Abstract
Background
Enhanced recovery after surgery (ERAS) are evidence-based protocols associated with improved patient outcomes. The use of ERAS pathways is well documented in various surgical specialties. The aim of this systematic review and meta-analysis was to examine the efficacy of ERAS protocols in patients undergoing abdominal wall reconstruction (AWR).
Methods
This systematic review and meta-analysis were reported according to PRISMA and MOOSE guidelines. The databases PubMed, EMBASE, CINAHL, Web of Science and Cochrane Library were searched for original studies comparing ERAS with standard care in patients undergoing AWR. The primary outcome was length of stay (LOS) and secondary outcomes were readmission and surgical site infection (SSI) and/or surgical site occurrences (SSO).
Results
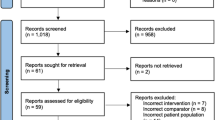
Five studies were included in the meta-analysis. All were retrospective cohort studies including 453 patients treated according to ERAS protocols, and 494 patients treated according to standard care. The meta-analysis demonstrated that patients undergoing AWR managed with ERAS had a mean 0.89 days reduction in LOS compared with patients treated with standard care (95% CI − 1.70 to − 0.07 days, p = 0.03). There was no statistically significant difference in readmission rate (OR 1.00, 95% CI 0.53 to 1.87, p = 1.00) or SSI/SSO (OR 1.19, 95% CI 0.67 to 2.11, p = 0.56) between groups.
Conclusions
The use of ERAS in patients undergoing AWR was found to significantly reduce LOS without increasing the readmission rate or SSI/SSO. Based on the existing literature, ERAS protocols should be implemented for patients undergoing AWR.




Similar content being viewed by others
References
Kleppe KL, Greenberg JA (2018) Enhanced recovery after surgery protocols: rationale and components. Surg Clin North Am. https://doi.org/10.1016/j.suc.2018.01.006
Kehlet H (1997) Multimodal approach to control postoperative pathophysiology and rehabilitation. Br J Anaesth 78:606
Scott MJ, Baldini G, Fearon KCH, Feldheiser A, Feldman LS, Gan TJ, Ljungqvist O, Lobo DN, Rockall TA, Schricker T, Carli F (2015) Enhanced recovery after surgery (ERAS) for gastrointestinal surgery, part 1: pathophysiological considerations. Acta Anaesthesiol Scand 59:1212
Fayezizadeh M, Petro CC, Rosen MJ, Novitsky YW (2014) Enhanced recovery after surgery pathway for abdominal wall reconstruction: pilot study and preliminary outcomes. Plast Reconstr Surg. https://doi.org/10.1097/PRS.0000000000000674
Spanjersberg WR, Reurings J, Keus F, van Laarhoven CJ (2011) Fast track surgery versus conventional recovery strategies for colorectal surgery. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd007635.pub2
Orenstein SB, Martindale RG (2018) Enhanced recovery pathway for complex abdominal wall reconstruction. Plast Reconstr Surg. https://doi.org/10.1097/PRS.0000000000004869
Moher D, Liberati A, Tetzlaff J, Altman DG, Altman D, Antes G, Atkins D, Barbour V, Barrowman N, Berlin JA, Clark J, Clarke M, Cook D, D’Amico R, Deeks JJ, Devereaux PJ, Dickersin K, Egger M, Ernst E, Gøtzsche PC, Grimshaw J, Guyatt G, Higgins J, Ioannidis JPA, Kleijnen J, Lang T, Magrini N, McNamee D, Moja L, Mulrow C, Napoli M, Oxman A, Pham B, Rennie D, Sampson M, Schulz KF, Shekelle PG, Tovey D, Tugwell P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. J Am Med Assoc 283:2008–2012. https://doi.org/10.1001/jama.283.15.2008
DeBord J, Novitsky Y, Fitzgibbons R, Miserez M, Montgomery A (2018) SSI, SSO, SSE, SSOPI: the elusive language of complications in hernia surgery. Hernia 22:737
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan AW, Churchill R, Deeks JJ, Hróbjartsson A, Kirkham J, Jüni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schünemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: A tool for assessing risk of bias in non-randomised studies of interventions. BMJ. https://doi.org/10.1136/bmj.i4919
Balshem H, Helfand M, Schünemann HJ, Oxman AD, Kunz R, Brozek J, Vist GE, Falck-Ytter Y, Meerpohl J, Norris S, Guyatt GH (2011) GRADE guidelines: 3. Rating the quality of evidence. J Clin Epidemiol. https://doi.org/10.1016/j.jclinepi.2010.07.015
McMaster University (2015) GRADEpro GDT: GRADEpro guideline development tool [software]. Evid. Prime Inc., Springfield
Schünemann H, Brożek J, Guyatt G, Oxman A (2013) GRADE handbook for grading quality of evidence and strength of recommendations. BMJ 3328:1490
Mohapatra SK, Balaji M, Ganapathi R (2019) Application of enhanced recovery pathway in abdominal wall reconstruction surgery in a tertiary care hospital in Andhra Pradesh. Int J Surg Sci. https://doi.org/10.33545/surgery.2019.v3.i4c.231
Majumder A, Fayezizadeh M, Neupane R, Elliott HL, Novitsky YW (2016) Benefits of multimodal enhanced recovery pathway in patients undergoing open ventral hernia repair. J Am Coll Surg 222:1106
