Abstract
Background
Laparoscopic proximal gastrectomy (LPG) is increasingly preferred for operative management of early gastric cancer, although there is no consensus on a standard reconstruction method after resection. Two popular methods used after LPG are double tract reconstruction (DTR) and double flap technique (DFT). This study assessed comprehensive clinical outcomes including quality of life (QoL) and body composition change 1 year after DFT and DTR.
Methods
We retrospectively reviewed prospectively collected data from 51 to 18 patients who underwent DTR and DFT, respectively, between September 2014 and December 2018. Short-term surgical outcomes, presence of reflux esophagitis, nutritional supplementation, medications, nutritional status (laboratory results and body composition analysis), and QoL measured preoperatively and at 1 year postoperatively were compared between both groups.
Results
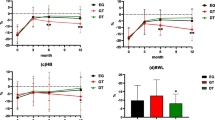
Both groups did not differ significantly in clinicopathological characteristics. The DFT as compared to the DTR group required significantly longer time for anastomosis (79.4 vs. 60.9 min, p < 0.001) and use of fewer staplers (3.39 vs. 6.86, p < 0.001). While the presence of endoscopic reflux esophagitis and iron/vitamin B12 replacement were comparable, the DTR group showed a higher tendency of taking anti-reflux medications for reflux symptoms (DTR: 13.7% vs. DFT: 0.0%, p = 0.177). The DTR group lost significantly more weight (p = 0.038) and body fat (p = 0.009). QoL analysis showed significant deterioration in diarrhea, eating restriction, and taste problems in both groups (DTR group: p = 0.008, p < 0.001, p = 0.010, respectively, and DFT group: p = 0.017, p = 0.024, p = 0.034, respectively). However, only the DTR group showed significant deterioration in physical function (p = 0.009), role function (p = 0.033), nausea/vomiting (p = 0.041), appetite loss (p = 0.019), dysphagia (p = 0.001), pain (p = 0.025), and body image (p = 0.004).
Conclusions
Despite requiring a longer anastomosis time, performing DFT after LPG was shown to be an ideal reconstruction method in terms of better 1-year QoL and nutritional outcome. Further larger studies over longer postoperative periods are necessary to confirm our findings.






Similar content being viewed by others
References
Information Committee of Korean Gastric Cancer Association (2016) Korean gastric cancer association nationwide survey on gastric cancer in 2014. J Gastric Cancer 16:131–140
Tanioka T, Waratchanont R, Fukuyo R, Saito T, Umebayashi Y, Kanemoto E, Kobayashi K, Nakagawa M, Inokuchi M (2020) Surgical and nutritional outcomes of laparoscopic proximal gastrectomy versus total gastrectomy: a meta-analysis. Surg Endosc 34:1061–1069
Kamikawa Y, Kobayashi T, Kamiyama S, Satomoto K (2001) A new procedure of esophagogastrostomy to prevent reflux following proximal gastrectomy (in Japanese). Shoukakigeka 24:1053–1060
Shaibu Z, Chen Z, Mzee SAS, Theophilus A, Danbala IA (2020) Effects of reconstruction techniques after proximal gastrectomy: a systematic review and meta-analysis. World J Surg Oncol 18:171
Hayami M, Hiki N, Nunobe S, Mine S, Ohashi M, Kumagai K, Ida S, Watanabe M, Sano T, Yamaguchi T (2017) Clinical outcomes and evaluation of laparoscopic proximal gastrectomy with double-flap technique for early gastric cancer in the upper third of the stomach. Ann Surg Oncol 24:1635–1642
Jung DH, Lee Y, Kim DW, Park YS, Ahn SH, Park DJ, Kim HH (2017) Laparoscopic proximal gastrectomy with double tract reconstruction is superior to laparoscopic total gastrectomy for proximal early gastric cancer. Surg Endosc 31:3961–3969
Son MW, Kim YJ, Jeong GA, Cho GS, Lee MS (2014) Long-term outcomes of proximal gastrectomy versus total gastrectomy for upper-third gastric cancer. J Gastric Cancer 14:246–251
Nomura E, Lee SW, Kawai M, Yamazaki M, Nabeshima K, Nakamura K, Uchiyama K (2014) Functional outcomes by reconstruction technique following laparoscopic proximal gastrectomy for gastric cancer: double tract versus jejunal interposition. World J Surg Oncol 12:20
Washington K (2010) 7th edition of the AJCC cancer staging manual: stomach. Ann Surg Oncol 17:3077–3079
Japanese Gastric Cancer Association (2017) Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer 20:1–19
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Lundell LR, Dent J, Bennett JR, Blum AL, Armstrong D, Galmiche JP, Johnson F, Hongo M, Richter JE, Spechler SJ, Tytgat GN, Wallin L (1999) Endoscopic assessment of oesophagitis: clinical and functional correlates and further validation of the Los Angeles classification. Gut 45:172–180
Fayers PM, Aaronson NK, Bjordal K, Groenvold M, Curran D, Bottomley A (2001) The EORTC QLQ-C30 scoring manual, 3rd edn. EORTC, Brussels
Uyama I, Ogiwara H, Takahara T, Kikuchi K, Iida S (1995) Laparoscopic and minilaparotomy proximal gastrectomy and esophagogastrostomy: technique and case report. Surg Laparosc Endosc 5:487–491
