Abstract
Background
The primary goal of this hospital-based retrospective multicenter case series study was to determine the incidence of large bowel full-thickness injury associated with colonoscopy in Lithuania. We assessed characteristics of patients who were treated as a result of this complication; management and outcomes were the secondary goals of this study.
Methods
The medical records of patients with iatrogenic large bowel perforations resulting from colonoscopy within the period January 1, 2007, to December 31, 2011, were retrospectively reviewed. Representatives of 14 Lithuanian public and private hospitals participated in the survey.
Results
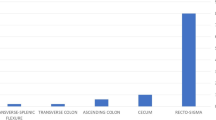
A total of 56,882 colonoscopies were performed. Forty patients (23 female and 17 male patients) were reported to have iatrogenic full-thickness large bowel injury. Diagnostic and therapeutic colonoscopies resulted in perforation for 28 of 49,795 patients and 12 of 7,087 patients, respectively. A mean age of 70 years and a female preponderance for this complication was revealed. Sigmoid colon and rectosigmoid junction was perforated in 28 patients. All patients underwent surgical management, either primary repair (70.0 %) or bowel resection (30.0 %). Postoperative complications were diagnosed in 15 patients. Immediate treatment resulted in fewer intestinal resections and shorter hospital stays (p < 0.05). Smoking [odds ratio (OR) 14.4, 95 % confidence interval (CI) 1.16–179.8] and a large size perforation site (15 ± 10 vs. 8 ± 5 mm; OR 1.19, 95 % CI 1.03–1.38) were risk factors for developing a postoperative complication after curative surgery. Six patients died. All deaths were related to diagnostic colonoscopy.
Conclusions
Total incidence of large bowel full-thickness injury in Lithuanian hospitals is 0.07 %. Incidence of this complication after diagnostic and therapeutic colonoscopies is 0.056 and 0.169 %, respectively. The most common site of perforation is sigmoid colon and rectosigmoid junction, at 70 %. Risk rises when colonoscopy is performed in low-volume practice centers. Urgent surgical management resulted in overall mortality rate of 15.0 % and morbidity of 37.5 %.



Similar content being viewed by others
References
Iqbal CW, Cullinane DC, Schiller HJ, Sawyer MD, Zietlow SP, Farley DR (2008) Surgical management and outcomes of 165 colonoscopic perforations from a single institution. Arch Surg 143(7):701–706
Lohsiriwat V (2010) Colonoscopic perforation: incidence, risk factors, management and outcome. World J Gastroenterol 16(4):425–430
Levin TR, Zhao W, Conell C, Seeff LC, Manninen DL, Shapiro JA, Schulman J (2006) Complications of colonoscopy in an integrated health care delivery system. Ann Intern Med 145:880–886
McDonnell WM (2007) Complications of colonoscopy. Ann Intern Med 147:212–213
Lohsiriwat V, Sujarittanakarn S, Akaraviputh T, Lertakyamanee N, Lohsiriwat D, Kachinthorn U (2008) Colonoscopic perforation: a report from World Gastroenterology Organization endoscopy training center in Thailand. World Gastroenterol 14:6722–6725
Teoh AY, Poon CM, Lee JF, Leong HT, Ng SS, Sung JJ, Lau JY (2009) Outcomes and predictors of mortality and stoma formation in surgical management of colonoscopic perforations: a multicenter review. Arch Surg 144:9–13
Lüning TH, Keemers-Gels ME, Barendregt WB, Tan AC, Rosman C (2007) Colonoscopic perforations: a review of 30,366 patients. Surg Endosc 21:994–997
Mai CM, Wen CC, Wen SH, Hsu KF, Wu CC, Jao SW, Hsiao CW (2010) Iatrogenic colonic perforation by colonoscopy: a fatal complication for patients with a high anesthetic risk. Int J Colorectal Dis 25(4):449–454
Dafnis G, Ekbom A, Pahlman L, Blomqvist P (2001) Complications of diagnostic and therapeutic colonoscopy within a defined population in Sweden. Gastrointest Endosc 54(3):302–309
Araghizadeh FY, Timmcke AE, Opelka FG, Hicks TC, Beck DE (2001) Colonoscopic perforations. Dis Colon Rectum 44:713–716
Gatto NM, Frucht H, Sundararajan V, Jacobson JS, Grann VR, Neugut AI (2003) Risk of perforation after colonoscopy and sigmoidoscopy: a population-based study. J Natl Cancer Inst 95:230–236
Korman LY, Overholt BF, Box T, Winker CK (2003) Perforation during colonoscopy in endoscopic ambulatory surgical centers. Gastrointest Endosc 58:554–557
Cobb WS, Heniford BT, Sigmon LB, Hasan R, Simms C, Kercher KW, Matthews BD (2004) Colonoscopic perforations: incidence, management, and outcomes. Am Surg 70:750–758
Rathgaber SW, Wick TM (2006) Colonoscopy completion and complication rates in a community gastroenterology practice. Gastrointest Endosc 64(4):556–562
Rabeneck L, Paszat LF, Hilsden RJ, Saskin R, Leddin D, Grunfeld E, Wai E, Goldwasser M, Sutradhar R, Stukel TA (2008) Bleeding and perforation after outpatient colonoscopy and their risk factors in usual clinical practice. Gastroenterology 135:1899–1906
