Abstract
Background
Laparoscopic inguinal hernia repair is still not the gold standard for patients with inguinal hernia. The aim of this study was to compare testicular dysfunction, incidence and factors influencing chronic groin pain, and quality of life after laparoscopic and open mesh repair.
Methods
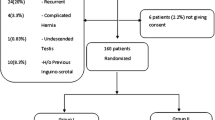
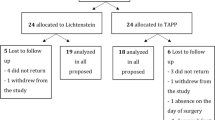
One hundred twenty patients were studied in a prospective randomized trial. One hundred seventeen patients completed the required follow-up, 60 following laparoscopic repair and 57 following open repair. Testicular functions were assessed by testicular volume, blood flow, and hormones, and quality of life was assessed with Short Form 36 version 2 preoperatively and postoperatively at 3 months. Pain was assessed at different time intervals preoperatively and postoperatively.
Results
Preoperative profiles of both groups were well matched. A significant decrease in testicular volume (p = 0.01) and less improvement in blood flow (p = 0.048) was seen after open repair. There was also a significant reduction in serum testosterone level (p = 0.02) with a significant increase in FSH and LH level (p < 0.001); however, there was no testicular atrophy. Incidence and severity of chronic groin pain were significantly less after laparoscopic repair during normal and strenuous activities, though they were similar to those after open repair during rest after 3 months postoperatively. Age, preoperative pain, pain at 1 week, and open repair were found to be independent risk factors for chronic pain on multivariate analysis. Quality of life was significantly better postoperatively in terms of physical functions, role physical, bodily pain, and general health after laparoscopic repair.
Conclusion
Laparoscopic repair seems favorable in terms of better preservation of testicular functions, lower incidence of acute and chronic groin pain, and significant improvement in quality of life when compared to open repair. Younger age, preoperative pain, pain after 1 week postoperatively, and open mesh repair were found to be significant risk factors for chronic groin pain.






Similar content being viewed by others
References
Devlin HB (1995) Trends in hernia surgery in the land of Astley Cooper. In: Soper NJ (ed) Problems in general surgery, vol 12. Lippincott Raven, Philadelphia, pp 85–92
Kingsnorth A, LeBlanc K (2003) Hernias: inguinal and incisional. Lancet 362:1561–1571
Hernia Trialists Collaboration EU (2002) Repair of groin hernia with synthetic mesh: meta-analysis of randomized controlled trials. Ann Surg 235:322–332
McCormack K, Scott NW, Go PM, Ross S, Grant AM, EU Hernia Trialists Collaboration (2003) Laparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database Syst Rev (1):CD001785
Reid I, Devlin HE (1994) Testicular atrophy as a consequence of inguinal hernia repair. Br J Surg 81:91–93
Zieren J, Beyersdorff D, Beier KM, Müller JM (2001) Sexual function and testicular perfusion after inguinal hernia repair with mesh. Am J Surg 181:204–206
Bay-Nielsen M, Perkins FM, Kehlet H, Database Danish Hernia (2001) Pain and functional impairment 1 year after inguinal herniorrhaphy: a nationwide questionnaire study. Ann Surg 233:1–7
Bozuk M, Schuster R, Stewart D, Hicks K, Greaney G, Waxman K (2003) Disability and chronic pain after open mesh and laparoscopic inguinal hernia repair. Am Surg 69:839–841
Laparoscopic The MRC, Group Groin Hernia Trial (1999) Laparoscopic versus open repair of groin hernia: a randomized comparison. Lancet 354:185–190
Poobalan AS, Bruce J, Smith WC, King PM, Krukowski ZH, Chambers WA (2003) A review of chronic pain after inguinal herniorrhaphy. Clin J Pain 19:48–54
Korolija D, Sauerland S, Wood-Dauphinee S, Abbou CC, Eypasch E, Caballero MG, Lumsden MA, Millat S, Monson JR, Nilsson G, Pointner R, Schwenk W, Shamiyeh A, Szold A, Targarona E, Ure B, Neugebauer E (2004) Evaluation of quality of life after laparoscopic surgery: evidence-based guidelines of the European Association for Endoscopic Surgery. Surg Endosc 18:879–897