Warren JA, Stoddard C, Hunter AL, Horton AJ, Atwood C, Ewing JA, Pusker S, Cancellaro VA, Walker KB, Cobb WS, Carbonell AM, Morgan RR (2017) Effect of multimodal analgesia on opioid use after open ventral hernia repair. J Gastrointest Surg. https://doi.org/10.1007/s11605-017-3529-4
Jensen KK, Dressler J, Baastrup NN, Kehlet H, Jørgensen LN (2019) Enhanced recovery after abdominal wall reconstruction reduces length of postoperative stay: an observational cohort study. Surgery (United States). https://doi.org/10.1016/j.surg.2018.07.035
Colvin J, Rosen M, Prabhu A, Rosenblatt S, Petro C, Zolin S, Krpata D (2019) Enhanced recovery after surgery pathway for patients undergoing abdominal wall reconstruction. Surgery (United States). https://doi.org/10.1016/j.surg.2019.05.023
Ueland W, Walsh-Blackmore S, Nisiewicz M, Davenport DL, Plymale MA, Plymale M, Roth JS (2019) The contribution of specific enhanced recovery after surgery (ERAS) protocol elements to reduced length of hospital stay after ventral hernia repair. Surg Endosc. https://doi.org/10.1007/s00464-019-07233-8
Guyatt GH, Oxman AD, Vist G, Kunz R, Brozek J, Alonso-Coello P, Montori V, Akl EA, Djulbegovic B, Falck-Ytter Y, Norris SL, Williams JW, Atkins D, Meerpohl J, Schünemann HJ (2011) GRADE guidelines: 4. Rating the quality of evidence—study limitations (risk of bias). J Clin Epidemiol. https://doi.org/10.1016/j.jclinepi.2010.07.017
Jensen KK, Brondum TL, Harling H, Kehlet H, Jorgensen LN (2016) Enhanced recovery after giant ventral hernia repair. Hernia. https://doi.org/10.1007/s10029-016-1471-0
Visioni A, Shah R, Gabriel E, Attwood K, Kukar M, Nurkin S (2018) Enhanced recovery after surgery for noncolorectal surgery? A systematic review and meta-analysis of major abdominal surgery. Ann Surg. https://doi.org/10.1097/SLA.0000000000002267
Huang ZD, Gu HY, Zhu J, Luo J, Shen XF, Deng QF, Zhang C, Li YB (2020) The application of enhanced recovery after surgery for upper gastrointestinal surgery: meta-analysis. BMC Surg. https://doi.org/10.1186/s12893-019-0669-3
AlBalawi Z, Gramlich L, Nelson G, Senior P, Youngson E, McAlister FA (2018) The Impact of the Implementation of the enhanced recovery after surgery (ERAS®) program in an entire health system: a natural experiment in Alberta, Canada. World J Surg. https://doi.org/10.1007/s00268-018-4559-0
Jensen KK, Henriksen NA, Jorgensen LN (2014) Endoscopic component separation for ventral hernia causes fewer wound complications compared to open components separation: a systematic review and meta-analysis. Surg Endosc. https://doi.org/10.1007/s00464-014-3599-2
Kehlet H (2009) Multimodal approach to postoperative recovery. Curr Opin Crit Care 15:355
Lovecchio F, Farmer R, Souza J, Khavanin N, Dumanian GA, Kim JYS (2014) Risk factors for 30-day readmission in patients undergoing ventral hernia repair. Surgery (United States). https://doi.org/10.1016/j.surg.2013.12.021
Hawn MT, Gray SH, Snyder CW, Graham LA, Finan KR, Vick CC (2011) Predictors of mesh explantation after incisional hernia repair. Am J Surg. https://doi.org/10.1016/j.amjsurg.2010.10.011
Sanchez VM, Abi-Haidar YE, Itani KMF (2011) Mesh infection in ventral incisional hernia repair: Incidence, contributing factors, and treatment. Surg Infect 12:205
Warren JA, Carbonell AM, Jones LK, Mcguire A, Hand WR, Cancellaro VA, Ewing JA, Cobb WS (2019) Length of stay and opioid dose requirement with transversus abdominis plane block vs epidural analgesia for ventral hernia repair. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2018.12.017
Prabhu AS, Krpata DM, Perez A, Phillips S, Huang LC, Haskins IN, Rosenblatt S, Poulose BK, Rosen MJ (2018) Is it time to reconsider postoperative epidural analgesia in patients undergoing elective ventral hernia repair? Ann Surg. https://doi.org/10.1097/SLA.0000000000002214
Jensen KK (2019) Comment on “is it time to reconsider postoperative epidural analgesia in patients undergoing elective ventral hernia repair?”. Ann Surg 267:971
Harryman C, Plymale MA, Stearns E, Davenport DL, Chang W, Roth JS (2019) Enhanced value with implementation of an ERAS protocol for ventral hernia repair. Surg Endosc. https://doi.org/10.1007/s00464-019-07166-2
Funding
No funds were received for the current study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Lise Lode, Erling Oma, Nadia A. Henriksen and Kristian K. Jensen have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lode, L., Oma, E., Henriksen, N.A. et al. Enhanced recovery after abdominal wall reconstruction: a systematic review and meta-analysis. Surg Endosc 35, 514–523 (2021). https://doi.org/10.1007/s00464-020-07995-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07995-6