Abstract
Background
The coronavirus pandemic has caused a worldwide health crisis. Bariatric patients require extensive pre- and post-operative follow-up, which may be less feasible during public health social distancing mandates. We assessed the impact of the pandemic on the behaviors and weight loss outcomes of our pre- and post-operative bariatric patients.
Methods
A retrospective review of a prospectively maintained database identified patients who underwent either sleeve gastrectomy (SG) or Roux-en-Y gastric bypass (RYGB) at a single institution between March 2018 and May 2020. A cohort undergoing surgery within 12 months before the pandemic as well as a cohort undergoing a medically supervised diet prior to surgery was surveyed regarding pre- and post-COVID-19 lifestyle habits. Excess weight loss (EWL) outcomes from a group of pre-COVID surgical patients were compared to that of a group of post-COVID surgical patients. Primary outcome was whether the lockdown changed 1-year weight loss outcomes. Secondary outcome was whether patient lifestyle behaviors were changed during the pandemic.
Results
There was no difference in 1-year EWL between pre- and post-COVID SG patients (51.7% versus 55.9%, p = 0.35), or between pre- and post-COVID RYGB patients (88.9% versus 80.4%, p = 0.42). Pre-stay-at-home order, 91.8% endorsed physical activity compared to 80.3% post-stay-at-home order (p = 0.0025). Mean physical activity decreased from 4.2 h/week to 2.7 h/week after the stay-at-home order (p < 0.0001). Additionally, 41.3% reported worsened dietary habits post-stay-at-home order.
Conclusion
The COVID-19 pandemic has greatly impacted the behaviors of bariatric surgery patients. Despite deterioration of lifestyle habits, 1-year weight loss outcomes after bariatric surgery remained the same before and after the instatement of social distancing measures. In the short term, the biological effect of metabolic procedures may mask the effects of suboptimal diet and physical activity, but more studies are necessary to better assess the impact of COVID-19 on outcomes after bariatric surgery.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Obesity is a global pandemic with rates rapidly increasing in the US [1, 2]. This rise has contributed to increasing rates of chronic conditions, such as cardiovascular disease and metabolic syndrome [3, 4]. For those with body mass index (BMI) ≥ 40 or ≥ 35 with comorbidities, surgical weight loss should be considered [5]. Bariatric surgery is also the most effective method of weight reduction; mean weight loss is 20–30% at 3 years [6, 7]. This, in turn, can lead to improvement and remission of the associated medical issues [7,8,9,10]. Studies show that 30-day mortality is improved if weight loss is achieved prior to bariatric surgery; many patients undergo a medically supervised diet (MSD) to achieve this goal [11, 12].
The rise of a new pandemic, the novel coronavirus (SARS-CoV-2) 2019 (COVID-19), has caused a worldwide health and economic crisis. To limit contagion, much of the population has been more isolated, practicing social distancing measures. Following CMS guidelines, elective surgeries, including bariatric procedures, were put on hold, as were in-person visits in preparation for these elective surgeries [13]. Surgical obesity management, both pre- and post-operatively, has understandably been affected by this crisis. Patients are not able to receive required preoperative assessments, nor are they able to attend dietitian and medical weight loss appointments in-person. Post-operative care, including nutrition and metabolic management, has also transitioned to a virtual platform.
Beyond these practical clinical issues, social distancing has affected patient routines during COVID-19. Observations from the previous SARS epidemic as well as vacation/holiday-induced changes in usual daily habits show that isolation and routine change are associated with significant weight gain in adults [14,15,16]. Pre- and post-operative weight loss requires access to healthy foods, behavior modification, social and professional support, and physical activity, all of which may be difficult during a pandemic [17, 18]. In addition, the increased stress that comes with self-isolation can lead to emotional eating and binge-eating behavior [19, 20].
Taking these aspects of self-isolation during COVID-19 into account, we aim to assess how this pandemic has affected our pre- and post-operative bariatric patients by assessing behavioral changes as well as weight loss outcomes.
Materials and methods
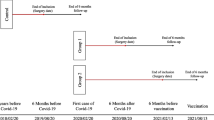
A retrospective review of a prospectively maintained database identified patients who underwent sleeve gastrectomy (SG) or Roux-en-Y gastric bypass (RYGB) between March 2018 and May 2020. The study was performed under the approval of an Institutional Review Board. Patient data included age, sex, Charlson Comorbidity Index (CCI), BMI at initial bariatric visit, and BMI at most recent clinic visit. 1-year excess weight loss (EWL) outcomes from a group of pre-COVID surgical patients (undergoing bariatric surgery between March 2018 and February 2019) was compared to that of a group of post-COVID surgical patients (undergoing bariatric surgery between June 2019 and May 2020).
