Abstract
Background
Interval appendectomy or non-operative management is commonly performed for complicated appendicitis in adult patients. However, these treatments are still controversial because the incidence rate of appendiceal tumors recognized after interval appendectomy is reportedly higher than that after emergency appendectomy. Thus, this study aimed to compare the appendiceal tumor rates between uncomplicated and complicated appendicitis.
Methods
This study was a retrospective review of patients with appendicitis who underwent surgical removal at a single institution over 7.5 years. The primary objective was the comparison of the incidence rate of appendiceal tumors using propensity score matching, and the secondary objective was the same comparison among older patients, defined as patients aged ≥ 60 years.
Results
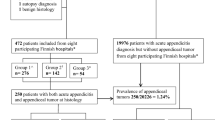
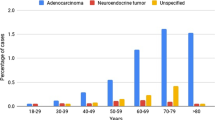
A total of 1277 patients were included. Of these patients, 297 (23.3%) were preoperatively diagnosed with complicated appendicitis. Moreover, 22 (1.7%) patients, including 14 cases of complicated appendicitis and 8 cases of uncomplicated appendicitis, were diagnosed with appendiceal tumors based on pathological examination. No significant difference was found in the incidence rate of appendiceal tumors between the two groups after matching for patients’ background, including age, sex, and history of appendicitis by propensity score matching (P = 0.073). However, among patients aged ≥ 60 years, the incidence of appendiceal tumors was significantly higher in complicated than in uncomplicated appendicitis (P = 0.006).
Conclusions
Although the overall risk of appendiceal tumors did not differ between complicated and uncomplicated appendicitis when analyzed by the propensity score matching, in older patients aged ≥ 60 years, the risk increased among those with complicated appendicitis. Therefore, although the incidence is low, complicated appendicitis, particularly, among older patients, should be examined carefully and be performed IA when unusual findings exist.
Similar content being viewed by others
References
Connor SJ, Hanna GB, Frizelle FA (1998) Appendiceal tumors: retrospective clinicopathologic analysis of appendiceal tumors from 7,970 appendectomies. Dis Colon Rectum 41:75–80
Murphy EM, Farquharson SM, Moran BJ (2006) Management of an unexpected appendiceal neoplasm. Br J Surg 93:783–792
Bolmers MDM, de Jonge J, van Rossem CC, van Geloven AAW, Bemelman WA, Snapshot Appendicitis Collaborative Study group (2020) Appendicular neoplasms and consequences in patients undergoing surgery for suspected acute appendicitis. Int J Colorectal Dis 35:2065–2071
Wright GP, Mater ME, Carroll JT, Choy JS, Chung MH (2015) Is there truly an oncologic indication for interval appendectomy? Am J Surg 209:442–446
Teixeira FJR Jr, Couto Netto SDD, Akaishi EH, Utiyama EM, Menegozzo CAM, Rocha MC (2017) Acute appendicitis, inflammatory appendiceal mass and the risk of a hidden malignant tumor: a systematic review of the literature. World J Emerg Surg 9(12):12
Bucher P, Mathe Z, Demirag A, Morel P (2004) Appendix tumors in the era of laparoscopic appendectomy. Surg Endosc 18:1063–1066
Furman MJ, Cahan M, Cohen P, Lambert LA (2013) Increased risk of mucinous neoplasm of the appendix in adults undergoing interval appendectomy. JAMA Surg 148:703–706
Hayes D, Reiter S, Hagen E, Lucas G, Chu I, Muñiz T, Martinez R (2021) Is interval appendectomy really needed? A closer look at neoplasm rates in adult patients undergoing interval appendectomy after complicated appendicitis. Surg Endosc 35:3855–3860
Lietzén E, Grönroos JM, Mecklin JP, Leppäniemi A, Nordström P, Rautio T, Rantanen T, Sand J, Paajanen H, Kaljonen A, Salminen P (2019) Appendiceal neoplasm risk associated with complicated acute appendicitis-a population based study. Int J Colorectal Dis 34:39–46
Carpenter SG, Chapital AB, Merritt MV, Johnson DJ (2012) Increased risk of neoplasm in appendicitis treated with interval appendectomy: single-institution experience and literature review. Am Surg 78:339–343
Fournier K, Rafeeq S, Taggart M, Kanaby P, Ning J, Chen HC, Overman M, Raghav K, Eng C, Mansfield P, Royal R (2017) Low-grade appendiceal mucinous neoplasm of uncertain malignant potential (LAMN-UMP): prognostic factors and implications for treatment and follow-up. Ann Surg Oncol 24:187–193
Klag T, Wehkamp J, Bösmüller H, Falch C, Johannink J, Malek NP, Kirschniak A, Goetz M (2017) Low-grade appendiceal mucinous neoplasm (LAMN) - 3-year endoscopic follow-up underlines benign course of LAMN type 1. Z Gastroenterol 55:149–152
Rymer B, Forsythe RO, Husada G (2015) Mucocoele and mucinous tumours of the appendix: a review of the literature. Int J Surg 18:132–135
Bennett GL, Tanpitukpongse TP, Macari M, Cho KC, Babb JS (2009) CT diagnosis of mucocele of the appendix in patients with acute appendicitis. AJR Am J Roentgenol 192:W103–W110
Van Hooser A, Williams TR, Myers DT (2018) Mucinous appendiceal neoplasms: pathologic classification, clinical implications, imaging spectrum and mimics. Abdom Radiol (NY) 43:2913–2922
Acknowledgements
Not applicable
Funding
Drs. Takuya Sugimoto, Yasutomo Nagasue, Eiji Tanaka, and Hiroshi Yokomizo have no conflict of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Takuya Sugimoto, Yasutomo Nagasue, Eiji Tanaka, and Hiroshi Yokomizo have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sugimoto, T., Nagasue, Y., Tanaka, E. et al. Comparison of the risk of appendiceal tumors in uncomplicated and complicated appendicitis. Surg Endosc 36, 8107–8111 (2022). https://doi.org/10.1007/s00464-022-09246-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09246-2