Abstract
Background
Curative resection of hilar cholangiocarcinoma (HC) is typically carried out using open surgery. In the present study, we examined the safety (postoperative complication) and effectiveness (resection margin status and patient survival) of minimally invasive surgery (MIS) for HC.
Methods
This retrospective analysis included 158 patients receiving MIS for HC at 10 participating centers between December 2013 and November 2019. Patient demographics, surgical outcomes, and oncological outcomes were retrospectively analyzed.
Results
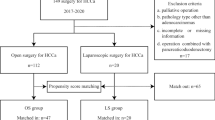
Clinical information obtained from 10 different clinical centers did not show any evident cohort-bias clustering. One hundred and twenty-six (79.7%) patients underwent LRHC, 12 (7.6%) patients underwent RARHC, conversion to an open procedure occurred in 20 (12.7%) patients. The operation time and estimated blood loss were 410.8 ± 128.9 min and 477.8 ± 706.3 mL, respectively. The surgical radicality of the 158 patients was R0, 129 (81.6%); R1, 20 (18.4%) and R2, 9 (5.7%). Grades I–II complications was occurred in 68 (43.0%) patients. Severe morbidity (grade III–V) occurred in 14 (8.7%) patients. The median overall survival in whole cohort was 25.4 months. The overall survival rate was 67.6% at year 1, 28.8% at year 3, and 19.2% at year 5. Comparing the first half of MISHC performed by each center with the following cases, the operation time and postoperative hospital stay does not decrease with the increasing cases. On literature review, MISHC is non-inferior to open surgery at least in perioperative period.
Conclusions
In this Chinese MIS for HC multicenter study, the largest to date, long-term overall survival rates after MIS appear comparable to those reported in current open series. Further randomized controlled trials are necessary to assess the global impact of MISHC.




Similar content being viewed by others
Data availability
The dataset that supports the findings of this study is available from the corresponding author upon request.
References
Mizuno T, Ebata T, Nagino M (2019) Advanced hilar cholangiocarcinoma: An aggressive surgical approach for the treatment of advanced hilar cholangiocarcinoma: Perioperative management, extended procedures, and multidisciplinary approaches. Surgical oncology undefined:undefined
Cillo U, Fondevila C, Donadon M, Gringeri E, Mocchegiani F, Schlitt H, Ijzermans J, Vivarelli M, Zieniewicz K, Olde Damink S, Groot Koerkamp B (2019) Surgery for cholangiocarcinoma. Liver international : official journal of the International Association for the Study of the Liver null:143–155
Lidsky ME, Jarnagin WR (2018) Surgical management of hilar cholangiocarcinoma at Memorial Sloan Kettering Cancer Center. Ann Gastroenterol Surg 2:304–312
Burke EC, Jarnagin WR, Hochwald SN, Pisters PW, Fong Y, Blumgart LH (1998) Hilar Cholangiocarcinoma: patterns of spread, the importance of hepatic resection for curative operation, and a presurgical clinical staging system. Ann Surg 228:385–394
Parikh A, Abdalla E, Vauthey J (2005) Operative considerations in resection of hilar cholangiocarcinoma. HPB : the official journal of the International Hepato Pancreato Biliary Association 7:254–258
