Abstract
Purpose
The purpose of this study was to investigate and analyze the level of actual participation and perceived importance of shared decision-making on treatment and care of lung cancer patients, to compare their differences and to explore their influencing factors.
Methods
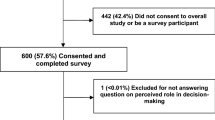
A total of 290 lung cancer patients were collected from oncology and thoracic surgery departments of a comprehensive medical center in Qingdao from October 2018 to December 2019. Participants completed a cross-sectional questionnaire to assess their actual participation and perceived importance in shared decision-making on treatment and care. Descriptive analysis and non-parametric tests were carried out to assess the status quo of patients' shared decision-making on treatment and care. Binary logistic regression analysis with a stepwise back-wards was applied to predict factors that affected patients' participation in shared decision-making.
Results
The results showed that patients with lung cancer had a low degree of participation in shared decision-making. There were significant differences between actual participation and perceived importance of shared decision-making on treatment and care. Education level, age, gender, income, marital status, personality, the course of the disease (> 6 months), and the pathological TNM staging (III) affected patient's level of participation in shared decision-making.
Conclusion
Actual participation in shared decision-making on the treatment and care of lung cancer patients was low and considered unimportant. We could train oncology nurses to use patient decision aids to help patients and families participate in shared decision-making on patients’ value, preferences and needs.
Similar content being viewed by others
Availability of data and materials
All authors declared that all data and materials as well as software application or custom code support their published claims and comply with field standards.
References
Berger-Höger B, Liethmann K, Mühlhauser I, Haastert B, Steckelberg A (2019) Nurse-led coaching of shared decision-making for women with ductal carcinoma in situ in breast care centers: a cluster randomized controlled trial. Int J Nurs Stud 93:141–152. https://doi.org/10.1016/j.ijnurstu.2019.01.013
Brenner AT, Malo TL, Margolis M, Elston Lafata J, James S, Vu MB, Reuland DS (2018) Evaluating shared decision making for lung cancer screening. JAMA Intern Med 178(10):1311–1316. https://doi.org/10.1001/jamainternmed.2018.3054
Chang HL, Li FS, Lin CF (2019) Factors influencing implementation of shared medical decision making in patients with cancer. Patient Prefer Adherence 13:1995–2005. https://doi.org/10.2147/PPA.S217561
Chen YC, Huang HM, Kao CC, Sun CK, Chiang CY, Sun FK (2016) The Psychological process of breast cancer patients receiving initial chemotherapy: rising from the ashes. Cancer Nurs 39(6):E36-e44. https://doi.org/10.1097/ncc.0000000000000331
Coulter A (2017) Shared decision making: everyone wants it, so why isn’t it happening? World Psychiatry 16(2):117–118. https://doi.org/10.1002/wps.20407
Cuypers M, Lamers RED, de Vries M, Husson O, Kil PJM, van de Poll-Franse LV (2016) Prostate cancer survivors with a passive role preference in treatment decision-making are less satisfied with information received: results from the PROFILES registry. Urol Oncol 34(11):482.e11-482.e18. https://doi.org/10.1016/j.urolonc.2016.06.015
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT (2017) The eighth edition lung cancer stage classification. Chest 151(1):193–203. https://doi.org/10.1016/j.chest.2016.10.010.
Duma N, Santana-Davila R, Molina JR (2019) Non-small cell lung cancer: epidemiology, screening, diagnosis, and treatment. Mayo Clin Proc 94(8):1623–1640. https://doi.org/10.1016/j.mayocp.2019.01.013
Durand MA, Yen RW, O’Malley AJ, Schubbe D, Politi MC, Saunders CH, Elwyn G (2020) What matters most: randomized controlled trial of breast cancer surgery conversation aids across socioeconomic strata. Cancer 127(3):422–436. https://doi.org/10.1002/cncr.33248
Elwyn G, Durand MA, Song J, Aarts J, Barr PJ, Berger Z, Van der Weijden T (2017) A three-talk model for shared decision making: multistage consultation process. BMJ 359:j4891. https://doi.org/10.1136/bmj.j4891
Elwyn G, O'Connor A, Stacey D, Volk R, Edwards A, Coulter A, et al, International Patient Decision Aids Standards (IPDAS) Collaboration (2006). Developing a quality criteria framework for patient decision aids: online international Delphi consensus process. BMJ (Clinical research ed.) 333(7565):417. https://doi.org/10.1136/bmj.38926.629329.AE.
