prevention of fluid overload by governing the details of “ins and outs,” monitor daily %FO (using 10–20 % as a threshold to consider RRT), and consider RRT early to optimize the delivery of fluids (predominantly nutrition).
The management of electrolyte and acid–base balance by the kidney, specifically the equilibrium of bicarbonate (HCO3 −), carbonic acid (H2CO3), and carbon dioxide (CO2), is critical to lung function. Carbonic anhydrase (CA) directly controls pH in the body via:
where H20 = water and H+ = hydrogen ion. Under normal conditions, when arterial pH begins to shift, compensation (buffering) occurs by both the lungs and kidneys. In response to a respiratory acidosis, the kidneys will increase bicarbonate reabsorption from the proximal and distal tubules to enhance acid buffering and prevent a shift in the equilibrium (Eq. 7) toward acidosis. Conversely, with metabolic acidosis, from decreased availability of bicarbonate, medullary chemoreceptors will trigger hyperventilation to lower the pCO2 in the blood to prevent a shift toward acidosis. The balancing act is similar for states of alkalosis. When either the lungs or the kidneys suffer injury, the ability to maintain this crucial balance is lost and the controls over acid–base regulation/buffering become compromised.
In summary, understanding the pathophysiology of uremia, fluid movement, and acid–base balance allows intensivists to understand the effect of kidney function, and the consequence of kidney injury, on lung function.
AKI and lung function: from the bench
While the clinical effects of AKI on lung function are obvious, subtle and equally important “subclinical” effects of AKI on lung function also occur. Negative effects on lung function have been demonstrated after isolated kidney ischemia: alveolar concentrations of pro-inflammatory cytokines and chemokines (as measured in bronchoalveolar fluid) are increased [56], macrophage-mediated pulmonary vascular permeability is increased [57], epithelial sodium channel (ENaC) and aquaporin-5 are downregulated [49], caspase-dependent apoptosis is upregulated [58], and T-cell trafficking of antigen in the lungs is disrupted [33]. The combined effect of ischemic AKI is thus a lung that is “wetter,” “inflamed,” and potentially less able to deal with secondary injury. A dry lung is a happy lung! Owing to the microvascular nature of the pulmonary effects of experimental AKI, absent overt fluid overload (in experimental animals), a condition of nephrogenic pulmonary edema, has been proposed [59]. A natural secondary question then becomes whether the lung is “primed” for injury after ischemic AKI. Several two-hit models combining ALI and AKI have demonstrated conflicting results. In models of mechanical ventilation, mice with AKI had improvements in lung injury induced by high tidal volume ventilation versus mice without AKI [60]. Further, in aseptic ALI (hydrochloric acid), uremic neutrophils appears to decrease inflammatory mediator recruitment to the lung, thereby decreasing lung injury [61]. However, decreased neutrophil recruitment carries the risk of worsened bacterial pneumonia and a secondary lipopolysaccharide-induced ALI after antecedent ischemic AKI demonstrated augmented lung inflammation [62].
Taken together, clinical evidence and experimental evidence demonstrate clearly how deleterious AKI can be on lung function. In children, this connection is amplified owing to several factors. As stated earlier, increased chest wall compliance in children makes positive pressure ventilation particularly challenging and potentially has a more negative impact on cardiac output (and therefore renal perfusion). Children have a higher percentage of total body water than adults—meaning that the precise fluid balance maintained between the lungs and the kidneys has even less room for error (or less tolerance to injury). The systemic inflammatory response manifest by children during multi-organ disease (of which lung and kidney are the two most commonly injured organs) is unique from the adult response in the following ways: maturation of cells responsible for immune mediation, expression and chemokine receptor sensitivity, and the propagation of the pro- and anti- inflammatory response. The intensivist must be mindful of the myriad consequences of AKI, from the subtle to the obvious, on lung function.