Kang HY, Kang HW, Kim SG, Kim JS, Park KJ, Jung HC, Song IS (2008) Incidence and management of colonoscopic perforations in Korea. Digestion 78:218–223
Arora G, Mannalithara A, Singh G, Gerson LB, Triadafilopoulos G (2009) Risk of perforation from a colonoscopy in adults: a large population-based study. Gastrointest Endosc 69:654–664
Araujo SE, Seid VE, Caravatto PP, Dumarco R (2009) Incidence and management of colonoscopic colon perforations: 10 years’ experience. Hepatogastroenterology 56:1633–1636
Lohsiriwat V, Sujarittanakarn S, Akaraviputh T, Lertakyamanee N, Lohsiriwat D, Kachinthorn U (2009) What are the risk factors of colonoscopic perforations? BMC Gastroenterol 9:71
Anderson ML, Pasha TM, Leighton JA (2000) Endoscopic perforation of the colon: lessons from a 10-years study. Am J Gastroenterol 95:3418–3422
Repici A, Pellicano R, Strangio G, Danese S, Fagoonee S, Malesci A (2009) Endoscopic mucosal resection for early colorectal neoplasia: pathologic basis, procedures, and outcomes. Dis Colon Rectum 52:1502–1515
Lorenzo-Zuniga V, Vega VM, Domenech E, Manosa M, Planas R, Boix J (2010) Endoscopist experience as a risk factor for colonic complications. Colorectal Dis 12:e273–e277
Saunders BP, Fukumoto M, Halligan S, Jobling C, Moussa ME, Bartram CI, Williams CB (1996) Why is colonoscopy more difficult in women? Gastrointest Endosc 43:124–126
Waye JD (2000) Colonoscopic polypectomy. Diagn Ther Endosc 6:111–124
Lalor PF, Mann BD (2007) Splenic rupture after colonoscopy. J Soc Laparoend Surg 11:151–156
Skipworth JRA, Raptis DA, Rawal JS, Damink SO, Shankar A, Malago M, Imber C (2009) Splenic injury following colonoscopy—an underdiagnosed, but soon to increase, phenomenon? Ann R Coll Surg Engl 91:1–6
Tulchinsky H, Madhala-Givon O, Wasserberg N, Lelcuk S, Niv Y (2006) Incidence and management of colonoscopic perforations: 8 years experience. World J Gastroenterol 12:4211–4213
Castellvi J, Pi F, Sueiras A, Vallet J, Bollo J, Tomas A, Verge J, Caballero F, Iglesias C, Castro JD (2011) Colonoscopic perforation: useful parameters for early diagnosis and conservative treatment. Int J Colorectal Dis 26:1183–1190
Avgerinos DV, Llaguna OH, Lo AY, Leitman IM (2008) Evolving management of colonoscopic perforations. J Gastrointest Surg 12(10):1783–1789
Yoshikane H, Hidano H, Sakakibara A, Ayakawa T, Mori S, Kawashima H, Goto H, Niwa Y (1997) Endoscopic repair by clipping of iatrogenic colonic perforation. Gastrointest Endosc 46:464–466
Magdeburg R, Collet P, Post S, Kaehler G (2008) Endoclipping of iatrogenic colonic perforation to avoid surgery. Surg Endosc 62(5):791–795
Jovanovic I, Zimmermann L, Fry LC, Mönkemüller K (2011) Feasibility of endoscopic closure of an iatrogenic colon perforation occurring during colonoscopy. Gastrointest Endosc 73(3):550–555
Alfonso-Ballester R, Lo Pez-Mozos F (2006) Laparoscopic treatment of endoscopy sigmoid colon perforation: a case report and literature review. Surg Laparosc Endosc Percutan Tech 16:44–46
Rumstadt B, Schilling D, Sturm J (2008) The role of laparoscopy in the treatment of complications after colonoscopy. Surg Laparosc Endosc Percutan Tech 18(6):561–564
Bleier JI, Moon V, Feingold D, Whelan RL, Arnell T, Sonoda T, Milsom JW, Lee SW (2008) Initial repair of iatrogenic colon perforation using laparoscopic methods. Surg Endosc 22:646–649
Hansen AJ, Tesier DJ, Anderson ML, Schlinkert RT (2007) Laparoscopic repair of colonoscopic perforations: indications and guidelines. J Gastrointest Surg 11:655–659
Iqbal CW, Chun YS, Farley DR (2005) Colonoscopic perforations: a retrospective review. J Gastrointest Surg 9:1229–1235
Acknowledgments
We would like to acknowledge the invaluable contribution of Varut Lohsiriwat, Department of Surgery, Siriraj Hospital, Mahidol University, Bangkok, Thailand, for participation in designing this study. Special thanks to Arturas Razbadauskas, Klaipeda Jurininku Hospital, Klaipeda, Lithuania; Vincas Abaliksta, Siauliai Republican Hospital, Siauliai, Lithuania; and Gintautas Puteikis, Utena City Hospital, Utena, Lithuania, for kind collaboration in providing the addition data.
Disclosures
Drs. Samalavicius, Kazanavicius, Lunevicius, Poskus, Valantinas, Stanaitis, Grigaliunas, Gradauskas, Venskutonis, Samuolis, Sniuolis, Gajauskas, Kaselis, Leipus, and Radziunas have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Samalavicius, N.E., Kazanavicius, D., Lunevicius, R. et al. Incidence, risk, management, and outcomes of iatrogenic full-thickness large bowel injury associated with 56,882 colonoscopies in 14 Lithuanian hospitals. Surg Endosc 27, 1628–1635 (2013). https://doi.org/10.1007/s00464-012-2642-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-012-2642-4