Abstract
Background
While endoscopic vacuum assisted closure (EVAC) therapy is a validated treatment for gastrointestinal leaks, its impact on long-term quality of life (QoL) is uncertain. The purpose of this study was to evaluate the impact of successful EVAC management on long-term QoL outcomes.
Methods
An institutional review board approved prospectively maintained database was retrospectively reviewed to identify patients undergoing treatment for gastrointestinal leaks between June 2012 and July 2022. The Short-Form 36 (SF-36) survey was used to assess QoL. Patients were contacted by telephone and sent the survey electronically. QoL outcomes between patients who underwent successful EVAC therapy and those who required conventional treatment (CT) were analyzed and compared.
Results
A total of 44 patients (17 EVAC; 27 CT) completed the survey and were included in our analysis. All included patients had foregut leaks with sleeve gastrectomy being the most common sentinel operation (n = 20). The mean time from the sentinel operation was 3.8 years and 4.8 years for the EVAC and CT groups, respectively. When evaluating long-term QoL, the EVAC group scored higher in all QoL domains when compared to the CT group with physical functioning (87.3 vs 69.3, p = 0.04), role limitations due to physical health (84.1 vs 45.7, p = 0.02), energy/fatigue (60.0 vs 40.9, p = 0.04), and social functioning (86.2 vs 64.1, p = 0.04) reaching statistical significance. Overall, patients who achieved organ preservation via successful EVAC therapy scored higher in all domains with role limitations due to physical health (p = 0.04) being statistically significant. In a multivariable regression analysis, increased age and a history of prior abdominal surgery at the time of the sentinel operation were patient characteristics that negatively impacted QoL outcomes.
Conclusion
Patients with gastrointestinal leaks successfully managed by EVAC therapy have better long-term QoL outcomes when compared to patients undergoing other treatments.
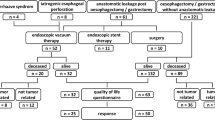
Graphical abstract



Similar content being viewed by others
References
McKinley SK, Dirks RC, Walsh D et al (2021) Surgical treatment of GERD: systematic review and meta-analysis. Surg Endosc 35(8):4095–4123. https://doi.org/10.1007/s00464-021-08358-5
Xie J, Vatsan MS, Gangemi A (2021) Laparoscopic versus robotic-assisted Heller myotomy for the treatment of achalasia: a systematic review with meta-analysis. Int J Med Robot Comput Assist Surg 17(4):e2253. https://doi.org/10.1002/rcs.2253
Sheetz KH, Claflin J, Dimick JB (2020) Trends in the adoption of robotic surgery for common surgical procedures. JAMA Netw Open 3(1):e18911. https://doi.org/10.1001/jamanetworkopen.2019.18911
Chao GF, Yang J, Thumma J et al (2021) Volume–outcome relationships for Roux-en-Y gastric bypass patients in the sleeve gastrectomy era. Surg Endosc 36(6):3884–3892. https://doi.org/10.1007/s00464-021-08705-6
Griffiths EA, Singh P, Evans RPT et al (2020) Risk factors and outcomes associated with anastomotic leaks following esophagectomy: a systematic review and meta-analysis. Dis Esophagus 33(3):doz089. https://doi.org/10.1093/dote/doz089
Gujjuri RR, Kamarajah SK, Markar SR (2021) Effect of anastomotic leaks on long-term survival after oesophagectomy for oesophageal cancer: systematic review and meta-analysis. Dis Esophagus 34(3):doaa085. https://doi.org/10.1093/dote/doaa085
Taleb S, Nedelcu M, Skalli M, Loureiro M, Nedelcu A, Nocca D (2021) The evolution of surgical treatment for chronic leak following sleeve. Surg Obes Relat Dis 17(2):278–283. https://doi.org/10.1016/j.soard.2020.10.008