Primary outcome was whether the lockdown changed 1-year weight loss outcomes. Secondary outcome was whether the lockdown changed patient lifestyle behaviors. Patients were excluded if they were awaiting laparoscopic band removal, undergoing MSD prior to a non-bariatric procedure, or treated with bariatric revision. Percent excess weight loss (EWL) was calculated using the following formula: (initial weight − current weight)/excess weight. Excess weight was defined as initial weight (at time of entry into the bariatric program) − ideal weight (corresponding to BMI 25).
A cohort of patients who underwent surgery during the pandemic between March 2019 and March 2020 were surveyed. Patients in the process of undergoing insurance-mandated medically supervised diets (MSD) within the same time frame as part of our bariatric center’s preoperative protocol were also surveyed. MSD durations ranged from 2 to 8 weeks, with the majority falling between 2 and 5 weeks. The survey for this study was hosted in Google Forms. Patients were given anonymized numbers prior to form entry and were contacted by phone. Survey assessments included: pre- and post-COVID-19 physical activity regimen and barriers to physical activity, as well as characterization of pre- and post-COVID-19 diet and food source. Data were also collected regarding pre- and post-COVID-19 drug and alcohol use in drinks per week, presence of new or worsening medical issues, and pre- and post-COVID-19 weight loss goals.
Continuous variables were analyzed using Student’s t test. Pearson χ2 test and Fisher’s exact test was used for categorical variables. All analyses were performed using R (Version 4.1.2, Vienna, Austria). All statistical tests were 2-sided with p < 0.05 considered to be statistically significant.
Results
We identified 138 patients undergoing either SG or RYGB. Mean patient age was 41.3 years, mean BMI at initial bariatric encounter was 46.9 kg/m2. Gender distribution included 80% female patients. There were no major differences in demographics between pre- and post-COVID SG or RYGB patients (Table 1). There was no difference in one-year EWL between pre- and post-COVID SG patients (51.7% versus 55.9%, p = 0.35), and there was no difference in 1-year EWL between pre- and post-COVID RYGB patients (88.9% versus 80.4%, p = 0.42) (Table 2).
Survey data: physical activity
A total of 184 patients were successfully contacted for the survey. Of these patients, 55 (29.9%) received SG, 24 (13%) received RYGB, and 91 (49.5%) were undergoing pre-operative MSD. Demographic data for surveyed patients are shown in Table 3. Revision bariatric surgery was performed on 4.3% of patients, while 3.3% were awaiting revision procedures. When evaluating their post-COVID-19 physical activity habits, 60.9% reported decreased physical activity, 12.5% noted increased physical activity, and 26.6% endorsed stable rates of physical activity (Table 4). Pre-stay-at-home order, the percentage of patients endorsing physical activity was 91.8% compared to 80.3% post-stay-at-home order (p = 0.0025). Mean physical activity decreased from an average of 4.2 h/week to 2.7 h/week after the stay-at-home order (p < 0.0001) (Table 5). The primary method of physical activity during COVID-19 was walking (136 [73.9%] patients). Prior to COVID-19, 48 (26.1%) patients were exercising at the gym; during COVID-19, no patients were. The most commonly cited barriers to physical activity were the stay-at-home order (65 patients), gym closure (54 patients), and inability due to a chronic medical issue (23 patients).
Survey data: diet, substance, and mental health
When patients reported their post-COVID-19 dietary habits, 41.3% were worsened, 16.3% were improved, and 42.4% were unchanged (Table 4). Of the 74 patients specifying how their diet had worsened, 26 (35.1%) reported increased intake of processed carbohydrates, 31 (41.9%) reported increased snacking, 15 (20.3%) reported a combination of the former two, and 2 (2.7%) had difficulty obtaining healthy food options due to isolation during COVID-19.
Thirty-eight patients endorsed alcohol use. Intake remained stable for 84.2% of these patients, with 8.2% endorsing increased intake and 7.6% noting decreased intake. Seven patients endorsed drug use, all of whom were using marijuana—each of these patients reported increased or stable patterns of use. During COVID-19, 37 (20.1%) patients reported worsening of chronic medical issues; 104 (56.6%) had increased anxiety and depression.