Dinant S, Gerhards M, Busch O, Obertop H, Gouma D, Van Gulik T (2005) The importance of complete excision of the caudate lobe in resection of hilar cholangiocarcinoma. HPB : the official journal of the International Hepato Pancreato Biliary Association 7:263–267
Nagino M, Ebata T, Yokoyama Y, Igami T, Sugawara G, Takahashi Y, Nimura Y (2013) Evolution of surgical treatment for perihilar cholangiocarcinoma: a single-center 34-year review of 574 consecutive resections. Ann Surg 258:129–140
Song SC, Choi DW, Kow AW, Choi SH, Heo JS, Kim WS, Kim MJ (2013) Surgical outcomes of 230 resected hilar cholangiocarcinoma in a single centre. ANZ J Surg 83:268–274
Giulianotti PC, Sbrana F, Bianco FM, Addeo P (2010) Robot-assisted laparoscopic extended right hepatectomy with biliary reconstruction. J Laparoendosc Adv Surg Tech A 20:159–163
Klatskin G (1965) Adenocarcinoma of the Hepatic Duct at Its Bifurcation within the Porta Hepatis. An Unusual Tumor with Distinctive Clinical and Pathological Features. The American journal of medicine 38:241–256
Ito F, Cho CS, Rikkers LF, Weber SM (2009) Hilar Cholangiocarcinoma: Current Management. Ann Surg 250:210–218
Labib PL, Goodchild G, Pereira SP (2019) Molecular Pathogenesis of Cholangiocarcinoma BMC cancer 19:185
Krasinskas AM (2018) Cholangiocarcinoma Surgical pathology clinics 11:403–429
Razumilava N, Gores GJ (2014) Cholangiocarcinoma. Lancet (London, England) 383:2168–2179
Fisher AV, Ronnekleiv-Kelly SM (2018) Surgical Management of Hilar Cholangiocarcinoma. Current Surgery Reports 6
Jarnagin WR, Fong Y, DeMatteo RP, Gonen M, Burke EC, Bodniewicz BJ, Youssef BM, Klimstra D, Blumgart LH (2001) Staging, resectability, and outcome in 225 patients with hilar cholangiocarcinoma. Ann Surg 234:507–517
Cho MS, Kim SH, Park SW, Lim JH, Choi GH, Park JS, Chung JB, Kim KS (2012) Surgical outcomes and predicting factors of curative resection in patients with hilar cholangiocarcinoma: 10-year single-institution experience. J Gastrointest Surg 16:1672–1679
Ruys AT, Busch OR, Gouma DJ, van Gulik TM (2012) Staging Laparoscopy for Hilar Cholangiocarcinoma: Is it Still Worthwhile? Indian journal of surgical oncology 3:147–153
Li H, Wei Y (2019) Laparoscopic Extended Left Hemi-Hepatectomy plus Caudate Lobectomy for Caudate Lobe Hepatocellular Carcinoma. J Gastrointest Surg 23:617
Kim JH (2017) Laparoscopy-specific ventral approach in laparoscopic hemihepatectomy. J Surg Oncol 116:159–163
Ho KM, Han HS, Yoon YS, Cho JY, Choi YR, Jang JS, Kwon SU, Kim S, Choi JK (2017) Laparoscopic Total Caudate Lobectomy for Hepatocellular Carcinoma. J Laparoendosc Adv Surg Tech A 27:1074–1078
Oh D, Kwon CH, Na BG, Lee KW, Cho WT, Lee SH, Choi JY, Choi GS, Kim JM, Joh JW (2016) Surgical Techniques for Totally Laparoscopic Caudate Lobectomy. J Laparoendosc Adv Surg Tech A 26:689–692
Wang M, Peng B, Liu J, Yin X, Tan Z, Liu R, Hong D, Zhao W, Wu H, Chen R, Li D, Huang H, Miao Y, Liu Y, Liang T, Wang W, Cai Y, Xing Z, Cheng W, Zhong X, Zhao Z, Zhang J, Yang Z, Li G, Shao Y, Lin G, Jiang K, Wu P, Jia B, Ma T, Jiang C, Peng S, Qin R (2019) Practice Patterns and Perioperative Outcomes of Laparoscopic Pancreaticoduodenectomy in China: A Retrospective Multicenter Analysis of 1029 Patients. Ann Surg
Song KB, Kim SC, Lee W, Hwang DW, Lee JH, Kwon J, Park Y, Lee SJ, Park G (2019) Laparoscopic pancreaticoduodenectomy for periampullary tumors: lessons learned from 500 consecutive patients in a single center. Surg Endosc
