Abstract
Background
In medical practice, the tendency to remove an inflamed gallbladder is deeply rooted. Cholecystectomy, however, is associated with relatively high complication rates, and therefore the decision whether or not to perform surgery should be well considered. For some patients, the surgical risk–benefit profile may favour conservative treatment. The objective of this study was to examine the short- and long-term outcome of conservative treatment of patients with acute calculous cholecystitis.
Methods
A systematic search of MEDLINE, Embase and Cochrane Library databases was performed. Prospective studies reporting on the success rate of conservative treatment (i.e. non-invasive treatment) of acute cholecystitis during index admission were included, as well as prospective and retrospective studies reporting on the recurrence rate of gallstone-related disease during long-term follow-up (i.e. ≥12 months) after initial non-surgical management. Study selection was undertaken independently by two reviewers using predefined criteria. The risk of bias was assessed. The pooled success and mortality rate during index admission and the pooled recurrence rate of gallstone-related disease during long-term follow-up were calculated using a random-effects model.
Results
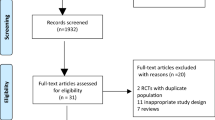
A total of 1841 patients were included in 10 randomized controlled trials and 14 non-randomized studies. Conservative treatment during index admission was successful in 87 % of patients with acute calculous cholecystitis and in 96 % of patients with mild disease. In the long term, 22 % of the patients developed recurrent gallstone-related disease. Pooled analysis showed a success rate of 86 % (95 % CI 0.8–0.9), a mortality rate of 0.5 % (95 % CI 0.001–0.009) and a recurrence rate of 20 % (95 % CI 0.1–0.3).
Discussion
Conservative treatment of acute calculous cholecystitis during index admission seems feasible and safe, especially in patients with mild disease. During long-term follow-up, less than a quarter of the patients appear to develop recurrent gallstone-related disease, although this outcome is based on limited data.




Similar content being viewed by others
References
Solomkin JS, Mazuski JE, Bradley JS, Rodvold KA, Goldstein EJ, Baron EJ, O’Neill PJ, Chow AW, Dellinger EP, Eachempati SR, Gorbach S, Hilfiker M, May AK, Nathens AB, Sawyer RG, Bartlett JG (2010) Diagnosis and management of complicated intra-abdominal infection in adults and children: guidelines by the Surgical Infection Society and the Infectious Diseases Society of America. Surg Infect (Larchmt) 11:79–109. doi:10.1089/sur.2009.9930
The Dutch guidelines for gallstone disease (web site). http://www.heelkunde.nl/uploads/_6/re/_6reZZkgrYUAuCG6uvcN-A/richtlijn_galsteen.pdf. Accessed July 2015
Yokoe M, Takada T, Strasberg SM, Solomkin JS, Mayumi T, Gomi H, Pitt HA, Garden OJ, Kiriyama S, Hata J, Gabata T, Yoshida M, Miura F, Okamoto K, Tsuyuguchi T, Itoi T, Yamashita Y, Dervenis C, Chan AC, Lau WY, Supe AN, Belli G, Hilvano SC, Liau KH, Kim MH, Kim SW, Ker CG, Committee Tokyo Guidelines Revision (2013) TG13 diagnostic criteria and severity grading of acute cholecystitis (with videos). J Hepatobiliary Pancreat Sci 20:35–46. doi:10.1007/s00534-012-0568-9
Mayumi T, Takada T, Kawarada Y, Nimura Y, Yoshida M, Sekimoto M, Miura F, Wada K, Hirota M, Yamashita Y, Nagino M, Tsuyuguchi T, Tanaka A, Gomi H, Pitt HA (2007) Results of the Tokyo consensus meeting Tokyo guidelines. J Hepatobiliary Pancreat Surg 14:114–121. doi:10.1007/s00534-006-1163-8
Cao AM, Eslick GD, Cox MR (2015) Early cholecystectomy is superior to delayed cholecystectomy for acute cholecystitis: a meta-analysis. J Gastrointest Surg 19:848–857. doi:10.1007/s11605-015-2747-x
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62:e1–34. doi:10.1016/j.jclinepi.2009.06.006
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Open Med 3:e123–e130
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716. doi:10.1046/j.1445-2197.2003.02748.x
