Abstract
Background
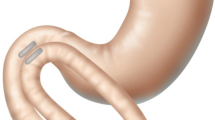
Current standard of care for creation of small bowel anastomoses after a loop ileostomy reversal includes the use of stapler devices and sutures. Compression anastomosis devices have been used for decades, aimed toward improved outcomes with a “staple free” & “suture free” anastomosis. The self-forming magnet (SFM) device is a type of compression anastomosis device used to safely and effectively create an end-to-end small bowel anastomosis without the localized inflammatory response seen with sutures or staples, as no foreign bodies are left behind.
Methods
A Good Laboratory Practice preclinical study using a porcine model to evaluate creating an in vivo anastomosis via magnetic compression between two segments of small bowel (jejunum or ileum) was performed. Magnetic anastomoses were compared to stapled and handsewn anastomoses. Six animals were used for the magnetic anastomosis and eight for the two control groups for a total of 14 subjects.
Results
Mean creation times were 17.1 min (SD 6.06) for the SFM group, 10.3 min (SD 6.55, CI 95%) for the stapled anastomosis group, and 28.3 min (SD 2.63, CI 95%) for the suture anastomosis group, with a statistically significant difference among groups (p < 0.0021). All evaluated SFM anastomosis, stapled anastomosis, and handsewn anastomosis underwent a burst test with a pressure of 1.3 PSI. All six magnets used for anastomoses were naturally expelled. The range of days to expel magnets was 10–17 days. Intestinal anastomoses using magnets had considerably less residual scarring and intestinal distortion than anastomoses done with either suture or staples.
Conclusion
This preclinical study documents the safety and efficacy of creating end-to-end small bowel anastomoses after ileostomy takedown using a magnetic compression device. The result is an anastomosis free of foreign objects with less inflammation, scarring, distortion, and mural thickening than seen in sutured or stapled anastomoses.














Similar content being viewed by others
References
Choy PYG, Bissett IP, Docherty JG, Parry BR, Merrie A, Fitzgerald A (2011) Stapled versus handsewn methods for ileocolic anastomoses. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD004320.pub3
Katz S, Izhar M, Mirelman D (1981) Bacterial adherence to surgical sutures. A possible factor in suture induced infection. Ann Surg 194(1):35–41. https://doi.org/10.1097/00000658-198107000-00007
Ballantyne GH (1984) The experimental basis of intestinal suturing—effect of surgical technique, inflammation, and infection on enteric wound healing. Dis Colon Rectum 27(1):61–71. https://doi.org/10.1007/BF02554084
Telem DA, Chin EH, Nguyen SQ, Divino CM (2010) Risk factors for anastomotic leak following colorectal surgery: a case-control study. Arch Surg 145(4):371–376. https://doi.org/10.1001/archsurg.2010.40
Wullstein C, Gross E (2000) Compression anastomosis (AKA-2) in colorectal surgery: results in 442 consecutive patients. Br J Surg 87(8):1071–1075. https://doi.org/10.1046/j.1365-2168.2000.01489.x
An Y, Zhang Y, Liu H et al (2018) Gastrojejunal anastomosis in rats using the magnetic compression technique. Sci Rep 8(1):1–9. https://doi.org/10.1038/s41598-018-30075-8
Gonzalez LM, Moeser AJ, Blikslager AT (2015) Porcine models of digestive disease: the future of large animal translational research. Transl Res 166(1):12–27. https://doi.org/10.1016/j.trsl.2015.01.004
Kopelman D, Hatoum OA, Kimmel B et al (2007) Compression gastrointestinal anastomosis. Expert Rev Med Devices 4(6):821–828. https://doi.org/10.1586/17434440.4.6.821
Graves CE, Co C, Hsi RS et al (2017) Magnetic compression anastomosis (Magnamosis): first-in-human trial. J Am Coll Surg 225(5):676-681.e1. https://doi.org/10.1016/j.jamcollsurg.2017.07.1062
Funding
This study was funded by GI Windows.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Askenasy and Dr. Baldwin are consultants for GI Windows. Dr. Ryou is a consultant for Boston Scientific, Medtronic, Olympus, Cook and Fujifilm. He is the Chief Medical Officer and co-founder of GI Windows. Dr. Thompson is a consultant for Apollo Endosurgery, Boston Scientific, Covidien/Medtronic, Enterasense Ltd, Fractyl, GI Dynamics, Lumendi and USGI Medical. Received research support from Aspire Bariatrics and USGI medical. A research grant from ERBE, FujiFilm, Lumendi and USGI Medical. He is a general partner at BlueFlame Healthcare, serves as a board member at EnVision Endoscopy and an advisory board member at USGI Medical and Fractyl. He should say has ownership interest at GI Windows. The facilities, animals, and OR cost were paid by GI Windows. Both authors/surgeons Ana Sofia Ore and Evangelos Messaris (first and senior author) do not have any conflict of interest and are not paid consultants. Dr. Ore and Dr. Messaris have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ore, A.S., Askenasy, E., Ryou, M. et al. Evaluation of sutureless anastomosis after ileostomy takedown using the self-forming magnet anastomosis system in a porcine model. Surg Endosc 36, 7664–7672 (2022). https://doi.org/10.1007/s00464-022-09082-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09082-4