Abstract
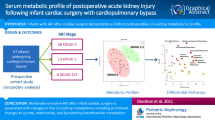
Acute kidney injury (AKI) is a major complication in children who undergo cardiopulmonary bypass surgery. We performed metabonomic analyses of urine samples obtained from 40 children that underwent cardiac surgery for correction of congenital cardiac defects. Serial urine samples were obtained from each patient prior to surgery and at 4 h and 12 h after surgery. AKI, defined as a 50% or greater rise in baseline level of serum creatinine, was noted in 21 children at 48–72 h after cardiac surgery. The principal component analysis of liquid chromatography/mass spectrometry (LC/MS) negative ionization data of the urine samples obtained 4 h and 12 h after surgery from patients who develop AKI clustered away from patients who did not develop AKI. The LC/MS peak with mass-to-charge ratio (m/z) 261.01 and retention time (tR) 4.92 min was further analyzed by tandem mass spectrometry (MS/MS) and identified as homovanillic acid sulfate (HVA-SO4), a dopamine metabolite. By MS single-reaction monitoring, the sensitivity was 0.90 and specificity was 0.95 for a cut-off value of 24 ng/μl for HVA-SO4 at 12 h after surgery. We concluded that urinary HVA-SO4 represents a novel, sensitive, and predictive early biomarker of AKI after pediatric cardiac surgery.






Similar content being viewed by others
References
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG, Levin A (2007) Acute Kidney Injury Network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 11:R31
Morelli S, Ricci Z, Di Chiara L, Stazi GV, Polito A, Vitale V, Giorni C, Iacoella C, Picardo S (2007) Renal replacement therapy in neonates with congenital heart disease. In: Ronco C, Bellomo R, Kellum JA (eds) Contributions to nephrology, vol 156. Karger, Basel, pp 428–433
Skippen PW, Krahn GE (2005) Acute renal failure in children undergoing cardiopulmonary bypass. Crit Care Resusc 7:286–291
Bailey D, Phan V, Litalien C, Ducruet CT, Merouani A, Lacroix J, Gauvin F (2007) Risk factors of acute renal failure in critically ill children: a prospective descriptive epidemiological study. Pediatr Crit Care Med 8:29–35
Williams DM, Sreedhar SS, Mickell JJ, Chan JC (2002) Acute kidney failure: a pediatric experience over 20 years. Arch Pediatr Adolesc Med 156:893–900
Moghal NE, Brocklebank JT, Meadow SR (1998) A review of acute renal failure in children: incidence, etiology and outcome. Clin Nephrol 49:91–95
Goldstein SL (2006) Pediatric acute kidney injury: it’s time for real progress. Pediatr Nephrol 21:891–895
Nguyen MT, Devarajan P (2007) Biomarkers for the early detection of acute kidney injury. Pediatr Nephrol DOI https://doi.org/10.1007/s00467-007-0470-x
Portilla D, Dent C, Sugaya T, Nagothu K, Kundi I, Moore P, Noiri E, Devarajan P (2008) Liver fatty acid binding protein as a biomarker of acute kidney injury after cardiac surgery. Kidney Int 73:465–472
Fiehn O (2002) Metabolomics—the link between genotypes and phenotypes. Plant Mol Biol 48:155–171
Nicholson JK, Lindon JC, Holmes E (1999) ‘Metabonomics’: understanding the metabolic responses of living systems to pathophysiological stimuli via multivariate statistical analysis of biological NMR spectroscopic data. Xenobiotica 29:1181–1189
Dunn WB, Ellis DI (2005) Metabolomics: current analytical platforms and methodologies. Trends Anal Chem 24:285–294
Robertson DG (2005) Metabonomics in toxicology: a review. Toxicol Sci 85:809–822
Lenz EM, Wilson ID (2007) Analytical strategies in metabonomics. J Proteome Res 6:443–458