Franken LC, van der Poel MJ, Latenstein AEJ, Zwart MJ, Roos E, Busch OR, Besselink MG, van Gulik TM (2019) Minimally invasive surgery for perihilar cholangiocarcinoma: a systematic review. J Robot Surg
Kasai M, Cipriani F, Gayet B, Aldrighetti L, Ratti F, Sarmiento JM, Scatton O, Kim KH, Dagher I, Topal B, Primrose J, Nomi T, Fuks D, Abu Hilal M (2018) Laparoscopic versus open major hepatectomy: a systematic review and meta-analysis of individual patient data. Surgery 163:985–995
Livingston EH, Rege RV (2004) A nationwide study of conversion from laparoscopic to open cholecystectomy. Am J Surg 188:205–211
Dumitrascu T, Chirita D, Ionescu M, Popescu I (2013) Resection for hilar cholangiocarcinoma: analysis of prognostic factors and the impact of systemic inflammation on long-term outcome. J Gastrointest Surg 17:913–924
Tamoto E, Hirano S, Tsuchikawa T, Tanaka E, Miyamoto M, Matsumoto J, Kato K, Shichinohe T (2014) Portal vein resection using the no-touch technique with a hepatectomy for hilar cholangiocarcinoma. HPB (Oxford) 16:56–61
Kondo S, Hirano S, Ambo Y, Tanaka E, Okushiba S, Morikawa T, Katoh H (2004) Forty consecutive resections of hilar cholangiocarcinoma with no postoperative mortality and no positive ductal margins: results of a prospective study. Ann Surg 240:95–101
Launois B, Terblanche J, Lakehal M, Catheline JM, Bardaxoglou E, Landen S, Campion JP, Sutherland F, Meunier B (1999) Proximal bile duct cancer: high resectability rate and 5-year survival. Ann Surg 230:266–275
Ramesh H, Kuruvilla K, Venugopal A, Lekha V, Jacob G (2004) Surgery for hilar cholangiocarcinoma: feasibility and results of parenchyma-conserving liver resection. Dig Surg 21:114–122
Saxena A, Chua TC, Chu FC, Morris DL (2011) Improved outcomes after aggressive surgical resection of hilar cholangiocarcinoma: a critical analysis of recurrence and survival. Am J Surg 202:310–320
Hirano S, Kondo S, Tanaka E, Shichinohe T, Tsuchikawa T, Kato K, Matsumoto J, Kawasaki R (2010) Outcome of surgical treatment of hilar cholangiocarcinoma: a special reference to postoperative morbidity and mortality. J Hepatobiliary Pancreat Sci 17:455–462
Hemming AW, Mekeel K, Khanna A, Baquerizo A, Kim RD (2011) Portal vein resection in management of hilar cholangiocarcinoma. J Am Coll Surg 212:604–613
Lee SG, Song GW, Hwang S, Ha TY, Moon DB, Jung DH, Kim KH, Ahn CS, Kim MH, Lee SK, Sung KB, Ko GY (2010) Surgical treatment of hilar cholangiocarcinoma in the new era: the Asan experience. J Hepatobiliary Pancreat Sci 17:476–489
Nagino M, Nimura Y, Nishio H, Ebata T, Igami T, Matsushita M, Nishikimi N, Kamei Y (2010) Hepatectomy with simultaneous resection of the portal vein and hepatic artery for advanced perihilar cholangiocarcinoma: an audit of 50 consecutive cases. Ann Surg 252:115–123
Tan JW, Hu BS, Chu YJ, Tan YC, Ji X, Chen K, Ding XM, Zhang A, Chen F, Dong JH (2013) One-stage resection for Bismuth type IV hilar cholangiocarcinoma with high hilar resection and parenchyma-preserving strategies: a cohort study. World J Surg 37:614–621
Li H, Qin Y, Cui Y, Chen H, Hao X, Li Q (2011) Analysis of the surgical outcome and prognostic factors for hilar cholangiocarcinoma: a Chinese experience. Dig Surg 28:226–231
