Abstract
Background
The purpose of this study is the evaluation of the surgical and oncological results of laparoscopic liver resection (LLR) for hepatocellular carcinoma (HCC) by comparing laparoscopic and open liver resection (OLR) in the treatment of this disease. Retrospective analysis of laparoscopic and OLR for HCC (<5 cm) performed over a 4-year period was conducted. The LLR was done by a single surgeon.
Methods
The study was performed on patients who received liver resection for HCC between July 2007 and August 2011 in our institution. Propensity-based matched analyses were used to account for operative method selection biases. During the 4 years, 1,050 patients with HCC received an operation. Among them patients who never received TACE or RFA before surgery and had HCC (<5 cm) were selected for this study.
Results
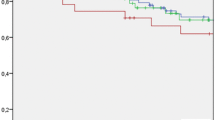
174 patients had OLR, and 58 patients underwent LLR. Patients who received LLR had lower operative time, transfusion rate, complication rate, and shorter hospital days. There were significant differences in hospital mortality and morbidity between the two groups. Dietary recovery was relatively fast in the group of LLR. Overall and disease-free survival rates during the 4 years were also not significantly different between the two groups.
Conclusions
LLR is a developing and safe technique in a select group of patients including those with malignancies, and use of this procedure is associated with short hospital stays, a rapid return to a normal diet, full mobility, and minimal morbidity, with acceptable oncological parameters. It may be an optimal method of hepatectomy in HCC (<5 cm). Further, long-term follow-up should be acquired for adequate evaluation for survival.



Similar content being viewed by others
References
Kim KH, Jung DH, Park KM, Lee YJ, Kim DY, Kim KM, Lee SG (2011) Comparison of open and laparoscopic live donor left lateral sectionectomy. Br J Surg 98:1302–1308
Panaro F, Piardi T, Cag M, Cinqualbre J, Wolf P, Audet M (2011) Robotic liver resection as a bridge to liver transplantation. JSLS 15:86–89
Buell JF, Thomas MT, Rudich S, Marvin M, Nagubandi R, Ravindra KV, Brock G, McMasters KM (2008) Experience with more than 500 minimally invasive hepatic procedures. Ann Surg 248:475–486
Vibert E, Perniceni T, Levard H, Denet C, Shahri NK, Gayet B (2006) Laparoscopic liver resection. Br J Surg 93:67–72
Cherqui D, Husson E, Hammoud R, Malassagne B, Stéphan F, Bensaid S, Rotman N, Fagniez PL (2000) Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 232:753–762
Otsuka Y, Tsuchiya M, Maeda T, Katagiri T, Isii J, Tamura A, Yamazaki K, Kubota Y, Suzuki T, Suzuki T, Kagami S, Kaneko H (2009) Laparoscopic hepatectomy for liver tumors: proposals for standardization. J Hepatobiliary Pancreat Surg 16:720–725
Troisi R, Debruyne R, Rogiers X (2009) Laparoscopic living donor hepatectomy for pediatric liver transplantation. Acta Chir Belg 109:559–562
Edwin B, Nordin A, Kazaryan AM (2011) Laparoscopic liver surgery: new frontiers. Scand J Surg 100:54–65
Ishida H, Murata N, Yamada H, Nomura T, Shimomura K, Fujioka M, Idezuki Y (2000) Influence of trocar placement and CO(2) pneumoperitoneum on port site metastasis following laparoscopic tumor surgery. Surg Endosc 14:193–197
Nguyen KT, Gamblin TC, Geller DA (2008) Laparoscopic liver resection for cancer. Future Oncol 4:661–670
Nitta H, Sasaki A, Fujita T, Itabashi H, Hoshikawa K, Takahara T, Takahashi M, Nishizuka S, Wakabayashi G (2010) Laparoscopy-assisted major liver resections employing a hanging technique: the original procedure. Ann Surg 251:450–453
Hasegawa K, Kokudo N, Imamura H, Matsuyama Y, Aoki T, Minagawa M, Sano K, Sugawara Y, Takayama T, Makuuchi M (2005) Prognostic impact of anatomic resection for hepatocellular carcinoma. Ann Surg 242:252–259