Therapeutics of AKI: ameliorating crosstalk with the lung
Unfortunately, no specific single therapy currently exists for AKI. Intensivists are therefore left to deal with facets of AKI management that can limit the extent of injury, particularly the characteristics of AKI that have a negative impact on lung function. The four mainstays of therapy for AKI in this regard are: early diagnosis, limitation of ventilation-induced kidney injury, regulation of the acid–base balance, and limitation of fluid overload.
Research investigating early and real-time diagnosis of AKI is biomarker-based. Unfortunately for clinicians, most patients do not have a time zero injury (deviating from animal models) and are also quite heterogeneous (the typical MODs patient) and thus the applicability of a new AKI biomarker(s) (derived in homogeneous models) may be quite limited. The construct of renal angina attempts to risk-stratify patients to optimize biomarker testing. Akin to the clinical signs and risk factors that optimize the performance of Troponin-I measurements in the diagnosis of a myocardial infarction (MI), renal angina risk stratifies patients for AKI based on epidemiologically proven risk factors with early and subtle clinical signs [63–65]. Simply stated, since AKI does not “hurt” like an MI typically does, renal angina is a methodology to identify patients (like changes on the electrocardiogram of obese smokers is for heart disease); thus, a clinician can utilize biomarkers with the highest yield (troponins are also useless in patients without acute coronary syndrome) [66].
Intensivists should be judicious about the effects of mechanical ventilation on cardiac output. Understanding the effects of mechanical ventilation on venous return and ventricular afterload will allow intensivists to simultaneously limit ventilator-associated barotrauma and optimize cardiac output (and thus renal perfusion). Pediatric intensivists should be especially mindful of the effects of chest wall compliance differences by age, the effects of chest wall inertia (increased with fluid accumulation and subcutaneous edema), and the effects of the unique features of pediatric airway resistance on the pressure delivery requirements for invasive mechanical ventilation.
Intensivists should vigilantly monitor electrolyte balance. As the kidney and lung balance alkalemia and acidemia, physiological states (shock), which can lead to a large acid load should be treated aggressively to prevent both pulmonary and renovascular constriction and the triggering of “compensatory” mechanisms, which often make the problem worse (i.e., sympathetic stimulation on renal vasculature). Similarly, the removal of all non-essential nephrotoxins and adjustment of all renally cleared medications in patients with AKI limits the aggregate effects of renal parenchymal injury. Adjustments based on fluid and weight are particularly important in children whose total body volume and water/fat composition are quite variable compared with adults.
Finally, intensivists are becoming increasingly cognizant of the deleterious effects of fluid overload. During oliguric AKI, the PPCRRT registry has demonstrated repeatedly in retrospective studies that higher fluid overload at time of CRRT initiation is associated with increased length of stay, increased duration of mechanical ventilation, and increased mortality. For intensivists, it is important to understand that there are pulmonary bed regulatory mechanisms in place to handle fluid (Starling mechanism), but that these mechanisms can be overwhelmed by not only excessive fluid but also the inflammatory mediators associated with AKI. Again, in pediatrics, it is paramount for the intensivist to understand that fluid is a drug—prescribed, dosed, and delivered like all other medications—and that it is possible to overdose! No other evidence of kidney–lung crosstalk is more explicit than the effects on the lung of oliguric AKI.
Conclusions
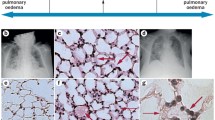
The crosstalk that occurs between the kidney and lung in a normal host is under precise control. The mechanisms responsible for this control are vulnerable to disruption during AKI, carrying significant consequences (Fig. 3). It is imperative for the intensivist, especially the pediatric intensivist, to have a proper understanding of the pathophysiology of not only AKI, but also the multiple connections that can cause harmful kidney–lung crosstalk during illness.