Discussion
Our study showed that despite adverse effects of the COVID-19 pandemic on self-reported lifestyle behaviors, the short-term weight loss outcomes after bariatric surgery were not different. These results were observed for both SG and RYGB. If one considers weight loss after surgical intervention to be mostly governed by voluntary modification of dietary and physical activity habits, this finding would seem surprising and paradoxical. If, however, the physiologic effects of metabolic surgery predominate, post-operative weight loss may, to a large degree, be independent of volitional behaviors, especially in the short-term when the entero-neurohormonal mechanisms are most potent. Indeed, it is now widely accepted that the effectiveness of surgical weight loss is mediated through pleiotropic hormonal mechanisms [21]. Likewise, post-surgical weight regain may also be influenced by genetic and physiologic factors. Investigators have shown that weight regain was not prevented by intense lifestyle interventions 4 years after gastric bypass [22]. By no means, however, should one leap to the conclusion that lifestyle optimization is unnecessary and unimportant.
Almost all aspects of life have fallen victim to the COVID-19 pandemic, and healthy lifestyle habits are no exception. In the present study, we aimed to evaluate self-reported dietary and physical activity behaviors in our bariatric patients, both before and after surgery, to underline the ubiquitous effects of social distancing and public health infection control measures for all patients moving through the surgical weight loss pathway. Over half of the patients noted a decrease in their weekly physical activity, and the percentage of patients ceasing all physical activity more than doubled during the pandemic, which can partially be explained by the most commonly identified barriers such as gym closure and orders to stay at home. It has been established that lack of physical activity is positively associated with increased weight regain after bariatric surgery, but this is more germane to longer term results [23]. Moreover, other studies using high volume physical activity interventions have failed to show any effect on weight after surgical interventions with gastric bypass and adjustable gastric banding, in both the short-term and long-term [24]. Interestingly, while observational studies suggest positive correlations between exercise and post-operative weight loss, intervention studies do not consistently support causality [25, 26].
COVID-19 also contributes to regression of healthy nutrition behaviors; over a third of our patients indicated that they had worsened eating habits, with snacking as one of the primary factors. Maladaptive eating and snacking have both been significantly associated with weight regain after bariatric surgery, but these observations and associations are more apparent with medium- and long-term outcomes [23, 27, 28]. The stress of changing routines and fear of falling ill, along with increased symptoms of depression and anxiety that we noted in our study, may be factors as well, as stress is associated with poor eating behaviors and increased snacking [29]. Depression in particular has been significantly associated with post-operative weight regain in bariatric patients [30].
One of the strengths of this study was the use of a comparator group that underwent bariatric surgery soon before the pandemic restrictions, with the same surgeons and multidisciplinary team, the main difference being a transition from face-to-face visits to the majority of postoperative care conducted via telemedicine. Another study revealed worse weight loss outcomes one year after surgery when post-pandemic patients were compared to pre-pandemic patients, but it was limited to only SG intervention in a European center where there may have been different COVID-19 public health regulations [31]. In our center, no changes were made to the follow-up schedule during the pandemic with the goal of seeing patients with the same frequency as the pre-COVID timeframe. While there was likely an adjustment period during the transition to remote visits, it is possible that the convenience of telemedicine made healthcare more accessible as patients and providers became accustomed to the new system. Although overall short-term weight loss outcomes were superior in our RYGB patients, there were no differences between the pre- and post-pandemic groups when separated by procedure type.
This study is limited by the fact that the data relied on patient perception and recall, which introduces a number of potential biases. It is unlikely that the survey biases differ significantly from in-clinic patient reporting, though remote patients may have tended to under-report negative outcomes. The pandemic also affected patients to different extents and different ways, which can lead to a heterogenous data set. Finally, there was some difficulty in reaching patients for survey via the telephone.
Further investigation should examine bariatric patients’ weight status at extended time points to assess whether weight loss differs in the medium- or long-term, although the pandemic will likely confer less impact on lifestyle behaviors as public health restrictions relax. In addition, change in weight-loss habits and comorbidities should be assessed prospectively and more systematically to reduce the risk of recall and social desirability bias. Knowledge and data regarding the impact of lifestyle support and interventions on weight loss and weight regain after bariatric surgery may better inform how best to allocate resources for patients at various post-operative time points during possible future COVID-19 surges.
Conclusion
During the COVID-19 pandemic, public health and social distancing mandates adversely affected patients’ healthy behaviors as they progressed through the bariatric surgery path. Despite this deterioration of lifestyle habits, weight loss at 1 year after bariatric surgery was not different before and after social distancing measures took hold. In the short term, the biological effect of metabolic procedures may mask the effects of suboptimal diet and physical activity, but more studies are necessary to better assess the impact of COVID-19 on outcomes after bariatric surgery.