Kano Y, Ohashi M, Ida S, Kumagai K, Nunobe S, Sano T, Hiki N (2019) Oncological feasibility of laparoscopic subtotal gastrectomy compared with laparoscopic proximal or total gastrectomy for cT1N0M0 gastric cancer in the upper gastric body. Gastric Cancer 22:1060–1068
Yura M, Yoshikawa T, Otsuki S, Yamagata Y, Morita S, Katai H, Nishida T, Yoshiaki T (2019) Oncological safety of proximal gastrectomy for T2/T3 proximal gastric cancer. Gastric Cancer 22:1029–1035
Xu Y, Gao J, Wang Y, Tan Y, Xi C, Ye N, Wu D, Xu X (2020) Validation of a novel reconstruction method of laparoscopic gastrectomy for proximal early gastric cancer: a systematic review and meta-analysis. World J Surg Oncol 18:214
Guideline Committee of the Korean Gastric Cancer Association, Development Working Group & Review Panel (2019) Korean practice guideline for gastric cancer 2018: an evidence-based, multi-disciplinary approach. J Gastric Cancer 19:1–48
Japanese Gastric Cancer Association (2021) Japanese gastric cancer treatment guidelines 2018 (5th edition). Gastric Cancer 24:1–21
Kim HH, Han SU, Kim MC, Kim W, Lee HJ, Ryu SW, Cho GS, Kim CY, Yang HK, Park DJ, Song KY, Lee SI, Ryu SY, Lee JH, Hyung WH, Korean Laparoendoscopic Gastrointestinal Surgery Study (KLASS) Group (2019) Effect of laparoscopic distal gastrectomy vs open distal gastrectomy on long-term survival among patients with stage I gastric cancer: the KLASS-01 randomized clinical trial. JAMA Oncol 5:506–513
Nozaki I, Kurita A, Nasu J, Kubo Y, Aogi K, Tanada M, Takashima S (2007) Higher incidence of gastric remnant cancer after proximal than distal gastrectomy. Hepatogastroenterology 54:1604–1608
Ohyama S, Tokunaga M, Hiki N, Fukunaga T, Fujisaki J, Seto Y, Yamaguchi T (2009) A clinicopathological study of gastric stump carcinoma following proximal gastrectomy. Gastric Cancer 12:88–94
Morgagni P, Gardini A, Marrelli D, Vittimberga G, Marchet A, de Manzoni G, Di Cosmo MA, Rossi GM, Garcea D, Roviello F, Italian Research Group for Gastric Cancer (2015) Gastric stump carcinoma after distal subtotal gastrectomy for early gastric cancer: experience of 541 patients with long-term follow-up. Am J Surg 209:1063–1068
Nozaki I, Hato S, Kobatake T, Ohta K, Kubo Y, Nishimura R, Kurita A (2014) Incidence of metachronous gastric cancer in the remnant stomach after synchronous multiple cancer surgery. Gastric Cancer 17:61–66
Climent M, Munarriz M, Blazeby JM, Dorcaratto D, Ramón JM, Carrera MJ, Fontane L, Grande L, Pera M (2017) Weight loss and quality of life in patients surviving 2 years after gastric cancer resection. Eur J Surg Oncol 43:1337–1343
Park YS, Park DJ, Lee Y, Park KB, Min SH, Ahn SH, Kim HH (2018) Prognostic roles of perioperative body mass index and weight loss in the long-term survival of gastric cancer patients. Cancer Epidemiol Biomark Prev 27:955–962
Kosuga T, Ichikawa D, Komatsu S, Okamoto K, Konishi H, Shiozaki A, Fujiwara H, Otsuji E (2015) Feasibility and nutritional benefits of laparoscopic proximal gastrectomy for early gastric cancer in the upper stomach. Ann Surg Oncol 22:S929–S935
Ahn SH, Jung DH, Son SY, Lee CM, Park DJ, Kim HH (2014) Laparoscopic double-tract proximal gastrectomy for proximal early gastric cancer. Gastric Cancer 17:562–570
Fujimoto D, Taniguchi K, Kobayashi H (2020) Double-tract reconstruction designed to allow more food flow to the remnant stomach after laparoscopic proximal gastrectomy. World J Surg 44:2728–2735
Takiguchi N, Takahashi M, Ikeda M, Inagawa S, Ueda S, Nobuoka T, Ota M, Iwasaki Y, Uchida N, Kodera Y, Nakada K (2015) Long-term quality-of-life comparison of total gastrectomy and proximal gastrectomy by postgastrectomy syndrome assessment scale (PGSAS-45): a nationwide multi-institutional study. Gastric Cancer 18:407–416
Yabusaki H, Kodera Y, Fukushima N, Hiki N, Kinami S, Yoshida M, Aoyagi K, Ota S, Hata H, Noro H, Oshio A, Nakada K (2020) Comparison of postoperative quality of life among three different reconstruction methods after proximal gastrectomy: insights from the PGSAS study. World J Surg 44:3433–3440
Kuroda S, Choda Y, Otsuka S, Ueyama S, Tanaka N, Muraoka A, Hato S, Kimura T, Tanakaya K, Kikuchi S, Tanabe S, Noma K, Nishizaki M, Kagawa S, Shirakawa Y, Kamikawa Y, Fujiwara T (2019) Multicenter retrospective study to evaluate the efficacy and safety of the double-flap technique as antireflux esophagogastrostomy after proximal gastrectomy (rD-FLAP study). Ann Gastroenterol Surg 3:96–103
Funding
The authors declare they have no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Byunghyuk Yu, Ki Bum Park, Ji Yeon Park, Seung Soo Lee, Oh Kyoung Kwon, Ho Young Chung, and Yoon Jin Hwang have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Yu, B., Park, K.B., Park, J.Y. et al. Double tract reconstruction versus double flap technique: short-term clinical outcomes after laparoscopic proximal gastrectomy for early gastric cancer. Surg Endosc 36, 5243–5256 (2022). https://doi.org/10.1007/s00464-021-08902-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-021-08902-3