Acute kidney injury (AKI) significantly affects kidney–lung crosstalk. Through numerous mechanisms, both clinically manifest and subtle, AKI leads to aberrant kidney–lung homeostasis. DL CO diffusion limitation of carbon monoxide—a marker of alveolar gas exchange capability, FVC forced vital capacity, FEV 1 forced exhaled volume in 1 s
References
Rosenberger C, Rosen S, Heyman SN (2006) Renal parenchymal oxygenation and hypoxia adaptation in acute kidney injury. Clin Exp Pharmacol Physiol 33:980–988
Rivers E, Nguyen B, Havstad S, Ressler J, Muzzin A, Knoblich B, Peterson E, Tomlanovich M (2001) Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Engl J Med 345:1368–1377
Brierley J, Carcillo JA, Choong K, Cornell T, Decaen A, Deymann A, Doctor A, Davis A, Duff J, Dugas MA, Duncan A, Evans B, Feldman J, Felmet K, Fisher G, Frankel L, Jeffries H, Greenwald B, Gutierrez J, Hall M, Han YY, Hanson J, Hazelzet J, Hernan L, Kiff J, Kissoon N, Kon A, Irazuzta J, Lin J, Lorts A, Mariscalco M, Mehta R, Nadel S, Nguyen T, Nicholson C, Peters M, Okhuysen-Cawley R, Poulton T, Relves M, Rodriguez A, Rozenfeld R, Schnitzler E, Shanley T, Kache S, Skippen P, Torres A, von Dessauer B, Weingarten J, Yeh T, Zaritsky A, Stojadinovic B, Zimmerman J, Zuckerberg A (2009) Clinical practice parameters for hemodynamic support of pediatric and neonatal septic shock: 2007 update from the American College of Critical Care Medicine. Crit Care Med 37:666–688
Schneider J, Khemani R, Grushkin C, Bart R (2010) Serum creatinine as stratified in the RIFLE score for acute kidney injury is associated with mortality and length of stay for children in the pediatric intensive care unit. Crit Care Med 38:933–939
Bailey D, Phan V, Litalien C, Ducruet T, Merouani A, Lacroix J, Gauvin F (2007) Risk factors of acute renal failure in critically ill children: a prospective descriptive epidemiological study. Pediatr Crit Care Med 8:29–35
Akcan-Arikan A, Zappitelli M, Loftis LL, Washburn KK, Jefferson LS, Goldstein SL (2007) Modified RIFLE criteria in critically ill children with acute kidney injury. Kidney Int 71:1028–1035
Symons JM, Chua AN, Somers MJ, Baum MA, Bunchman TE, Benfield MR, Brophy PD, Blowey D, Fortenberry JD, Chand D, Flores FX, Hackbarth R, Alexander SR, Mahan J, McBryde KD, Goldstein SL (2007) Demographic characteristics of pediatric continuous renal replacement therapy: a report of the prospective pediatric continuous renal replacement therapy registry. Clin J Am Soc Nephrol 2:732–738
Zappitelli M, Bernier PL, Saczkowski RS, Tchervenkov CI, Gottesman R, Dancea A, Hyder A, Alkandari O (2009) A small post-operative rise in serum creatinine predicts acute kidney injury in children undergoing cardiac surgery. Kidney Int 76:885–892
Kirkendall E, Schaffzin J, Ashby M, Goldstein S (2012) Nephrotoxic medication associated acute kidney injury; the epidemic exists. Pediatric Academic Societies, Boston
Skippen PW, Krahn GE (2005) Acute renal failure in children undergoing cardiopulmonary bypass. Crit Care Resusc 7:286–291
Blinder JJ, Goldstein SL, Lei VV, Baycroft A, Fraser CD Jr, Nelson DP, Jefferies JL (2012) Congenital heart surgery in infants: effects of acute kidney injury on outcomes. J Thorac Cardiovasc Surg 143:368–374
Randolph AG (2009) Management of acute lung injury and acute respiratory distress syndrome in children. Crit Care Med 37:2448–2454