Friesen-Storms JH, Bours GJ, van der Weijden T, Beurskens AJ (2015) Shared decision making in chronic care in the context of evidence based practice in nursing. Int J Nurs Stud 52(1):393–402. https://doi.org/10.1016/j.ijnurstu.2014.06.012
Fulford K, Handa A (2021) New resources for understanding patients’ values in the context of shared clinical decision-making. World Psychiatry 20(3):446–447. https://doi.org/10.1002/wps.20902
Hall H, Tocock A, Burdett S, Fisher D, Ricketts WM, Robson J, et al (2021) Association between time-to-treatment and outcomes in non-small cell lung cancer: a systematic review. Thorax. https://doi.org/10.1136/thoraxjnl-2021-216865.
Hobbs GS, Landrum MB, Arora NK et al (2015) The role of families in decisions regarding cancer treatments. Cancer 121(7):1079–1087. https://doi.org/10.1002/cncr.29064
Hoefel L, Lewis KB (2020) 20th anniversary update of the ottawa decision support framework: part 2 subanalysis of a systematic review of patient decision aids. Med Decis Mak 40(4):522–539. https://doi.org/10.1177/0272989x20924645
Hull O, Niranjan SJ, Wallace AS, Williams BR, Turkman YE, Ingram SA, Rocque GB (2020) Should we be talking about guidelines with patients? A qualitative analysis in metastatic breast cancer. Breast Cancer Res Treat 184(1):115–121. https://doi.org/10.1007/s10549-020-05832-x
John Beebe CJ (2016) Psychological types. Routledge, New York
Kinsey K, Firth J, Elwyn G, Edwards A, Brain K, Marrin K, Wood F (2017) Patients’ views on the use of an option grid for knee osteoarthritis in physiotherapy clinical encounters: an interview study. Health Expect 20(6):1302–1310. https://doi.org/10.1111/hex.12570
Kunneman M, Montori VM, Castaneda-Guarderas A, Hess EP (2016) What is shared decision making? (and what it is not). Acad Emerg Med 23(12):1320–1324. https://doi.org/10.1111/acem.13065
Lee SK, Knobf MT (2016) Family involvement for breast cancer decision making among Chinese–American women. Psychooncology 25(12):1493–1499. https://doi.org/10.1002/pon.3989
Leng A, Jing J, Nicholas S, Wang J (2019) Geographical disparities in treatment and health care costs for end-of-life cancer patients in China: a retrospective study. BMC Cancer 19(1):39. https://doi.org/10.1186/s12885-018-5237-1
Loh K, Tsang M, LeBlanc T, Back A, Duberstein P, Mohile S, Lee S (2020) Decisional involvement and information preferences of patients with hematologic malignancies. Blood Adv 4(21):5492–5500. https://doi.org/10.1182/bloodadvances.2020003044
Lowenstein M, Vijayaraghavan M, Burke NJ, Karliner L, Wang S, Peters M, Kaplan CP (2019) Real-world lung cancer screening decision-making: barriers and facilitators. Lung Cancer 133:32–37. https://doi.org/10.1016/j.lungcan.2019.04.026
Ma L (2004) Research on the status quo and influencing factors of cancer patients' participation in treatment and nursing decisions. (Master), Peking Union Medical College, Beijing
Montori VM, Kunneman M, Brito JP (2017) Shared decision making and improving health care: the answer is not in. JAMA 318(7):617–618. https://doi.org/10.1001/jama.2017.10168
Nakayama K, Osaka W, Matsubara N, Takeuchi T, Toyoda M, Ohtake N, Uemura H (2020) Shared decision making, physicians’ explanations, and treatment satisfaction: a cross-sectional survey of prostate cancer patients. BMC Med Inform Decis Mak 20(1):334. https://doi.org/10.1186/s12911-020-01355-z
O'Connor AM, Stacey D, Entwistle V, Llewellyn-Thomas H, Rovner D, Holmes-Rovner M, Tait V, Tetroe J, Fiset V, Barry M, Jones J (2003) Decision aids for people facing health treatment or screening decisions. Cochrane Database System Rev. https://doi.org/10.1002/14651858.CD001431
Passalacqua R, Caminiti C, Salvagni S, Barni S, Beretta GD, Carlini P, Campione F (2004) Effects of media information on cancer patients’ opinions, feelings, decision-making process and physician-patient communication. Cancer 100(5):1077–1084. https://doi.org/10.1002/cncr.20050
Patient Decision Aids (2020) Patient Decision Aids. Retrieved 02–20, 2021, from https://decisionaid.ohri.ca/index.html
Rahn AC, Köpke S, Backhus I, Kasper J, Anger K, Untiedt B, Heesen C (2018) Nurse-led immunotreatment DEcision Coaching In people with Multiple Sclerosis (DECIMS) - Feasibility testing, pilot randomised controlled trial and mixed methods process evaluation. Int J Nurs Stud 78:26–36. https://doi.org/10.1016/j.ijnurstu.2017.08.011
