Abstract
Background
The European Association for Endoscopic Surgery (EAES) strives to be a leader in promoting the development and expansion of minimally invasive surgery (MIS). Part of the association’s mission statement is “to become an information hub for all practitioners of MIS”. It is therefore important that the education segment of the association continues to be actively monitored and updated to ensure this mission statement is met. This project aimed to understand the trainees requirement in fulfilling this role, and to develop an practical action plan to ensure such requirements are adequately met.
Methods
Two sequential questionnaires were sent to all members of the EAES. The questionnaires sought to understand the demographics of the EAES membership, and their training requirements. This followed a Delphi methodology. The data collected included training status, level of competence in laparoscopic surgery and tools needed for improving laparoscopic skills.
Results
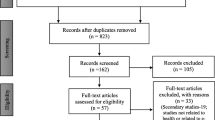
Four hundred and sixty-five responded to the first survey, and 209 responded to the second survey. There were 112 trainees (24.1%) in the first round. More than 50% of trainees were less than 8 years from graduation from medical school. Only 162 (34.8%) of respondents performed MIS in more than half their practice. Videos of common procedures were ranked the highest in terms of what trainees required to help improve their laparoscopic skills, followed by e-learning modules.
Conclusion
There is a significant training gap identified amongst the trainee population of the EAES with regards to MIS training. Trainees were not performing MIS enough for them to feel confident with their skills. The EAES could fulfill this training requirement via expertly curated videos, and e-learning modules written by senior specialists.






Similar content being viewed by others
References
Morales-Conde S, Peeters A, Meyer YM, Antoniou SA, del Agua IA, Arezzo A et al (2019) European association for endoscopic surgery (EAES) consensus statement on single-incision endoscopic surgery. Surg Endosc 33(4):996–1019
Gorter RR, Eker HH, Gorter-Stam MAW, Abis GSA, Acharya A, Ankersmit M et al (2016) Diagnosis and management of acute appendicitis. EAES consensus development conference 2015. Surg Endosc 30:4668
Blencowe NS, Parsons BA, Hollowood AD (2011) Effects of changing work patterns on general surgical training over the last decade. Postgrad Med J 87(1034):795–799
Celentano V, Smart N, Cahill RA, McGrath JS, Gupta S, Griffith JP et al (2018) Use of laparoscopic videos amongst surgical trainees in the United Kingdom. Surgeon 14:334–339
Thangaratinam S, Redman CW (2005) The delphi technique. Obstetr Gynaecol 7(2):120–125
Shore EM, Lefebvre GG, Husslein H, Bjerrum F, Sorensen JL, Grantcharov TP (2015) Designing a standardized laparoscopy curriculum for gynecology residents: a delphi approach. J Grad Med Educ 7(2):197–202
Palter VN, Graafland M, Schijven MP, Grantcharov TP (2012) Designing a proficiency-based, content validated virtual reality curriculum for laparoscopic colorectal surgery: a Delphi approach. Surgery 151(3):391–397
Aggarwal R, Moorthy K, Darzi A (2004) Laparoscopic skills training and assessment. Br J Surg 91(12):1549–1558
Buzink SN, Shiappa JM, Castelo HB, Fingerhut A, Hanna G, Jakimowicz JJ (2012) The e laparoscopic surgical skills programme: setting the European standard. Rev Port Cir 20:33–40
Buzink S, Soltes M, Radonak J, Fingerhut A, Hanna G, Jakimowicz J (2012) Laparoscopic surgical skills programme: preliminary evaluation of grade i level 1 courses by trainees. Wideochirurgia I Inne Tech Maloinwazyjne 7(3):188–192
Elsey EJ, Griffiths G, Humes DJ, West J (2017) Meta-analysis of operative experiences of general surgery trainees during training. Br J Surg 104(1):22–33
YouTube (2019) Colorectal Disease Journal. https://www.youtube.com/channel/UCi8Rw-2e92Eiam7kjrfMn_g Accessed 12 Aug 2019
Sinha S, Hofman D, Stoker DL, Friend PJ, Poloniecki JD, Thompson MM, Holt PJ (2013) Epidemiological study of provision of cholecystectomy in England from 2000 to 2009: retrospective analysis of Hospital Episode Statistics. Surg Endosc 27(1):162–175
Kemp JA, Zuckerman RS, Finlayson SR (2008) Trends in adoption of laparoscopic cholecystectomy in rural versus urban hospitals. J Am Coll Surg 206(1):28–32
Finlayson SR, Laycock WS, Birkmeyer JD (2003) National trends in utilization and outcomes of antireflux surgery. Surg Endosc 17(6):864–867
Funding
This study has no funding sources to declare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Dr. Balaji Mahendran, Dr. Valerio Celentano, Dr. Carlos Moreno Sanz, Dr. Bjørn Edwin and Dr. Mohammed Abu Hilal have no conflicts of interest or financial ties to disclose. Dr. Mark Coleman is a member of the Education and Training sub-committee of the EAES. Dr. Dorin Popa is a member of the Education and Training sub-committee of the EAES. Dr. Marek Soltes is a member of the Education and Training sub-committee of the EAES. Dr. Michel Adamina is a member of the Education and Training sub-committee of the EAES.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mahendran, B., Celentano, V., Soltes, M. et al. EAES online educational resources: a survey of the membership of the European Association for Endoscopic Surgery (EAES). Surg Endosc 35, 2059–2066 (2021). https://doi.org/10.1007/s00464-020-07602-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07602-8