Dahlem P, van Aalderen WM, Bos AP (2007) Pediatric acute lung injury. Paediatr Respir Rev 8:348–362
Dahlem P, van Aalderen WM, Hamaker ME, Dijkgraaf MG, Bos AP (2003) Incidence and short-term outcome of acute lung injury in mechanically ventilated children. Eur Respir J 22:980–985
Watson RS, Carcillo JA, Linde-Zwirble WT, Clermont G, Lidicker J, Angus DC (2003) The epidemiology of severe sepsis in children in the United States. Am J Respir Crit Care Med 167:695–701
Riley C, Basu RK, Kissoon N, Wheeler DS (2012) Pediatric sepsis: preparing for the future against a global scourge. Curr Infect Dis Rep 14:503–511
Levy EM, Viscoli CM, Horwitz RI (1996) The effect of acute renal failure on mortality. A cohort analysis. JAMA 275:1489–1494
Kelly KJ (2003) Distant effects of experimental renal ischemia/reperfusion injury. J Am Soc Nephrol 14:1549–1558
Bongartz LG, Cramer MJ, Doevendans PA, Joles JA, Braam B (2005) The severe cardiorenal syndrome: ‘Guyton revisited’. Eur Heart J 26:11–17
Price JF, Mott AR, Dickerson HA, Jefferies JL, Nelson DP, Chang AC, O’Brian Smith E, Towbin JA, Dreyer WJ, Denfield SW, Goldstein SL (2008) Worsening renal function in children hospitalized with decompensated heart failure: evidence for a pediatric cardiorenal syndrome? Pediatr Crit Care Med 9:279–284
Ferguson JH, Lewis JH, Zucker MB (1956) Bleeding tendency in uremia. Blood 11:1073–1076
Tan CC, Tan LH, Eckardt KU (1996) Erythropoietin production in rats with post-ischemic acute renal failure. Kidney Int 50:1958–1964
Silverberg DS, Wexler D, Iaina A, Steinbruch S, Wollman Y, Schwartz D (2006) Anemia, chronic renal disease and congestive heart failure—the cardio renal anemia syndrome: the need for cooperation between cardiologists and nephrologists. Int Urol Nephrol 38:295–310
Morgera S, Heering P, Szentandrasi T, Niederau C, Grabensee B (1997) Erythropoietin in patients with acute renal failure and continuous veno-venous haemofiltration. Int Urol Nephrol 29:245–250
Li X, Hassoun HT, Santora R, Rabb H (2009) Organ crosstalk: the role of the kidney. Curr Opin Crit Care 15:481–487
Warren KS, Nathan DG (1958) The passage of ammonia across the blood–brain-barrier and its relation to blood pH. J Clin Invest 37:1724–1728
Sutherland SM, Alexander SR, Sarwal MM, Berquist WE, Concepcion W (2008) Combined liver-kidney transplantation in children: indications and outcome. Pediatr Transplant 12:835–846
Liu M, Liang Y, Chigurupati S, Lathia JD, Pletnikov M, Sun Z, Crow M, Ross CA, Mattson MP, Rabb H (2008) Acute kidney injury leads to inflammation and functional changes in the brain. J Am Soc Nephrol 19:1360–1370
Battaglia F, Quartarone A, Bagnato S, Rizzo V, Morgante F, Floccari F, Romeo A, Sant’Angelo A, Grasso G, Girlanda P, Buemi M (2005) Brain dysfunction in uremia: a question of cortical hyperexcitability? Clin Neurophysiol 116:1507–1514
D’Hooge R, De Deyn PP, Van de Vijver G, Antoons G, Raes A, Van Bogaert PP (1999) Uraemic guanidino compounds inhibit gamma-aminobutyric acid-evoked whole cell currents in mouse spinal cord neurones. Neurosci Lett 265:83–86
Corral L, Javierre CF, Ventura JL, Marcos P, Herrero JI, Manez R (2012) Impact of non-neurological complications in severe traumatic brain injury outcome. Crit Care 16:R44