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA, Cochrane Bias Methods Group, Cochrane Statistical Methods Group (2011) The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ 343:d5928. doi:10.1136/bmj.d5928
Agrawal R, Sood KC, Agarwal B (2015) Evaluation of early versus delayed laparoscopic cholecystectomy in acute cholecystitis. Surg Res Pract 2015:349801. doi:10.1155/2015/349801
Mazeh H, Mizrahi I, Dior U, Simanovsky N, Shapiro M, Freund HR, Eid A (2012) Role of antibiotic therapy in mild acute calculus cholecystitis: a prospective randomized controlled trial. World J Surg 36:1750–1759. doi:10.1007/s00268-012-1572-6
Kolla SB, Aggarwal S, Kumar A, Kumar R, Chumber S, Parshad R, Seenu V (2004) Early versus delayed laparoscopic cholecystectomy for acute cholecystitis: a prospective randomized trial. Surg Endosc 18:1323–1327. doi:10.1007/s00464-003-9230-6
Johansson M, Thune A, Blomqvist A, Nelvin L, Lundell L (2003) Management of acute cholecystitis in the laparoscopic era: results of a prospective, randomized clinical trial. J Gastrointest Surg 7:642–645. doi:10.1016/S1091-255X(03)00065-9
Vetrhus M, Soreide O, Nesvik I, Sondenaa K (2003) Acute cholecystitis: delayed surgery or observation. A randomized clinical trial. Scand J Gastroenterol 38:985–990
Hatzidakis AA, Prassopoulos P, Petinarakis I, Sanidas E, Chrysos E, Chalkiadakis G, Tsiftsis D, Gourtsoyiannis NC (2002) Acute cholecystitis in high-risk patients: percutaneous cholecystostomy vs conservative treatment. Eur Radiol 12:1778–1784. doi:10.1007/s00330-001-1247-4
Lai PB, Kwong KH, Leung KL, Kwok SP, Chan AC, Chung SC, Lau WY (1998) Randomized trial of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Br J Surg 85:764–767. doi:10.1046/j.1365-2168.1998.00708.x
Lo CM, Liu CL, Fan ST, Lai EC, Wong J (1998) Prospective randomized study of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Ann Surg 227:461–467
Rodriguez-Cerrillo M, Poza-Montoro A, Fernandez-Diaz E, Inurrieta-Romero A, Matesanz-David M (2012) Home treatment of patients with acute cholecystitis. Eur J Intern Med 23:e10–e13. doi:10.1016/j.ejim.2011.07.012
Barak O, Elazary R, Appelbaum L, Rivkind A, Almogy G (2009) Conservative treatment for acute cholecystitis: clinical and radiographic predictors of failure. Isr Med Assoc J 11:739–743
Paran H, Zissin R, Rosenberg E, Griton I, Kots E, Gutman M (2006) Prospective evaluation of patients with acute cholecystitis treated with percutaneous cholecystostomy and interval laparoscopic cholecystectomy. Int J Surg 4:101–105. doi:10.1016/j.ijsu.2006.01.001
Serralta AS, Bueno JL, Planells MR, Rodero DR (2003) Prospective evaluation of emergency versus delayed laparoscopic cholecystectomy for early cholecystitis. Surg Laparosc Endosc Percutan Tech 13:71–75
Vracko J, Markovic S, Wiechel KL (2006) Conservative treatment versus endoscopic sphincterotomy in the initial management of acute cholecystitis in elderly patients at high surgical risk. Endoscopy 38:773–778. doi:10.1055/s-2006-925448
Gutt CN, Encke J, Koninger J, Harnoss JC, Weigand K, Kipfmuller K, Schunter O, Gotze T, Golling MT, Menges M, Klar E, Feilhauer K, Zoller WG, Ridwelski K, Ackmann S, Baron A, Schon MR, Seitz HK, Daniel D, Stremmel W, Buchler MW (2013) Acute cholecystitis: early versus delayed cholecystectomy, a multicenter randomized trial (ACDC study, NCT00447304). Ann Surg 258:385–393. doi:10.1097/SLA.0b013e3182a1599b
Schmidt M, Sondenaa K, Vetrhus M, Berhane T, Eide GE (2011) Long-term follow-up of a randomized controlled trial of observation versus surgery for acute cholecystitis: non-operative management is an option in some patients. Scand J Gastroenterol 46:1257–1262. doi:10.3109/00365521.2011.598548
Rodriguez-Sanjuan JC, Arruabarrena A, Sanchez-Moreno L, Gonzalez-Sanchez F, Herrera LA, Gomez-Fleitas M (2012) Acute cholecystitis in high surgical risk patients: percutaneous cholecystostomy or emergency cholecystectomy? Am J Surg 204:54–59. doi:10.1016/j.amjsurg.2011.05.013