Cheng QB, Yi B, Wang JH, Jiang XQ, Luo XJ, Liu C, Ran RZ, Yan PN, Zhang BH (2012) Resection with total caudate lobectomy confers survival benefit in hilar cholangiocarcinoma of Bismuth type III and IV. Eur J Surg Oncol 38:1197–1203
Chen XP, Lau WY, Huang ZY, Zhang ZW, Chen YF, Zhang WG, Qiu FZ (2009) Extent of liver resection for hilar cholangiocarcinoma. Br J Surg 96:1167–1175
Otto G, Hoppe-Lotichius M, Bittinger F, Schuchmann M, Duber C (2011) Klatskin tumour: meticulous preoperative work-up and resection rate. Z Gastroenterol 49:436–442
Todoroki T, Kawamoto T, Koike N, Takahashi H, Yoshida S, Kashiwagi H, Takada Y, Otsuka M, Fukao K (2000) Radical resection of hilar bile duct carcinoma and predictors of survival. Br J Surg 87:306–313
Havlik R, Sbisa E, Tullo A, Kelly MD, Mitry RR, Jiao LR, Mansour MR, Honda K, Habib NA (2000) Results of resection for hilar cholangiocarcinoma with analysis of prognostic factors. Hepatogastroenterology 47:927–931
Kawasaki S, Imamura H, Kobayashi A, Noike T, Miwa S, Miyagawa S (2003) Results of surgical resection for patients with hilar bile duct cancer: application of extended hepatectomy after biliary drainage and hemihepatic portal vein embolization. Ann Surg 238:84–92
Konstadoulakis MM, Roayaie S, Gomatos IP, Labow D, Fiel MI, Miller CM, Schwartz ME (2008) Aggressive surgical resection for hilar cholangiocarcinoma: is it justified? Audit of a single center’s experience. Am J Surg 196:160–169
Seyama Y, Kubota K, Sano K, Noie T, Takayama T, Kosuge T, Makuuchi M (2003) Long-term outcome of extended hemihepatectomy for hilar bile duct cancer with no mortality and high survival rate. Ann Surg 238:73–83
Ogura Y, Mizumoto R, Tabata M, Matsuda S, Kusuda T (1993) Surgical treatment of carcinoma of the hepatic duct confluence: analysis of 55 resected carcinomas. World J Surg 17:85–92
Shimada K, Sano T, Sakamoto Y, Kosuge T (2005) Safety and effectiveness of left hepatic trisegmentectomy for hilar cholangiocarcinoma. World J Surg 29:723–727
Ercolani G, Zanello M, Grazi GL, Cescon M, Ravaioli M, Del Gaudio M, Vetrone G, Cucchetti A, Brandi G, Ramacciato G, Pinna AD (2010) Changes in the surgical approach to hilar cholangiocarcinoma during an 18-year period in a Western single center. J Hepatobiliary Pancreat Sci 17:329–337
Funding
This research was funded by the Department of Education, Sichuan Province (16TDD00025, to Jingdong Li), Scientific Research Project of Affiliated Hospital of North Sichuan Medical College (2020ZD001, to Yongfu Xiong; 2020JC035, to Gang Yang), and Pre-research of State-level Project of North Sichuan Medical College (CBY19-YZ17, to Yongfu Xiong); Project of multicentre clinical research of Shanghai Jiaotong University School of Medicine (DLY201807, to Zhaohui Tang).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Li Jingdong, Xiong Yongfu, Gang Yang, Xu Jian, Huang Xujian, Liu Jianhua, Zhao Wenxing, Qin Renyi, Yin Xinming, Zheng Shuguo, Liang Xiao, Peng Bin, Zhang Qifan, Li Dewei and Tang Zhao-hui have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jingdong, L., Yongfu, X., Yang, G. et al. Minimally invasive surgery for hilar cholangiocarcinoma: a multicenter retrospective analysis of 158 patients. Surg Endosc 35, 6612–6622 (2021). https://doi.org/10.1007/s00464-020-08161-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08161-8