Grigoryev DN, Liu M, Hassoun HT, Cheadle C, Barnes KC, Rabb H (2008) The local and systemic inflammatory transcriptome after acute kidney injury. J Am Soc Nephrol 19:547–558
Lie ML, White LE, Santora RJ, Park JM, Rabb H, Hassoun HT (2012) Lung T lymphocyte trafficking and activation during ischemic acute kidney injury. J Immunol 189:2843–2851
Hoste EA, Blot SI, Lameire NH, Vanholder RC, De Bacquer D, Colardyn FA (2004) Effect of nosocomial bloodstream infection on the outcome of critically ill patients with acute renal failure treated with renal replacement therapy. J Am Soc Nephrol 15:454–462
Bonventre JV, Zuk A (2004) Ischemic acute renal failure: an inflammatory disease? Kidney Int 66:480–485
Kilburn KH, Dowell AR (1971) Renal function in respiratory failure. Effects of hypoxia, hyperoxia, and hypercapnia. Arch Intern Med 127:754–762
Kuiper JW, Groeneveld AB, Slutsky AS, Plotz FB (2005) Mechanical ventilation and acute renal failure. Crit Care Med 33:1408–1415
Zillig B, Schuler G, Truniger B (1978) Renal function and intrarenal hemodynamics in acutely hypoxic and hypercapnic rats. Kidney Int 14:58–67
Rose CE Jr, Walker BR, Erickson A, Kaiser DL, Carey RM, Anderson RJ (1982) Renal and cardiovascular responses to acute hypercapnic acidosis in conscious dogs: role of renin-angiotensin. J Cardiovasc Pharmacol 4:676–687
Hemlin M, Ljungman S, Carlson J, Maljukanovic S, Mobini R, Bech-Hanssen O, Skoogh BE (2007) The effects of hypoxia and hypercapnia on renal and heart function, haemodynamics and plasma hormone levels in stable COPD patients. Clin Respir J 1:80–90
Ko GJ, Rabb H, Hassoun HT (2009) Kidney-lung crosstalk in the critically ill patient. Blood Purif 28:75–83
Ranieri VM, Suter PM, Tortorella C, De Tullio R, Dayer JM, Brienza A, Bruno F, Slutsky AS (1999) Effect of mechanical ventilation on inflammatory mediators in patients with acute respiratory distress syndrome: a randomized controlled trial. JAMA 282:54–61
Kamath SS, Super DM, Mhanna MJ (2010) Effects of airway pressure release ventilation on blood pressure and urine output in children. Pediatr Pulmonol 45:48–54
Annat G, Viale JP, Bui Xuan B, Hadj Aissa O, Benzoni D, Vincent M, Gharib C, Motin J (1983) Effect of PEEP ventilation on renal function, plasma renin, aldosterone, neurophysins and urinary ADH, and prostaglandins. Anesthesiology 58:136–141
Daum S, Janota M, Boudik F (1965) Diffusion capacity of the lung in patients with uremia. Cas Lek Cesk 104:1285–1290
Karacan O, Tutal E, Uyar M, Eyuboglu FO, Sezer S, Ozdemir FN (2004) Pulmonary function in uremic patients on long-term hemodialysis. Ren Fail 26:273–278
Chase MP, Wheeler DS (2007) Disorders of the Pediatric Chest in Pediatric Critical Care Medicine; Basic Science and Clinical Evidence, 1st ed; Springer, London, pp 361–375
Demling RH, LaLonde C, Ikegami K (1993) Pulmonary edema: pathophysiology, methods of measurement, and clinical importance in acute respiratory failure. New Horiz 1:371–380
Rabb H, Wang Z, Nemoto T, Hotchkiss J, Yokota N, Soleimani M (2003) Acute renal failure leads to dysregulation of lung salt and water channels. Kidney Int 63:600–606
Arikan AA, Zappitelli M, Goldstein SL, Naipaul A, Jefferson LS, Loftis LL (2012) Fluid overload is associated with impaired oxygenation and morbidity in critically ill children. Pediatr Crit Care Med 13:253–258
