Abstract
Background
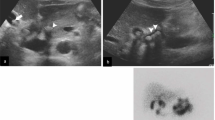
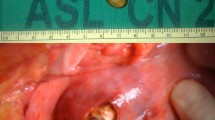
Mirizzi syndrome (MS) is characterized by an obstruction of the proximal bile duct due to extrinsic compression by either an impacted stone in the gallbladder neck or local inflammatory changes. Although this is a rare syndrome in developed countries (0.7–1.4 %), preoperative diagnosis and careful surgical management are essential to avoid bilio-vascular injuries and misdiagnosed malignancy.
Methods
The purpose of this study was to review our experience in the diagnosis and management of MS, assess the role of laparoscopy and the risk of concomitant gallbladder carcinoma. This study took place in a large county hospital which serves indigent and undocumented immigrants without easy access to healthcare. Data were collected through a retrospective chart review of 4939 patients that underwent cholecystectomy over 6 years. Patient demographics, preoperative, intraoperative, postoperative data and outcomes were analyzed.
Results
MS was identified in 60 of 4939 patients (1.21 %) who underwent cholecystectomy. The mean age at presentation was 47 years, and 35 patients were females. The most common symptom at presentation was abdominal pain (100 %) followed by nausea/vomiting (87 %) and jaundice (43 %). Type I MS was diagnosed in 16 patients and 44 had type II MS. Preoperative diagnosis was achieved in 43 patients (71 %). Magnetic resonance cholangiopancreatography was the best diagnostic modality. Laparoscopic cholecystectomy was successful in 4 out of 16 patients with type I MS. Three patients (5.26 %) had simultaneous gallbladder cancer. Overall morbidity was 27 % and mortality was 0. Clavien grade ≥3 complications were seen in six patients (10 %). The mean length of follow-up was 2.3 months (range 0–5) for type I MS patients and 5.4 months (range 0–46) for type II patients.
Conclusions
MS is rare, but preoperative diagnosis or intraoperative suspicion is important. Laparoscopic cholecystectomy may be possible in selected type I cases. Open cholecystectomy is the standard of care for type II MS.




Similar content being viewed by others
References
Mirizzi P (1948) Syndrome del conducto hepatico. J Int Chir 8:731–777
Kehr H (1905) Die in meiner Klinik geübte Technik der Gallenstein operationen mit einem Hinweis auf die Indikationen und die Dauererfolge Auf Grund eigener, bei 1000 Laparotomien gesammelter Erfahrungen. Lehmann, München
Ruge E (1908) Beitraege zur chirurgischen anatomie der grossen gallenwege (ductus hepaticus, cysticus, choledochus und pancreaticus). Arch Klin Chir 87:47–78
Csendes A, Diaz JC, Burdiles P, Maluenda F, Nava O (1989) Mirizzi syndrome and cholecystobiliary fistula: a unifying classification. Br J Surg 76:1139–1143
McSherry CK, Ferstenberg H, Virshup M (1982) The Mirizzi syndrome: suggested classification and surgical therapy. Surg Gastroenterol 1:219–225
Baer HU, Matthews JB, Schweizer WP, Gertsch P, Blumgart LH (1990) Management of the Mirizzi syndrome and the surgical implications of cholecystocholedochal fistula. Br J Surg 77:743–745
Mishra MC, Vashishtha S, Tandon R (1990) Biliobiliary fistula: preoperative diagnosis and management implications. Surgery 108:835–839
Kwon AH, Inui H (2007) Preoperative diagnosis and efficacy of laparoscopic procedures in the treatment of Mirizzi syndrome. J Am Coll Surg 204:409–415
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications. A new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Redaelli CA, Büchler MW, Schilling MK, Krähenbühl L, Ruchti C, Blumgart LH, Baer HU (1997) High coincidence of Mirizzi syndrome and gallbladder carcinoma. Surgery 121:58–63
Prasad TL, Kumar A, Sikora SS, Saxena R, Kapoor VK (2006) Mirizzi syndrome and gallbladder cancer. J Hepatobiliary Pancreat Surg 13(4):323–326
Tan KY, Chng HC, Chen CYY, Tan SM, Poh BK, Hoe MN (2004) Mirizzi syndrome: noteworthy aspects of a retrospective study in one center. ANZ J Surg 74:833–837
Beltran MA (2012) Mirizzi syndrome: history, current knowledge and proposal of a simplified classification. World J Gastroenterol 18(34):4639–4650
Erben Y, Benavente-Chenhalls LA, Donahue JM, Que FG, Kendrick ML, Reid-Lombardo KM, Farnell MB, Nagorney DM (2011) Diagnosis and treatment of Mirizzi syndrome: 23 year Mayo clinic experience. J Am Coll Surg 213(1):114–119
Chowbey PK, Sharma A, Mann V, Khullar R, Baijal M, Vashistha A (2000) The management of Mirizzi syndrome in the laparoscopic era. Surg Laparosc Endosc Percutan Tech 10:11–14
Sare M, Gurer S, Taskin V, Aladaq M, Hilmioqlu F, Gurel M (1998) Mirizzi syndrome: choice of surgical procedure in the laparoscopic era. Surg Laparosc Endosc 8:63–67
Bagia JS, North L, Hunt DR (2001) An extra hazard for laparoscopic surgery. ANZ J Surg 71:394–397
Lai ECH, Lau WY (2006) Mirizzi syndrome: history, present and future development. ANZ J Surg 76:251–257
Tsuyuguchi T, Sakai Y, Sugiyama H, Ishihara T, Yokosuka O (2011) Long-term follow-up after peroral cholangioscopy-directed lithotripsy in patients with difficult bile duct stones, including Mirizzi syndrome: an analysis of risk factors predicting stone recurrence. Surg Endosc 25:2179–2185
England RE, Martin DF (1997) Endoscopic management of Mirizzi’s syndrome. Gut 40:272–276
Cairns SR, Watson GN, Lees WR, Salmon PR (1987) Percutaneous lithotripsy and endo-prosthesis: a new treatment for obstructive jaundice in Mirizzi’s syndrome. BMJ 295:1448
Oxtoby JW, Yeong CC, West DJ (1994) Mirizzi syndrome treated by percutaneous stone removal. Cardiovasc Intervent Radiol 17:207–209
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Kulkarni, Hotta, Sher, Buxbaum, Selby, Parekh and Stapfer have no conflicts of interests or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Kulkarni, S.S., Hotta, M., Sher, L. et al. Complicated gallstone disease: diagnosis and management of Mirizzi syndrome. Surg Endosc 31, 2215–2222 (2017). https://doi.org/10.1007/s00464-016-5219-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5219-9