Abstract
Background
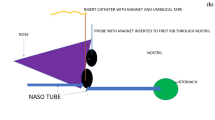
Percutaneous endoscopic gastrostomy (PEG) tubes are often placed in head and neck cancer patients to provide nutritional support, but studies have found the complication rates to be higher than other subsets of patients who undergo PEG placement. Complication rates as high as 50% have been reported, with the bulk of these complications being PEG site issues (i.e., cellulitis, abscess, fascitis, and tumor implantation). Because the pull technique has been the primary technique used, the theory is that the transoral tube passage is the source of the complications in these patients. Alternatively, the introducer technique uses a transabdominal approach to place the device, avoiding any tube contamination by upper aerodigestive organisms or tumor cells. At our institution, this technique has been used exclusively for head and neck cancer patients and this article reports our experience.
Methods
One hundred forty-nine head and neck cancer patients who had a prophylactic PEG tube placed were reviewed from January 1, 1999 to December 31, 2003. The rates of placement success, morbidity, and complications were determined.
Results
Successful placement was achieved in 148 (99%) patients without any PEG-related deaths. Overall, 17 complications (11%) occurred, with only one major complication (0.7%) identified. PEG site infections were uncommon with only five cases (3.4%) and all were mild cellulitis.
Conclusions
The introducer technique is the safest method for PEG tube placement in head and neck cancer patients. The overall rate of complications is low and PEG site infectious complications are rare. The introducer technique should be the method of choice for PEG tubes in head and neck cancer patients.

Similar content being viewed by others
References
Akkersdijk WL, van Bergeijk JD, van Egmond T, Mulder CJ, van Berge Henegouwen GP, van deer Werken C, van Erpecum KJ (1995) Percutaneous endoscopic gastrostomy (PEG): comparison of push and pull methods and evaluation of antibiotic prophylaxis. Endoscopy 27(4): 313–316
Alverdy JC, Aoys E, Moss GS (1988) Total parenteral nutrition promotes bacterial translocation from the gut. Surgery 104(2): 185–190
Baredes S, Behin D, Deitch E (2004) Percutaneous endoscopic gastrostomy tube feeding in patients with head and neck cancer. Ear Nose Throat J 83(6): 417–419
Beaver ME, Myers JN, Griffenberg L, Waugh K (1998) Percutaneous fluoroscopic gastrostomy tube placement in patients with head and neck cancer. Arch Otolaryngol Head Neck Surg 124(10): 1141–1144
Border JR, Hassett J, LaDuca J, Seibel R, Steinberg S, Mille B, Losi P, Border D (1987) The gut origin septic states in blunt multiple trauma (ISS = 40) in the ICU. Ann Surg 206(4): 427–448
Bozzetti F (2002) Rationale and indications for preoperative feeding of malnourished surgical cancer patients. Nutrition 18(11-12): 953–959
Brown AS, Mueller PR, Ferrucci JT Jr (1986) Controlled percutaneous gastrostomy: nylon T-fastener for fixation of the anterior gastric wall. Radiology 158(2): 543–545
Bushnell L, White TW, Hunter JG (1991) Metastatic implantation of laryngeal carcinoma at a PEG exit site. Gastrointest Endosc 37(4): 480–482
Capra S, Ferguson M, Ried K (2001) Cancer: impact of nutrition intervention outcome—nutrition issues for patients. Nutrition 17(9): 769–772
Chandu A, Smith AC, Douglas M (2003) Percutaneous endoscopic gastrostomy in patients undergoing resection for oral tumors: a retrospective review of complications and outcomes. J Oral Maxillofac Surg 61(11): 1279–1284
Cohen J, Lefor AT (2001) Nutrition support and cancer. Nutrition 17(7–8): 698–699
Cruz I, Mamel JJ, Brady PG, Cass-Garcia M (2005) Incidence of abdominal wall metastasis complicating PEG tube placement in untreated head and neck cancer. Gastrointest Endosc 62(5): 708-711; quiz 752, 753
de Luis DA, Aller R, Izaola O, Cuellar L, Terroba MC (2002) Postsurgery enteral nutrition in head and neck cancer patients. Eur J Clin Nutr 56(11): 1126-1129
Ehrsson YT, Langius-Eklof A, Bark T, Laurell G (2004) Percutaneous endoscopic gastrostomy (PEG)—a long-term follow-up study in head and neck cancer patients. Clin Otolaryngol Allied Sci 29(6): 740–746
Gauderer MW, Ponsky JL, Izant RJ Jr (1980) Gastrostomy without laparotomy: a percutaneous endoscopic technique. J Pediatr Surg 15(6): 872–875
