Abstract
Background
Long-lasting minimally invasive procedures are increasingly used for children. However, the hemodynamic effects of a prolonged carbon dioxide (CO2) pneumoperitoneum (PP) on small infants are poorly understood and may differ from the effects on adolescents. This study aimed to detect and compare these effects in neonatal and adolescent pigs.
Methods
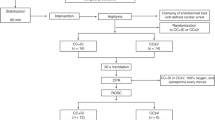
Six neonatal pigs weighing 5.6–6.4 kg and six adolescent pigs weighing 51–57 kg underwent a prolonged CO2 PP of 180 min. Five neonatal pigs weighing 5.7–6.6 kg underwent sham PP as an additional control group. All the animals received crystalloid electrolyte solution at 10 ml/kg/h during the experiments. After CO2 decompression, all the animals were monitored for a further 120 min. The end points of the study were mean arterial pressure (MAP), central venous pressure (CVP), and cardiac index (CI). The parameters were assessed after a 60-min resting phase (i.e., after initial placement of catheters in the jugular vein, the carotid artery, and the femoral artery four times during CO2 PP and three times afterward.
Results
The comparison of neonates and adolescent pigs showed that neonates had a significantly more pronounced decrease in MAP during CO2 PP (88.1 ± 2.7% of baseline vs 95.1 ± 1.6%; p < 0.05) and the recovery period (71 ± 5.1% vs 86.4 ± 1.4%; p < 0.05). Differences in CVP changes between the neonatal and adolescent pigs during and after CO2 PP were not significant. For the neonates, the decrease in CI was most pronounced during the recovery period after decompression of the CO2 PP and significantly less than in adolescents (84.3 ± 3.3% of baseline vs 97.4 ± 4.5%; p < 0.05). The neonates with sham PP did not show any significant MAP, CVP, or CI changes during the experiments.
Conclusions
A prolonged CO2 PP induces hypotension and cardiac depression in neonatal but not in adolescent pigs. Thus, intensive monitoring during prolonged laparoscopic procedures and particularly afterward may be mandatory for neonates.




Similar content being viewed by others
References
Alishahi S, Francis N, Crofts S, Duncan L, Bickel A, Cuschieri A (2001) Central and peripheral adverse hemodynamic changes during laparoscopic surgery and their reversal with a novel intermittent sequential pneumatic compression device. Ann Surg 233:176–182
Bax NM (2005) Laparoscopic surgery in infants and children. Eur J Pediatr Surg 15:319–324
Bickel A, Drobot A, Aviram M, Eitan A (2007) Validation and reduction of the oxidative stress following laparoscopic operations: a prospective randomized controlled study. Ann Surg 246:31–35
Durkin ET, Shaaban AF (2008) Recent advances and controversies in pediatric laparoscopic surgery. Surg Clin North Am 88:1101–1119
Gerges FJ, Kanazi GE, Jabbour-Khoury SI (2006) Anesthesia for laparoscopy: a review. J Clin Anesth 18:67–78
Harrington S, Simmons K, Thomas C, Scully S (2008) Pediatric laparoscopy. AORN J 88:211–236
Kalfa N, Allal H, Raux O, Lopez M, Forgues D, Guibal MP, Picaud JC, Galifer RB (2005) Tolerance of laparoscopy and thoracoscopy in neonates. Pediatrics 116:e785–e791
Kalfa N, Allal H, Raux O, Lardy H, Varlet F, Reinberg O, Podevin G, Héloury Y, Becmeur F, Talon I, Harper L, Vergnes P, Forgues D, Lopez M, Guibal MP, Galifer RB (2007) Multicentric assessment of the safety of neonatal videosurgery. Surg Endosc 21:303–308
Meininger D, Westphal K, Bremerich DH, Runkel H, Probst M, Zwissler B, Byhahn C (2008) Effects of posture and prolonged pneumoperitoneum on hemodynamic parameters during laparoscopy. World J Surg 32:1400–1405
Metzelder ML, Jesch N, Dick A, Kuebler J, Petersen C, Ure BM (2006) Impact of prior surgery on the feasibility of laparoscopic surgery for children: a prospective study. Surg Endosc 20:1733–1737
Osthaus WA, Huber D, Baeumker C, Witt L, Metzelder M, Kuebler J, Suempelmann R (2008) Plasma volume replacement with HES 130/0.42 obviates negative side effects of pneumoperitoneum in piglets. Paediatr Anaesth 18:922–928
Suempelmann R, Schuerholz T, Marx G, Jesch NK, Osthaus WA, Ure BM (2006) Hemodynamic changes during acute elevation of intraabdominal pressure in rabbits. Paediatr Anaesth 16:1262–1267
Suempelmann R, Schuerholz T, Marx G, Haertel D, Hecker H, Ure BM, Jesch NK (2006) Haemodynamic, acid-base, and blood volume changes during prolonged low pressure pneumoperitoneum in rabbits. Br J Anaesth 96:563–568
Struthers AD, Cuschieri A (1998) Cardiovascular consequences of laparoscopic surgery. Lancet 352:568–570
Travassos DV, Bax NM, Van der Zee DC (2007) Duhamel procedure: a comparative retrospective study between an open and a laparoscopic technique. Surg Endosc 21:2163–2165
Truchon R (2004) Anaesthetic considerations for laparoscopic surgery in neonates and infants: a practical review. Best Pract Res Clin Anaesthesiol 18:343–355
Ure BM, Schier F, Schmidt AI, Nustede R, Petersen C, Jesch NK (2005) Laparoscopic resection of congenital choledochal cyst, choledochojejunostomy, and extraabdominal Roux-en-Y anastomosis. Surg Endosc 19:1055–1057
Ure BM, Suempelmann R, Metzelder MM, Kuebler J (2007) Physiological responses to endoscopic surgery in children. Semin Pediatr Surg 16:217–223
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Metzelder, M.L., Kuebler, J.F., Huber, D. et al. Cardiovascular responses to prolonged carbon dioxide pneumoperitoneum in neonatal versus adolescent pigs. Surg Endosc 24, 670–674 (2010). https://doi.org/10.1007/s00464-009-0654-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0654-5