Chouillard E, Chahine E, Schoucair N et al (2014) Roux-En-Y Fistulo-Jejunostomy as a salvage procedure in patients with post-sleeve gastrectomy fistula. Surg Endosc 28(6):1954–1960. https://doi.org/10.1007/s00464-014-3424-y
Mahmoud M, Maasher A, Al Hadad M, Salim E, Nimeri AA (2016) Laparoscopic Roux En Y esophago-jejunostomy for chronic leak/fistula after laparoscopic sleeve gastrectomy. Obes Surg 26(3):679–682. https://doi.org/10.1007/s11695-015-2018-7
Leeds SG, Kerlee KR, Fair L et al (2023) Esophagojejunostomy or fistulojejunostomy are safe salvage operations for bariatric surgery leaks. Foregut. https://doi.org/10.1177/26345161221145918
Chung Y, Park DG, Kim YJ (2021) Endoscopic management of staple line leak after bariatric surgery: surgeon’s perspective. Clin Endosc. https://doi.org/10.5946/ce.2020.298
Rogalski P, Swidnicka-Siergiejko A, Wasielica-Berger J et al (2021) Endoscopic management of leaks and fistulas after bariatric surgery: a systematic review and meta-analysis. Surg Endosc 35(3):1067–1087. https://doi.org/10.1007/s00464-020-07471-1
Smith ZL, Park KH, llano EM, et al (2019) Outcomes of endoscopic treatment of leaks and fistulae after sleeve gastrectomy: results from a large multicenter U.S. cohort. Surg Obes Relat Dis 15(6):850–855. https://doi.org/10.1016/j.soard.2019.04.009
de Moura DTH, de Moura EGH, Neto MG et al (2019) Outcomes of a novel bariatric stent in the management of sleeve gastrectomy leaks: a multicenter study. Surg Obes Relat Dis 15(8):1241–1251. https://doi.org/10.1016/j.soard.2019.05.022
Mencio MA, Ontiveros E, Burdick JS, Leeds SG (2018) Use of a novel technique to manage gastrointestinal leaks with endoluminal negative pressure: a single institution experience. Surg Endosc 32(7):3349–3356. https://doi.org/10.1007/s00464-018-6055-x
Leeds SG, Mencio M, Ontiveros E, Ward MA (2019) Endoluminal vacuum therapy: how i do it. J Gastrointest Surg 23(5):1037–1043. https://doi.org/10.1007/s11605-018-04082-z
Mann C, Berlth F, Tagkalos E, Hadzijusufovic E, Lang H, Grimminger P (2022) Endoscopic management of complications—endovacuum for management of anastomotic leakages: a narrative review. Ann Esophagus 5:15–15. https://doi.org/10.21037/aoe-21-16
Archid R, Bazerbachi F, Abu Dayyeh BK et al (2021) Endoscopic Negative Pressure Therapy (ENPT) is superior to stent therapy for staple line leak after sleeve gastrectomy: a single-center cohort study. Obes Surg 31(6):2511–2519. https://doi.org/10.1007/s11695-021-05287-z
Donatelli G, Spota A, Cereatti F et al (2021) Endoscopic internal drainage for the management of leak, fistula, and collection after sleeve gastrectomy: our experience in 617 consecutive patients. Surg Obes Relat Dis 17(8):1432–1439. https://doi.org/10.1016/j.soard.2021.03.013
Aziz M, Haghbin H, Sharma S et al (2021) Safety and effectiveness of endoluminal vacuum-assisted closure for esophageal defects: systematic review and meta-analysis. Endosc Int Open 9(9):E1371–E1380. https://doi.org/10.1055/a-1508-5947
Mandarino FV, Barchi A, D’Amico F et al (2023) Endoscopic Vacuum Therapy (EVT) versus Self-Expandable Metal Stent (SEMS) for anastomotic leaks after upper gastrointestinal surgery: systematic review and meta-analysis. Life 13(2):287. https://doi.org/10.3390/life13020287
Dhayat SA, Schacht R, Mennigen R et al (2019) Long-term quality of life assessment after successful endoscopic vacuum therapy of defects in the upper gastrointestinal tract quality of life after EVT. J Gastrointest Surg 23(2):280–287. https://doi.org/10.1007/s11605-018-4038-9