References
Tremmel M, Gerdtham UG, Nilsson PM, Saha S (2017) Economic burden of obesity: a systematic literature review. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph14040435
Seidell JC, Halberstadt J (2015) The global burden of obesity and the challenges of prevention. Ann Nutr Metab 66(Suppl 2):7–12. https://doi.org/10.1159/000375143
Hales CM, Carroll MD, Fryar CD, Ogden CL (2020) Prevalence of obesity and severe obesity among adults: United States, 2017–2018. NCHS Data Brief 360:1–8
Vest AR, Heneghan HM, Schauer PR, Young JB (2013) Surgical management of obesity and the relationship to cardiovascular disease. Circulation 127(8):945–959. https://doi.org/10.1161/circulationaha.112.103275
NIH Conference (1991) Gastrointestinal surgery for severe obesity. Consensus Development Conference Panel. Ann Intern Med 115(12):956–961
Trastulli S, Desiderio J, Guarino S, Cirocchi R, Scalercio V, Noya G, Parisi A (2013) Laparoscopic sleeve gastrectomy compared with other bariatric surgical procedures: a systematic review of randomized trials. Surg Obes Relat Dis 9(5):816–829. https://doi.org/10.1016/j.soard.2013.05.007
Ikramuddin S, Korner J, Lee WJ, Thomas AJ, Connett JE, Bantle JP, Leslie DB, Wang Q, Inabnet WB 3rd, Jeffery RW, Chong K, Chuang LM, Jensen MD, Vella A, Ahmed L, Belani K, Billington CJ (2018) Lifestyle intervention and medical management with vs without Roux-en-Y gastric bypass and control of hemoglobin A1c, LDL cholesterol, and systolic blood pressure at 5 years in the diabetes surgery study. JAMA 319(3):266–278. https://doi.org/10.1001/jama.2017.20813
Ribaric G, Buchwald JN, McGlennon TW (2014) Diabetes and weight in comparative studies of bariatric surgery vs conventional medical therapy: a systematic review and meta-analysis. Obes Surg 24(3):437–455. https://doi.org/10.1007/s11695-013-1160-3
Schauer PR, Bhatt DL, Kirwan JP, Wolski K, Aminian A, Brethauer SA, Navaneethan SD, Singh RP, Pothier CE, Nissen SE, Kashyap SR (2017) Bariatric surgery versus intensive medical therapy for diabetes - 5-year outcomes. N Engl J Med 376(7):641–651. https://doi.org/10.1056/NEJMoa1600869
Zhou K, Wolski K, Malin SK, Aminian A, Schauer PR, Bhatt DL, Kashyap SR (2019) Impact of weight loss trajectory following randomization to bariatric surgery on long-term diabetes glycemic and cardiometabolic parameters. Endocr Pract 25(6):572–579. https://doi.org/10.4158/ep-2018-0522
Sun Y, Liu B, Smith JK, Correia MLG, Jones DL, Zhu Z, Taiwo A, Morselli LL, Robinson K, Hart AA, Snetselaar LG, Bao W (2020) Association of preoperative body weight and weight loss with risk of death after bariatric surgery. JAMA Netw Open. https://doi.org/10.1001/jamanetworkopen.2020.4803
Tarnoff M, Kaplan LM, Shikora S (2008) An evidenced-based assessment of preoperative weight loss in bariatric surgery. Obes Surg 18(9):1059–1061. https://doi.org/10.1007/s11695-008-9603-y
Siddiqui S (2020) CMS Adult elective surgery and procedures recommendations. Cent medicare medicaid Serv. https://www.cms.gov/files/document/covid-elective-surgery-recommendations.pdf
Bhutani S, Cooper JA (2020) COVID-19-related home confinement in adults: weight gain risks and opportunities. Obesity (Silver Spring) 28(9):1576–1577. https://doi.org/10.1002/oby.22904
Cooper JA, Tokar T (2016) A prospective study on vacation weight gain in adults. Physiol Behav 156:43–47. https://doi.org/10.1016/j.physbeh.2015.12.028
Yanovski JA, Yanovski SZ, Sovik KN, Nguyen TT, O’Neil PM, Sebring NG (2000) A prospective study of holiday weight gain. N Engl J Med 342(12):861–867. https://doi.org/10.1056/nejm200003233421206
Papalazarou A, Yannakoulia M, Kavouras SA, Komesidou V, Dimitriadis G, Papakonstantinou A, Sidossis LS (2010) Lifestyle intervention favorably affects weight loss and maintenance following obesity surgery. Obesity (Silver Spring) 18(7):1348–1353. https://doi.org/10.1038/oby.2009.346
Nouh F, Elfagi S, Omar M (2020) Corona virus: the Paradox between Food Insecurity and Weight Gain. vol 2. East African Scholars Publisher, EAS J Nutr Food Sci