Lenz EM, Bright J, Knight R, Westwood FR, Davies D, Major H, Wilson ID (2005) Metabonomics with 1H-NMR spectroscopy and liquid chromatography-mass spectrometry applied to the investigation of metabolic changes caused by gentamicin-induced nephrotoxicity in the rat. Biomarkers 10:173–187
Devarajan P, Mishra J, Supavekin S, Patterson LT, Steven Potter S (2003) Gene expression in early ischemic renal injury: clues towards pathogenesis, biomarker discovery, and novel therapeutics. Mol Genet Metab 80:365–376
Mishra J, Ma Q, Prada A, Mitsnefes M, Zahedi K, Yang J, Barasch J, Devarajan P (2003) Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. J Am Soc Nephrol 4:2534–2543
Supavekin S, Zhang W, Kucherlapati R, Kaskel FJ, Moore LC, Devarajan P (2003) Differential gene expression following early renal ischemia/reperfusion. Kidney Int 63:1714–1724
Mishra J, Dent C, Tarabishi R, Mitsnefes MM, Ma Q, Kelly C, Ruff SM, Zahedi K, Shao M, Bean J, Mori K, Barasch J, Devarajan P (2005) Neutrophil gelatinase-associated lipocalin (NGAL) as a biomarker for acute renal injury after cardiac surgery. Lancet 365:1231–1238
Parikh CR, Abraham E, Ancukiewicz M, Edelstein CL (2005) Urine IL-18 is an early diagnostic marker for acute kidney injury and predicts mortality in the intensive care unit. J Am Soc Nephrol 16:3046–3052
Parikh CR, Mishra J, Thiessen-Philbrook H, Dursun B, Ma Q, Kelly C, Dent C, Devarajan P, Edelstein CL (2006) Urinary IL-18 is an early predictive biomarker of acute kidney injury after cardiac surgery. Kidney Int 70:199–203
Goldstein DS, Mezey E, Yamamoto T, Aneman A, Friberg P, Eisenhofer G (1995) Is there a third peripheral catecholaminergic system? Endogenous dopamine as an autocrine/paracrine substance derived from plasma DOPA and inactivated by conjugation. Hypertens Res 18:S93–S99
Lee MR (1993) Dopamine and the kidney: ten years on. Clin Sci 84:357–375
Wolfovitz E, Grossman E, Folio CJ, Keiser HR, Kopin IJ, Goldstein DS (1993) Derivation of urinary dopamine from plasma dihydroxyphenylalanine in humans. Clin Sci 84:549–557
Anggard E, Lewander T, Sjoquist B (1974) Determination of homovanillic acid turnover in man. Life Sci 15:111–122
Shimada M, Terazawa R, Kamiyama Y, Honma W, Nagata K, Yamazoe Y (2004) Unique properties of a renal sulfotransferase, St1d1, in dopamine metabolism. J Pharmacol Exp Ther 310:808–814
Sampaio-Maia B, Moreira-Rodrigues M, Pestana M (2006) Role of chronic inhibition of dopamine-metabolizing enzymes in the regulation of renal sodium and phosphate excretion in the rat remnant kidney. Nephron Physiol 103:14–24
Acknowledgments
Jinchun Sun was supported in part by appointments to the ORAU Research Program at the National Center for Toxicological Research administered by the Oak Ridge Associated Universities through an interagency agreement between the US Department of Energy and the US Food and Drug Administration. Waters LCT-Premiere, and MarkerLynx software, are part of a “beta test” material transfer agreement between Waters and the NCTR. The views presented in this article do not necessarily reflect those of the US Food and Drug Administration. This work was supported by National Institutes of Health grant RO1 DK075976 and a VA Merit and REAP Award to Dr. Didier Portilla. Dr. Devarajan is supported by grants from the National Institutes of Health/National Institute of Diabetes and Digestive and Kidney Diseases (RO1-DK53289, P50-DK52612, R21-DK070163).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beger, R.D., Holland, R.D., Sun, J. et al. Metabonomics of acute kidney injury in children after cardiac surgery. Pediatr Nephrol 23, 977–984 (2008). https://doi.org/10.1007/s00467-008-0756-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-008-0756-7