Melloul E, Denys A, Demartines N, Calmes JM, Schafer M (2011) Percutaneous drainage versus emergency cholecystectomy for the treatment of acute cholecystitis in critically ill patients: does it matter? World J Surg 35:826–833. doi:10.1007/s00268-011-0985-y
Griniatsos J, Petrou A, Pappas P, Revenas K, Karavokyros I, Michail OP, Tsigris C, Giannopoulos A, Felekouras E (2008) Percutaneous cholecystostomy without interval cholecystectomy as definitive treatment of acute cholecystitis in elderly and critically ill patients. South Med J 101:586–590. doi:10.1097/SMJ.0b013e3181757b77
Horn T, Christensen SD, Kirkegard J, Larsen LP, Knudsen AR, Mortensen FV (2015) Percutaneous cholecystostomy is an effective treatment option for acute calculous cholecystitis: a 10-year experience. HPB (Oxford) 17:326–331. doi:10.1111/hpb.12360
Chang YR, Ahn YJ, Jang JY, Kang MJ, Kwon W, Jung WH, Kim SW (2014) Percutaneous cholecystostomy for acute cholecystitis in patients with high comorbidity and re-evaluation of treatment efficacy. Surgery 155:615–622. doi:10.1016/j.surg.2013.12.026
McGillicuddy EA, Schuster KM, Barre K, Suarez L, Hall MR, Kaml GJ, Davis KA, Longo WE (2012) Non-operative management of acute cholecystitis in the elderly. Br J Surg 99:1254–1261. doi:10.1002/bjs.8836
Andren-Sandberg A, Haugsvedt T, Larssen TB, Sondenaa K (2001) Complications and late outcome following percutaneous drainage of the gallbladder in acute calculous cholecystitis. Dig Surg 18:393–398. doi:10.1159/000050180
Hamy A, Visset J, Likholatnikov D, Lerat F, Gibaud H, Savigny B, Paineau J (1997) Percutaneous cholecystostomy for acute cholecystitis in critically ill patients. Surgery 121:398–401. doi:10.1016/S0039-6060(97)90309-3
Li M, Li N, Ji W, Quan Z, Wan X, Wu X, Li J (2013) Percutaneous cholecystostomy is a definitive treatment for acute cholecystitis in elderly high-risk patients. Am Surg 79:524–527
Beckham H, Whitlow CB (2009) The medical and nonoperative treatment of diverticulitis. Clin Colon Rectal Surg 22:156–160. doi:10.1055/s-0029-1236159
Unlu C, Gunadi PM, Gerhards MF, Boermeester MA, Vrouenraets BC (2013) Outpatient treatment for acute uncomplicated diverticulitis. Eur J Gastroenterol Hepatol 25:1038–1043. doi:10.1097/MEG.0b013e328361dd5b
Bauer VP (2009) Emergency management of diverticulitis. Clin Colon Rectal Surg 22:161–168. doi:10.1055/s-0029-1236160
Mason RJ (2008) Surgery for appendicitis: is it necessary? Surg Infect (Larchmt) 9:481–488. doi:10.1089/sur.2007.079
Friedman GD, Raviola CA, Fireman B (1989) Prognosis of gallstones with mild or no symptoms: 25 years of follow-up in a health maintenance organization. J Clin Epidemiol 42:127–136. doi:10.1016/0895-4356(89)90086-3
Lam CM, Yuen AW, Wai AC, Leung RM, Lee AY, Ng KK, Fan ST (2005) Gallbladder cancer presenting with acute cholecystitis: a population-based study. Surg Endosc 19:697–701. doi:10.1007/s00464-004-9116-2
Oikarinen H (2006) Diagnostic imaging of carcinomas of the gallbladder and the bile ducts. Acta Radiol 47:345–358
Andren-Sandberg A (2012) Diagnosis and management of gallbladder cancer. N Am J Med Sci 4:293–299. doi:10.4103/1947-2714.98586
Wilson E, Gurusamy K, Gluud C, Davidson BR (2010) Cost-utility and value-of-information analysis of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Br J Surg 97:210–219. doi:10.1002/bjs.6872
Johner A, Raymakers A, Wiseman SM (2013) Cost utility of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Surg Endosc 27:256–262. doi:10.1007/s00464-012-2430-1
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Loozen, Dr. Oor, Dr. Van Ramshorst, Dr. Van Santvoort and Dr. Boerma have no conflict of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
Loozen, C.S., Oor, J.E., van Ramshorst, B. et al. Conservative treatment of acute cholecystitis: a systematic review and pooled analysis. Surg Endosc 31, 504–515 (2017). https://doi.org/10.1007/s00464-016-5011-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-016-5011-x