Mathur S, Barlett JRA, Gilkison W, Krishna G (2006) Quality of life assessment in patients with inguinal hernia. ANZ J Surg 76:491–493
Hope WW, Lincourt AE, Newcomb L, Schmelzer TS, Kercher KW, Heniford BT (2008) Comparing quality of life outcomes in symptomatic patients undergoing laparoscopic or open ventral hernia repair. J Laparosc Adv Surg Tech 18:567–571
Gholghesaei M, Langeveld HR, Veldkamp R, Bonjer HJ (2005) Cost and quality of life after endoscopic repair of inguinal hernia vs open tension free repair. Surg Endosc 19:816–821
Nyhus LM (1993) Individualization of hernia repair: a new era. Surgery 114:102
Kulaylat MN, Dayton MT (2008) Surgical Complications. In: Townsend CM, Beauchamp RD, Evers BM, Mattox KL (eds) Sabiston Textbook of Surgery. Saunders, Philadelphia, p 331
McCarthy M Jr, Chang CH, Pickard AS, Giobbie-Hurder A, Price DD, Jonasson O, Gibbs J, Fitzgibbons R, Neumayer L (2005) Visual analogue scales for assessing surgical pain. J Am Coll Surg 201:245–252
International Association for the Study of Pain Subcommittee on Taxonomy (1986) Classification of chronic pain: Description of chronic pain syndromes and definition of pain terms. Pain 3:S1-S226
Rutkow IM (2003) Demographic and socioeconomic aspects of hernia repair in the United States in 2003. Surg Clin North Am 83:1045–1051
Bay-Nielsen M, Kehlet H, Strand L, Malmstrom J, Andersen FH, Wara P, Juul P, Callesen T, Danish Hernia Database Collaboration (2001) Quality assessment of 26304 herniorrhaphies in Denmark: a prospective study. Lancet 358:1124–1128
Schmedt CG, Sauerland S, Bittner R (2005) Comparison of endoscopic procedures vs Lichtenstein and other open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Surg Endosc 19:188–199
Gould J (2008) Laparoscopic versus open inguinal hernia repair. Surg Clin North Am 88:1073–1081
Junge K, Binnebösel M, Rosch R, Öttinger A, Stumpf M, Mühlenbruch G, Schumpelick V, Klinge U (2008) Influence of mesh materials on the integrity of the vas deferens following Lichtenstein hernioplasty: an experimental model. Hernia 12:621–626
Akbulut G, Serteser M, Yucel A, Degirmenci B, Yilmaz S, Polat C, San O, Dilek ON (2003) Can laparoscopic hernia repair alter function and volume of testis? Randomized clinical trial. Surg Laparosc Endosc Percutan Tech 13:377–381
Ersin S, Aydin D, Makay O, Icoz G, Tamsel S, Sozbilen M, Killi R (2006) Is testicular perfusion influenced during laparoscopic inguinal hernia surgery? Surg Endosc 20:685–689
Beddy P, Ridgway PF, Geoghegan T, Peirce C, Govender P, Keane FB, Torreggiani WC, Conlon KC (2006) Inguinal hernia repair protects testicular function: a prospective study of open and laparoscopic herniorrhaphy. J Am Coll Surg 203:17–23
Dilek ON, Yucel A, Akbulut G, Degirmenci B (2005) Are there adverse effects of herniorrhaphy techniques on testicular perfusion? Evaluation by color Doppler ultrasonography. Urol Int 75:167–169
Koksal N, Altinli E, Sumer A, Celik A, Onur E, Demir K, Sumer H, Kus D (2010) Impact of herniorrhaphy technique on testicular perfusion: results of a prospective study. Surg Laparosc Endosc Percutan Tech 20:186–189
Celik AS, Memmi N, Celebi F, Guzey D, Celik A, Kaplan R, Oncu M (2009) Impact of slit and nonslit mesh technique on testicular perfusion and volume in the early and late postoperative period of the totally extraperitoneal preperitoneal technique in patients with inguinal hernia. Am J Surg 2:287–291
Peeters E, Spiessens C, Oyen R, De Wever L, Vanderschueren D, Penninckx F, Miserez M (2010) Laparoscopic inguinal hernia repair in men with lightweight meshes may significantly impair sperm motility: a randomized controlled trial. Ann Surg 252:240–246