Valentine SL, Sapru A, Higgerson RA, Spinella PC, Flori HR, Graham DA, Brett M, Convery M, Christie LM, Karamessinis L, Randolph AG (2012) Fluid balance in critically ill children with acute lung injury. Crit Care Med 40:2883–2889
Sutherland SM, Zappitelli M, Alexander SR, Chua AN, Brophy PD, Bunchman TE, Hackbarth R, Somers MJ, Baum M, Symons JM, Flores FX, Benfield M, Askenazi D, Chand D, Fortenberry JD, Mahan JD, McBryde K, Blowey D, Goldstein SL (2010) Fluid overload and mortality in children receiving continuous renal replacement therapy: the prospective pediatric continuous renal replacement therapy registry. Am J Kidney Dis 55:316–325
Goldstein SL, Currier H, Graf C, Cosio CC, Brewer ED, Sachdeva R (2001) Outcome in children receiving continuous venovenous hemofiltration. Pediatrics 107:1309–1312
Foland JA, Fortenberry JD, Warshaw BL, Pettignano R, Merritt RK, Heard ML, Rogers K, Reid C, Tanner AJ, Easley KA (2004) Fluid overload before continuous hemofiltration and survival in critically ill children: a retrospective analysis. Crit Care Med 32:1771–1776
Hayes LW, Oster RA, Tofil NM, Tolwani AJ (2009) Outcomes of critically ill children requiring continuous renal replacement therapy. J Crit Care 24:394–400
Klein CL, Hoke TS, Fang WF, Altmann CJ, Douglas IS, Faubel S (2008) Interleukin-6 mediates lung injury following ischemic acute kidney injury or bilateral nephrectomy. Kidney Int 74:901–909
Kramer AA, Postler G, Salhab KF, Mendez C, Carey LC, Rabb H (1999) Renal ischemia/reperfusion leads to macrophage-mediated increase in pulmonary vascular permeability. Kidney Int 55:2362–2367
Hassoun HT, Lie ML, Grigoryev DN, Liu M, Tuder RM, Rabb H (2009) Kidney ischemia-reperfusion injury induces caspase-dependent pulmonary apoptosis. Am J Physiol Renal Physiol 297:F125–F137
Basu RK, Wheeler D (2011) Effects of ischemic acute kidney injury on lung water balance: nephrogenic pulmonary edema? Pulm Med 2011:414253
Dodd OJ, Hristopoulos M, Scharfstein D, Brower R, Hassoun P, King LS, Becker P, Liu M, Wang W, Hassoun HT, Rabb H (2009) Interactive effects of mechanical ventilation and kidney health on lung function in an in vivo mouse model. Am J Physiol Lung Cell Mol Physiol 296:L3–L11
Singbartl K (2011) Renal-pulmonary crosstalk. Contrib Nephrol 174:65–70
Basu RK, Donaworth E, Wheeler DS, Devarajan P, Wong HR (2011) Antecedent acute kidney injury worsens subsequent endotoxin-induced lung inflammation in a two-hit mouse model. Am J Physiol Renal Physiol 301:F597–F604
Basu RK, Chawla LS, Wheeler DS, Goldstein SL (2012) Renal angina: an emerging paradigm to identify children at risk for acute kidney injury. Pediatr Nephrol 27:1067–1078
Goldstein SL (2011) Acute kidney injury biomarkers: renal angina and the need for a renal troponin I. BMC Med 9:135
Goldstein SL, Chawla LS (2010) Renal angina. Clin J Am Soc Nephrol 5:943–949
Lim W, Whitlock R, Khera V, Devereaux PJ, Tkaczyk A, Heels-Ansdell D, Jacka M, Cook D (2010) Etiology of troponin elevation in critically ill patients. J Crit Care 25:322–328
Acknowledgments
None.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Basu, R.K., Wheeler, D.S. Kidney–lung cross-talk and acute kidney injury. Pediatr Nephrol 28, 2239–2248 (2013). https://doi.org/10.1007/s00467-012-2386-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-012-2386-3