Abstract
Introduction
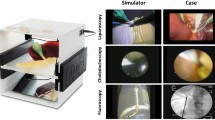
Laparoscopic common bile duct exploration (LCBDE) is an effective, single-stage treatment for choledocholithiasis. However, LCBDE requires specific cognitive and technical skills, is infrequently performed by residents, and currently lacks suitable training and assessment modalities outside of the operating room. To address this gap in training, a simulator model for transcystic and transcholedochal LCBDE was developed and evaluated.
Methods
A procedure algorithm incorporating essential cognitive and technical steps of LCBDE was developed, along with a physical model to allow performance of a simulated procedure. Modified Objective Structured Assessment of Technical Skills (OSATS) rating scales were developed to assess performance on the model. Construct validity was assessed by comparing the performance of novices (residents and surgeons without LCBDE experience) versus experienced subjects (surgeons with previous LCBDE experience). Concurrent validity was assessed by comparing scores from the LCBDE scales to those from the standard OSATS scale. Internal consistency and interrater reliability were assessed by comparing performance scores assigned by three independent raters.
Results
Sixteen novices and five experienced subjects performed simulated procedures, with novices scoring lower than experienced subjects on both transcystic (20 ± 3 vs. 33 ± 2 [possible score range, 0–45], p < 0.001) and transcholedochal (25 ± 8 vs. 42 ± 3 [possible score range, 0–53], p < 0.001) rating scales. Scores on the rating scales correlated significantly with scores from the standard OSATS scale. Internal consistency and interrater reliability of the LCBDE rating scales were favorable.
Conclusions
The LCBDE simulator is a low-cost yet realistic physical model that allows performance and evaluation of technical skills required for LCBDE. The LCBDE rating scales show evidence of construct validity, concurrent validity, internal consistency, and interrater reliability. Use of the LCBDE model and associated rating scales allows procedure-specific feedback for trainees and could be used to improve current training.




Similar content being viewed by others
References
Tranter SE, Thompson MH (2003) Spontaneous passage of bile duct stones: frequency of occurrence and relation to clinical presentation. Ann R Coll Surg Engl 85:174–177
Rhodes M, Sussman L, Cohen L, Lewis MP (1998) Randomised trial of laparoscopic exploration of common bile duct versus postoperative endoscopic retrograde cholangiography for common bile duct stones. Lancet 351:159–161
Tranter SE, Thompson MH (2002) Comparison of endoscopic sphincterotomy and laparoscopic exploration of the common bile duct. Br J Surg 89:1495–1504
Christensen M, Matzen P, Schulze S, Rosenberg J (2004) Complications of ERCP: a prospective study. Gastrointest Endosc 60:721–731
Martin DJ, Vernon DR, Toouli J (2006) Surgical versus endoscopic treatment of bile duct stones. Cochrane Database Syst Rev:CD003327
Poulose BK, Arbogast PG, Holzman MD (2006) National analysis of in-hospital resource utilization in choledocholithiasis management using propensity scores. Surg Endosc 20:186–190
Bell RH Jr, Biester TW, Tabuenca A, Rhodes RS, Cofer JB, Britt LD, Lewis FR Jr (2009) Operative experience of residents in U.S. general surgery programs: a gap between expectation and experience. Ann Surg 249:719–724
Chung R, Pham Q, Wojtasik L, Chari V, Chen P (2003) The laparoscopic experience of surgical graduates in the United States. Surg Endosc 17:1792–1795
Ponsky JL (2010) Laparoscopic biliary surgery: will we ever learn? Surg Endosc 24:2367
Doraiswamy A, Phillips EH (2009) Surgery of the extrahepatic bile ducts. In: Swanstrom LL, Eubanks WS, Soper NJ (eds) Mastery of endoscopic and laparoscopic surgery. Lippincott Williams & Wilkins, Philadelphia
Reznick R, Regehr G, MacRae H, Martin J, McCulloch W (1997) Testing technical skill via an innovative “bench station” examination. Am J Surg 173:226–230
Watson MJ (2004) Laparoscopic CBDE. SAGES Top 14: procedures every practicing surgeon should know, Cine-Med, Inc., Woodbury
Scott DJ, Dunnington GL (2008) The new ACS/APDS skills curriculum: moving the learning curve out of the operating room. J Gastrointest Surg 12:213–221
Scott DJ, Watson MJ. American College of Surgeons: Division of Education: Surgical Skills Curriculum Information
Martin IJ, Bailey IS, Rhodes M, O’Rourke N, Nathanson L, Fielding G (1998) Towards T-tube free laparoscopic bile duct exploration: a methodologic evolution during 300 consecutive procedures. Ann Surg 228:29–34
Lyass S, Phillips EH (2006) Laparoscopic transcystic duct common bile duct exploration. Surg Endosc 20(Suppl 2):S441–S445
Fanelli RD, Gersin KS (2001) Laparoscopic endobiliary stenting: a simplified approach to the management of occult common bile duct stones. J Gastrointest Surg 5:74–80
Cameron BH, O’Regan PJ, Anderson DL (1994) A pig model for advanced laparoscopic biliary procedures. Surg Endosc 8:1423–1424
Crist DW, Davoudi MM, Parrino PE, Gadacz TR (1994) An experimental model for laparoscopic common bile duct exploration. Surg Laparosc Endosc 4:336–339
Watson DI, Treacy PJ, Williams JA (1995) Developing a training model for laparoscopic common bile duct surgery. Surg Endosc 9:1116–1118
Common Bile Duct Exploration Model | Practice Common Bile Duct Exploration | Simulab Corporation
Bittner JG, Mellinger JD, Imam T, Schade RR, Macfadyen BV Jr (2010) Face and construct validity of a computer-based virtual reality simulator for ERCP. Gastrointest Endosc 71:357–364
Acknowledgments
This work was supported by a 2010 SAGES Education and Research Foundation Grant. The authors thank the SAGES Education and Research Foundation for grant support for the project and Cook Medical and Karl-Storz Endoscopy for donating some of the instruments used in this study.
Disclosures
Dr. Santos, Dr. Nagle, Deborah Rooney, and Taylor Reif have no conflicts of interest or financial ties to disclose. Dr. Hungness has a consulting agreement with Olympus and is a member of the scientific advisory board for Ethicon Endo-Surgery. Dr. Soper is a member of scientific advisory boards for Covidien, Terumo, Transenterix, Boston Scientific, and EndoGastric Solutions, Inc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Santos, B.F., Reif, T.J., Soper, N.J. et al. Development and evaluation of a laparoscopic common bile duct exploration simulator and procedural rating scale. Surg Endosc 26, 2403–2415 (2012). https://doi.org/10.1007/s00464-012-2213-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-012-2213-8