Elster EA, Hale DA, Mannon RB, Cendales LC, Kleiner D, Swanson SJ, Kirk AD (2005) Surgical transplant physical examination: correlation of renal resistance index and biopsy-proven chronic allograft nephropathy. J Am Coll Surg 200:552–556
Neumayer L, Hurdcr AG, Jonasson O, Fitzgibbons R, Dunlop D., Gibbs J, Reda D, Henderson W; Veterans Affairs Cooperative Studies Program 456 Investigators (2004) Open mesh vs laparoscopic mesh repair of inguinal hernia. N Engl J Med 350:1819-1827
Aasvang E, Kehlat H (2005) Chronic postoperative pain: the case of inguinal herniorrhaphy. Br J Anaesth 95:69–76
Cunningham J, Temple WJ, Mitchell P, Nixon JA, Preshaw RM, Hagen NA (1996) Cooperative hernia study. Pain in the post repair patient. Ann Surg 224:598–602
Courtney CA, Duffy K, Serpell MG, O’Dwyer PJ (2002) Outcome of patients with severe chronic pain following repair of groin hernia. Br J Surg 89:1310–1314
Wright D, Paterson C, Scott N, Hair A, O’Dwyer PJ (2002) Five-year follow-up of patients undergoing laparoscopic or open groin hernia repair: a randomized controlled trial. Ann Surg 235:333–337
Salcedo-Wasicek MC, Thirlby RC (1995) Postoperative course after inguinal herniorrhaphy. A case-controlled comparison of patients receiving workers’ compensation vs patients with commercial insurance. Arch Surg 130:29–32
Page B, Paterson C, Young D, O’Dwyer PJ (2002) Pain from primary inguinal hernia and the effect of repair on pain. Br J Surg 89:1315–1318
Liem MS, van Duyn EB, van der Graaf Y, van Vroonhoven TJ; Coala Trial Group (2003) Recurrences after conventional anterior and laparoscopic inguinal hernia repair: a randomized comparison. Ann Surg 237:136–141
Lau H, Patil NG, Yuen WK, Lee F (2003) Prevalence and severity of chronic groin pain after endoscopic totally extraperitoneal inguinal hernioplasty. Surg Endosc 17:1620–1623
Heikkinen T, Bringman S, Ohtonen P, Kunelius P, Haukipuro K, Hulkko A (2004) Five-year outcome of laparoscopic and Lichtenstein hernioplasties. Surg Endosc 18:518–522
Callesen T, Bech K, Kehlet H (1999) Prospective study of chronic pain after groin hernia repair. Br J Surg 86:1528–1531
Kehlet H, Bay-Nielsen M, Kingsnorth A (2002) Chronic postherniorrhaphy pain—a call for uniform assessment. Hernia 6:178–181
Perkins FM, Kehlet H (2000) Chronic pain as an outcome of surgery. A review of predictive factors. Anesthesiology 93:1123–1133
Mussack T, Ladurner R, Vogel T, Lienemann A, Eder-Willwohl A, Hallfeldt KK (2006) Health-related quality of life changes after laparoscopic and open incisional hernia repair: a matched pair analysis. Surg Endosc 20:410–413
McCormack K, Wake B, Perez J, Fraser C, Cook J, McIntosh E, Vale L, Grant A (2005) Laparoscopic surgery for inguinal hernia repair: systematic review of effectiveness and economic evaluation. Health Technol Assess 9:1–203
de Jonge P, Lloyd A, Horsfall L, Tan R, O’Dwyer PJ (2008) The measurement of chronic pain and health-related quality of life following inguinal hernia repair: a review of the literature. Hernia 12:561–569
Srsen D, Druzijanić N, Pogorelić Z, Perko Z, Juricić J, Kraljević D, Krnić D, Bilan K, Mimica Z (2008) Quality of life analysis after open and laparoscopic inguinal hernia repair–retrospective study. Hepatogastroenterology 55:2112–2115
Myers E, Browne KM, Kavanagh DO, Hurley M (2010) Laparoscopic (TEP) versus Lichtenstein inguinal hernia repair: a comparison of quality-of-life outcomes. World J Surg 34:2059–2064
Disclosures
Drs. Anand Narayan Singh, Virinder Kumar Bansal, M. C. Misra, Subodh Kumar, S. Rajeshwari, Atin Kumar, Rajesh Sagar, and Anand Kumar have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Singh, A.N., Bansal, V.K., Misra, M.C. et al. Testicular functions, chronic groin pain, and quality of life after laparoscopic and open mesh repair of inguinal hernia: a prospective randomized controlled trial. Surg Endosc 26, 1304–1317 (2012). https://doi.org/10.1007/s00464-011-2029-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-2029-y