Sockalingam S, Leung SE, Cassin SE (2020) The impact of coronavirus disease 2019 on bariatric surgery: redefining psychosocial care. Obesity (Silver Spring) 28(6):1010–1012. https://doi.org/10.1002/oby.22836
Cotter EW, Kelly NR (2018) Stress-related eating, mindfulness, and obesity. Health Psychol 37(6):516–525. https://doi.org/10.1037/hea0000614
Evers SS, Sandoval DA, Seeley RJ (2017) The physiology and molecular underpinnings of the effects of bariatric surgery on obesity and diabetes. Annu Rev Physiol 79:313–334. https://doi.org/10.1146/annurev-physiol-022516-034423
Hanvold SE, Vinknes KJ, Løken EB, Hjartåker A, Klungsøyr O, Birkeland E, Risstad H, Gulseth HL, Refsum H, Aas AM (2019) Does lifestyle intervention after gastric bypass surgery prevent weight regain? A randomized clinical trial. Obes Surg 29(11):3419–3431. https://doi.org/10.1007/s11695-019-04109-7
Livhits M, Mercado C, Yermilov I, Parikh JA, Dutson E, Mehran A, Ko CY, Gibbons MM (2011) Patient behaviors associated with weight regain after laparoscopic gastric bypass. Obes Res Clin Pract 5(3):e169-266. https://doi.org/10.1016/j.orcp.2011.03.004
Shah M, Snell PG, Rao S, Adams-Huet B, Quittner C, Livingston EH, Garg A (2011) High-volume exercise program in obese bariatric surgery patients: a randomized, controlled trial. Obesity (Silver Spring) 19(9):1826–1834. https://doi.org/10.1038/oby.2011.172
Egberts K, Brown WA, Brennan L, O’Brien PE (2012) Does exercise improve weight loss after bariatric surgery? A systematic review. Obes Surg 22(2):335–341. https://doi.org/10.1007/s11695-011-0544-5
Kalarchian MA, Marcus MD, Courcoulas AP, Cheng Y, Levine MD, Josbeno D (2012) Optimizing long-term weight control after bariatric surgery: a pilot study. Surg Obes Relat Dis 8(6):710–715. https://doi.org/10.1016/j.soard.2011.04.231
Conceição E, Mitchell JE, Vaz AR, Bastos AP, Ramalho S, Silva C, Cao L, Brandão I, Machado PP (2014) The presence of maladaptive eating behaviors after bariatric surgery in a cross sectional study: importance of picking or nibbling on weight regain. Eat Behav 15(4):558–562. https://doi.org/10.1016/j.eatbeh.2014.08.010
Sarwer DB, Wadden TA, Moore RH, Baker AW, Gibbons LM, Raper SE, Williams NN (2008) Preoperative eating behavior, postoperative dietary adherence, and weight loss after gastric bypass surgery. Surg Obes Relat Dis 4(5):640–646. https://doi.org/10.1016/j.soard.2008.04.013
O’Connor DB, Jones F, Conner M, McMillan B, Ferguson E (2008) Effects of daily hassles and eating style on eating behavior. Health Psychol 27(1s):S20-31. https://doi.org/10.1037/0278-6133.27.1.s20
Yanos BR, Saules KK, Schuh LM, Sogg S (2015) Predictors of lowest weight and long-term weight regain among Roux-en-Y gastric bypass patients. Obes Surg 25(8):1364–1370. https://doi.org/10.1007/s11695-014-1536-z
El Moussaoui I, Navez J, El Moussaoui K, Barea-Fernandez M, Schaeken A, Closset J (2021) Impact of COVID-19 lockdown on short-term results after laparoscopic sleeve gastrectomy. Obes Surg 31(6):2614–2618. https://doi.org/10.1007/s11695-021-05283-3
Funding
No funding information to disclose for this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Jacobsen receives a teaching honorarium from Gore Medical. Dr. Grunvald has received consulting honararia for Novo Nordisk, Currax Pharmaceuticals, and Gelesis Inc. Dr. Sandler is a consultant for Intuitive Surgical and Boston Scientific. Dr. Horgan is a consultant for Intuitive Surgical, Alume Biosciences, Stryker Corporation, and Fortimedix Surgical. Drs. Huang, Blitzer, Lee, Broderick, Li, and Cheverie have no relevant conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Huang, E.Y., Grunvald, E., Blitzer, R.R. et al. Despite regression of healthy lifestyle habits, weight loss after bariatric surgery is not affected during the COVID-19 pandemic. Surg Endosc 37, 607–612 (2023). https://doi.org/10.1007/s00464-022-09356-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09356-x