Heits N, Bernsmeier A, Reichert B et al (2018) Long-term quality of life after endovac-therapy in anastomotic leakages after esophagectomy. J Thorac Dis 10(1):228–240. https://doi.org/10.21037/jtd.2017.12.31
Farivar SS, Cunningham WE, Hays RD (2007) Correlated physical and mental health summary scores for the SF-36 and SF-12 Health Survey, V. 1. Health Qual Life Outcomes 5(1):1–8
Hopman WM, Berger C, Joseph L et al (2009) Health-related quality of life in Canadian adolescents and young adults: normative data using the SF-36. Can J Public Health 100:449–452
Ware J, Kosinski M, Keller S (1994) SF-36 physical and mental component summary measures: a user’s manual. The Health Institute, New England Medical Center, Boston
Ware JE Jr (2000) SF-36 health survey update. Spine 25(24):3130–3139
Taft C, Karlsson J, Sullivan M (2001) Do SF-36 summary component scores accurately summarize subscale scores? Qual Life Res 10(5):395–404. https://doi.org/10.1023/a:1012552211996
Schaheen L, Blackmon SH, Nason KS (2014) Optimal approach to the management of intrathoracic esophageal leak following esophagectomy: a systematic review. Am J Surg 208(4):536–543. https://doi.org/10.1016/j.amjsurg.2014.05.011
Egberts JH, Schniewind B, Bestmann B et al (2008) Impact of the site of anastomosis after oncologic esophagectomy on quality of life—a prospective, longitudinal outcome study. Ann Surg Oncol 15(2):566–575. https://doi.org/10.1245/s10434-007-9615-1
Seetahal S, Obirieze A, Cornwell EE, Fullum T, Tran D (2015) Open abdominal surgery: a risk factor for future laparoscopic surgery? Am J Surg 209(4):623–626. https://doi.org/10.1016/j.amjsurg.2014.12.017
Ghoneim MM, O’Hara MW (2016) Depression and postoperative complications: an overview. BMC Surg 16:5. https://doi.org/10.1186/s12893-016-0120-y
Massarweh NN, Legner VJ, Symons RG, McCormick WC, Flum DR (2009) Impact of advancing age on abdominal surgical outcomes. Arch Surg 144(12):1108–1114. https://doi.org/10.1001/archsurg.2009.204
Gajdos C, Kile D, Hawn MT, Finlayson E, Henderson WG, Robinson TN (2013) Advancing age and 30-day adverse outcomes after nonemergent general surgeries. J Am Geriatr Soc 61(9):1608–1614. https://doi.org/10.1111/jgs.12401
Molena D, Mungo B, Stem M, Feinberg RL, Lidor AO (2014) Outcomes of operations for benign foregut disease in elderly patients: a National Surgical Quality Improvement Program database analysis. Surgery 156(2):352–360. https://doi.org/10.1016/j.surg.2014.04.005
Baquero GA, Rich MW (2015) Perioperative care in older adults. J Geriatr Cardiol 12(5):465–469. https://doi.org/10.11909/j.issn.1671-5411.2015.05.018
Author information
Authors and Affiliations
Contributions
LF, MW, MV, RR, TM, BA, and SL contributed to study conception, study design, and data acquisition. GO performed data analysis and interpretation. LF and SL drafted the original manuscript. All authors provided final approval of the submitted version of the manuscript.
Corresponding author
Ethics declarations
Disclosures
Dr. Steven Leeds and Dr. Marc Ward are paid consultants for Boston Scientific. Dr. Lucas Fair, Meghana Vankina, Rashmeen Rana, Titus McGowan, Dr. Gerald Ogola, and Dr. Bola Aladegbami have no conflicts of interest or funding sources to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fair, L., Ward, M., Vankina, M. et al. Comparison of long-term quality of life outcomes between endoscopic vacuum therapy and other treatments for upper gastrointestinal leaks. Surg Endosc 37, 6538–6547 (2023). https://doi.org/10.1007/s00464-023-10181-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-023-10181-z