Yamamoto M, Takasaki K, Ohtsubo T, Katsuragawa H, Fukuda C, Katagiri S (2001) Effectiveness of systematized hepatectomy with Glisson’s pedicle transection at the hepatic hilus for small nodular hepatocellular carcinoma: retrospective analysis. Surgery 130:443–448
Polignano FM, Quyn AJ, de Figueiredo RS, Henderson NA, Kulli C, Tait IS (2008) Laparoscopic versus open liver segmentectomy: prospective, case-matched, intention-to-treat analysis of clinical outcomes and cost effectiveness. Surg Endosc 22:2564–2570
Topal B, Fieuws S, Aerts R, Vandeweyer H, Penninckx F (2008) Laparoscopic versus open liver resection of hepatic neoplasms: comparative analysis of short-term results. Surg Endosc 22:2208–2213
Koffron AJ, Auffenberg G, Kung R, Abecassis M (2007) Evaluation of 300 minimally invasive liver resections at a single institution: less is more. Ann Surg 246:385–392 discussion 392-394
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2,804 patients. Ann Surg 250:831–841
Farges O, Jagot P, Kirstetter P, Marty J, Belghiti J (2002) Prospective assessment of the safety and benefit of laparoscopic liver resections. J Hepatobiliary Pancreat Surg 9:242–248
Endo Y, Ohta M, Sasaki A, Kai S, Eguchi H, Iwaki K, Shibata K, Kitano S (2009) A comparative study of the long-term outcomes after laparoscopy-assisted and open left lateral hepatectomy for hepatocellular carcinoma. Surg Laparosc Endosc Percutan Tech 19:e171–e174
Papp A, Vereczkei, Lantos J, Horváth OP (2003) The effect of different levels of peritoneal CO2 pressure on bleeding time of spleen capsule injury. Surg Endosc 17:1125–1128
Jarnagin WR, Gonen M, Fong Y, DeMatteo RP, Ben-Porat L, Little S, Corvera C, Weber S, Blumgart LH (2002) Improvement in perioperative outcome after hepatic resection: analysis of 1,803 consecutive cases over the past decade. Ann Surg 236:397–406 discussion 406-407
Kooby DA, Stockman J, Ben-Porat L, Gonen M, Jarnagin WR, Dematteo RP, Tuorto S, Wuest D, Blumgart LH, Fong Y (2003) Influence of transfusions on perioperative and long-term outcome in patients following hepatic resection for colorectal metastases. Ann Surg 237:860–869 discussion 869-870
Stephenson KR, Steinberg SM, Hughes KS, Vetto JT, Sugarbaker PH, Chang AE (1988) Perioperative blood transfusions are associated with decreased time to recurrence and decreased survival after resection of colorectal liver metastases. Ann Surg 208:679–687
Soubrane O, Cherqui D, Scatton O, Stenard F, Bernard D, Branchereau S, Martelli H, Gauthier F (2006) Laparoscopic left lateral sectionectomy in living donors: safety and reproducibility of the technique in a single center. Ann Surg 244:815–820
Castaing D, Vibert E, Ricca L, Azoulay D, Adam R, Gayet B (2009) Oncologic results of laparoscopic versus open hepatectomy for colorectal liver metastases in two specialized centers. Ann Surg 250:849–855
Pilgrim CH, To H, Usatoff V, Evans PM (2009) Laparoscopic hepatectomy is a safe procedure for cancer patients. HPB (Oxford) 11:247–251
Aravalli RN, Steer CJ, Cressman EN (2008) Molecular mechanisms of hepatocellular carcinoma. Hepatology 48:2047–2063
El-Serag HB, Rudolph KL (2007) Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 132:2557–2576
Kluger MD, Cherqui D (2013) Laparoscopic resection of hepatocellular carcinoma. Recent Results Cancer Res 190:111–126
Vigano L, Laurent A, Tayar C, Tomatis M, Ponti A, Cherqui D (2009) The learning curve in laparoscopic liver resection: improved feasibility and reproducibility. Ann Surg 250:772–782
Conflict of interest
The authors have no conflicts of interest.
Disclosures
Sam-Youl Yoon, Ki-Hun Kim, Dong-Hwan Jung, Sung-Gyu Lee, and Ami Yu has no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yoon, SY., Kim, KH., Jung, DH. et al. Oncological and surgical results of laparoscopic versus open liver resection for HCC less than 5 cm: case-matched analysis. Surg Endosc 29, 2628–2634 (2015). https://doi.org/10.1007/s00464-014-3980-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-014-3980-1