Rahn AC, Jull J, Boland L, Finderup J, Loiselle MC, Smith M, Köpke S, Stacey D (2021) Guidance and/or decision coaching with patient decision aids: scoping reviews to inform the international patient decision aid standards (IPDAS). Med Decis Mak 41(7):938–953. https://doi.org/10.1177/0272989X21997330
Sainio C, Lauri S (2003) Cancer patients’ decision-making regarding treatment and nursing care. J Adv Nurs 41(3):250–260. https://doi.org/10.1046/j.1365-2648.2003.02525.x
Scalia P, Durand MA, Faber M, Kremer JA, Song J, Elwyn G (2019) User-testing an interactive option grid decision aid for prostate cancer screening: lessons to improve usability. BMJ Open 9(5):e026748. https://doi.org/10.1136/bmjopen-2018-026748
Schmidt K, Damm K, Prenzler A, Golpon H, Welte T (2016) Preferences of lung cancer patients for treatment and decision-making: a systematic literature review. Eur J Cancer Care 25(4):580–591. https://doi.org/10.1111/ecc.12425
Sferra SR, Cheng JS, Boynton Z, DiSesa V, Kaiser LR, Ma GX, Erkmen CP (2020) Aiding shared decision making in lung cancer screening: two decision tools. J Public Health (Oxf). https://doi.org/10.1093/pubmed/fdaa063.
Shen HN, Lin CC, Hoffmann T, Tsai CY, Hou WH, Kuo KN (2019) The relationship between health literacy and perceived shared decision making in patients with breast cancer. Patient Educ Couns 102(2):360–366. https://doi.org/10.1016/j.pec.2018.09.017
Stacey D, Légaré F (2020) 20th anniversary Ottawa decision support framework: part 3 overview of systematic reviews and updated framework. Med Decis Making 40(3):379–398. https://doi.org/10.1177/0272989x20911870
Sullivan DR, Eden KB, Dieckmann NF, Golden SE, Vranas KC, Nugent SM, Slatore CG (2019) Understanding patients’ values and preferences regarding early stage lung cancer treatment decision making. Lung Cancer 131:47–57. https://doi.org/10.1016/j.lungcan.2019.03.009
The Health Foundation (2012) A simple tool to facilitate shared decisions. Retrieved June 15, 2021, from http://www.health.org.uk/newsletter-feature/a-simple-tool-to-facilitate-shared-decisions
Wolff JL, Roter DL (2011) Family presence in routine medical visits: a meta-analytical review. Soc Sci Med 72(6):823–831. https://doi.org/10.1016/j.socscimed.2011.01.015
Woodard GA, Jones KD, Jablons DM (2016) Lung cancer staging and prognosis. Cancer Treat Res 170:47–75. https://doi.org/10.1007/978-3-319-40389-2_3
World Health Organization (2021a) Cancer. Retrieved 05–01, 2021a, from https://www.who.int/news-room/fact-sheets/detail/cancer
World Health Organization (2021b) Palliative care. Retrieved 05–01, 2022, from https://www.who.int/news-room/fact-sheets/detail/palliative-care
Funding
The study was funded by Project of Research Planning Foundation on Humanities and Social Sciences of the Ministry of Education (No. 20YJAZH144).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Study design and material preparation were performed by Ying Wang, Bo Hu, and Jinna Zhang. Data collection and analysis were performed by Ying Wang, Jinna Zhang, Bo Hu, Jizhe Wang, Laixiang Zhang, Xiaohua Li, and Xiuli Zhu. The first draft of the manuscript was written by Ying Wang, Jinna Zhang, and Bo Hu and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethics approval
This study was conducted according to the Declaration of Helsinki and were supported by the ethical committee of the university which the researchers affiliated.
Consent to participate
Before distributing the questionnaires, all the patients signed the informed consents. That indicated that they understood the nature and purpose of the study and they knew that their personal information would not be divulged.
Consent for publication
Not applicable. Because this is not a case study, but cross-sectional study. We collect data anonymously. We present the results by analysing a large number of quantitative data and there will be no information leakage of any participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, Y., Zhang, J., Hu, B. et al. Influencing factors of lung cancer patients' participation in shared decision-making: a cross-sectional study. J Cancer Res Clin Oncol 148, 3303–3312 (2022). https://doi.org/10.1007/s00432-022-04105-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-022-04105-y