Gossner L, Keymling J, Hahn EG, Ell C (1999) Antibiotic prophylaxis in percutaneous endoscopic gastrostomy (PEG): a prospective randomized clinical trial. Endoscopy 31(2): 119–124
Hunter JG (2003) Tumor implantation at PEG exit sites in head and neck cancer patients: how much evidence is enough? J Clin Gastroenterol 37(4): 280
Keymling M (1994) Technical aspects of enteral nutrition. Gut 35(1 Suppl): S77–S80
Kozarek RA, Ball TJ, Ryan JA Jr (1986) When push comes to shove: a comparison between two methods of percutaneous endoscopic gastrostomy. Am J Gastroenterol 81(8): 642–646
Lobato-Mendizabal E, Lopez-Martinez B, Ruiz-Arguelles GJ (2003) A critical review of the prognostic value of the nutritional status at diagnosis in the outcome of therapy of children with acute lymphoblastic leukemia. Rev Invest Clin 55(1): 31–35
Logemann JA, Bytell DE (1979) Swallowing disorders in three types of head and neck surgical patients. Cancer 44(3): 1095–1105
Maetani I, Tada T, Ukita T, Inoue H, Sakai Y, Yoshikawa M (2003) PEG with introducer or pull method: a prospective randomized comparison. Gastrointest Endosc 57(7): 837–841
Maetani I, Yasuda M, Seike M, Ikeda M, Tada T, Ukita T, Sakai Y (2005) Efficacy of an overtube for reducing the risk of peristomal infection after PEG placement: a prospective, randomized comparison study. Gastrointest Endosc 61(4): 522–527
Martini DV, Har-El G, Lucente FE, Slavit DH (1997) Swallowing and pharyngeal function in postoperative pharyngeal cancer patients. Ear Nose Throat J 76(7): 450–453, 456
Murry T, Madasu R, Martin A, Robbins KT (1998) Acute and chronic changes in swallowing and quality of life following intraarterial chemoradiation for organ preservation in patients with advanced head and neck cancer. Head Neck 20(1): 31–37
Robertson FM, Crombleholme TM, Latchaw LA, Jacir NN (1996) Modification of the “push” technique for percutaneous endoscopic gastrostomy in infants and children. J Am Coll Surg 182(3): 215–218
Russell TR, Brotman M, Norris F (1984) Percutaneous gastrostomy. A new simplified and cost-effective technique. Am J Surg 148(1): 132-137
Sabnis A, Liu R, Chand B, Ponsky J (2006) SLiC technique. A novel approach to percutaneous gastrostomy. Surg Endosc 20(2): 256–262
Saunders JR Jr, Brown MS, Hirata RM, Jaques DA (1991) Percutaneous endoscopic gastrostomy in patients with head and neck malignancies. Am J Surg 162(4): 381–383
Sharma P, Berry SM, Wilson K, Neale H, Fink AS (1994) Metastatic implantation of an oral squamous-cell carcinoma at a percutaneous endoscopic gastrostomy site. Surg Endosc 8(10): 1232–1235
Thakore JN, Mustafa M, Suryaprasad S, Agrawal S (2003) Percutaneous endoscopic gastrostomy associated gastric metastasis. J Clin Gastroenterol 37(4): 307–311
Thompson JS, Vaughan WP, Forst CF, Jacobs DL, Weekly JS, Rikkers LF (1987) The effect of the route of nutrient delivery on gut structure and diamine oxidase levels. JPEN J Parenter Enteral Nutr 11(1): 28–32
Torosian MH, Rombeau JL (1980) Feeding by tube enterostomy. Surg Gynecol Obstet 150(6): 918–927
Tucker AT, Gourin CG, Ghegan MD, Porubsky ES, Martindale RG, Terris DJ (2003) ‘Push’ versus ‘pull’ percutaneous endoscopic gastrostomy tube placement in patients with advanced head and neck cancer. Laryngoscope 113(11): 1898–1902
Twomey PL, Patching SC (1985) Cost-effectiveness of nutritional support. JPEN J Parenter Enteral Nutr 9(1): 3–10
van Erpecum KJ, Akkersdijk WL, Warlam-Rodenhuis CC, van Berge Henegouwen GP, van Vroonhoven TJ (1995) Metastasis of hypopharyngeal carcinoma into the gastrostomy tract after placement of a percutaneous endoscopic gastrostomy catheter. Endoscopy 27(1): 124–127
Vokes EE, Kies MS, Haraf DJ, Stenson K, List M, Humerickhouse R, Dolan ME, Pelzer H, Sulzen L, Witt ME, Hsieh YC, Mittal BB, Weichselbaum RR (2000) Concomitant chemoradiotherapy as primary therapy for locoregionally advanced head and neck cancer. J Clin Oncol 18(8): 1652–1661
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Foster, J.M., Filocamo, P., Nava, H. et al. The introducer technique is the optimal method for placing percutaneous endoscopic gastrostomy tubes in head and neck cancer patients. Surg Endosc 21, 897–901 (2007). https://doi.org/10.1007/s00464-006-9068-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-006-9068-9